Xopenex HFA: Package Insert / Prescribing Info
Package insert / product label
Generic name: levalbuterol tartrate
Dosage form: aerosol, metered
Drug class: Adrenergic bronchodilators
Medically reviewed by Drugs.com. Last updated on Aug 3, 2025.
On This Page
- Indications and Usage
- Dosage and Administration
- Dosage Forms and Strengths
- Contraindications
- Warnings and Precautions
- Adverse Reactions/Side Effects
- Drug Interactions
- Use In Specific Populations
- Overdosage
- Description
- Clinical Pharmacology
- Nonclinical Toxicology
- Clinical Studies
- How Supplied/Storage and Handling
- Patient Counseling Information
Highlights of Prescribing Information
XOPENEX HFA® (levalbuterol tartrate) inhalation aerosol, for oral inhalation use
Initial U.S. Approval: 1999
Indications and Usage for Xopenex HFA
XOPENEX HFA is a beta2-adrenergic agonist indicated for the treatment or prevention of bronchospasm in patients 4 years of age and older with reversible obstructive airway disease. (1.1)
Xopenex HFA Dosage and Administration
For Oral Inhalation Only (2.2)
- Adults and children 4 years of age and older: 2 inhalations repeated every 4 to 6 hours; in some patients, 1 inhalation every 4 hours may be sufficient. (2.1)
- Prime XOPENEX HFA before using for the first time and when the inhaler has not been used for more than 3 days. To prime XOPENEX HFA, release 4 sprays into the air away from the face. (2.2)
- At least once a week, wash the actuator with warm water and let it air-dry completely. (2.2)
Dosage Forms and Strengths
Inhalation Aerosol: Each actuation delivers 59 mcg of levalbuterol tartrate (equivalent to 45 mcg of levalbuterol free base) from the actuator mouthpiece.
- 15 g pressurized canister containing 200 actuations (3)
Contraindications
Hypersensitivity to levalbuterol, racemic albuterol or any other component of XOPENEX HFA Inhalation Aerosol. (4)
Warnings and Precautions
- Life-threatening paradoxical bronchospasm may occur. Discontinue XOPENEX HFA immediately and treat with alternative therapy. (5.1)
- Need for more doses of XOPENEX HFA than usual may be a sign of deterioration of asthma and requires reevaluation of treatment. (5.2)
- XOPENEX HFA is not a substitute for corticosteroids. (5.3)
- Cardiovascular effects may occur. Consider discontinuation of XOPENEX HFA if these effects occur. Use with caution in patients with underlying cardiovascular disorders. (5.4)
- Excessive use may be fatal. Do not exceed recommended dose. (5.5)
- Immediate hypersensitivity reactions may occur. Discontinue XOPENEX HFA immediately. (5.6)
- Hypokalemia and changes in blood glucose may occur. (5.7, 5.8)
Adverse Reactions/Side Effects
Most common adverse reactions (≥ 2% and > placebo) are accidental injury, bronchitis, dizziness, pain, pharyngitis, rhinitis, and vomiting. (6)
To report SUSPECTED ADVERSE REACTIONS, contact Lupin Pharmaceuticals, Inc. at 1-800-399-2561 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Drug Interactions
- Other short-acting sympathomimetic aerosol bronchodilators and adrenergic drugs: May potentiate effect. (7)
- Beta-blockers: May block bronchodilatory effects of beta-agonists and produce severe bronchospasm. Patients with asthma should not normally be treated with beta-blockers. (7.1)
- Diuretics: May worsen electrocardiographic changes or hypokalemia associated with diuretics may worsen. Consider monitoring potassium levels. (7.2)
- Digoxin: May decrease serum digoxin levels. Consider monitoring digoxin levels. (7.3)
- Monoamine oxidase inhibitors (MAOs) or tricyclic antidepressants: May potentiate effect of albuterol on the cardiovascular system. Consider alternative therapy in patients taking MAO inhibitors or tricyclic antidepressants. (7.4)
See 17 for PATIENT COUNSELING INFORMATION and FDA-approved patient labeling.
Revised: 7/2025
Full Prescribing Information
2. Xopenex HFA Dosage and Administration
2.1 Recommended Dosages
The recommended dosage of XOPENEX HFA for adults and children 4 years of age and older is 2 inhalations (90 mcg of levalbuterol free base) repeated every 4 to 6 hours; in some patients, 1 inhalation (45 mcg of levalbuterol free base) every 4 hours may be sufficient. More frequent administration or a larger number of inhalations is not routinely recommended.
If a previously effective dosage regimen fails to provide the usual response, this may be a marker of destabilization of asthma and requires reevaluation of the patient and the treatment regimen, giving special consideration to the possible need for anti-inflammatory treatment, e.g., corticosteroids.
2.2 Administration Information
- Shake well before use.
- Avoid spraying in the eyes.
- Prime the inhaler before using for the first time and when the inhaler has not been used for more than 3 days by releasing 4 test sprays into the air, away from the face.
- To maintain proper use of XOPENEX HFA, it is critical to wash the actuator with warm water and air-dry thoroughly at least once a week. The inhaler may cease to deliver levalbuterol tartrate if not properly cleaned and dried thoroughly. Keep the plastic actuator clean to prevent medication build-up and blockage. If the actuator becomes blocked with levalbuterol tartrate, wash the actuator to remove the blockage.
- The canister is fitted with a dose indicator, which indicates how many inhalations remain. The dose indicator display will move after every tenth actuation. When nearing the end of the usable inhalations, the color behind the number in the dose indicator window changes to red. Discard the inhaler when the dose indicator display window shows zero, corresponding to the use of 200 actuations.
3. Dosage Forms and Strengths
Inhalation aerosol: XOPENEX HFA is a pressurized, metered dose aerosol.
Each XOPENEX HFA 15 gram canister contains 200 metered actuations (or inhalations).
Each canister is fitted with a dose indicator and is supplied with a blue plastic actuator mouthpiece and a red mouthpiece cap. After priming, each actuation of the inhaler delivers 59 mcg of levalbuterol tartrate (equivalent to 45 mcg of levalbuterol free base) from the actuator mouthpiece.
4. Contraindications
XOPENEX HFA is contraindicated in patients with a history of hypersensitivity to levalbuterol, racemic albuterol, or any other component of XOPENEX HFA. Reactions have included urticaria, angioedema, rash, bronchospasm, anaphylaxis, and oropharyngeal edema.
5. Warnings and Precautions
5.1 Paradoxical Bronchospasm
XOPENEX HFA can produce paradoxical bronchospasm, which may be life-threatening. If paradoxical bronchospasm occurs, XOPENEX HFA should be discontinued immediately and alternative therapy instituted. It should be recognized that paradoxical bronchospasm, when associated with inhaled formulations, frequently occurs with the first use of a new canister.
