Urinary Sphincter Replacement
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
WHAT YOU NEED TO KNOW:
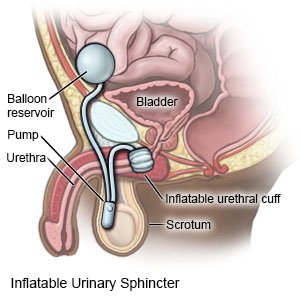
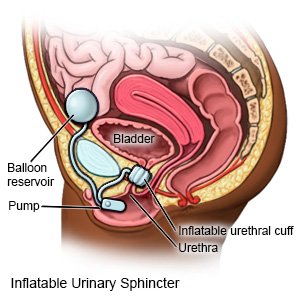
Urinary sphincter replacement is surgery to replace your urinary sphincter with an artificial urinary sphincter (AUS). The urinary sphincter is a muscle that surrounds your urethra. The sphincter squeezes the urethra to keep urine in the bladder until it is time to urinate. An AUS device has a balloon reservoir, a cuff, and a pump. When the AUS is turned on, liquid inside the balloon flows into the cuff. When the cuff is filled, it squeezes your urethra to prevent urine from leaking out of your bladder. To urinate, you press the pump. This relaxes the cuff and allows urine to flow out of your bladder.
 |
 |
HOW TO PREPARE:
Before your surgery:
- Arrange to have someone drive you home when you are discharged.
- Tell your surgeon about all medicines you currently take. He or she will tell you if you need to stop any medicine for surgery, and when to stop. He or she will tell you which medicines to take or not take on the day of your surgery.
- You may need blood or urine tests. You may also need an MRI or cystoscopy.
- You may meet with a healthcare provider to talk about what to expect after your surgery. The healthcare provider will show you how to use the AUS.
The night before your surgery:
You may be told not to eat or drink anything after midnight.
The day of your surgery:
- You or a close family member will be asked to sign a legal document called a consent form. It gives healthcare providers permission to do the procedure or surgery. It also explains the problems that may happen, and your choices. Make sure all your questions are answered before you sign this form.
- Take only the medicines your surgeon told you to take.
- An IV will be placed into a vein. You may be given medicine or liquid through the IV.
- An anesthesiologist will talk to you before your surgery. You may need medicine to keep you asleep or numb an area of your body during surgery. Tell healthcare providers if you or anyone in your family has had a problem with anesthesia in the past.
- A sample of your urine will be tested to check for a urinary tract infection.
WHAT WILL HAPPEN:
What will happen:
- An incision will be made to reach your urethra. For men, the incision will be made in the scrotum or perineum (area between the penis and anus). For some men, the entire surgery may be done through the incision in the scrotum. For women, the incision will be made in the abdomen or vagina.
- Your surgeon will measure your urethra to choose the correct AUS cuff size. He or she will place the AUS cuff around your urethra. A small incision may be made in your lower abdomen to place the balloon reservoir. Tubing connected to the balloon reservoir is tunneled through your abdomen to reach the AUS pump.
- For men, the AUS pump will be placed in the scrotum. Tubing from the cuff is often tunneled down into the scrotum. For women, the pump is placed in the labia (skin folds found on each side of the vagina). Tubing from the cuff and the balloon reservoir will be connected to the pump. Your surgeon will check the pump to see that it works properly. Then he or she will turn the pump off. Your incisions will be stitched closed and covered with bandages.
After your surgery:
You will be taken to a room to rest until you are fully awake. Healthcare providers will monitor you closely for any problems. Do not get out of bed until your healthcare provider says it is okay. When your healthcare provider sees that you are okay, you will be able to go home or be taken to your hospital room.
CONTACT YOUR HEALTHCARE PROVIDER IF:
- You have a fever.
- You get a cold or the flu.
- You have questions or concerns about your surgery.
Risks
You may bleed more than expected or develop an infection. You may have trouble urinating after the surgery. Your urethra, bladder, or nearby tissues may be damaged. Women may have bruising or damage to the labia or vagina. Men may have bruising or damage to the scrotum. If your AUS becomes infected, it may need to be removed. Your urethra may be damaged by the pressure from the AUS cuff. The cuff may break down, or the tubing may become blocked. The AUS may not work and you may continue to leak urine. You may need another surgery to fix or replace the AUS.
Related medications
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
