Chronic prostatitis
Medically reviewed by Drugs.com. Last updated on May 15, 2024.
What is chronic prostatitis?

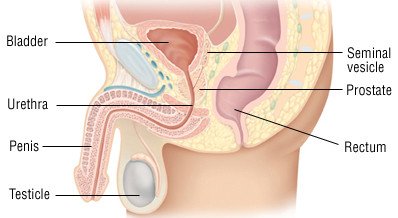
The prostate is a walnut-sized gland that sits below the bladder in men. This gland makes fluid that mixes with sperm to form semen.
|
|
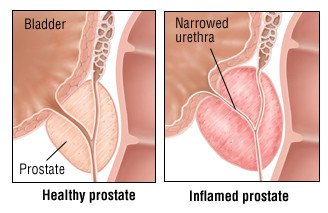
Prostatitis is inflammation or swelling of the prostate gland. When symptoms start gradually and linger for more than a couple of weeks, the condition is called chronic prostatitis.
|
|
Three major types of chronic prostatitis are:
- Chronic bacterial prostatitis — In this condition, a bacterial infection causes swelling and inflammation of the prostate. Doctors can definitively make this diagnosis if bacteria and white blood cells are found in the urine. White blood cells are present when there is inflammation that may or may not be related to an actual infection. True chronic bacterial infection accounts for a small percentage of cases of chronic prostatitis. Sometimes doctors suspect a lingering bacterial infection even though no bacteria are identified.
- Chronic non-bacterial prostatitis, also called inflammatory chronic pelvic pain syndrome — Doctors make this diagnosis when patients have typical symptoms of chronic prostatitis, but no bacteria are found in a urine sample. The cause of most cases of non-bacterial prostatitis is not well understood. The urine often contains white blood cells. Some patients may have a persistent low-grade infection that cannot be detected in a routine urine sample. However, most patients with non-bacterial prostatitis have no evidence of infection, even when sophisticated tests are done.
- Prostadynia, also called non-inflammatory chronic pelvic pain syndrome — This term is used when symptoms of prostatitis are present, but there is no evidence of prostate infection or inflammation. Doctors understand very little about why some people — often young, otherwise healthy men — develop this problem. Theories to explain prostadynia include an abnormal buildup of pressure in the urinary tract, irritation resulting from an autoimmune or chemical process, or pain generated in the nerves and muscles within the pelvis.
Chronic prostatitis is common and affects adult men of all ages and from all backgrounds. About five percent of men experience symptoms of chronic prostatitis at some point in their lives. Chronic prostatitis is the reason for up to 25% of office visits to urologists. Urologists are doctors who specialize in diseases of the urinary tract.
Some men develop a chronic infection in the prostate that does not cause any symptoms. Men with this problem may be diagnosed during an evaluation for other urological conditions, such as enlarged prostate or infertility. Doctors often treat the infection with the same antibiotics used for chronic bacterial prostatitis.
Bacterial infection of the prostate gland also can cause acute prostatitis, which starts suddenly and usually causes fever and more serious symptoms. Acute prostatitis is less common than chronic prostatitis.
Symptoms of chronic prostatitis
Prostatitis usually causes swelling of the prostate gland. The prostate surrounds the urethra (the tube that carries urine out of the body from the bladder). The swollen prostate presses on the urethra causing pain or other problems with urination.
Typical symptoms of chronic prostatitis include:
- burning during or after urination
- difficulty starting the urine stream
- dribbling after urination has been completed
- a need to urinate frequently or urgently
- a sensation that the bladder cannot be emptied completely
- pain felt above the penis, in or below the scrotum, or in the back or rectum
- pain experienced during or after orgasm.
In some men, symptoms may be hardly noticed or only slightly annoying. Other men are quite bothered by chronic prostatitis and find that the symptoms interfere with work, leisure activities and sexual enjoyment.
Diagnosing chronic prostatitis
If your doctor suspects prostatitis, he or she will ask you to describe your symptoms in detail. Your doctor will also want to know:
- your general medical history
- what medications you take
- how much caffeine and alcohol you drink
- whether you have had sexual contacts that may increase your risk of sexually transmitted infections. The symptoms of some sexually transmitted infections can mimic prostatitis.
