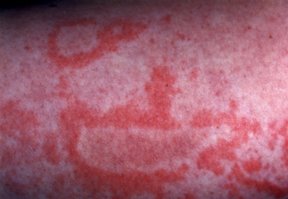
Hives (urticaria)
Medically reviewed by Drugs.com. Last updated on Sep 24, 2024.
What are hives?

Hives, also called urticaria, are circumscribed swellings on the skin that often are itchy. Often they are pink or red, but they don't have to be. Hives happen when the cells in the skin called mast cells release histamine, a chemical that causes tiny blood vessels (capillaries) to leak fluid. When this leaking fluid accumulates in the skin, it forms the swellings that we recognize as hives.
Hives can be triggered by physical factors such as heat, cold, exercise, sunlight, stress, sustained pressure on a skin area (such as from a belt or shoulder strap), a sudden increase in body temperature (from a fever or a hot bath or shower) or from an irritating chemical, cosmetic or soap applied to the skin. Hives also can be one symptom of a whole-body (systemic) allergic reaction to something that was:
- inhaled — pollens, animal dander, molds
- injected — insect stings or bites, especially bee stings, or injected medication
- ingested — foods (tree nuts; fish and shellfish; dairy products; legumes, especially peanuts), food additives, medications such as penicillin or aspirin.
Hives probably affect about 20% of people in the United States at some time in life, with the greatest number of episodes occurring in people aged 20 to 30. In rare cases, allergic reactions that trigger hives set off a chain reaction throughout the body, resulting in a life-threatening condition called anaphylaxis. Sometimes, hives last for six weeks or more, a condition called chronic (or idiopathic) urticaria. Often, no cause is found for this chronic condition, and it usually goes away on its own after several weeks.
Symptoms of hives
Hives appear as "wheals" (swellings) on the skin, sometimes pink or red and surrounded by a red blotch. Typically round or oval, hives often itch. Hives vary in size, and some may blend to form larger areas of swelling. Hives can affect skin on any area of the body, especially the trunk, thighs, upper arms and face. Most individual hives fade quickly, but new crops may appear every 24 to 72 hours if the person continues to be exposed to the environment or substance that triggered the hives.
|
|
If hives are an early sign of a whole-body reaction, other symptoms to look for include swelling of the tongue, lips or face; wheezing; dizziness; chest tightness; and breathing difficulties. If these symptoms occur, get immediate medical attention. You could be developing anaphylaxis, a life-threatening condition.
Diagnosing hives
Your doctor will ask about your history of allergic reactions, and about your recent exposure to pets, plants, insects or new foods or medications. During a physical examination, your doctor usually can distinguish between hives and other types of skin rashes. Also, he or she will check for other signs of a serious allergic reaction.
If the condition occurs frequently, your doctor may order blood tests or perform skin testing for allergies. If your doctor suspects that you are undergoing anaphylaxis, he or she will begin treatment immediately and closely monitor your blood pressure and breathing.
Expected duration of hives
Individual hives usually fade within eight to 12 hours, but recurrent hives can continue to reappear for weeks or months. In cases of chronic urticaria (hives), the condition may last for six months or more.
Preventing hives
You can prevent hives by identifying and avoiding the particular circumstance or substance that triggered your skin reaction. If your doctor determines that you are allergic to insect venom, you may be advised to keep an epinephrine kit for emergency injections to prevent anaphylaxis. Keep the medicine in a convenient place if you work outside or play a sport. Keep an antihistamine in your medicine cabinet and take it the first signs of hives or itching. Older adults and people with heart disease should double check with their doctor before taking antihistamines.
Drugs used to treat this and similar conditions
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Treating hives
To relieve most uncomplicated episodes of hives, your doctor may suggest a lotion such as Sarna or an antihistamine, such as cetirizine (Zyrtec, others) or loratadine (Claritin, others). There are many over-the-counter antihistamines available. Generic versions work as well as the brand name drugs. It is critical to relieve the itching because scratching can stimulate more hives and itching.
If these medications are not effective, you may be given a prescription medication such as cyproheptadine (Periactin) hydroxyzine (Atarax or Vistaril) or desloratadine (Clarinex).
For cases that are even more resistant to treatment, H2 receptor blockers might be added. These include nizatidine (Axid), famotidine (Pepcid) or cimetidine (Tagamet). Doxepin (Adapin, Sinequan) before bed is particularly helpful for people having a difficulty sleeping because of the itching.
When other options fail, medications that suppress or alter the immune system may be prescribed. These include omalizumab (Xolair), montelukast (Singulair), zafirlukast (Accolate) or corticosteroids (such as prednisone).
When to call a professional
Call your doctor immediately if hives appear after you have started taking a new medication or after you have been stung by an insect. Get emergency treatment if hives occur with wheezing, dizziness, chest tightness, breathing difficulties or swelling of the tongue, lips or face.
Prognosis
Most simple cases of hives fade quickly, and the affected skin returns to normal within hours. Even when you have episodes that recur over several weeks, without a known cause, they often stop coming back after a few months. Consult your doctor if hives persist for several days or if itching interferes with your ability to sleep or perform normal daily activities.
Additional info
American Academy of Allergy, Asthma, and Immunology (AAAAI)
https://www.aaaai.org/
American Academy of Dermatology
https://www.aad.org/
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.