Cortisone Acetate: Package Insert / Prescribing Info
Package insert / product label
Dosage form: tablet
Drug class: Glucocorticoids
Medically reviewed by Drugs.com. Last updated on Jun 12, 2025.
On This Page
Cortisone Acetate Description
Glucocorticoids are adrenocortical steroids, both naturally occurring and synthetic, which are readily absorbed from the gastrointestinal tract.
Cortisone acetate is a white or practically white, odorless, crystalline powder. It is stable in air. It is insoluble in water. The molecular weight is 402.48. It is designated chemically as 17,21-Dihydroxypregn-4-ene-3,11,20-trione 21-acetate. The molecular formula is C 23H 30O 6 and the structural formula is:
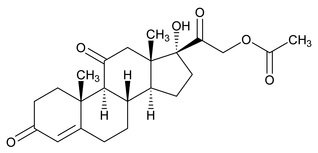
Each tablet, for oral administration, contains 25 mg of cortisone acetate.
Inactive ingredients are lactose monohydrate, corn starch, sucrose, and calcium stearate.
Cortisone Acetate - Clinical Pharmacology
Naturally occurring glucocorticoids (hydrocortisone and cortisone), which also have salt-retaining properties, are used as replacement therapy in adrenocortical deficiency states. They are also used for their potent anti-inflammatory effects in disorders of many organ systems.
Glucocorticoids cause profound and varied metabolic effects. In addition, they modify the body’s immune responses to diverse stimuli.
Indications and Usage for Cortisone Acetate
When oral therapy is not feasible:
1. Endocrine Disorders
- Primary or secondary adrenocortical insufficiency (hydrocortisone or cortisone is the first choice; synthetic analogs may be used in conjunction with mineralocorticoids where applicable; in infancy mineralocorticoid supplementation is of particular importance).
- Congenital adrenal hyperplasia
- Nonsuppurative thyroiditis
- Hypercalcemia associated with cancer
2. Rheumatic Disorders
As adjunctive therapy for short-term administration (to tide the patient over an acute episode or exacerbation) in:
- Psoriatic arthritis
- Rheumatoid arthritis, including juvenile rheumatoid arthritis (selected cases may require low-dose maintenance therapy)
- Ankylosing spondylitis
- Acute and subacute bursitis
- Acute nonspecific tenosynovitis
- Acute gouty arthritis
- Post-traumatic osteoarthritis
- Synovitis of osteoarthritis
- Epicondylitis
3. Collagen Diseases
During an exacerbation or as maintenance therapy in selected cases of:
- Systemic lupus erythematosus
- Acute rheumatic carditis
- Systemic dermatomyositis (polymyositis)
4. Dermatologic Diseases
- Pemphigus
- Bullous dermatitis herpetiformis
- Severe erythema multiforme (Stevens-Johnson syndrome)
- Exfoliative dermatitis
- Mycosis fungoides
- Severe psoriasis
- Severe seborrheic dermatitis
5. Allergic States
Control of severe or incapacitating allergic conditions intractable to adequate trials of conventional treatment in:
- Seasonal or perennial allergic rhinitis
- Bronchial asthma
- Contact dermatitis
- Atopic dermatitis
- Serum sickness
- Drug hypersensitivity reactions
6. Ophthalmic Diseases
Severe acute and chronic allergic and inflammatory processes involving the eye and its adnexa, such as:
- Allergic conjunctivitis
- Keratitis
- Allergic corneal marginal ulcers
- Herpes zoster ophthalmicus
- Iritis and iridocyclitis
- Chorioretinitis
- Anterior segment inflammation
- Diffuse posterior uveitis and choroiditis
- Optic neuritis
- Sympathetic ophthalmia
7. Respiratory Diseases
- Symptomatic sarcoidosis
- Loeffler’s syndrome not manageable by other means
- Berylliosis
- Fulminating or disseminated pulmonary tuberculosis when used concurrently with appropriate antituberculosis chemotherapy
- Aspiration pneumonitis
8. Hematologic Disorders
- Idiopathic thrombocytopenic purpura in adults
- Secondary thrombocytopenia in adults
- Acquired (autoimmune) hemolytic anemia
- Erythroblastopenia (RBC anemia)
- Congenital (erythroid) hypoplastic anemia
9. Neoplastic Diseases
For palliative management of:
- Leukemias and lymphomas in adults
- Acute leukemia of childhood
10. Edematous States
- To induce a diuresis or remission of proteinuria in the nephrotic syndrome, without uremia, of the idiopathic type or that due to lupus erythematosus
11. Gastrointestinal Diseases
To tide the patient over a critical period of the disease in:
- Ulcerative colitis
- Regional enteritis
12. Miscellaneous
- Tuberculous meningitis with subarachnoid block or impending block when used concurrently with appropriate antituberculous chemotherapy
- Trichinosis with neurologic or myocardial involvement
Warnings
In patients on corticosteroid therapy subjected to unusual stress, increased dosage of rapidly acting corticosteroids before, during, and after the stressful situation is indicated.