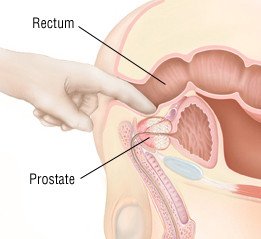
Your doctor will examine your prostate gland by inserting a gloved and lubricated finger into your rectum. In chronic prostatitis, the gland may be swollen, firm and tender, or it may feel normal. You may experience pain or an urgent need to urinate when pressure is applied to the prostate. Your doctor will examine you to look for other problems that may be causing your symptoms.
|
|
The next step will be to examine a urine specimen to look for white blood cells and bacteria. Often your doctor will ask you to produce separate urine specimens before and after your prostate gland is examined. Typical findings depend on the specific type of chronic prostatitis:
- In bacterial prostatitis, the urine will contain white blood cells and bacteria, especially after the doctor has pressed firmly on the prostate. The urine usually will contain the type of bacteria found in most urinary tract infections.
- In non-bacterial prostatitis, the urine collected after prostate massage may contain white blood cells. However, no bacteria will be seen, and a urine culture will be normal.
- In prostadynia, the urine specimen will be clear, even after the doctor has pressed firmly on the prostate.
In most cases of chronic prostatitis, this simple evaluation is all that is needed to make a diagnosis and begin treatment. Occasionally, a person may have vague or unusual symptoms. Then your doctor will consider other diagnoses, such as interstitial cystitis, urethritis, benign enlargement of the prostate, or even prostate cancer. In such a situation, your doctor may recommend additional blood or urine tests, an ultrasound of the prostate, an examination of the bladder with a lighted telescope (cystoscopy) or a needle biopsy of the prostate.
Expected duration of chronic prostatitis
Chronic prostatitis may last for weeks or months before it is diagnosed. Some cases of chronic prostatitis respond promptly to treatment, and symptoms disappear over several days. In other cases, symptoms may linger for weeks or months or may come and go over a period of years.
Preventing chronic prostatitis
Chronic prostatitis cannot be prevented.
Drugs used to treat this and similar conditions
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Treating chronic prostatitis
For many years, antibiotics have been the mainstay of treatment for chronic prostatitis. Antibiotics such as trimethoprim-sulfa (Bactrim, Septra), ciprofloxacin (Cipro) and levofloxacin (Levaquin) are used most often to treat chronic bacterial prostatitis. Because it is difficult for antibiotics to get into the prostate gland, they must be given at high doses for an extended period, often four or more weeks.
Even if no bacteria are seen in the urine, your doctor may still be concerned that you have a chronic bacterial prostatitis. In that situation, he or she may prescribe a course of antibiotics. Some men may get relief from this treatment.
However, in many cases, antibiotics alone will not eliminate the problem. Other treatments that men may consider include:
- Alpha-blocker medications, such as tamsulosin (Flomax) or alfuzosin (Uroxatral), may be prescribed to relax the muscles that control the bladder. These may relieve symptoms of urgency, hesitancy or dribbling. For men with an enlarged prostate, similar symptom improvement may be seen with drugs that shrink the size of the prostate, such as finasteride (Proscar) or dutasteride (Avodart).
- Pain relievers, anti-inflammatory drugs and muscle relaxants may help with pain and muscle spasms. Some men find relief with warm baths or with biofeedback programs designed to reduce tension in the pelvic muscles.
- Eliminating caffeine and alcohol may reduce irritation of the bladder and prostate.
- Physical therapy aimed at releasing muscle tension in the pelvic floor.
- Some physicians recommend reducing congestion in the prostate by ejaculating more frequently or by massaging the prostate regularly.
Often the exact reason why a man with chronic prostatitis has symptoms is not clear. And there may be more than one contributing factor. A treatment for one man may not work in another man with similar symptoms.
Some men will improve on their own or with the first treatment that is tried. Others will continue to experience symptoms despite a variety of treatments.
When to call a professional
Contact a health care professional if you develop:
- difficulty with urination
- pain in the groin, testicles or back
- pain during sexual intercourse
- an adverse reaction to an antibiotic or other medication given to treat your prostate infection.
Prognosis
Chronic prostatitis can be very difficult to cure. Many men do not respond to one or more prolonged courses of antibiotics. Because little is understood about prostatitis that is not caused by infection, finding the right treatment may be difficult. Nonetheless, several potentially effective treatments are available.
Don't be discouraged if your symptoms have not responded to the first or even second treatment. Keep working with your doctor to help you get relief. If you have unusual or particularly troubling symptoms, your doctor may refer you to a urologist or other specialist.
There is no evidence that chronic prostatitis increases the risk of developing prostate cancer.
Additional info
National Institute of Diabetes and Digestive and Kidney Disorders
https://www.niddk.nih.gov/
American Urological Association
https://www.auanet.org/
Learn more about Chronic prostatitis
Treatment options
Care guides
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.