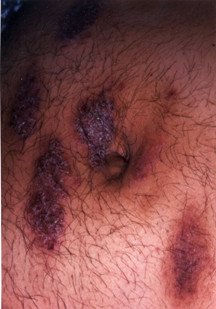
Eczema
Medically reviewed by Drugs.com. Last updated on Jan 12, 2024.
What is eczema?

Dermatitis is a skin inflammation. Eczema is the most common type of dermatitis.
Eczema first appears as an episode of itching and redness of the skin. You also may have tiny bumps or blisters.
When eczema develops into a long-term condition, it is called chronic eczema. This leads to:
- thickening of the skin
- scaling
- flaking
- dryness
- color changes.
There are many types of eczema. The type depends on the cause, shape and location of the rash.
Some eczemas are related to allergies or to contact with irritating substances. Some are associated with fluid retention in the legs.
Following are types of eczema:
|
|
- Atopic eczema (atopic dermatitis) — This type of eczema comes and goes repeatedly. It usually occurs in people with an inherited tendency to allergies. These allergies may include allergic asthma, hay fever or food allergies.
Atopic eczema usually appears early in life, usually by 18 months. In babies, atopic eczema primarily affects the:
- face
- neck
- ears
- torso
- tops of feet or outside of elbows (less commonly)
Atopic eczema can also develop in adults. In older children, teenagers, and adults it usually involves the:
- skin inside the creases of the elbow
- knee
- ankle or wrist joints
- hands
- upper eyelids
- Contact dermatitis — When irritants touch the skin, they can produce two types of contact dermatitis. Irritant contact dermatitis is the direct irritation of the skin. It can be caused by prolonged contact with irritants such as:
- detergents
- bubble bath
- harsh soap
- sweat
- saliva
- urine
The second type of contact dermatitis is allergic contact dermatitis. This is an allergic reaction in the skin. This type occurs in people who have an allergy to a specific substance. The most common allergens are poison ivy, poison oak and poison sumac.
The substances that can trigger skin allergies are commonly found in:
- some building materials
- cleaning products
- deodorants
- cosmetics
- nickel in jewelry
- fragrances
- skin cream and lotions
- shampoos
- shoes
- clothing
- Hand eczema — Hand eczema is limited to the hands. It can be related to atopic eczema. Or it can result from repeated hand washing or exposure to strong detergents. Occasionally, it is caused by an allergy, such as to latex.
- Nummular eczema — This type of eczema is coin-sized patches of irritated skin. It typically appears on the legs, arms, or chest. It usually occurs in adults. It can be related to atopic dermatitis.
- Asteatotic eczema — This eczema appears as very dry skin, causing fine cracks. It often first involves the lower legs. It commonly occurs in the elderly. It is common during winter months spent indoors in low-humidity environments.
- Stasis dermatitis — This eczema appears on the calves, ankles, and feet. It occurs in people who have swelling due to poorly functioning veins in the lower legs. The veins cause fluid to collect in the legs (stasis). This leads to leg swelling, which leads to the signs of stasis dermatitis:
- itching
- fine red bumps
- skin redness or darkening
- weeping sores
- Lichen simplex chronicus — This eczema is a reaction to repeated scratching or rubbing of the skin. A nervous scratching habit can lead to thickened, discolored skin. Skin picking can lead to smaller bumps of the same type of rash.
- Seborrheic dermatitis — This type creates a greasier rash than usual for eczema. This scaly dermatitis commonly appears on the scalp of infants (as cradle cap). In adults, it appears as dandruff. It commonly affects the face or neck around the nose and at the scalp line.
Symptoms of eczema
Short-term symptoms of eczema include itchy skin, redness and tiny bumps or blisters.
If these symptoms remain untreated, the skin can become thick, scaly and dry. There can be areas of hair loss and color changes. Skin affected by long-term eczema is more vulnerable to secondary infections.
Each type of eczema has specific characteristics and patterns of symptoms:
- Atopic eczema (atopic dermatitis) — Atopic dermatitis appears as irritated, red, dry, crusted patches on the skin. If the skin becomes infected, it may develop a wet (weeping) look. Scratching the itchy patches causes more irritation, and increases the risk of infection.
- Contact dermatitis — When an irritant causes contact dermatitis, symptoms can range from a mild redness to severe skin blistering or ulceration.
When triggered by an allergic reaction, it usually causes skin redness, fine red bumps or blisters and severe itching.
A reaction caused by plant allergies (like poison ivy or poison oak) is usually intense. It appears as bumps and blisters in lines or streaks where the plant brushed against the skin.
- Hand eczema — Hand eczema usually appears during the winter as patches of dry, cracked skin. There may or may not be redness. Hand eczema may also cause itching, red bumps or blisters and scaling. Irritation often occurs under rings from soap trapped under the rings.