Immunosuppression and Increased Risk of Infection
Corticosteroids, including cortisone acetate tablets, suppress the immune system and increase the risk of infection with any pathogen, including viral, bacterial, fungal, protozoan, or helminthic pathogens. Corticosteroids can;
- Reduce resistance to new infections
- Exacerbate existing infections
- Increase the risk of disseminated infections
- Increase the risk of reactivation or exacerbation of latent infections
- Mask some signs of infection
Corticosteroid-associated infections can be mild but can be severe and at times fatal. The rate of infectious complication increases with increasing corticosteroid dosages.
Monitor for the development of infection and consider cortisone acetate tablets withdrawal or dosage reduction as needed.
Tuberculosis
If cortisone acetate tablets are used to treat a condition in patients with latent tuberculosis or tuberculin reactivity, reactivation of tuberculosis may occur. Closely monitor such patients for reactivation. During prolonged cortisone acetate therapy, patients with latent tuberculosis or tuberculin reactivity should receive chemoprophylaxis.
Varicella Zoster and Measles Viral Infections
Varicella and measles can have a serious or even fatal course in non-immune patients taking corticosteroids, including cortisone acetate tablets. In corticosteroid-treated patients who have not had these diseases or are nonimmune, particular care should be taken to avoid exposure to varicella and measles:
- If a cortisone acetate tablets-treated patient is exposed to varicella, prophylaxis with varicella zoster immune globulin may be indicated. If varicella develops, treatment with antiviral agents may be considered.
- If a cortisone acetate tablets-treated patient is exposed to measles, prophylaxis with immunoglobulin may be indicated.
Hepatitis B Virus Reactivation
Hepatitis B virus reactivation can occur in patients who are hepatitis B carriers treated with immunosuppressive dosages of corticosteroids, including cortisone acetate tablets. Reactivation can also occur infrequently in corticosteroid-treated patients who appear to have resolved hepatitis B infection.
Screen patients for hepatitis B infection before initiating immunosuppressive (e.g., prolonged) treatment with cortisone acetate tablets. For patients who show evidence of hepatitis B infection, recommend consultation with physicians with expertise in managing hepatitis B regarding monitoring and consideration for hepatitis B antiviral therapy.
Fungal Infections
Corticosteroids, including cortisone acetate tablets, may exacerbate systemic fungal infections; therefore, avoid cortisone acetate tablets use in the presence of such infections unless cortisone acetate tablets are needed to control drug reactions. For patients on chronic cortisone acetate tablets therapy who develop systemic fungal infections, cortisone acetate tablets withdrawal or dosage reduction is recommended.
Amebiasis
Corticosteroids, including cortisone acetate tablets, may activate latent amebiasis. Therefore, it is recommended that latent amebiasis or active amebiasis be ruled out before initiating cortisone acetate tablets in patients who have spent time in the tropics or patients with unexplained diarrhea.
Strongyloides Infestation
Corticosteroids, including cortisone acetate tablets, should be used with great care in patients with known or suspected Strongyloides (threadworm) infestation. In such patients, corticosteroid-induced immunosuppression may lead to Strongyloides hyperinfection and dissemination with widespread larval migration, often accompanied by severe enterocolitis and potentially fatal gram-negative septicemia.
Cerebral Malaria
Avoid corticosteroids, including cortisone acetate tablets, in patients with cerebral malaria.
Kaposi’s Sarcoma
Kaposi’s sarcoma has been reported to occur in patients receiving corticosteroid therapy, most often for chronic conditions. Discontinuation of corticosteroids may result in clinical improvement of Kaposi’s sarcoma.