5.2 Deterioration of Asthma
Asthma may deteriorate acutely over a period of hours or chronically over several days or longer. If the patient needs more doses of XOPENEX HFA than usual, this may be a marker of destabilization of asthma and requires reevaluation of the patient and treatment regimen, giving special consideration to the possible need for anti-inflammatory treatment, e.g., corticosteroids.
5.3 Use of Anti-Inflammatory Agents
The use of a beta-adrenergic agonist alone may not be adequate to control asthma in many patients. Early consideration should be given to adding anti-inflammatory agents, e.g., corticosteroids, to the therapeutic regimen.
5.4 Cardiovascular Effects
XOPENEX HFA, like other beta-adrenergic agonists, can produce clinically significant cardiovascular effects in some patients, as measured by heart rate, blood pressure, and symptoms. Although such effects are uncommon after administration of XOPENEX HFA at recommended doses, if they occur, the drug may need to be discontinued. In addition, beta-agonists have been reported to produce electrocardiogram (ECG) changes, such as flattening of the T-wave, prolongation of the QTc interval, and ST segment depression. The clinical significance of these findings is unknown. Therefore, XOPENEX HFA, like all sympathomimetic amines, should be used with caution in patients with cardiovascular disorders, especially coronary insufficiency, cardiac arrhythmias, and hypertension.
5.5 Do Not Exceed Recommended Dose
Fatalities have been reported in association with excessive use of inhaled sympathomimetic drugs in patients with asthma. The exact cause of death is unknown, but cardiac arrest following an unexpected development of a severe acute asthmatic crisis and subsequent hypoxia is suspected.
5.6 Immediate Hypersensitivity Reactions
Immediate hypersensitivity reactions may occur after administration of racemic albuterol, as demonstrated by rare cases of urticaria, angioedema, rash, bronchospasm, anaphylaxis, and oropharyngeal edema. The potential for hypersensitivity must be considered in the clinical evaluation of patients who experience immediate hypersensitivity reactions while receiving XOPENEX HFA.
5.7 Coexisting Conditions
XOPENEX HFA, like all sympathomimetic amines, should be used with caution in patients with cardiovascular disorders, especially coronary insufficiency, hypertension, and cardiac arrhythmias; in patients with convulsive disorders, hyperthyroidism, or diabetes mellitus; and in patients who are unusually responsive to sympathomimetic amines. Clinically significant changes in systolic and diastolic blood pressure have been seen in individual patients and could be expected to occur in some patients after the use of any beta-adrenergic bronchodilator.
Large doses of intravenous racemic albuterol have been reported to aggravate preexisting diabetes mellitus and ketoacidosis.
5.8 Hypokalemia
As with other beta-adrenergic agonist medications, XOPENEX HFA may produce significant hypokalemia in some patients, possibly through intracellular shunting, which has the potential to produce adverse cardiovascular effects. The decrease is usually transient, not requiring supplementation.
6. Adverse Reactions/Side Effects
Use of XOPENEX HFA may be associated with the following:
- Paradoxical bronchospasm [see Warnings and Precautions (5.1)]
- Cardiovascular effects [see Warnings and Precautions (5.4)]
- Immediate hypersensitivity reactions [see Warnings and Precautions (5.6)]
- Hypokalemia [see Warnings and Precautions (5.8)]
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared with rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Adults and Adolescents 12 Years of Age and Older
Adverse reaction information concerning XOPENEX HFA in adults and adolescents is derived from two 8-week, multicenter, randomized, double-blind, active- and placebo-controlled trials in 748 adult and adolescent patients with asthma that compared XOPENEX HFA, a marketed albuterol HFA inhaler, and an HFA-134a placebo inhaler. Table 1 lists the incidence of all adverse reactions (whether considered by the investigator to be related or unrelated to drug) from these trials that occurred at a rate of 2% or greater in the group treated with XOPENEX HFA and more frequently than in the HFA-134a placebo inhaler group.
|
* This table includes all adverse reactions (whether considered by the investigator to be related or unrelated to drug) from these trials that occurred at a rate of 2% or greater in the group treated with XOPENEX HFA and more frequently than in the HFA-134a placebo inhaler group. |
||||
| Body System
| Preferred Term
| XOPENEX HFA 90 mcg (n=403)
| Racemic Albuterol HFA 180 mcg (n=179)
| Placebo (n=166)
|
| Respiratory System | Asthma | 9% | 7% | 6% |
| Pharyngitis | 8% | 2% | 2% |
|
| Rhinitis | 7% | 2% | 3% |
|
| Body as a Whole | Pain | 4% | 3% | 4% |
| Central Nervous System | Dizziness | 3% | 1% | 2% |
Adverse reactions reported by less than 2% and at least 2 or more of the adolescent and adult patients receiving XOPENEX HFA and by a greater proportion than receiving HFA-134a placebo inhaler include cyst, flu syndrome, viral infection, constipation, gastroenteritis, myalgia, hypertension, epistaxis, lung disorder, acne, herpes simplex, conjunctivitis, ear pain, dysmenorrhea, hematuria, and vaginal moniliasis. There were no significant laboratory abnormalities observed in these studies.
Pediatric Patients 4 to 11 Years of Age
Adverse reaction information concerning XOPENEX HFA in children is derived from a 4-week, randomized, double-blind trial of XOPENEX HFA, a marketed albuterol HFA inhaler, and an HFA-134a placebo inhaler in 150 children aged 4 to 11 years with asthma. Table 2 lists the adverse reactions reported for XOPENEX HFA in children at a rate of 2% or greater and more frequently than for placebo.
|
* This table includes all adverse reactions (whether considered by the investigator to be related or unrelated to drug) from the trial that occurred at a rate of 2% or greater in the group treated with XOPENEX HFA and more frequently than in the HFA-134a placebo inhaler group. |
||||
| Body System
| Preferred Term
| XOPENEX HFA 90 mcg (n=76)
| Racemic Albuterol HFA 180 mcg (n=39)
| Placebo (n=35)
|
| Digestive System | Vomiting | 11% | 8% | 6% |
| Body as a Whole | Accidental injury | 9% | 10% | 6% |
| Respiratory System | Pharyngitis | 7% | 13% | 6% |
| Bronchitis | 3% | 0% | 0% |
|
The incidence of systemic beta-adrenergic adverse reactions (e.g., tremor, nervousness) was low and comparable across all treatment groups, including placebo.
6.2 Post-marketing Experience
In addition to the adverse reactions reported in clinical trials, the following adverse reactions have been observed in post-approval use of levalbuterol inhalation solution. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure. These events have been chosen for inclusion due to their seriousness, their frequency of reporting, or their likely beta-mediated mechanism: angioedema, anaphylaxis, arrhythmias (including atrial fibrillation, supraventricular tachycardia, extrasystoles), asthma, chest pain, cough increased, dysphonia, dyspnea, gastrooesophageal reflux disease (GERD), metabolic acidosis, nausea, nervousness, rash, tachycardia, tremor, urticaria.
