Asthma in Children
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is asthma?
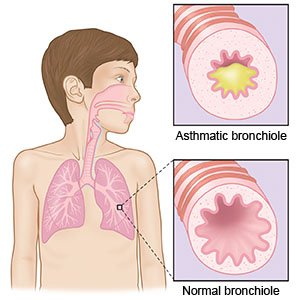
Asthma is a condition that causes breathing problems. Inflammation and narrowing of your child's airway prevents air from getting to his or her lungs. An asthma attack is when your child's symptoms get worse. If your child's asthma is not managed, symptoms may become chronic or life-threatening.
 |
What is cough-variant asthma?
Cough-variant asthma is a type of asthma with symptoms of a dry cough that comes and goes. A dry cough may be your child's only symptom, or he or she may also have chest tightness. Your child's cough may be worse at night. These symptoms may be caused by exercise or exposure to odors, allergens, or respiratory infections. Cough-variant asthma is treated the same way as typical asthma.
What are the signs and symptoms of asthma in children?
- Coughing
- Wheezing
- Shortness of breath
- Fast breathing in infants
- Chest tightness
What may trigger an asthma attack?
- A sinus infection, cold, or the flu
- Exercise
- Intense crying, laughing, or yelling
- Cold air, or a change in weather temperature
- Air pollution or pollen
- Tobacco smoke
- Acid reflux
- Pets, fur, dust mites, cockroaches, or mold
How is asthma in children diagnosed?
Tell your child's pediatrician if your child has a family history of asthma. Tell the provider about your child's symptoms and what you think may trigger symptoms. The provider will examine your child and listen to his or her lungs. Your child may need to be tested for allergies that could trigger asthma attacks. He or she may also need the following:
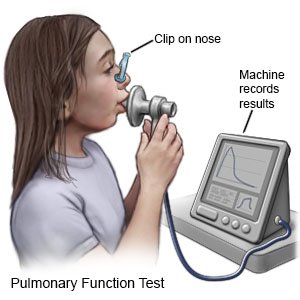
- Pulmonary function tests (PFTs) are done to show how well your child can breathe.
- A chest x-ray is used to check for other lung problems such as an infection.
Related medications
How is asthma in children treated?
Treatment depends on your child's age and how well his or her asthma is controlled. The cause of your child's asthma, such as acid reflux, may need to be treated. Your child may need any of the following:
- Medicines decrease inflammation, open your child's airway, and make breathing easier. Your child may need rescue medicine that works quickly during an attack. He or she may also need long-acting medicine that works over time to prevent asthma attacks. Other medicines may be needed if your child's regular medicines are not able to prevent attacks. Asthma medicine may be inhaled, taken as a pill, or injected.
- Allergy testing may be used to find allergies that trigger an asthma attack. Your child may need allergy shots or medicine to control allergies that make his or her asthma worse.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
What is an Asthma Action Plan (AAP)?
An AAP is a written plan to help you manage your child's asthma. It is created with your child's pediatrician. Give the AAP to all of your child's care providers. This includes your child's teachers and school nurse. An AAP contains the following information:
- A list of what triggers your child's asthma
- How to keep your child away from triggers
- When and how to use a peak flow meter
- What your child's peak numbers are for the Green, Yellow, and Red Zones
- Symptoms to watch for and how to treat them
- Names and doses of medicines, and when to use each medicine
- Emergency telephone numbers and locations of emergency care
- Instructions for when to call the doctor and when to seek immediate care
What else can I do to manage my child's asthma?
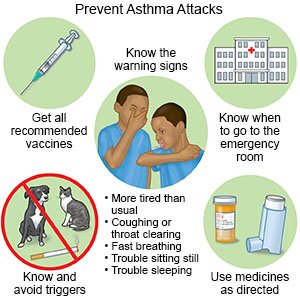 |
- Keep a diary of your child's asthma symptoms. This will help identify asthma triggers so you can keep your child away from them.
- Do not smoke near your child. Do not smoke in your car or anywhere in your home. Do not let your older child smoke. Nicotine and other chemicals in cigarettes and cigars can make your child's asthma worse. Ask your child's pediatrician for information if you or your child currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your child's pediatrician before you or your child use these products.
- Manage your child's other health conditions. This includes allergies and acid reflux. These conditions can make your child's symptoms worse.
- Ask about vaccines your child may need. Vaccines can help prevent infections that could worsen your child's symptoms. Your child may need a yearly flu vaccine.
Call your local emergency number (911 in the US) if:
- Your child has severe shortness of breath.
- The skin around your child's neck and ribs pulls in with each breath.
- Your child's peak flow numbers are in the red zone of his or her AAP.
When should I seek immediate care?
- Your child has shortness of breath, even after he or she takes short-term medicine as directed.
- Your child's lips or nails turn blue or gray.
When should I call my child's doctor?
- You run out of medicine before your child's next refill is due.
- Your child's symptoms get worse.
- Your child needs to take more medicine than usual to control his or her symptoms.
- You have questions or concerns about your child's condition or care.
Care Agreement
You have the right to help plan your child's care. Learn about your child's health condition and how it may be treated. Discuss treatment options with your child's healthcare providers to decide what care you want for your child. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Asthma
Treatment options
Care guides
- Asthma
- COPD (Chronic Obstructive Pulmonary Disease)
- Exercise-Induced Bronchoconstriction
- Moderate and Severe Persistent Asthma
- Reactive Airways Disease
Symptoms and treatments
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
