Uveitis
Medically reviewed by Drugs.com. Last updated on Feb 18, 2024.
What is uveitis?

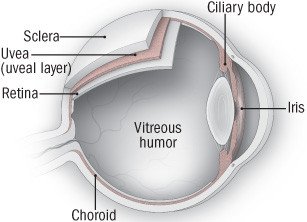
Uveitis means inflammation of the part of the eye called the uvea. The uvea, also called the uveal tract, is a continuous layer of fibrous tissue that surrounds the eye. It is made up of three structures:
- The iris — the donut-shaped part that gives the eye its color
- The choroid — a membrane full of tiny blood vessels that lines the eye
- The ciliary body — a thick ring of tissue that helps control the shape of the lens, and is attached to the iris and to the front portion of the choroid.
|
|
Various terms are used for the condition, depending on the part of the uvea affected. They include:
- anterior uveitis (iritis) — affects the front portion of the uvea, the iris
- iridocyclitis — affects the iris and the ciliary body
- intermediate uveitis (also called pars planitis) — affects the middle portion of the uvea, between the retina and the ciliary body
- posterior uveitis (choroiditis) — affects the back part of the uvea, the choroids
- diffuse uveitis — inflammation of all portions of the uvea.
The most common types of uveitis are anterior uveitis and iridocyclitis. Posterior uveitis is rare.
Many cases of uveitis are related to an autoimmune disorder (such as ankylosing spondylitis, lupus, juvenile idiopathic arthritis, multiple sclerosis or sarcoidosis) or an infection, such as tuberculosis, toxoplasmosis, herpes, syphilis or cytomegalovirus (especially in patients with AIDS).
A number of conditions, including pars planitis, birdshot choroidopathy and sympathetic ophthalmia, are diseases of the eye that may cause uveitis but usually do not affect other parts of the body.
Rarely, uveitis occurs as a side effect of a medication. In up to half of cases, the cause is not known, but recent research has linked certain genes to the development of the disease. One possibility is that some people are prone to uveitis because they have genes that program the immune system to attack the uvea, a process that may be triggered by an infection.
Symptoms of uveitis
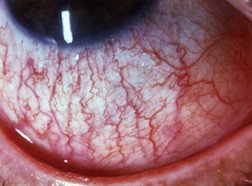
Symptoms of uveitis can vary depending on the location of the inflammation. Severe symptoms generally are associated with anterior uveitis, and can include:
- eye pain
- eye redness
|
|
- sensitivity to light
- blurred or decreased vision.
Intermediate and posterior uveitis can have more subtle symptoms, including small specks or clouds that move in your field of vision, called floaters, and decreased vision.
Diagnosing uveitis
If your physician suspects you have uveitis, you are likely to be referred to an ophthalmologist (eye specialist), who will give you a thorough eye exam, including:
- tests of visual acuity, to determine if vision has decreased. This can be as simple as reading an eye chart.
- a funduscopic exam, in which the pupil is dilated (widened) so that the ophthalmologist can look into the eye and see structures at the back of the eye.
- measures of the pressure inside the eye to make sure it has not reached high levels that might be dangerous. This painless test involves an instrument called a tonometer that either blows a puff of air or lightly presses on the surface of the eye and measures how the surface of the eye responds.
- a slit-lamp exam, in which a narrow beam of light is shone into the eye so that a magnifying lens can closely examine the highlighted portion of the eye. Your doctor will use eye drops to dilate the pupil of the eye. A drop of fluorescein dye may be placed in the eye. This dye temporarily stains the surface of the eye and can help to determine which layers of the eye are inflamed.
In addition, your physician probably will ask you about your medical history, and will examine you. Depending on the results, he or she may order blood tests and X-rays (such as a chest X-ray to look for evidence of sarcoidosis). Because uveitis often is associated with a viral infection or an autoimmune disease, other conditions need to be discovered and treated as well.
Expected duration of uveitis
With treatment, most people with uveitis will improve within days or weeks. However, the condition may last longer, especially if related to an autoimmune disease or untreated infection. Chronic (long-term) forms of the disease can be very difficult to cure and may return. If you have been treated successfully for uveitis, you should expect to have follow-up visits to your doctor every one to six months to make sure that the disease remains stable.
Preventing uveitis
Avoiding medications that may cause uveitis and avoiding certain infections, including syphilis or HIV, may prevent uveitis. For other type of uveitis, there is no known way to prevent the condition.
Drugs used to treat this and similar conditions
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Treating uveitis
Treatment of uveitis focuses on reducing inflammation and relieving pain. If you have an infection, your doctor will prescribe antibiotics for a bacterial infection, or antiviral medications if due to a virus. For noninfectious uveitis, treatment will usually include prescription eye drops or ointments containing corticosteroids to reduce inflammation. If uveitis affects the iris, eye drops that dilate the pupil also may be prescribed so that the iris won't move and cause pain. Your doctor may recommend sunglasses because bright light may cause discomfort.
For more severe cases, your ophthalmologist may recommend injections of corticosteroids into the eye, oral forms of corticosteroids, or additional immunosuppressive medications. Examples of immunosuppressive therapies used in the treatment of uveitis include methotrexate, cyclosporine, tacrolimus, azathioprine, and mycophenolate mofetil. More recently, options available to treat people with severe uveitis that does not respond to other therapies include adalimumab, infliximab, or steroid implants surgically inserted into the eye.
Any complications of uveitis, such as glaucoma or cataracts, also will need to be treated. For many patients, a team of physicians will be involved, including a general medical physician, an ophthalmologist, and sometimes other specialists (for example, an infectious disease expert or a rheumatologist).
When to call a professional
See your health care professional if you experience blurred vision, pain in one or both eyes, sensitivity to light, or eye redness.
Prognosis
The outlook varies, depending on the type of uveitis, its severity and duration, whether it responds promptly to treatment and whether there is an associated illness. When diagnosed and treated promptly, the prognosis is generally good, and patients can expect to recover eventually. Left untreated, the complications of uveitis can be serious, and may include glaucoma, cataracts or permanent loss of vision.
Additional info
American Academy of Ophthalmology
www.aao.org
National Eye Institute
www.nei.nih.gov
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.