Urinary Incontinence
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
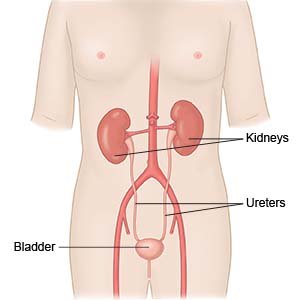
Urinary incontinence (UI) is loss of bladder control. UI develops because your bladder cannot store or empty urine properly. The 3 most common types of UI are stress incontinence, urge incontinence, or both.
 |
DISCHARGE INSTRUCTIONS:
Return to the emergency department if:
- You have severe pain.
- You are confused or cannot think clearly.
- You see blood in your urine.
- You have pain when you urinate.
- You have new or worse pain, even after treatment.
Call your doctor if:
- You have a fever.
- Your mouth feels dry or you have vision changes.
- Your urine is cloudy or smells bad.
- You have questions or concerns about your condition or care.
Related medications
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Medicines:
- Medicines may be given to help strengthen your bladder control.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Manage UI:
- Do pelvic muscle exercises often. Your pelvic muscles help you stop urinating. Squeeze these muscles tight for 5 seconds, then relax for 5 seconds. Gradually work up to squeezing for 10 seconds. Do 3 sets of 15 repetitions a day, or as directed. This will help strengthen your pelvic muscles and improve bladder control.
- Keep a UI record. Write down how often you leak urine and how much you leak. Make a note of what you were doing when you leaked urine.
- Train your bladder. Go to the bathroom at set times, such as every 2 hours, even if you do not feel the urge to go. You can also try to hold your urine. For example, hold your urine for 5 minutes when you feel the urge to go. As that becomes easier, hold your urine for 10 minutes. Behavior therapy may help you learn to control the urge to urinate.
- Drink liquids as directed. Ask your healthcare provider how much liquid to drink each day and which liquids are best for you. You may need to limit the amount of liquid you drink to help control your urine leakage. Do not drink any liquid right before you go to bed. Limit or do not have drinks that contain caffeine or alcohol.
- Prevent constipation. Eat a variety of high-fiber foods. Good examples are high-fiber cereals, beans, vegetables, and whole-grain breads. Prune juice may help make your bowel movement softer. Walking is the best way to trigger your intestines to have a bowel movement.

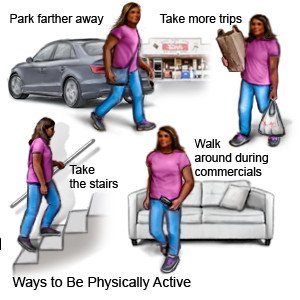
- Be physically active and maintain a healthy weight. Ask your healthcare provider what a healthy weight is for you. Extra weight puts pressure on your bladder and may make your symptoms worse. Your provider can help you create a weight loss plan, if needed. The plan will include ways to be physically active that will not put extra pressure on your bladder.
- Use a catheter as directed to help empty your bladder. A catheter is a tiny, plastic tube that is put into your bladder to drain your urine. Your provider may tell you to use a catheter to prevent your bladder from getting too full and leaking urine.
Follow up with your doctor or urologist as directed:
If you keep a UI record, take it with you to your follow-up visits. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Urinary Incontinence
Treatment options
Care guides
Symptoms and treatments
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