In addition, XOPENEX HFA, like other sympathomimetic agents, can cause adverse reactions such as hypertension, angina, vertigo, central nervous system stimulation, sleeplessness, headache, and drying or irritation of the oropharynx.
Related/similar drugs
7. Drug Interactions
Other short-acting sympathomimetic aerosol bronchodilators or epinephrine should not be used concomitantly with XOPENEX HFA. If additional adrenergic drugs are to be administered by any route, they should be used with caution to avoid deleterious cardiovascular effects.
7.1 Beta-blockers
Beta-blockers: Beta-adrenergic receptor blocking agents not only block the pulmonary effect of beta-adrenergic agonists, such as XOPENEX HFA, but may produce severe bronchospasm in asthmatic patients. Therefore, patients with asthma should not normally be treated with beta-blockers. However, under certain circumstances, e.g., as prophylaxis after myocardial infarction, there may be no acceptable alternatives to the use of beta-adrenergic blocking agents in patients with asthma. In this setting, cardioselective beta-blockers should be considered, although they should be administered with caution.
7.2 Diuretics
The ECG changes or hypokalemia that may result from the administration of non-potassium-sparing diuretics (such as loop and thiazide diuretics) can be acutely worsened by beta-agonists, especially when the recommended dose of the beta-agonist is exceeded. Although the clinical significance of these effects is not known, caution is advised in the coadministration of beta-agonists with non-potassium-sparing diuretics. Consider monitoring potassium levels.
7.3 Digoxin
Mean decreases of 16% to 22% in serum digoxin levels were demonstrated after single-dose intravenous and oral administration of racemic albuterol, respectively, to normal volunteers who had received digoxin for 10 days. The clinical significance of these findings for patients with obstructive airway disease who are receiving XOPENEX HFA and digoxin on a chronic basis is unclear. Nevertheless, it would be prudent to carefully evaluate the serum digoxin levels in patients who are currently receiving digoxin and XOPENEX HFA.
7.4 Monoamine Oxidase Inhibitors or Tricyclic Antidepressants
XOPENEX HFA should be administered with extreme caution to patients being treated with monoamine oxidase inhibitors or tricyclic antidepressants, or within 2 weeks of discontinuation of such agents, because the action of albuterol on the vascular system may be potentiated. Consider alternative therapy in patients taking MAO inhibitors or tricyclic antidepressants.
8. Use In Specific Populations
8.1 PREGNANCY
There are no adequate and well-controlled studies of XOPENEX HFA in pregnant women. There are clinical considerations with the use of XOPENEX HFA in pregnant women [see Clinical Considerations].
Following oral administration of levalbuterol HCl to pregnant rabbits, there was no evidence of teratogenicity at doses up to 25 mg/kg/day [approximately 750 times the maximum recommended human daily inhalation dose (MRHDID) of levalbuterol tartrate for adults on a mg/m2 basis]; however, racemic albuterol sulfate was teratogenic in mice (cleft palate) and rabbits (cranioschisis) at doses slightly higher than the human therapeutic range (see Data).
The estimated background risk of major birth defects and miscarriage for the indicated population(s) are unknown. In the U.S. general population, the estimated risk of major birth defects and miscarriage in clinically recognized pregnancies is 2 to 4% and 15 to 20%, respectively.
Clinical Considerations
Disease-Associated Maternal and/or Embryo/Fetal Risk
In women with poorly or moderately controlled asthma, there is an increased risk of preeclampsia in the mother and prematurity, low birth weight, and small for gestational age in the neonate. Pregnant women should be closely monitored and medication adjusted as necessary to maintain optimal control.
Labor or Delivery
Because of the potential for beta-adrenergic agonists to interfere with uterine contractility, the use of XOPENEX HFA for the treatment of bronchospasm during labor should be restricted to those patients in whom the benefits clearly outweigh the risk.
XOPENEX HFA has not been approved for the management of preterm labor. The benefit:risk ratio when levalbuterol tartrate is administered for tocolysis has not been established. Serious adverse reactions, including maternal pulmonary edema, have been reported during or following treatment of premature labor with beta2-agonists, including racemic albuterol.
Data
Animal Data
The oral administration of levalbuterol HCl to pregnant New Zealand White rabbits during the period of organogenesis found no evidence of teratogenicity at doses up to 25 mg/kg/day (approximately 750 times the MRHDID of levalbuterol tartrate for adults on a mg/m2 basis). In a rat developmental study, a racemic albuterol sulfate (comprising approximately 50% levalbuterol)/HFA-134a formulation administered by inhalation did not produce any teratogenic effects at exposures approximately 160 times the MRHDID (on a mg/m2 basis at a maternal dose of 10.5 mg/kg).
However, other developmental studies with the racemic albuterol sulfate, did result in teratogenic effects in mice and rabbits at doses slightly higher than the human therapeutic range. In a rabbit development study, orally administered albuterol sulfate induced cranioschisis in 7 of 19 fetuses (37%) at approximately 1500 times the MRHDID (on a mg/m2 basis at a maternal dose of 50 mg/kg). In a mouse developmental study, subcutaneously administered albuterol sulfate produced cleft palate formation in 5 of 111 (4.5%) fetuses at an exposure approximately 2 times MRHDID for adults (on a mg/m2 basis at a maternal dose of 0.25 mg/kg/day) and in 10 of 108 (9.3%) fetuses at approximately 20 times MRHDID (on a mg/m2 basis at a maternal dose of 2.5 mg/kg/day). Similar effects were not observed at approximately 0.2 times MRHDID of levalbuterol tartrate for adults on a mg/m2 basis (i.e., less than the therapeutic dose). Cleft palate also occurred in 22 of 72 (30.5%) fetuses from females treated subcutaneously with isoproterenol (positive control).
8.2 Lactation
There are no available data on the presence of levalbuterol in human milk, the effects on the breastfed child, or the effects on milk production.
The developmental and health benefits of breastfeeding should be considered along with the mother's clinical need for XOPENEX HFA and any potential adverse effects on the breastfed child from XOPENEX HFA or from the underlying maternal condition.
8.4 PEDIATRIC USE
Pediatric Patients 4 Years of Age and Older
The safety and efficacy of XOPENEX HFA have been established in pediatric patients 4 years of age and older in an adequate and well-controlled clinical trial [see Adverse Reactions (6) and Clinical Studies (14)].
Pediatric Patients less than 4 Years of Age
XOPENEX HFA is not indicated for pediatric patients less than 4 years of age. A clinical trial in pediatric patients below the age of 4 years showed no statistical significant difference between treatment groups in the primary efficacy endpoint. There was an increased incidence of asthma-related adverse reactions reported in pediatric patients below the age of 4 years treated with XOPENEX HFA compared to placebo.
