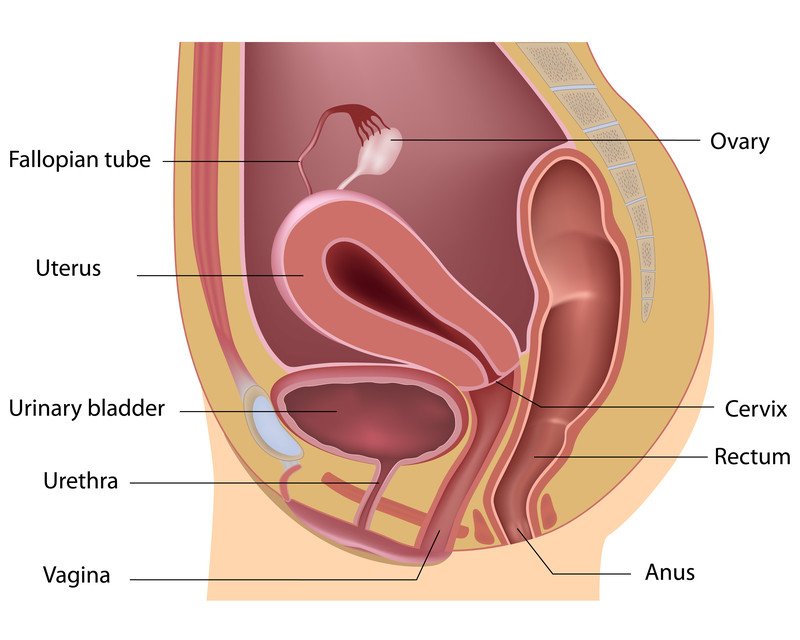
Vaginal atrophy (atrophic vaginitis)
Medically reviewed by Drugs.com. Last updated on Feb 12, 2024.
What is vaginal atrophy?

Vaginal atrophy is a change of the vagina that develops when there is a significant decrease in levels of the female hormone estrogen. The condition also is called atrophic vaginitis.
Estrogen, which is produced by the ovaries, plays a vital role in keeping vaginal tissues lubricated and healthy. When levels of estrogen are low, vaginal tissue tends to become atrophic — thin, dry and shrunken. The vagina is then more prone to inflammation in an atrophic state.
Common conditions with low estrogen levels that cause vaginal atrophy include:
- menopause, when normal, age-related body changes cause the ovaries to decrease their production of estrogen
- surgical removal of the ovaries before the age of natural menopause, which can be done at the same time as a hysterectomy (removal of the uterus)
- treatment with medications used to decrease estrogen levels in women who have conditions such as uterine fibroids or endometriosis
- premature menopause, which occurs before age 40, a younger age than is considered normal for the average woman
- breastfeeding.
Vaginal atrophy typically develops so slowly that a woman may not notice any symptoms until five to ten years after menopause begins.
|
|
Symptoms of vaginal atrophy
Common signs of vaginal atrophy include:
- vaginal dryness
- vaginal itch or a burning sensation
- painful sexual intercourse
- light bleeding after intercourse.
Diagnosing vaginal atrophy
If you are a middle-aged woman, your doctor will ask whether you have started menopause or whether you have been experiencing menopausal symptoms (absent or irregular menstrual periods, mood swings, hot flashes, difficulty sleeping at night, night sweats).
If you are a woman of childbearing age, your doctor will inquire whether you are breastfeeding or having irregular menstrual periods, which could be caused by low estrogen levels or by an imbalance in female hormones. Your doctor also will review your medical and surgical history and ask about your current medications.
The doctor may suspect vaginal atrophy based on your age, symptoms and medical history. To confirm the diagnosis, the doctor will perform a pelvic examination to examine your vulva and vagina for signs of dryness, redness and thinning of tissue.
If you are menopausal and have bleeding after intercourse, your doctor may want to check for endometrial cancer (cancer of the uterine lining) by doing an endometrial biopsy. In this procedure, a small piece of tissue is removed from the uterine lining, and is examined in a laboratory. The doctor also may want to check for a problem with the cervix by doing a Pap test.
Expected duration of vaginal atrophy
The condition will continue until it is treated or estrogen levels return to normal.
Preventing vaginal atrophy
A water-soluble vaginal lubricant can be used to moisten the tissues and prevent painful sexual intercourse. Regular sexual activity also can help to prevent symptoms. This is because sexual intercourse improves blood circulation to the vagina, which helps to maintain vaginal tissue.
Drugs used to treat this and similar conditions
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Treating vaginal atrophy
Treatments range from over-the-counter moisturizers to prescription-only hormone therapy. Women can often manage mild symptoms with nonhormonal moisturizers and, during sexual intercourse, vaginal lubricants. Sexual activity itself may improve the symptoms. If none of these approaches helps, you may need low-dose estrogen in the form of a cream, tablet, or ring inserted into the vagina. Here's how the various options work:
- Vaginal moisturizers. Water-based vaginal moisturizers adhere to the surface of the vagina, releasing water and producing a moist film over vaginal tissue. They also help restore vaginal pH. One type of moisturizer, Replens, is inserted with an applicator and lasts up to three days. A silicone-based product, K-Y Liquibeads, consists of small beads, also inserted with an applicator, that last up to four days. Moisturizers are a good choice if vaginal dryness is bothersome most of the time and not just during sexual activity.
- Vaginal lubricants. In addition to a moisturizer, you may want to use a lubricant during intercourse. One example is Astroglide, a clear, thin, odorless liquid with a slippery feel that closely approximates natural vaginal secretions. You can apply it before intercourse to the vaginal opening or to the penis. Astroglide is water-based and non-staining and has a neutral pH, so it won't irritate the vagina or promote vaginal infections. (Olive oil and saliva are other time-tested lubricants.) There are many different lubricants, but no studies have been done comparing them.
- Low-dose vaginal estrogen. Estrogen in any form — oral, transdermal (via skin patch), or vaginal — can help restore normal vaginal pH and beneficial bacteria, thicken the epithelium, increase vaginal secretions, and decrease vaginal dryness. But it's best to apply the estrogen directly to the vagina. Compared with oral or transdermal estrogen, vaginal application requires a lower dose and involves less exposure of breast and endometrial tissues, where estrogen can increase the risk of cancer by stimulating the growth of cells. Low-dose estrogen products recommended specifically for the treatment of vaginal atrophy include vaginal creams (Estrace and Premarin), the vaginal tablet Vagifem, and Estring (an estradiol-infused silicone ring that sits around the cervix and releases a very low, steady dose of estrogen).
When to call a professional
Schedule an appointment with your doctor if you experience any vaginal bleeding, vaginal dryness, burning or itching, or if painful sexual intercourse is not relieved with a water-soluble lubricant.
Prognosis
In most people, the outlook is excellent.
Additional info
American College of Obstetricians and Gynecologists
https://www.acog.org/
Learn more about Vaginal atrophy
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.