Drug-induced secondary adrenocortical insufficiency may result from too rapid withdrawal of corticosteroids and may be minimized by gradual reduction of dosage. This type of relative insufficiency may persist for months after discontinuation of therapy; therefore, in any situation of stress occurring during that period, hormone therapy should be reinstituted. If the patient is receiving steroids already, dosage may have to be increased. Since mineralocorticoid secretion may be impaired, salt and/or a mineralocorticoid should be administered concurrently.
In cerebral malaria, a double-blind trial has shown that the use of corticosteroids is associated with prolongation of coma and a higher incidence of pneumonia and gastrointestinal bleeding.
Prolonged use of corticosteroids may produce posterior subsapsular cataracts, glaucoma with possible damage to the optic nerves, and may enhance the establishment of secondary ocular infections due to fungi or viruses.
Average and large doses of hydrocortisone or cortisone can cause elevation of blood pressure, salt and water retention, and increased excretion of potassium. These effects are less likely to occur with the synthetic derivatives except when used in large doses. Dietary salt restriction and potassium supplementation may be necessary. All corticosteroids increase calcium excretion.
Administration of live virus vaccines, including smallpox, is contraindicated in individuals receiving immunosuppressive doses of corticosteroids. If inactivated viral or bacterial vaccines are administered to individuals receiving immunosuppressive doses of corticosteroids, the expected serum antibody response may not be obtained. However, immunization procedures may be undertaken in patients who are receiving corticosteroids as replacement therapy, e.g., for Addison’s disease.
Literature reports suggest an apparent association between use of corticosteroids and left ventricular free wall rupture after a recent myocardial infarction; therefore, therapy with corticosteroids should be used with great caution in these patients.
Usage in pregnancy: Since adequate human reproduction studies have not been done with corticosteroids, use of these drugs in pregnancy or in women of childbearing potential requires that the anticipated benefits be weighed against the possible hazards to the mother and embryo or fetus. Infants born of mothers who have received substantial doses of corticosteroids during pregnancy should be carefully observed for signs of hypoadrenalism.
Corticosteroids appear in breast milk and could suppress growth, interfere with endogenous corticosteroid production, or cause other unwanted effects. Mothers taking pharmacologic doses of corticosteroids should be advised not to nurse.
Precautions
General:
Following prolonged therapy, withdrawal of corticosteroids may result in symptoms of the corticosteroid withdrawal syndrome including fever, myalgia, arthralgia, and malaise. This may occur in patients even without evidence of adrenal insufficiency.
There is an enhanced effect of corticosteroids in patients with hypothyroidism and in those with cirrhosis.
Corticosteroids should be used cautiously in patients with ocular herpes simplex because of possible corneal perforation.
The lowest possible dose of corticosteroid should be used to control the condition under treatment, and when reduction in dosage is possible, the reduction should be gradual.
Psychic derangements may appear when corticosteroids are used, ranging from euphoria, insomnia, mood swings, personality changes, and severe depression, to frank psychotic manifestations. Also, existing emotional instability or psychotic tendencies may be aggravated by corticosteroids.
Aspirin should be used cautiously in conjunction with corticosteroids in hypoprothrombinemia.
Steroids should be used with caution in nonspecific ulcerative colitis, if there is a probability of impending perforation, abscess, or other pyogenic infection, diverticulitis, fresh intestinal anastomoses, active or latent peptic ulcer, renal insufficiency, hypertension, osteoporosis, and myasthenia gravis. Signs of peritoneal irritation following gastrointestinal perforation in patients receiving large doses of corticosteroids may be minimal or absent. Fat embolism has been reported as a possible complication of hypercortisonism.
When large doses are given, some authorities advise that corticosteroids be taken with meals and antacids taken between meals to help to prevent peptic ulcer.
Growth and development of infants and children on prolonged corticosteroid therapy should be carefully observed.
Steroids may increase or decrease motility and number of spermatozoa in some patients.
Phenytoin, phenobarbital, ephedrine, and rifampin may enhance the metabolic clearance of corticosteroids, resulting in decreased blood levels and lessened physiologic activity, thus requiring adjustment in corticosteroid dosage.
The prothrombin time should be checked frequently in patients who are receiving corticosteroids and coumarin anticoagulants at the same time because of reports that corticosteroids have altered the response to these anticoagulants. Studies have shown that the usual effect produced by adding corticosteroids is inhibition of response to coumarins, although there have been some conflicting reports of potentiation not substantiated by studies.
When corticosteroids are administered concomitantly with potassium-depleting diuretics, patients should be observed closely for development of hypokalemia.