XOPENEX HFA was evaluated in one 4-week, multicenter, randomized, modified-blind, placebo-controlled, parallel group trial of 196 pediatric patients ages birth to <4 years of age with asthma or reactive airway disease (68 patients birth to <2 years of age and 128 patients 2 to <4 years of age). XOPENEX HFA 45 mcg (N=23), XOPENEX HFA 90 mcg (N=42), levalbuterol inhalation solution 0.31 mg (N=63), and placebo HFA (N=68) were administered three times daily. XOPENEX HFA or placebo HFA was delivered with the Monaghan AeroChamber MAX™ Valved Holding Chamber with mask. The primary efficacy endpoint was the mean change in Pediatric Asthma Caregiver Assessment (PACA) total score from baseline over the 4 week treatment period. There was no statistical difference in the change in PACA total score between XOPENEX HFA and placebo. Regarding safety, an increased number of treatment-emergent asthma-related adverse reactions were reported in XOPENEX HFA-treated patients. Eight subjects reported asthma-related adverse reactions for XOPENEX HFA compared to 3 subjects for placebo. There was one subject that discontinued treatment due to asthma in the XOPENEX HFA group compared to zero subjects in the placebo group (Table 3). Other adverse reactions were consistent with those observed in the clinical trial population of patients 4 years of age and older [see Adverse Reactions (6.1)].
|
*This table includes the following Preferred Terms (whether considered by the investigator to be related or unrelated to drug): asthma, cough, hypoxia, status asthmaticus, tachypnea |
|||
| XOPENEX HFA 45-90 mcg (n=65)
| Levalbuterol inhalation solution 0.31 mg (n=63)
| Placebo (n=68)
|
|
| Asthma-related adverse reactions*, n (%) | 8 (12%) | 6 (10%) | 3 (4%) |
| Treatment discontinuations due to asthma, n (%) | 1 (2%) | 2 (3%) | 0 |
8.5 GERIATRIC USE
Clinical studies of XOPENEX HFA did not include sufficient numbers of subjects aged 65 and older to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant diseases or other drug therapy.
8.6 Renal Impairment
Albuterol is known to be substantially excreted by the kidney, and the risk of toxic reactions may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to monitor renal function.
10. Overdosage
The expected symptoms with overdosage are those of excessive beta-adrenergic receptor stimulation and/or occurrence or exaggeration of any of the symptoms listed under Adverse Reactions (6), e.g., seizures, angina, hypertension or hypotension, tachycardia with rates up to 200 beats/minute, arrhythmias, nervousness, headache, tremor, dry mouth, palpitation, nausea, dizziness, fatigue, malaise, and sleeplessness. Hypokalemia also may occur. As with all sympathomimetic medications, cardiac arrest and even death may be associated with the abuse of XOPENEX HFA. Treatment consists of discontinuation of XOPENEX HFA together with appropriate symptomatic therapy. The judicious use of a cardioselective beta-receptor blocker may be considered, bearing in mind that such medication can produce bronchospasm. There is insufficient evidence to determine if dialysis is beneficial for overdosage of XOPENEX HFA.
11. Xopenex HFA Description
The active component of XOPENEX HFA inhalation aerosol is levalbuterol tartrate, the (R)-enantiomer of albuterol. Levalbuterol tartrate is a relatively selective beta2-adrenergic receptor agonist [see Clinical Pharmacology (12)]. Levalbuterol tartrate has the chemical name (R)-α1-[[(1,1-dimethylethyl)amino]methyl]-4-hydroxy-1,3-benzenedimethanol L-tartrate (2:1 salt), and it has the following chemical structure:
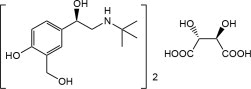
The molecular weight of levalbuterol tartrate is 628.71, and its empirical formula is (C13H21NO3)2 · C4H6O6. It is a white to light-yellow solid, freely soluble in water and very slightly soluble in ethanol.
Levalbuterol tartrate is the generic name for (R)-albuterol tartrate in the United States. XOPENEX HFA inhalation aerosol is a pressurized metered-dose aerosol inhaler (MDI) fitted with a dose indicator, which produces an aerosol for oral inhalation. It contains a suspension of micronized levalbuterol tartrate, propellant HFA-134a (1,1,1,2-tetrafluoroethane), Dehydrated Alcohol USP, and Oleic Acid NF.
After priming with 4 actuations, each actuation of the inhaler delivers 67.8 mcg of levalbuterol tartrate (equivalent to 51.6 mcg of levalbuterol free base) from the valve and 59 mcg of levalbuterol tartrate (equivalent to 45 mcg of levalbuterol free base) from the actuator mouthpiece. Each 15 g canister provides 200 actuations (or inhalations).
12. Xopenex HFA - Clinical Pharmacology
12.1 MECHANISM OF ACTION
Activation of beta2-adrenergic receptors on airway smooth muscle leads to the activation of adenylate cyclase and to an increase in the intracellular concentration of cyclic-3', 5'-adenosine monophosphate (cyclic AMP). The increase in cyclic AMP is associated with the activation of protein kinase A, which in turn, inhibits the phosphorylation of myosin and lowers intracellular ionic calcium concentrations, resulting in muscle relaxation. Levalbuterol relaxes the smooth muscles of all airways, from the trachea to the terminal bronchioles. Increased cyclic AMP concentrations are also associated with the inhibition of the release of mediators from mast cells in the airways. Levalbuterol acts as a functional antagonist to relax the airway irrespective of the spasmogen involved, thus protecting against all bronchoconstrictor challenges. While it is recognized that beta2-adrenergic receptors are the predominant receptors on bronchial smooth muscle, data indicate that there are beta-receptors in the human heart, 10% to 50% of which are beta2-adrenergic receptors. The precise function of these receptors has not been established [see Warnings and Precautions (5)]. However, all beta-adrenergic agonist drugs can produce a significant cardiovascular effect in some patients, as measured by pulse rate, blood pressure, symptoms, and/or electrocardiographic changes.
12.2 PHARMACOKINETICS
A population pharmacokinetic model was developed using plasma concentrations of (R)-albuterol obtained from 632 asthmatic patients aged 4 to 81 years in three large trials. For adolescent and adult patients 12 years and older, following 90 mcg dose of XOPENEX HFA, yielded mean peak plasma concentrations (Cmax) and systemic exposure (AUC0-6) of approximately 199 pg/mL and 695 pg•h/mL, respectively, compared to approximately 238 pg/mL and 798 pg•h/mL, respectively, following 180 mcg dose of Racemic Albuterol HFA metered-dose inhaler. For pediatric patients from 4 to 11 years of age, following 90 mcg dose of XOPENEX HFA, yielded Cmax and AUC0-6 of approximately 163 pg/mL and 579 pg•h/mL, respectively, compared to approximately 238 pg/mL and 828 pg•h/mL, respectively, following 180 mcg dose of Racemic Albuterol HFA metered-dose inhaler.
