Interstitial Cystitis
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is interstitial cystitis (IC)?
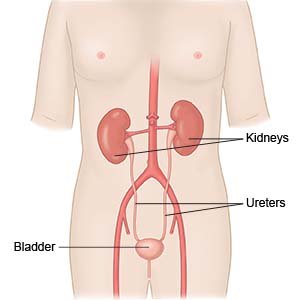
IC is a long-term condition that causes pressure and pain in your bladder and pelvic area. IC is also called bladder pain syndrome and painful bladder syndrome. The cause of IC is not known.
 |
What are other symptoms of IC?
Your symptoms may come and go. Common triggers include stress, menstrual period, sitting for a long time, or sexual activity.
- Urgent need to urinate during the day and night
- Pain with a full bladder that goes away when you urinate
- Urinating more often with smaller amounts
- Pain between the vagina and anus in women
- Pain between the scrotum and anus in men
- Pain during sex
How is IC diagnosed?
Your healthcare provider will examine you and ask about your symptoms. Tell your provider about your medical history and any medicines you take. You may need the following to rule out other causes of IC:
- Urine tests may show a urinary tract infection or abnormal cells.
- A cystoscopy is a procedure to look inside of your urethra and bladder. This test may show the size of your bladder. A sample of tissue (biopsy) may also be taken.
Related medications
How is IC treated?
The goal of treatment is to control your symptoms. You may need to try a combination of the following:
- Medicines:
- Acetaminophen decreases pain and fever. It is available without a doctor's order. Ask how much to take and how often to take it. Follow directions. Read the labels of all other medicines you are using to see if they also contain acetaminophen, or ask your doctor or pharmacist. Acetaminophen can cause liver damage if not taken correctly.
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. This medicine is available with or without a doctor's order. NSAIDs can cause stomach bleeding or kidney problems in certain people. If you take blood thinner medicine, always ask your healthcare provider if NSAIDs are safe for you. Always read the medicine label and follow directions.
- Prescription pain medicine may be given. Ask your healthcare provider how to take this medicine safely. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your healthcare provider how to prevent or treat constipation.
- Other medicines may be given to decrease symptoms, such as the need to urinate urgently or often. These medicines may be taken by mouth or placed directly into your bladder.
- Nerve stimulation helps increase blood flow to your bladder and strengthens the muscles that control your bladder. Mild electrical pulses are sent to the nerves in your bladder.
- Bladder distension is a procedure to stretch the walls of your bladder with water.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
How can I manage my symptoms?
- Keep a log. Include how much liquid you drink and how much you urinate. Bring this log to your appointments.
- Go to physical therapy. A physical therapist teaches you exercises to help improve movement and decrease pain.
- Nutrition changes may be needed. Citrus and spicy foods may irritate your bladder. Ask your healthcare provider which foods are best for you.
- Drink liquids as directed. You may need to drink extra water, or you may need to drink less. Carbonated drinks and caffeine may irritate your bladder. Ask how much liquid to drink each day and which liquids are best for you.
- Manage stress. Stress may worsen symptoms. Your healthcare provider may recommend you find ways to manage stress, such as relaxation techniques.
- Train your bladder to urinate less often. This can be done by going to the bathroom at scheduled times. Try to hold your urine when you feel the urge to go. For example, hold your urine for 5 minutes when you feel the urge to go. As that becomes easier, hold your urine for 10 minutes.
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can worsen your symptoms. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
When should I call my doctor?
- Your symptoms get worse, or you develop new symptoms.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Interstitial Cystitis
- Antibiotics For UTI Treatment - What Are My Options?
- Antibiotics and Birth Control Pill Interactions
- Can You Drink Alcohol with Antibiotics?
- Common Side Effects from Antibiotics, and Allergies and Reactions
Treatment options
Care guides
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
