Urticaria
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is urticaria?
Urticaria is also called hives. Hives can change size and shape, and appear anywhere on your skin. They can be mild or severe and last from a few minutes to a few days. Hives may be a sign of a severe allergic reaction called anaphylaxis that needs immediate treatment. Urticaria that lasts longer than 6 weeks may be a chronic condition that needs long-term treatment.
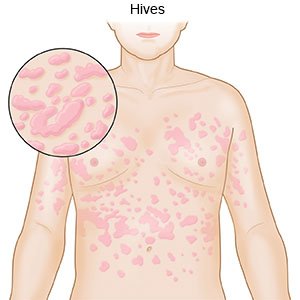 |
What causes urticaria?
Hives are caused by an immune system reaction. The following are common triggers:
- Food allergies, such as to nuts, eggs, or shellfish
- Food dyes, additives, or preservatives
- Medicine allergies, such as to ibuprofen or antibiotics
- Infections, such as a cold or mono
- Bug bites
- Pets, plants, or latex
- Stress
How is the cause of urticaria diagnosed?
Your healthcare provider will examine you and ask about your symptoms. He or she may also ask about your family medical history, medicines you take, and foods you eat. Tell your provider about any recent trauma, stress, or contact with allergens. You may need additional testing if you developed anaphylaxis after you were exposed to a trigger and then exercised. This is called exercise-induced anaphylaxis. You may need any of the following:
- A skin test is used to see how your skin reacts to possible triggers. Your provider will put a small amount of the trigger onto your skin. He or she will cover the area with a patch that stays on for 2 days. Then he or she will check your skin for a reaction.
- A challenge test is used to give you increasing doses of what may be causing your hives. Your provider will watch for a reaction.
How is urticaria treated?
Hives often go away without treatment. Chronic urticaria may need to be treated with more than one medicine, or other medicines than listed below. The following are common medicines used to treat urticaria:
- Antihistamines decrease mild symptoms such as itching or a rash.
- Steroids decrease redness, pain, and swelling.
- Epinephrine is used to treat severe allergic reactions such as anaphylaxis.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
What steps do I need to take for signs or symptoms of anaphylaxis?
- Immediately give 1 shot of epinephrine only into the outer thigh muscle.
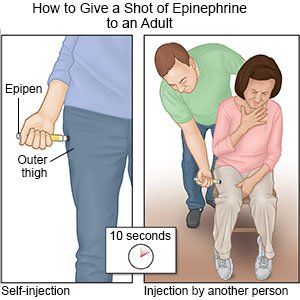
- Leave the shot in place as directed. Your provider may recommend you leave it in place for up to 10 seconds before you remove it. This helps make sure all of the epinephrine is delivered.
- Call 911 and go to the emergency department, even if the shot improved symptoms. Do not drive yourself. Bring the used epinephrine shot with you.
Related medications
What safety precautions do I need to take if I am at risk for anaphylaxis?
- Keep 2 shots of epinephrine with you at all times. You may need a second shot, because epinephrine only works for about 20 minutes and symptoms may return. Your provider can show you and family members how to give the shot. Check the expiration date every month and replace it before it expires.
- Create an action plan. Your provider can help you create a written plan that explains the allergy and an emergency plan to treat a reaction. The plan explains when to give a second epinephrine shot if symptoms return or do not improve after the first. Give copies of the action plan and emergency instructions to family members, work and school staff, and daycare providers. Show them how to give a shot of epinephrine.
- Be careful when you exercise. If you have had exercise-induced anaphylaxis, do not exercise right after you eat. Stop exercising right away if you start to develop any signs or symptoms of anaphylaxis. You may first feel tired, warm, or have itchy skin. Hives, swelling, and severe breathing problems may develop if you continue to exercise.
- Carry medical alert identification. Wear medical alert jewelry or carry a card that explains the allergy. Ask your provider where to get these items.
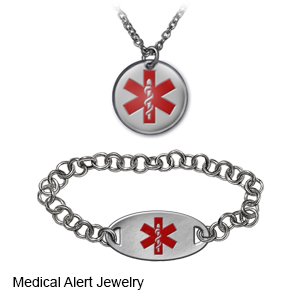
- Keep a record of triggers and symptoms. Record everything you eat, drink, or apply to your skin for 3 weeks. Include stressful events and what you were doing right before your hives started. Bring the record with you to follow-up visits with your provider.
What can I do to manage urticaria?
- Cool your skin. This may help decrease itching. Apply a cool pack to your hives. Dip a hand towel in cool water, wring it out, and place it on your hives. You may also soak your skin in a cool oatmeal bath.
- Do not rub your hives. This can irritate your skin and cause more hives.
- Wear loose clothing. Tight clothes may irritate your skin and cause more hives.
- Manage stress. Stress may trigger hives, or make them worse. Learn new ways to relax, such as deep breathing.
Call your local emergency number (911 in the US) for signs or symptoms of anaphylaxis,
such as trouble breathing, swelling in your mouth or throat, or wheezing. You may also have itching, a rash, or feel like you are going to faint.
When should I seek immediate care?
- Your heart is beating faster than it normally does.
- You have cramping or severe pain in your abdomen.
When should I call my doctor?
- You have a fever.
- Your skin still itches 24 hours after you take your medicine.
- You still have hives after 7 days.
- Your joints are painful and swollen.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Urticaria
Treatment options
Care guides
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