These pharmacokinetic data indicate that mean exposure to (R)-albuterol was 13% to 16% less in adult and 30% to 32% less in pediatric patients given XOPENEX HFA as compared to those given a comparable dose of racemic albuterol. When compared to adult patients, pediatric patients given 90 mcg of levalbuterol have a 17% lower mean exposure to (R)-albuterol.
Metabolism and Elimination
Information available in the published literature suggests that the primary enzyme responsible for the metabolism of albuterol enantiomers in humans is SULT1A3 (sulfotransferase). When racemic albuterol was administered either intravenously or via inhalation after oral charcoal administration, there was a 3- to 4-fold difference in the area under the concentration-time curves between the (R)- and (S)-albuterol enantiomers, with (S)-albuterol concentrations being consistently higher. However, without charcoal pretreatment, after either oral or inhalation administration the differences were 8- to 24-fold, suggesting that (R)-albuterol is preferentially metabolized in the gastrointestinal tract, presumably by SULT1A3.
The primary route of elimination of albuterol enantiomers is through renal excretion (80% to 100%) of either the parent compound or the primary metabolite. Less than 20% of the drug is detected in the feces. Following intravenous administration of racemic albuterol, between 25% and 46% of the (R)-albuterol fraction of the dose was excreted as unchanged (R)-albuterol in the urine.
Special Populations
Hepatic Impairment
The effect of hepatic impairment on the pharmacokinetics of XOPENEX HFA has not been evaluated.
Renal Impairment
The effect of renal impairment on the pharmacokinetics of racemic albuterol was evaluated in 5 subjects with creatinine clearance of 7 to 53 mL/min, and the results were compared with those from healthy volunteers. Renal disease had no effect on the half-life, but there was a 67% decline in racemic albuterol clearance. Caution should be used when administering high doses of XOPENEX HFA to patients with renal impairment [see Use in Specific Populations (8.6)].
13. Nonclinical Toxicology
13.1 CARCINOGENESIS & MUTAGENESIS & IMPAIRMENT OF FERTILITY
Although there have been no carcinogenesis studies with levalbuterol tartrate, racemic albuterol sulfate has been evaluated for its carcinogenic potential.
In a 2-year study in Sprague-Dawley rats, dietary administration of racemic albuterol sulfate resulted in a significant dose-related increase in the incidence of benign leiomyomas of the mesovarium at doses of 2 mg/kg/day and greater (approximately 30 times the MRHDID) of levalbuterol tartrate for adults and approximately 15 times the MRHDID of levalbuterol tartrate for children on a mg/m2 basis). In an 18-month study in CD-1 mice and a 22-month study in the golden hamster, dietary administration of racemic albuterol sulfate showed no evidence of tumorigenicity. Dietary doses in CD-1 mice were up to 500 mg/kg/day (approximately 3800 times the MRHDID of levalbuterol tartrate for adults and approximately 1800 times the MRHDID of levalbuterol tartrate for children on a mg/m2 basis) and doses in the golden hamster study were up to 50 mg/kg/day (approximately 500 times the MRHDID of levalbuterol tartrate for adults on a mg/m2 basis and approximately 240 times the MRHDID of levalbuterol tartrate for children on a mg/m2 basis).
Levalbuterol HCl was not mutagenic in the Ames test or the CHO/HPRT Mammalian Forward Gene Mutation Assay. Levalbuterol HCl was not clastogenic in the in vivo micronucleus test in mouse bone marrow. Racemic albuterol sulfate was not clastogenic in an in vitro chromosomal aberration assay in CHO cell cultures.
No fertility studies have been conducted with levalbuterol tartrate. Reproduction studies in rats using racemic albuterol sulfate demonstrated no evidence of impaired fertility at oral doses up to 50 mg/kg/day (approximately 750 times the MRHDID of levalbuterol tartrate for adults on a mg/m2 basis).
13.2 ANIMAL PHARMACOLOGY & OR TOXICOLOGY
In animals and humans, propellant HFA-134a was found to be rapidly absorbed and rapidly eliminated, with an elimination half-life of 3 to 27 minutes in animals and 5 to 7 minutes in humans. Time to maximum plasma concentration (tmax) and mean residence time are both extremely short, leading to a transient appearance of HFA-134a in the blood with no evidence of accumulation. Based on studies in animals, the propellant HFA-134a had no detectable toxicological activity at amounts less than 380 times the maximum human exposure based on comparisons of AUC values. The toxicological effects observed at these very high doses included ataxia, tremors, dyspnea, or salivation, similar to effects produced by the structurally-related chlorofluorocarbons (CFCs) used in metered-dose inhalers, that were extensively used in the past.
14. Clinical Studies
14.1 Bronchospasm Associated with Asthma
Adults and Adolescent Patients 12 Years of Age and Older
The efficacy and safety of XOPENEX HFA were established in two 8-week, multicenter, randomized, double-blind, active- and placebo-controlled trials in 748 adults and adolescents with asthma between the ages of 12 and 81 years. In these two trials, XOPENEX HFA (403 patients) was compared to an HFA-134a placebo MDI (166 patients), and the trials included a marketed albuterol HFA-134a MDI (179 patients) as an active control. Serial forced expiratory volume in 1 second (FEV1) measurements demonstrated that 90 mcg (2 inhalations) of XOPENEX HFA produced significantly greater improvement in FEV1 over the pretreatment value than placebo. The results from one of the trials are shown in Figure 1 as the mean percent change in FEV1 from test-day baseline at Day 1 (n=445) and Day 56 (n=387). The results from the second trial were similar.
Figure 1: Percent Change in FEV1
from Test-Day Baseline in Adults and Adolescents Aged 12 to 81 Years at Day 1 and Day 56
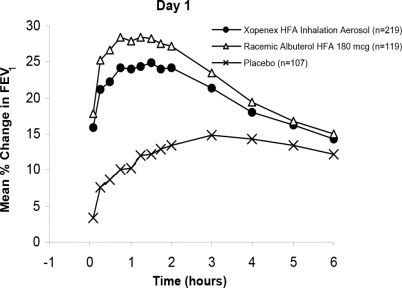
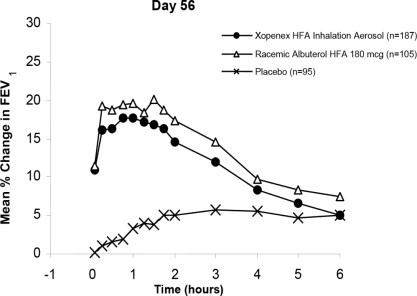
For XOPENEX HFA on Day 1, the median time to onset of a 15% increase in FEV1 ranged from 5.5 to 10.2 minutes and the median time to peak effect ranged from 76 to 78 minutes. In the responder population, on Day 1 the median duration of effect as measured by a 15% increase in FEV1 was 3 to 4 hours, with duration of effect in some patients of up to 6 hours.
