Juvenile Arthritis
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is juvenile arthritis?
Juvenile arthritis is a long-term autoimmune disease that causes pain and inflammation in one or more joints. Juvenile arthritis develops when the immune system attacks the tissues in the joints. Your child may have symptoms for only a few months, or for the rest of his or her life. Your child may have periods of remission (no signs or symptoms). Your child may have any of 6 subtypes of juvenile arthritis. Ask his or her healthcare provider for more information about the type he or she has.
What are the signs and symptoms of juvenile arthritis?
- Joint pain or stiffness, especially in the morning
- High fever or a skin rash
- Swollen lymph nodes
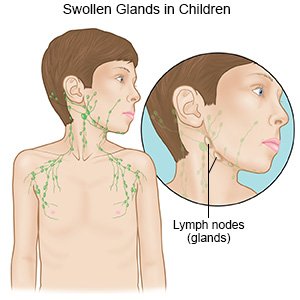
- Eye pain or a headache
- Swelling or nodules (growths) on or around the joints
- Nail changes, or bent or crooked fingers
- Fatigue or muscle weakness
- Loss of appetite, weight loss, abdominal pain, or diarrhea
What increases my child's risk for juvenile arthritis?
- Being female
- A family history of arthritis
- Certain infections, such as rubella or parvovirus
- Problems with your child's immune system
- High levels of immunoglobulin G (IgG) in your child's blood
How is juvenile arthritis diagnosed?
Your child's healthcare provider will examine your child. He or she may ask about other medical conditions your child has and medicines he or she is taking. Healthcare providers will also need to know when the joint problems and other symptoms started. Your child may also need any of the following tests:
- Blood tests are used to check your child's blood for signs of infection or inflammation.
- X-ray or MRI pictures may be taken of your child's joints. Your child may be given contrast liquid to help the joints show up better on the x-ray. Tell the healthcare provider if your child has ever had an allergic reaction to contrast liquid. Do not let your child enter the MRI room with anything metal. Metal can cause serious injury. Tell the healthcare provider if your child has any metal in or on his or her body.
- Arthrocentesis is a procedure used to drain fluid out of a joint. The fluid is tested for infection or other problems that can cause arthritis.
- Synovial biopsy may be used if your child's joint fluid cannot be drained or if he or she has signs of an infection. A piece of tissue is removed from the lining of a joint. The tissue is tested for possible causes of your child's arthritis.
Related medications
How is juvenile arthritis treated?
- Medicines: Your child may need more than one kind of medicine to control arthritis. Some medicines work quickly to help lower or control pain and inflammation. Other medicines prevent joint damage or slow the progression of arthritis.
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. This medicine is available with or without a doctor's order. NSAIDs can cause stomach bleeding or kidney problems in certain people. If your child takes blood thinner medicine, always ask if NSAIDs are safe for him or her. Always read the medicine label and follow directions. Do not give these medicines to children younger than 6 months without direction from a healthcare provider.
- Disease-modifying rheumatoid arthritis drugs (DMARDs) help prevent joint damage, slow the progression of arthritis, and reduce pain, stiffness, and inflammation. DMARDs can take time to start working. Your child may also need to take other medicines to control his or her symptoms until the DMARDs start to work.
- Steroid medicine helps decrease severe inflammation. These are usually given for a short time while other medicines are started that can take longer to be effective.
- Biologic therapy includes medicines used to help decrease joint swelling, pain, and stiffness. These medicines can increase the risk for serious infections. Your child's health will need to be monitored while he or she is taking this medicine.
- Surgery may be needed if your child's joints become severely affected. Surgery can be done to take out all or part of the joint and replace it with an artificial joint. This may be done to ease pain and repair the joint. It may also be done if the bones in your child's spine are pressing on the nerves.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
How can I help my child manage juvenile arthritis?
- Eye exams are used to check for uveitis (eye inflammation). Have your child's eyes examined regularly. Ask your child's healthcare provider or rheumatologist for more information about eye checks and how often your child should have them.
- A physical therapist can teach your child exercises to help improve movement and strength, and to decrease pain. An occupational therapist can teach him or her skills to help with his or her daily activities.
- Rest is important if your child's joints are painful. Limit his or her activities until his or her symptoms improve. Gradually let him or her start his or her regular activities when he or she can do them without pain. Have him or her avoid motions and activities that cause strain on his or her joints, such as heavy exercise and lifting.
- Ice or heat can help decrease swelling and pain. Ice may also help prevent tissue damage. Use an ice pack, or put crushed ice in a plastic bag. Cover it with a towel and place it on your child's joint for 15 to 20 minutes every hour as directed. You can also apply heat to his or her joints for 20 minutes every 2 hours. Heat treatment includes hot packs, heat lamps, warm baths, or showers.
- Splints may be given for your child to wear on his or her hands. Splints can help his or her joints rest and decrease inflammation.
- Physical activity can help increase strength and flexibility. Keep your child as active as possible while avoiding things that increase his or her pain. Ask your child's healthcare provider or rheumatologist about the best exercise plan for your child.
When should I seek immediate care?
- Your child has severe eye pain or vision changes.
- Your child's pain becomes worse.
- Your child has severe redness, swelling, or pain in one of his or her joints.
When should I call my child's doctor?
- Your child has a fever.
- Your child has problems eating or you feel he or she is not eating enough.
- Your child begins to lose weight, thinks more slowly, or seems sad most of the time.
- Your child has a severe headache or pain around his or her eyes.
- You have questions or concerns about your child's condition or care.
Care Agreement
You have the right to help plan your child's care. Learn about your child's health condition and how it may be treated. Discuss treatment options with your child's healthcare providers to decide what care you want for your child. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Juvenile Arthritis
Treatment options
Care guides
Symptoms and treatments
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
