Dry eye syndrome
Medically reviewed by Drugs.com. Last updated on Oct 25, 2023.
What is dry eye syndrome?

Dry eye syndrome occurs when there is an inadequate quantity or quality of tear production to moisten, protect and cleanse the eyes. Dry eye syndrome is one of the most common eye problems. And it becomes more common as people age because tear production can diminish as part of the aging process.
More women are affected than men. And the syndrome is more likely to flare up at times of hormonal change such as after menopause or during pregnancy or breastfeeding. Birth control pills can trigger dry eye syndrome, and so can many other medications, including antidepressants, antihistamines, decongestants, antianxiety agents and diuretics or other blood pressure pills. Some medicines that are used in the eye also can cause dry eyes as an allergic reaction.
Several autoimmune disorders also can affect the body's ability to produce tears normally, including Sjögren's syndrome, rheumatoid arthritis and myasthenia gravis, as well as other conditions such as Bell's palsy and thyroid dysfunction.
Symptoms of dry eye syndrome
Dry eye syndrome can cause:
- burning or itchy eyes
- a feeling of something gritty, like sand, in the eyes
- sensitivity to light
- difficulty wearing contact lenses
- excessive tearing.
Excessive tearing may seem to be an unusual symptom for dry eye syndrome. But these are called irritant tears, and are produced as a reflex reaction to the syndrome. They contain more water than normal tears, which have a balance of water, fat and mucus. Therefore, the excess tears just run off the eyes and cannot lubricate them as well as healthy tears do.
Diagnosing dry eye syndrome
After speaking with you about your eye symptoms and general health, including past medical problems, your doctor may suspect that you have dry eye syndrome. A complete physical examination, and sometimes, certain blood tests may help to determine whether you also have an autoimmune disorder. Your doctor may refer you to an optometrist or ophthalmologist so your eyes can be evaluated more completely for:
- dry spots on the cornea, revealed by putting a stain in the eye
- abnormal tear quality, as determined by analysis of the tears and their stability on the surface of the eye
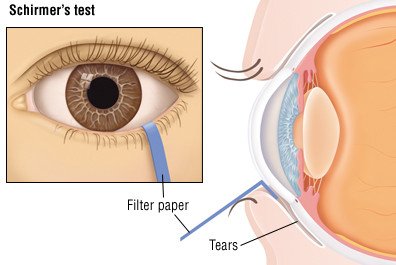
- insufficient tear production, measured by a procedure called Schirmer's test, in which a filter paper is placed inside the lower lid and, after five minutes, the amount of moisture in the paper is measured.
|
|
Expected duration of dry eye syndrome
Dryness of the eyes may be brief if it is related to a medication, hormonal fluctuation or other reversible condition. However, if it is related to an autoimmune condition, it may be chronic (longer lasting).
Preventing dry eye syndrome
To reduce your chances of developing dry eyes, try the following:
- Reduce your exposure to some of the conditions that can cause or aggravate the condition, including wind, smoke, chemical vapors, dry heat, hair dryers and air conditioning.
- Use a humidifier indoors.
- Stop wearing contact lenses if you have any dry eye symptoms.
- To avoid the diminished blinking that can make symptoms worse, take regular breaks if you spend long hours at a computer screen or doing close work.
Pay particular attention to these precautions if you have a medical condition or take a medication that is associated with dry eye syndrome. Sometimes, changing your medication may help, though this should be done only with your doctor's supervision. If your symptoms are severe, you can protect your eyes from dry air during outdoor activities by wearing swim or ski goggles or other protective eyewear to retain moisture around the eyes.
Drugs used to treat this and similar conditions
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Treating dry eye syndrome
The two most common methods of treatment are to replace tears or to conserve them. In most cases, you can use artificial tears, which mimic the composition of natural tears, and are available over the counter. Lubricating ointments can be used for more severe cases, but they tend to blur vision and so should be applied at bedtime.
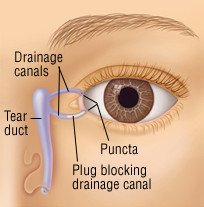
If these do not relieve the symptoms, your doctor may try to conserve tears by plugging the tear drain holes, called puncta, with tiny plugs made of collagen or silicone. In the worst cases, the holes can be closed permanently using electric cauterization.
|
|
If these treatments are not effective, another approach is to increase tear production by using topical drugs, including cyclosporine. Topical cyclosporine (Restasis) decreases inflammation in the tear-producing glands and that may lead to better tear production. Another topical treatment, lifitegrast (Xiidra) was approved by the FDA in 2016. It is thought to block the action of key immune cells and their chemical messengers involved in eye inflammation that leads to dryness. A nasal spray, varenicline, can increase tear production and reduce symptoms of dry eye disease. It was approved by the FDA for this condition in 2021.
Special contact lenses can help maintain tears over the eye but they are expensive and the fitting process is complicated. As a result, these lenses are not a common treatment.
Limited research suggests that other potentially effective treatments for dry eye syndrome include:
- oral antioxidant supplements
- topical vitamin A
- sodium hyaluronate applied to the eye
- topical glucocorticoids (although only for short term use and under the supervision of an ophthalmologist given the potential for significant side effects)
- omega-3 and omega-6 fatty acids
- acupuncture.
Humidifiers, wet compresses and glasses that protect the eyes from dry air (such as wrap-around sunglasses, goggles or glasses fitted with "shields" on the sides) also can help.
When to call a professional
Call your doctor if your symptoms last more than a few days. Consult a doctor before beginning treatment with over-the-counter artificial tears.
Prognosis
For most cases, the outlook is good because the condition is more of an annoyance than a danger to your health or your eyes. Symptoms often go away quickly if you remove contact lenses or change your medications or your environment. Even when symptoms persist, they usually can be controlled.
Additional info
National Eye Institute
https://www.nei.nih.gov/
American College of Rheumatology
https://www.rheumatology.org/
Arthritis Foundation
https://www.arthritis.org/
Learn more about Dry eye syndrome
Treatment options
Care guides
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.