Pediatric Patients 4 to 11 Years of Age
The efficacy and safety of XOPENEX HFA in children were established in a 4-week, multicenter, randomized, double-blind, active- and placebo-controlled trial in 150 pediatric patients with asthma between the ages of 4 and 11 years. In this trial, XOPENEX HFA (76 patients) was compared to a placebo HFA-134a MDI (35 patients), and the trial included a marketed albuterol HFA-134a MDI (39 patients) as an active control. Serial FEV1 measurements demonstrated that 90 mcg (2 inhalations) of XOPENEX HFA produced significantly greater improvement in FEV1 over the pretreatment value than placebo and were consistent with the efficacy findings in the adult studies.
For XOPENEX HFA, on Day 1 the median time to onset of a 15% increase in FEV1 was 4.5 minutes and the median time to peak effect was 77 minutes. In the responder population, the median duration of effect as measured by a 15% increase in FEV1 was 3 hours, with a duration of effect in some pediatric patients of up to 6 hours.
16. How is Xopenex HFA supplied
XOPENEX HFA inhalation aerosol is supplied as a pressurized aluminum canister in a box:
- NDC 27437-056-01: Canister labeled with a net weight of 15 grams containing 200 metered actuations (or inhalations)
Each canister is fitted with a dose indicator and is supplied with a blue plastic actuator mouthpiece, a red mouthpiece cap, and patient's instructions.
Shake well before using. Store between 20° and 25°C (68° and 77°F; see USP controlled room temperature). Protect from freezing temperatures and direct sunlight. Store inhaler with the actuator mouthpiece down.
Contents under pressure
Do not puncture or incinerate. Do not store near heat or open flame. Exposure to temperatures above 120°F may cause bursting. Never throw container into fire or incinerator. Keep out of reach of children
The blue actuator supplied with XOPENEX HFA should not be used with any other product canisters. Actuators from other products should not be used with a XOPENEX HFA canister. The correct amount of medication in each actuation cannot be assured after 200 actuations, even though the canister is not completely empty. When the dose indicator display window shows a red zone, approximately 20 inhalations are left, and a refill is required. The canister should be discarded when the dose indicator display window shows zero, indicating that 200 actuations have been used.
17. Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Patient Information and Instructions for Use).
Patients should be given the following information:
Frequency of Use
The action of XOPENEX HFA should last for 4 to 6 hours. Do not use XOPENEX HFA more frequently than recommended. Instruct patients to not increase the dose or frequency of doses of XOPENEX HFA without consulting their physician. If patients find that treatment with XOPENEX HFA becomes less effective for symptomatic relief, symptoms become worse, or they need to use the product more frequently than usual, they should seek medical attention immediately.
Priming, Cleaning and Storage
Priming: SHAKE WELL BEFORE USING. Patients should be instructed that priming XOPENEX HFA is essential to ensure appropriate levalbuterol content in each actuation. Patients should prime XOPENEX HFA before using for the first time and in cases where the inhaler has not been used for more than 3 days by releasing 4 test sprays into the air, away from the face.
Cleaning: To ensure proper dosing and prevent actuator orifice blockage, instruct patients to wash the actuator in warm water and air-dry thoroughly at least once a week. Patients should be informed that detailed cleaning instructions are included in the FDA-approved patient labeling.
Storage: Store canister between 20° and 25°C (68° and 77°F). Protect from freezing temperatures and direct sunlight.
Paradoxical Bronchospasm
Inform patients that XOPENEX HFA can produce paradoxical bronchospasm. Instruct patients to discontinue XOPENEX HFA if paradoxical bronchospasm occurs.
Concomitant Drug Use
While patients are using XOPENEX HFA, other inhaled drugs and asthma medications should be taken only as directed by the physician.
Common Adverse Reactions
Common adverse effects of treatment with inhaled beta-agonists include palpitations, chest pain, rapid heart rate, tremor, and nervousness.
Pregnancy
Patients who are pregnant or nursing should contact their physicians about the use of XOPENEX HFA.
General Information on Use
Effective and safe use of XOPENEX HFA includes an understanding of the way that it should be administered.
Shake the inhaler well immediately before each use.
Use XOPENEX HFA only with the actuator supplied with the product. When the dose indicator display window shows a red zone, approximately 20 inhalations are left, and a refill is required. Discard the inhaler when the dose indicator display window shows zero, indicating that 200 sprays have been used. Never immerse the canister in water to determine how full the canister is ("float test").
In general, the technique for administering XOPENEX HFA to children is similar to that for adults. Children should use XOPENEX HFA under adult supervision, as instructed by the patient's physician [advise the patient to read the FDA-approved patient labeling – (Patient Information and Instructions for Use)].
LUPIN®
Manufactured for and Distributed by:
Lupin Pharmaceuticals, Inc.
Naples, FL 34108
© 2005, 2012, 2024 Lupin Inc.
All rights reserved. XOPENEX HFA is a registered trademark of Lupin Inc.
and LUPIN is a registered trademark of Lupin Pharmaceuticals, Inc.
To report adverse events, call 1-800-399-2561.
For patent information: https://www.lupin.com/US/specialty/patent-information/
Revised August 2024
3200001065
PATIENT PACKAGE INSERT
| PATIENT INFORMATION
XOPENEX HFA® (zō-pen-eks hfa) (levalbuterol tartrate) inhalation aerosol, for oral inhalation use |
|||||
What is XOPENEX HFA?
|
|||||
Do not use XOPENEX HFA if you:
|
|||||
Before you use XOPENEX HFA, tell your doctor about all of your medical conditions, including if you:
|
|||||
| Tell your doctor about all the medicines you take , including prescription and over-the-counter medicines, vitamins, and herbal supplements. XOPENEX HFA may affect the way other medicines work, and other medicines may affect how XOPENEX HFA works. Especially tell your doctor if you take:
|
|||||
| Know the medicines you take. Keep a list of them to show your doctor and pharmacist when you get a new medicine. |
|||||
How should I use XOPENEX HFA?
o your asthma symptoms get worse o you need to use XOPENEX HFA more often than usual
|
|||||
| What are the possible side effects of XOPENEX HFA?
