Glaucoma
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is glaucoma?
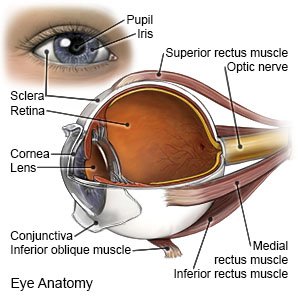
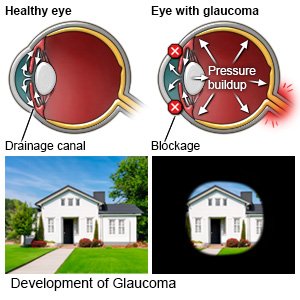
Glaucoma is an eye disease that causes vision loss in one or both eyes. Glaucoma is usually caused by fluid buildup behind the eye. This puts pressure on your optic nerve and damages it. The 2 main types are open-angle and closed-angle glaucoma. Fluid normally drains through canals in the eyes. The fluid contains deposits that get left behind in the canals as the fluid drains. Over time, the deposits create a blockage that keeps fluid from draining easily through the canals. Open-angle means the blockage cannot be seen in tests. Closed-angle means the blockage can be seen.
 |
What increases my risk for glaucoma?
- Being farsighted or nearsighted
- Age older than 40
- Being female
- Family history of glaucoma
- Certain medicines, such as antidepressants, antihistamines, or corticosteroids
- Medical conditions such as diabetes, hypothyroidism, or high blood pressure
- Severe eye injury
- Abnormal eye structures, such as a thick cornea
- Obstructive sleep apnea
What are the signs and symptoms of glaucoma?
- Open-angle glaucoma usually affects both eyes. Signs and symptoms may be worse in 1 eye. Any of the following may develop slowly over time:
- Blind spots or areas of vision loss that get larger over time and combine
- Loss of peripheral (side) vision
- Only seeing clearly when you look straight ahead
- Closed-angle glaucoma may cause any of the following in one or both eyes, and may happen suddenly:
- Vision loss or blurred vision
- Eye pain that may be severe
- Headaches that may get better when you sleep
- Trouble seeing at night
- Halos or rainbows around lights
 |
How is glaucoma diagnosed?
Your healthcare provider will ask about your symptoms and examine your eyes. He or she will check your peripheral vision. He or she may check how well your eyes drain fluid. Your pupils may be dilated (widened) for some of the following tests:
- A tonometry test is used to measure your eye pressure. Your eyes are numbed with eyedrops and your healthcare provider touches your eyes with an instrument. A puff of air may instead be blown into your eyes and pressure is measured with a light.
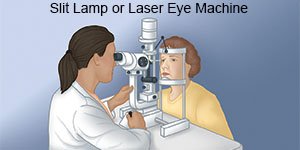
- A slit-lamp exam helps your healthcare provider have a better view of the inside of your eye. Your provider will shine a bright light in your eye to check for inflammation.
- An ophthalmoscope is used to check for optic nerve damage. Your healthcare provider will turn off the lights in the room and shine a bright light in your eyes.
Related medications
How is glaucoma treated?
The goal of treatment is to reduce eye pressure and prevent damage to your optic nerve. You may need any of the following:
- Eye pressure medicines help decrease eye pressure. They may also decrease the amount of fluid your eyes make or help your eyes drain better.
- Laser surgery may be needed if other treatments do not work. Healthcare providers use a laser to open your eye drainage system or create a new opening for eye fluid to drain.

Treatment options
The following list of medications are related to or used in the treatment of this condition.
What can I do to manage glaucoma?
- Get regular eye exams. This will help healthcare providers monitor your glaucoma.
- Avoid behaviors that increase eye pressure. Try not to strain when you have a bowel movement. Do not wear tight clothing around your neck or chest. Do not push or lift anything heavier than 5 pounds. Avoid strenuous activity.
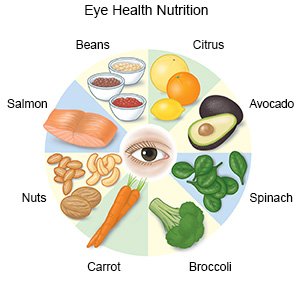
- Eat foods that are healthy for your eyes. Certain foods help get more blood to vessels in your eyes. An example is leafy green vegetables, such as fresh spinach. Your healthcare provider or a dietitian can help you create meals plans.
- Carry medical alert identification. Wear medical alert jewelry or carry a card that says you have glaucoma. Ask your healthcare provider where to get these items.
When should I seek immediate care?
- You have a sudden loss of vision.
- You have blurry vision and a severe headache.
- You have severe eye pain or a change in your vision.
- You have nausea and are vomiting, along with vision changes.
When should I call my doctor?
- Your symptoms get worse, even after treatment.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Glaucoma
Treatment options
- Medications for Glaucoma
- Medications for Glaucoma, Narrow Angle
- Medications for Glaucoma/Intraocular Hypertension
Symptoms and treatments
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
