Vesicovaginal Fistula Repair
Medically reviewed by Drugs.com. Last updated on Sep 23, 2025.
AMBULATORY CARE:
What you need to know about a vesicovaginal fistula repair:
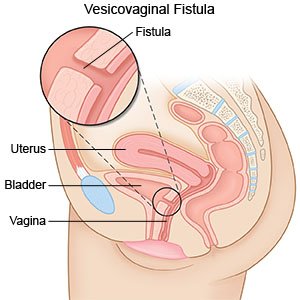
Vesicovaginal fistula repair is surgery to close or remove a fistula between your bladder and vagina. A fistula is an abnormal tissue connection or hole. When you have a fistula, urine exits your body through your vagina, and you cannot control the flow of urine.
 |
How to prepare for surgery:
Your healthcare provider will talk to you about how to prepare for surgery. He or she may tell you not to eat or drink anything after midnight on the day of your surgery. Your provider may tell you to shower the night before your surgery. He or she may tell you to use a certain soap to help prevent a surgical site infection. Your provider will tell you what medicines to take or not take on the day of your surgery. Arrange to have someone drive you home and stay with you after surgery.
What will happen during surgery:
- You will be given general anesthesia to keep you asleep and free from pain during surgery. You may also be given an antibiotic to help prevent an infection. Your surgeon may insert a scope through your urethra to check the location of your fistula. A stent will be placed in each ureter to protect them during surgery. Your surgeon will make an incision around the fistula. The fistula will be cut out or sewn closed. The outside walls of your vagina and bladder will be separated. Your surgeon will close the incision with stitches. Bandages soaked with antibiotic medicine may be placed in your vagina to help prevent infection.
- If your surgery is done through your abdomen, your surgeon will make an incision under your belly button. The wall of your bladder will be cut away from your vagina and the fistula removed. Your surgeon may put a suprapubic catheter through your abdomen and into your bladder before it is closed. The catheter is used to drain your urine and may stay in place for up to 3 weeks. You may also need a drain to remove extra blood and fluid. The incision will be closed with stitches.
Risks of surgery:
You may bleed more than expected or get an infection. Your ureters may be damaged. You may have bladder spasms and vaginal bleeding. You may develop bladder stones or not be able to empty your bladder completely. You may still leak urine or have urges to urinate often. Surgery may make your bladder smaller or shorten your vaginal canal. Even after having surgery to remove your fistula, a new fistula may form.
Call your local emergency number (911 in the US) if:
- You have trouble breathing.
Related medications
Call your doctor if:
- Blood soaks through your bandage.
- You are bleeding from your vagina and it is not your monthly period.
- You have a catheter and no urine is draining into the bag.
- You have a fever or chills.
- You have a burning or pain when you urinate.
- You are leaking urine from your vagina.
- You have yellow or bad smelling discharge from your vagina.
- Your wound is red, swollen, or draining pus.
- You have questions or concerns about your condition or care.
Medicines:
You may need any of the following:
- Medicines may help relax your bladder and prevent spasms.
- Prescription pain medicine may be given. Ask your how to take this medicine safely.
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. This medicine is available with or without a doctor's order. NSAIDs can cause stomach bleeding or kidney problems in certain people. If you take blood thinner medicine, always ask your healthcare provider if NSAIDs are safe for you. Always read the medicine label and follow directions.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Care for your catheter:
Keep the bag below your waist. This will prevent urine from flowing back into your bladder and causing an infection or other problems. Also, keep the tube free of kinks so the urine will drain properly. Do not pull on the catheter. This can cause pain and bleeding and may cause the catheter to come out. Empty your urine drainage bag when it is ½ to ⅔ full, or every 8 hours. If you have a smaller leg bag, empty it every 3 to 4 hours. Do the following when you empty your urine drainage bag:
- Hold the urine bag over a toilet or large container.
- Remove the drain spout from its sleeve at the bottom of the urine bag. Do not touch the tip of the drain spout. Open the slide valve on the spout.
- Let the urine flow out of the urine bag into the toilet or container. Do not let the drainage tube touch anything.
- Clean the end of the drain spout with alcohol when the bag is empty.
- Close the slide valve and put the drain spout into its sleeve at the bottom of the urine bag.
- Write down how much urine was in your bag if you were asked to keep a record.
Drink liquids as directed:
Ask how much liquid to drink each day and which liquids are best for you. Liquids help flush the blood from surgery out of your bladder through your urine.
Do not have sex or use tampons for at least 3 months after surgery:
This allows the tissues in your vagina to heal.
Follow up with your healthcare provider as directed:
You may need to return to have your stitches or catheter removed. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