XOPENEX HFA can cause serious side effects including:
|
|||||
| o swelling of the face, throat or tongue o hives | o rash o breathing problems |
||||
|
|||||
| Call your doctor or go to the nearest hospital emergency room right away if you have any of the serious side effects listed above or if you have worsening lung symptoms. The most common side effects of XOPENEX HFA include: |
|||||
|
|
|
|||
| These are not all the possible side effects of XOPENEX HFA. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. You may also report side effects to Lupin Pharmaceuticals, Inc. at 1-800-399-2561. |
|||||
How should I store XOPENEX HFA?
|
|||||
| Keep XOPENEX HFA and all medicines out of the reach of children.
|
|||||
| General information about the safe and effective use of XOPENEX HFA
Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. Do not use XOPENEX HFA for a condition for which it was not prescribed. Do not give XOPENEX HFA to other people, even if they have the same symptoms that you have. It may harm them. You can ask your pharmacist or doctor for information about XOPENEX HFA that is written for health professionals. |
|||||
| What are the ingredients in XOPENEX HFA?
Active ingredient : levalbuterol tartrate Inactive ingredients : propellant HFA-134a, Dehydrated Alcohol USP, Oleic Acid NF |
|||||
INSTRUCTIONS FOR USE
(zō-pen-eks hfa)
(levalbuterol tartrate)
inhalation aerosol, for oral inhalation use
Important Information:
- For oral inhalation use only
- Use XOPENEX HFA exactly as your doctor tells you to.
- If you have any questions about the use of your inhaler, ask your doctor or pharmacist.
The parts of your XOPENEX HFA inhaler (See Figure 1):
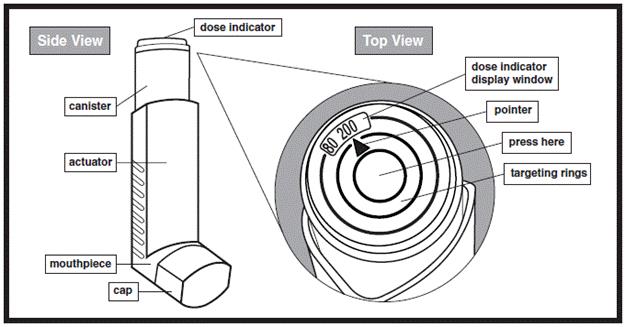
- XOPENEX HFA comes as a canister that fits into an actuator with a dose indicator.
- Do not use the XOPENEX HFA actuator with a canister of medicine from any other inhaler.
- Do not use the XOPENEX HFA canister with an actuator from any other inhaler.
- The dose indicator display window will show you how many sprays of medicine you have left in your inhaler. A spray of medicine is released each time you press down on the center of the dose indicator.
- It is important that you pay attention to the number of sprays left in your XOPENEX HFA inhaler by reading the dose indicator. You should also keep track of the number of sprays used from your inhaler.
Each canister of XOPENEX HFA contains enough medicine for you to spray your medicine 200 times (See Figure 2a).
- The pointer will be pointing between 180 and 200 after you take 10 sprays. This means that there are 190 sprays of medicine left in the canister (See Figure 2b).
- The pointer will be pointing to 180 after you take 10 more sprays. This means that there are 180 sprays of medicine left in the canister (See Figure 2c).
 |
 |
 |
| Figure 2a
| Figure 2b
| Figure 2c
|
| 200 sprays | 190 sprays | 180 sprays |
- The dose indicator display window will continue to move after every 10 sprays. The number on the dose indicator display window will continue to change after every 20 sprays.
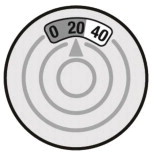
- The dose indicator display window will change to red, as shown in the shaded area, when there are only 20 sprays of medicine left in your inhaler (See Figure 2d). You should refill your prescription or ask your doctor if you need another prescription for XOPENEX HFA.
- When the number in the dose indicator display window reaches zero "0", this means that 200 sprays of medicine have been used. Throw away your XOPENEX HFA inhaler.
Note: Do not place the canister under water to find out the amount of medicine left in the canister.
Preparing your XOPENEX HFA inhaler for use:
- Your XOPENEX HFA inhaler should be at room temperature before you use it.
- Shake the inhaler well before each use.
Priming your XOPENEX HFA inhaler:
Before you use XOPENEX HFA for the first time or if you have not taken your medicine for 3 days in a row, you must prime the inhaler.
- Look at the dose indicator on top of the inhaler. Make sure that the pointer on the dose indicator is pointing to the "200" inhalation mark before you use your XOPENEX HFA inhaler for the first time.
- Take the cap off the mouthpiece of the actuator (See Figure 3). Check inside the mouthpiece for objects before use.
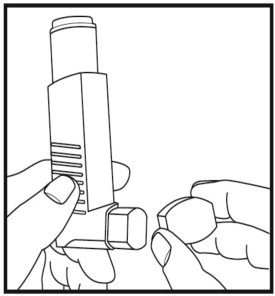
- Hold the inhaler in the upright position away from the face and shake the inhaler well (See Figure 4).
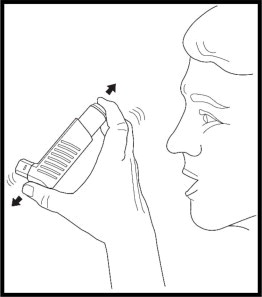
- Press down fully on the center of the dose indicator to release a spray of medicine from the mouthpiece (See Figure 5). You may hear a soft click from the dose indicator as it counts down during use.
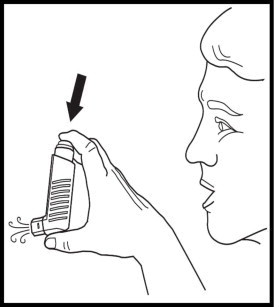
- Avoid spraying in your eyes.
- Repeat the priming steps 3 more times (See Figure 4 and Figure 5) to finish priming the inhaler.
- After priming 4 times the first time you use your XOPENEX HFA inhaler, the dose indicator should be pointing to "200" and your inhaler is now ready to use.
If you do not use your XOPENEX HFA inhaler for more than 3 days, you will need to prime the inhaler again before use.
Using your XOPENEX HFA inhaler:
Step 1: Take the cap off the mouthpiece of the actuator (See Figure 3). Check inside the mouthpiece for objects. Make sure the canister fits firmly in the actuator.
Step 2: Shake the inhaler well for 5 seconds before use.
Step 3: Hold the inhaler upright with the mouthpiece pointing towards you. Before you put the mouthpiece in your mouth, breathe out through your mouth and push out as much air from your lungs as you can (See Figure 6).
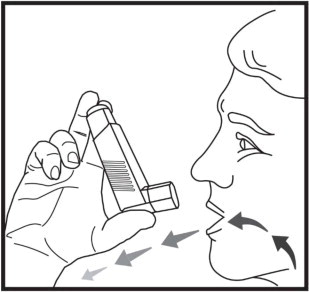
Step 4: Put the mouthpiece in your mouth and close your lips around it.
