Upper Endoscopy in Children
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
What you need to know about an upper endoscopy:
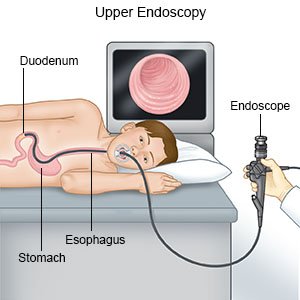
An upper endoscopy is also called an upper gastrointestinal (GI) endoscopy, or an esophagogastroduodenoscopy (EGD). The upper intestines include the esophagus, stomach, and duodenum (first part of the small intestine). A scope (thin, flexible tube with a light and camera) is used to examine the lining of your child's upper intestines. An upper endoscopy is used to look for problems, such as bleeding, swelling, polyps, ulcers, or infection. An upper endoscopy in children is often used to find the cause of abdominal pain, difficulty swallowing, or nausea and vomiting. It may also be done to remove foreign bodies such as a swallowed coin or toy.
 |
How to prepare your child for an upper endoscopy:
- Your child's provider will tell you when your child should stop eating or drinking before the procedure. If the procedure will be later in the day, you may be able to give your child clear liquids until 2 to 4 hours before the procedure. Clear liquids include water, oral rehydration solutions (ORS), or juices without pulp. Do not give your child clear liquids that are red or purple. Stop breastfeeding your child 4 hours before the procedure.
- Your child's provider will tell you what medicines your child should take or not take on the day of the procedure. If your child is 6 years of age or older, explain what might happen during the procedure, to decrease anxiety. This may also increase his or her cooperation and tolerance for the procedure. Your child's provider may give your child medicine to help him or her relax before the procedure starts.
What will happen during an upper endoscopy:
- Your child may receive IV sedation or general anesthesia. IV sedation will make your child feel sleepy and help him or her relax during the procedure. General anesthesia may be given to keep your child asleep and free from pain during the procedure. Your child's healthcare provider may have you come into the procedure room until your child is asleep. This may decrease your child's anxiety and help him or her cooperate with providers.
- Your child may also be given medicine to numb his or her throat. Your child may need to wear a plastic mouthpiece to help hold his or her mouth open and protect the teeth and tongue. Your child's provider will gently insert the endoscope through your child's mouth and down into the throat. Your child may feel pressure in his or her throat but should not feel pain. The endoscope will not prevent your child from breathing.
- Your child's provider will watch the scope on a monitor. He or she will take pictures with the scope and look for any abnormal areas. Your child's provider may gently inject air to see your child's digestive tract clearly. Tissue samples may be taken and sent to a lab for tests. Your child's provider may remove foreign objects, tumors, or polyps that may be blocking your child's upper intestines. He or she may also insert tools through the scope to treat bleeding or place a stent (tube). When the procedure is finished, the endoscope will be slowly removed.
What will happen after an upper endoscopy:
Your child may feel bloated, gassy, or have some abdominal discomfort or distention. Your child's throat may be sore for 24 to 36 hours after the procedure. It is normal for your child to spit up a small amount of blood. Your child may burp or pass gas from air that is still inside the body after the procedure. Your child may need to take short walks or lie on his or her left side to help move the gas out. Your child may be able to go home after he or she is awake and can drink liquids.
Risks of an upper endoscopy:
Your child's esophagus, stomach, or duodenum may be punctured or torn during the procedure. This is because of increased pressure as the scope and air are passing through. Your child may bleed more than expected or get an infection. Your child may have a slow or irregular heartbeat, or low blood pressure, during the procedure. This can cause sweating and fainting. Fluid may enter your child's lungs and he or she may have trouble breathing. These problems can be life-threatening.
Related medications
Call your local emergency number (911 in the US) if:
- Your child complains of pain in his or her chest.
- Your child has trouble breathing.
Seek care immediately if:
- Your child feels dizzy or faints.
- Your child has trouble swallowing.
- Your child has severe throat pain.
- Your child's bowel movements are very dark, black, or you can see bright red blood in them.
- Your child's stomach is very painful, feels hard, and is larger than usual.
- Your child vomits blood.
Contact your child's doctor if:
- Your child has a fever or chills.
- Your child cannot pass gas.
- Your child does not have a bowel movement for 3 days after the procedure.
- Your child has nausea or is vomiting.
- Your child's skin is itchy, swollen, or he or she has a rash.
- You have questions or concerns about your child's condition or care.
Care for your child:
- Limit your child's activity after the procedure. Have your child lie on the couch or rest quietly until the day after the procedure. He or she may feel tired and need frequent naps. Your child can take short walks to the bathroom or around the house to help pass gas. He or she should not play sports or do vigorous activity after the procedure. Your child may be able to go to school or return to daycare the day after the procedure. Ask your healthcare provider when your child can return to normal activities.
- Relieve your child's gas and discomfort. Have your child lie on his or her left side. Your child may need to take short walks to help move the gas out. Give your child small meals until the bloating has gone away. Start with clear liquids such as juice without pulp. If your child does okay with clear liquids, start with his or her usual foods. Ask your child's healthcare provider if your child needs to be on a special diet.
- Relieve your child's sore throat. Give your child crushed ice or flavored ice pops.
Follow up with your child's doctor as directed:
Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
