Moderate and Severe Persistent Asthma
Medically reviewed by Drugs.com. Last updated on Sep 23, 2025.
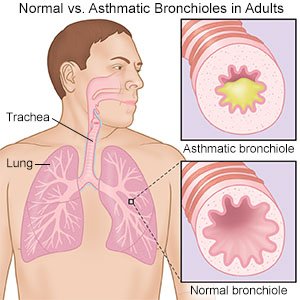
Moderate or severe persistent asthma means you have asthma symptoms every day. You may also need to use your rescue inhaler daily to treat shortness of breath. Your normal activities are affected by wheezing, shortness of breath, or chest tightness. You have frequent flare-ups when your symptoms become worse. Flare-ups at night can affect your sleep and happen at least 1 time each week.
 |
DISCHARGE INSTRUCTIONS:
Call your local emergency number (911 in the US) if:
- You have severe shortness of breath.
- The skin around your neck and ribs pulls in with each breath.
- Your peak flow numbers are in the red zone of your AAP.
Seek care immediately if:
- You have shortness of breath, even after you take your short-term medicine as directed.
- Your lips or nails turn blue or gray.
Related medications
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Call your doctor or asthma specialist if:
- You run out of medicine before your next refill is due.
- Your symptoms get worse.
- You need to take more medicine than usual to control your symptoms.
- You have questions or concerns about your condition or care.
Medicines:
- Medicines help decrease inflammation in your lungs, open your airways, and make it easier to breathe. You may need to use medicine to relieve your symptoms quickly during an attack. You may also need long-term medicine to help prevent future attacks. The medicines may be injected, inhaled, or given as a pill. Some medicines may help control your allergies. Other medicines may be needed if your regular medicines are not able to prevent attacks. Ask your asthma specialist for more information about the medicine you are given and how to take it safely.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Manage persistent asthma:
- Check your oxygen level, if directed. Your healthcare provider may recommend you use a pulse oximeter (pulse ox). A pulse ox is a device that measures the amount of oxygen in your blood. You may be given an oxygen level goal for when you are at rest and another goal for activity.

- Follow your asthma action plan. This is a written plan that you and your asthma specialist create. It explains which medicine you need and when to change doses if necessary. It also explains how you can monitor symptoms and use a peak flow meter. The meter measures how well air moves out of your lungs.
- Identify and avoid triggers. Keep your home free of pets, dust mites, cockroaches, and mold.
- Manage other health conditions , such as allergies, sinus problems, sleep apnea, or acid reflux.
- Do not smoke, and avoid others who smoke. Nicotine and other chemicals in cigarettes and cigars can cause lung damage. Ask your doctor for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your doctor before you use these products.
- Ask about the flu vaccine. The flu can make your asthma worse. You may need a yearly flu shot.
Follow up with your asthma specialist as directed:
You may need more tests to see how well your treatment is working. You may be asked to write down your peak flow values and bring them to your visits. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Moderate and Severe Persistent Asthma
Treatment options
Care guides
- Asthma
- Asthma in Children
- COPD (Chronic Obstructive Pulmonary Disease)
- Exercise-Induced Bronchoconstriction
- Moderate and Severe Persistent Asthma
- Reactive Airways Disease
Symptoms and treatments
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