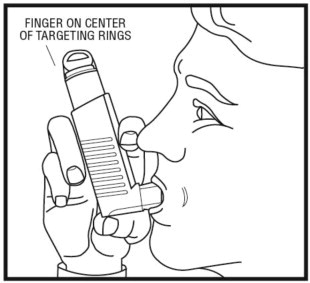
Step 5: While breathing in deeply and slowly, press down on the center of the targeting rings (See Figure 7) until a spray of medicine has been released. Then stop pressing the dose indicator.
Step 6: When you have finished breathing in, remove the mouthpiece from your mouth. Close your mouth and hold your breath for 10 seconds if possible. Then breathe out gently.
.
Step 7: Wait about 1 minute, then shake the inhaler well. Repeat steps 3 through 6 to take your second spray of XOPENEX HFA.
Step 8: Put the cap back on the mouthpiece right away after use.
Make sure the cap snaps firmly into place.
Cleaning your XOPENEX HFA inhaler:
Clean the inhaler 1 time each week. It is very important to keep the actuator clean so that medicine will not build up and block the spray from the mouthpiece (See Figure 8).
To clean the actuator:
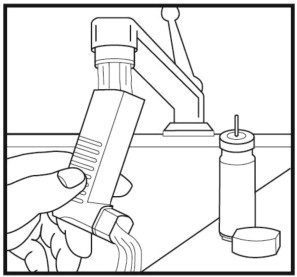
Step 1: Take the canister out of the actuator (See Figure 9). Do not clean the canister or let it get wet.
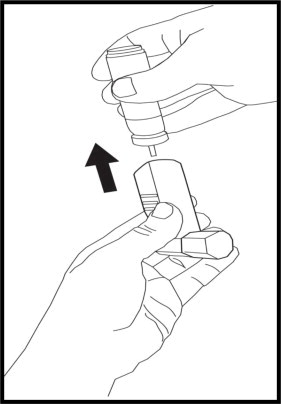
Step 2: Take the cap off the mouthpiece.
Step 3: Hold the actuator under the faucet and run warm water through it for at least 30 seconds. Turn the actuator upside down and rinse the actuator again through the mouthpiece for at least 30 seconds (See Figure 10).
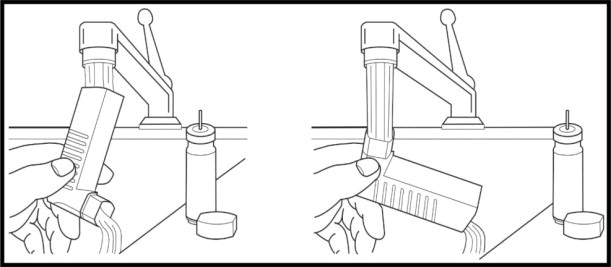
Step 4: Shake off as much water from the actuator as you can.
Step 5: Look inside the actuator and mouthpiece to make sure any medicine build-up has been completely washed away. Medicine build-up is more likely to happen if the actuator is not allowed to air-dry completely.
Step 6: Let the actuator air-dry overnight. Do not put the canister back into the actuator if it is still wet.
Step 7: When the actuator is dry, put the canister back in the actuator and put the cap back on the mouthpiece. Make sure to firmly press the canister down in the actuator.
Note: If your actuator becomes blocked, it means that little or no medicine is coming out of the mouthpiece (See Figure 11). Repeat Steps 1 through 7 above in the section "To clean the actuator".
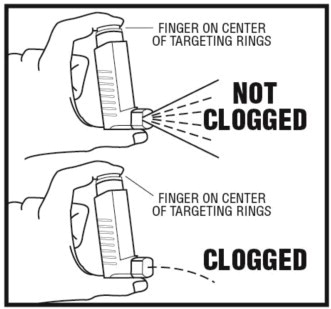
If you need to use your inhaler before the plastic actuator is completely dry:
- Shake off as much water from the actuator as you can.
- Put the canister back into the actuator and shake the inhaler well.
- To remove most of the water from your inhaler, press down on the center of the targeting rings 2 times to release a total of 2 sprays into the air away from your face.
- Take your prescribed dose of medicine.
- Repeat Steps 1 through 7above in the section "To clean the actuator".
How should I store XOPENEX HFA?
- Store XOPENEX HFA at room temperature between 68°F to 77°F (20°C to 25°C).
- Do not use or store XOPENEX HFA inhaler near heat or open flame. Temperatures above 120°F may cause the canister to burst.
- Do not freeze XOPENEX HFA.
- Keep XOPENEX HFA out of direct sunlight.
- Do not put a hole in the XOPENEX HFA canister.
- Store XOPENEX HFA with the mouthpiece down.
- Throw away XOPENEX HFA when the dose indicator display window reaches zero "0", showing that all 200 sprays (actuations) have been used.
- Do not throw XOPENEX HFA into a fire or incinerator.
Keep XOPENEX HFA and all medicines out of the reach of children.
© 2005, 2012, 2024 Lupin Inc. All rights reserved
XOPENEX HFA is a registered trademark of Lupin Inc.
and LUPIN is a registered trademark of Lupin Pharmaceuticals, Inc.
This Patient Information and Instructions for Use has been approved by the U.S. Food and Drug Administration.
LUPIN®
Manufactured for and Distributed by:
Lupin Pharmaceuticals, Inc.
Naples, FL 34108
To report adverse events, call 1-800-399-2561.
For patent information: https://www.lupin.com/US/specialty/patent-information/
Revised August 2024
3200001065
PACKAGE LABEL.PRINCIPAL DISPLAY PANEL
PRINCIPAL DISPLAY PANEL – TRADE CARTON - 45 MCG 200 ACTUATIONS
NDC 27437-056-01 Net Contents: 15g
Xopenex HFA®
(levalbuterol tartrate)
Inhalation Aerosol
45 mcg/actuation
200 Metered Inhalations
FOR ORAL INHALATION WITH Xopenex HFA® ACTUATOR ONLY
Shake well before using.
Rx only
LUPIN®

PACKAGE LABEL.PRINCIPAL DISPLAY PANEL
PRINCIPAL DISPLAY PANEL – TRADE CARTON - 45 MCG 200 ACTUATIONS
NDC 27437-056-01 Net Contents: 15g
Xopenex HFA®
(levalbuterol tartrate)
Inhalation Aerosol
45 mcg/actuation
200 Metered Inhalations
FOR ORAL INHALATION WITH Xopenex HFA® ACTUATOR ONLY
Shake well before using.
Rx only
LUPIN®

| XOPENEX HFA
levalbuterol tartrate aerosol, metered |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| Labeler - Lupin Pharmaceuticals, Inc. (089153071) |
Frequently asked questions
More about Xopenex HFA (levalbuterol)
- Check interactions
- Compare alternatives
- Pricing & coupons
- Reviews (5)
- Side effects
- Dosage information
- During pregnancy
- Drug class: adrenergic bronchodilators
- Breastfeeding
- En español