- Nummular eczema — Nummular eczema begins as small areas of irritation. They turn into round red, crusted or scaly patches.
- Asteatotic eczema — This type usually occurs on the lower legs. It causes itching or stinging pain in areas of dry, cracked, reddened skin. There may or may not be tiny bumps.
- Stasis dermatitis — Stasis dermatitis occurs in legs that are already puffy or swollen. It usually begins with mild redness and itching of the lower legs.
- Lichen simplex chronicus — This rash creates thickened, leathery skin with darkening of skin color. It is very itchy. Scratching makes the problem worse.
- Seborrheic dermatitis— Seborrheic dermatitis causes red, scaly patches with yellow, greasy crusts. These patches can be itchy or can cause burning.
Patches appear most commonly on the scalp as dandruff. But they also can occur elsewhere on the body. They may appear on the eyebrows, eyelids, ears and skin creases near the mouth and nose.
Scalp lesions in infants (cradle cap) can appear yellowish and greasy. They usually cause no discomfort.
Diagnosing eczema
Depending on your pattern of skin symptoms, your doctor will ask about your:
- personal and family allergy history
- history of exposure to irritating chemicals
- contact with potential allergy triggers, such as poison ivy.
In many cases, your doctor can diagnose eczema by examining the skin.
If your doctor suspects that allergies are involved, patch testing with various allergy-causing chemicals may be necessary.
Expected duration of eczema
Duration depends on the type of eczema. Symptoms may go away after a week or two. Or they may persist for years.
Preventing eczema
There are many things you can do to prevent or reduce eczema flare-ups.
- Avoid exposure to:
- extreme temperatures
- dry air
- harsh soaps
- perfumed products
- bubble baths
- Use blankets and clothing made of cotton. Avoid more irritating fabrics, such as wool. Avoid stiff synthetics, such as polyester.
- After showering or bathing, pat dry (rather than rub). That way, you leave a little moisture on your skin. Then apply a moisturizing cream or lotion to trap moisture in the skin.
- Use a humidifier to add moisture to indoor air during the winter heating season.
-
To help to prevent contact dermatitis, avoid skin contact with:
- dish detergent, cleaning solutions, and other irritating chemicals
- plants
- jewelry
- substances that trigger skin allergies
- If you have leg swelling, you can help prevent stasis dermatitis by:
- wearing compression stockings
- elevating your legs to the level of your hips if you sit for long periods.
Drugs used to treat this and similar conditions
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Treating eczema
Your doctor should review your skin care routine. Your doctor can ensure you are doing everything possible to prevent symptoms.
But sometimes eczema remains bothersome despite these measures.
Your doctor may prescribe a corticosteroid ointment or cream. In atopic dermatitis, mild or medium strength topical steroids generally are used. These are applied to the affected areas of the skin.
When topical corticosteroids are not sufficient or needed for long periods of time to control atopic dermatitis, your doctor may prescribe a topical calcineurin inhibitor. Tacrolimus and pimecrolimus topical agents are approved for use in children older than 2 years of age.
Strong steroids and oral antihistamines may be needed to treat allergic contact dermatitis.
If there are signs of bacterial skin infection, oral antibiotics usually are needed.
Sometimes, in very severe cases of eczema, your doctor will prescribe a short course of oral steroids or stronger immunosuppressants. However, these medications can have serious side effects. They must be used cautiously.
In some people, treatment with ultraviolet (UV) light is another option.
Seborrhea in adults is best treated with dandruff shampoo. Occasionally prescription antifungal facial creams or rinses may be needed.
Cradle cap in infants eventually clears up without treatment. However, it can last several months. The crust usually can be loosened. To do so, apply baby oil to the scalp 30 to 60 minutes before brushing with a soft brush. Then wash with baby shampoo.
When treating a contact allergy in a child, avoid topical treatments containing antihistamines. Skin reactions can occur.
When to call a professional
Call your doctor if you have an area of skin that is red and very itchy. Also call if your skin is cracked, blistered or painfully dry.
Ask your doctor for an urgent evaluation if you have signs of infection. These include an area of skin that:
- is painful
- is swollen
- has yellow drainage
- has streaking or spreading redness.
Prognosis
The prognosis varies from person to person. It depends on the type of eczema and its response to treatment.
Most contact dermatitis heals within two to three weeks. Most stasis dermatitis lasts for years.
About half of children with atopic eczema still have the problem as adults.
Additional info
National Eczema Foundation
http://eczema.org/
National Institute of Arthritis and Musculoskeletal and Skin Diseases
http://www.niams.nih.gov/
Learn more about Eczema
Treatment options
Care guides
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.