Opioid Safety
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What do I need to know about opioid safety?
Safety includes the correct use, storage, and disposal of opioids. Examples of opioid pain medicines are oxycodone, morphine, fentanyl, and codeine.
How are opioids given?
Opioids can be given as a pill, patch, or suppository. They can also be given as an injection into a vein, near a nerve, or into a joint. Your prescription may include one or both of the following:
- Short-acting opioids work fast and relieve pain for about 3 to 6 hours. They are often used for acute or breakthrough pain.
- Long-acting opioids usually last at least 8 hours. You can take them less often and they may be used for chronic pain.
How do I use opioids safely?
- Take prescribed opioids exactly as directed. Opioids come with directions based on the kind and how it is given. Talk to your healthcare provider or a pharmacist if you have any questions. Do not take more than the recommended amount. Too much can cause life-threatening poisoning. Do not crush, split, or dissolve opioid pills. These actions increase the risk for opioid poisoning.
- Do not continue a prescribed opioid after your pain stops. You may develop tolerance. This means you keep needing higher doses to get the same effect. You may also develop opioid use disorder. This means you are not able to control your opioid use. Your provider will help you make a plan to stop the opioid safely.
- Do not give opioids to others or take opioids that belong to someone else. The kind or amount one person takes may not be right for another. The person you share them with may also be taking medicines that do not mix with opioids. The person may drink alcohol or use other drugs that can cause life-threatening problems when mixed with opioids.
- Do not mix opioids with other medicines or alcohol. The combination can cause poisoning, or cause you to stop breathing. Alcohol, sleeping pills, and medicines such as antihistamines can make you sleepy. A combination with opioids can lead to a coma.
- Do not drive or operate heavy machinery after you use an opioid. You may feel drowsy or have trouble concentrating. You can injure yourself or others if you drive or use heavy machinery when you are not alert. Your provider or pharmacist can tell you how long to wait after a dose before you do these activities.
- Talk to your healthcare provider if you have any side effects. Side effects include nausea, sleepiness, itching, and trouble thinking clearly. Your provider may need to make changes to the kind or amount of opioid you are taking. Your provider can also help you find ways to prevent or relieve side effects.
What can I do to manage constipation?
Constipation is the most common side effect of opioid medicine. Constipation is when you have hard, dry bowel movements, or you go longer than usual between bowel movements. Tell your healthcare provider about all changes in your bowel movements while you are taking opioids. Your provider may recommend laxative medicine to help you have a bowel movement. Your provider may also change the kind of opioid you are taking, or change when you take it. The following are more ways you can prevent or relieve constipation:
- Drink liquids as directed. You may need to drink extra liquids to help soften and move your bowels. Ask how much liquid to drink each day and which liquids are best for you.
- Eat high-fiber foods. This may help decrease constipation by adding bulk to your bowel movements. High-fiber foods include fruits, vegetables, whole-grain breads and cereals, and beans. Your healthcare provider or dietitian can help you create a high-fiber meal plan. Your provider may also recommend a fiber supplement if you cannot get enough fiber from food.

- Exercise regularly. Regular physical activity can help stimulate your intestines. Walking is a good exercise to prevent or relieve constipation. Ask which exercises are best for you.

- Schedule a time each day to have a bowel movement. This may help train your body to have regular bowel movements. Bend forward while you are on the toilet to help move the bowel movement out. Sit on the toilet for at least 10 minutes, even if you do not have a bowel movement.
How do I store opioids safely?
- Store opioids where others cannot easily get them. Keep them in a locked cabinet or secure area. Do not keep them in a purse or other bag you carry with you. A person may be looking for something else and find the opioids.
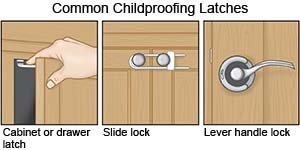
- Make sure opioids are stored out of the reach of children. A child can easily have opioid poisoning. Opioids may look like candy to a small child.
Related medications
What is the best way to dispose of opioids?
The laws vary by country and area. In the United States, the best way is to return the opioids through a take-back program. This program is offered by the US Drug Enforcement Agency (DEA). The following are options for using the program:
- Take the opioids to a DEA collection site. The site is often a law enforcement center. Call your local law enforcement center for scheduled take-back days in your area. You will be given information on where to go if the collection site is in a different location.
- Take the opioids to an approved pharmacy or hospital. A pharmacy or hospital may be set up as a collection site. You will need to ask if it is a DEA collection site if you were not directed there. A pharmacy or doctor's office may not be able to take back opioids unless it is a DEA site.
- Use a mail-back system. This means you are given containers to put the opioids into. You will then mail them in the containers.
- Use a take-back drop box. This is a place to leave the opioids at any time. People and animals will not be able to get into the box. Your local law enforcement agency can tell you where to find a drop box in your area.
What are some other safe ways to dispose of opioids?
The medicine may come with disposal instructions. The instructions may vary depending on the brand of medicine you are using. Instructions may come in a Medication Guide, but not every medicine has one. You may instead get instructions from your pharmacy or doctor. Follow instructions carefully. The following are general guidelines to follow:
- Find out if you can flush the opioid. Some opioids can be flushed down the toilet or poured into the sink. You will need to contact authorities in your area to see if this is an option for you. The FDA also offers a list of medicines that are safe to flush down the toilet. You can check the list if you cannot get the information for your local area.
- Ask your waste management company about rules for putting opioids in the trash. The company will be able to give you specific directions. Scratch out personal information on the original medicine label so it cannot be read. Then put it in the trash. Do not label the trash or put any information on it about the opioids. It should look like regular household trash so no one is tempted to look for the opioids. Keep the trash out of the reach of children and animals. Always make sure trash is secure.
- Talk to officials if you live in a facility. If you live in a nursing home or assisted living center, talk to an official. The person will know the rules for your area.
What are some other ways to manage pain?
- Ask your healthcare provider about non-opioid medicines to control pain. Some medicines may even work better than opioids, depending on the cause of your pain. Nonprescription medicines include NSAIDs (such as ibuprofen) and acetaminophen. Prescription medicines include muscle relaxers, antidepressants, and steroids.
- Pain may be managed without any medicines. Some ways to relieve pain include massage, aromatherapy, or meditation. Physical or occupational therapy may also help.
Where can I find more information?
- Drug Enforcement Administration
8701 Morrissette Drive
Springfield , VA 22152
Phone: 1- 800 - 882-9539
Web Address: https://www.deadiversion.usdoj.gov/drug_disposal/
- US Food and Drug Administration
10903 New Hampshire Avenue
Silver Spring , MD 20993
Phone: 1- 888 - 463-6332
Web Address: http://www.fda.gov
Call your local emergency number (911 in the US), or have someone call if:
- You have a seizure.
- You cannot be woken.
- You have trouble staying awake and your breathing is slow or shallow.
- Your speech is slurred, or you are confused.
- You are dizzy or stumble when you walk.
When should I or someone close to me call my doctor?
- You are extremely drowsy, or you have trouble staying awake or speaking.
- You have pale or clammy skin.
- You have blue fingernails or lips.
- Your heartbeat is slower than normal.
- You cannot stop vomiting.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
