Latex Allergy
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is a latex allergy?
A latex allergy is an immune system reaction to the protein in rubber latex. Latex gloves and other latex products contain this protein. You may have a reaction if you touch or breathe in the protein. A latex allergy may begin as a mild skin reaction and become worse each time you are exposed. Repeated exposure to latex may lead to a severe allergy to latex and can be life-threatening.
What products contain latex?
Latex is used to make many rubber products found in homes, hospitals, schools, and the workplace. Avoid contact with products that may contain latex:
- Gloves, tape, bandages, and tourniquets
- Medical tubes, rubber injection ports, plunger tips, and medicine bottles with rubber tops
- Face masks, breathing tubes, and other respiratory equipment
- Bite blocks used during dental visits
- Certain clothing items that contain elastic, such as bras, shoes, belts, and suspenders
- Foam pillows, carpet backing, golf or tennis grips, and garden hoses
- Condoms, diaphragms, contraceptive sponges, and female sanitary pads
- Diapers, bottle nipples, and pacifiers
What increases my risk for a latex allergy?
- Exposure to latex often, such as if you are a healthcare worker, hairdresser, or work with food or fabric.
- Other allergies, such as hay fever, asthma, food allergies, or skin conditions.
- Certain health conditions, such as spina bifida. Children who had surgery before their first birthday may have an increased risk for latex allergy.
- Previous reactions, such as other severe allergies or unexpected reactions during hospitalization or surgery.
What are the signs and symptoms of a latex allergy?
You may have symptoms only where latex has touched you. You may have more severe symptoms that include areas of your body not exposed to latex. Any of the following may develop from minutes up to 48 hours after exposure to latex:
- Itching or burning skin
- Bumps, sores, blisters, or a skin rash
- Cracking, peeling, or flaking skin
- Tingling in your mouth
- Facial swelling, especially around your eyes
- Dizziness or fast heart rate
- Chest or throat tightness, wheezing, or shortness of breath
How is a latex allergy diagnosed?
Your healthcare provider will ask about other health conditions you have. He or she will ask about your signs and symptoms, and blood may be taken for tests. You may also need skin tests. Ask your healthcare provider for more information about the tests that you need.
Related medications
How is a latex allergy treated?
- Antihistamines treat the symptoms of a mild latex allergy, such as a rash or hives.
- Epinephrine is medicine used to treat severe allergic reactions such as anaphylaxis.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
What steps do I need to take for signs or symptoms of anaphylaxis?
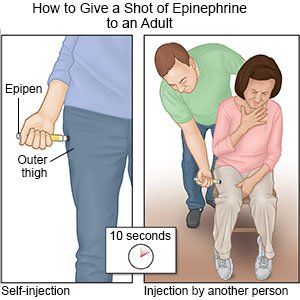
- Immediately give 1 shot of epinephrine only into the outer thigh muscle.
- Leave the shot in place as directed. Your healthcare provider may recommend you leave it in place for up to 10 seconds before you remove it. This helps make sure all of the epinephrine is delivered.
- Call your local emergency number (911 in the US), even if the shot improved symptoms. Do not drive yourself. Bring the used epinephrine shot with you.
 |
What safety precautions do I need to take if I am at risk for anaphylaxis?
- Keep 2 shots of epinephrine with you at all times. You may need a second shot, because epinephrine only works for about 20 minutes and symptoms may return. Your healthcare provider can show you and family members how to give the shot. Check the expiration date every month and replace it before it expires.
- Create an action plan. Your provider can help you create a written plan that explains the allergy and an emergency plan to treat a reaction. The plan explains when to give a second epinephrine shot if symptoms return or do not improve after the first. Give copies of the action plan and emergency instructions to family members, work and school staff, and daycare providers. Show them how to give a shot of epinephrine.
- Carry medical alert identification. Wear medical alert jewelry or carry a card that says you have a latex allergy. Ask your provider where to get these items.
- Tell all healthcare providers about your latex allergy. This includes dentists, nurses, doctors, and surgeons.
- Keep a supply of nonlatex gloves. Use vinyl or synthetic gloves if you need to wear gloves. Keep a supply of these nonlatex gloves in your house and car.
Call your local emergency number (911 in the US) if:
- You have signs or symptoms of anaphylaxis, such as the following:
- Trouble breathing
- Swelling in your mouth or throat
- Wheezing
- Skin itching, a rash, hives
- Feeling like you are going to faint
When should I seek immediate care?
- You feel warm and flushed.
- You have a fast heartbeat.
When should I call my doctor?
- Your symptoms have not gone away within 2 weeks.
- You have new symptoms that you did not have before.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Latex Allergy
- Allergies, Cough/Cold Medications and Alcohol Interactions
- Benadryl Dosage Charts for Infants and Children
- Claritin Dosage Charts for Infants and Children
- EpiPen Costs and Alternatives: What Are Your Best Options?
- Low Salicylate Diet
- Zyrtec Dosage Charts for Infants and Children
Treatment options
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