Information for Patients:
Persons who are on immunosuppressant doses of corticosteroids should be warned to avoid exposure to chickenpox or measles. Patients should also be advised that if they are exposed, medical advice should be sought without delay.
Adverse Reactions/Side Effects
Fluid and Electrolyte Disturbances
- Sodium retention
- Fluid retention
- Congestive heart failure in susceptible patients
- Potassium loss
- Hypokalemic alkalosis
- Hypertension
Musculoskeletal
- Muscle weakness
- Steroid myopathy
- Loss of muscle mass
- Osteoporosis
- Vertebral compression fractures
- Aseptic necrosis of femoral and humeral heads
- Pathologic fracture of long bones
- Tendon rupture
Gastrointestinal
- Peptic ulcer with possible perforation and hemorrhage
- Perforation of the small and large bowel, particularly in patients with inflammatory bowel disease
- Pancreatitis
- Abdominal distention
- Ulcerative esophagitis
Dermatologic
- Impaired wound healing
- Thin fragile skin
- Petechiae and ecchymoses
- Erythema
- Increased sweating
- May suppress reactions to skin tests
- Other cutaneous reactions, such as allergic dermatitis, urticaria, angioneurotic edema
Neurologic
- Convulsions
- Increased intracranial pressure with papilledema (pseudotumor cerbri) usually after treatment
- Vertigo
- Headache
- Psychic disturbances
Endocrine
- Menstrual irregularities
- Development of cushingoid state
- Suppression of growth in children
- Secondary adrenocortical and pituitary unresponsiveness, particularly in times of stress, as in trauma, surgery, or illness
- Decreased carbohydrate tolerance
- Manifestations of latent diabetes mellitus
- Increased requirements for insulin or oral hypoglycemic agents in diabetics
- Hirsutism
Ophthalmic
- Posterior subcapsular cataracts
- Increased intraocular pressure
- Glaucoma
- Exophthalmos
Metabolic
- Negative nitrogen balance due to protein catabolism
Other
- Hypersensitivity
- Thromboembolism
- Weight gain
- Increased appetite
- Nausea
- Malaise
To report SUSPECTED ADVERSE REACTIONS, contact Chartwell RX, LLC. Corp. at 1-845-232-1683, or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Related/similar drugs
Cortisone Acetate Dosage and Administration
For Oral Administration
DOSAGE REQUIREMENTS ARE VARIABLE AND MUST BE INDIVIDUALIZED ON THE BASIS OF THE DISEASE AND THE RESPONSE OF THE PATIENT.
The initial dosage varies from 25 to 300 mg a day depending on the disease being treated. In less severe diseases doses lower than 25 mg may suffice, while in severe diseases doses higher than 300 mg may be required. The initial dosage should be maintained or adjusted until the patient’s response is satisfactory. If satisfactory clinical response does not occur after a reasonable period of time, discontinue cortisone acetate tablets and transfer the patient to other therapy.
After a favorable initial response, the proper maintenance dosage should be determined by decreasing the initial dosage in small amounts to the lowest dosage that maintains an adequate clinical response.
Patients should be observed closely for signs that might require dosage adjustment, including changes in clinical status resulting from remissions or exacerbations of the disease, individual drug responsiveness, and the effect of stress (e.g., surgery, infection, trauma). During stress it may be necessary to increase dosage temporarily.
If the drug is to be stopped after more than a few days of treatment, it usually should be withdrawn gradually.
How is Cortisone Acetate supplied
Cortisone Acetate Tablets, USP 25 mg: white to off-white, round scored tablets, debossed with “C” bisect “E” on one side and “113” on the other side.
Bottles of 30 tablets. NDC 62135-173-30
Store at 20° to 25°C (68° to 77°F) [See USP Controlled Room Temperature]. Protect from light and moisture.
Preserve in well closed containers, as defined in the USP.
Manufactured for:
Chartwell RX, LLC.
Congers, NY 10920
L71189
Revised 06/2024
| CORTISONE ACETATE
cortisone acetate tablet |
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
| Labeler - Chartwell RX, LLC (079394054) |
Frequently asked questions
- What are the side effects of steroids?
- What is the difference between hydrocortisone and cortisone?
- How long do the effects of a cortisone injection shot last?
More about cortisone
- Check interactions
- Compare alternatives
- Pricing & coupons
- Reviews (7)
- Drug images
- Side effects
- Dosage information
- During pregnancy
- Support group
- Drug class: glucocorticoids
- Breastfeeding
- En español


