Colostomy Creation
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
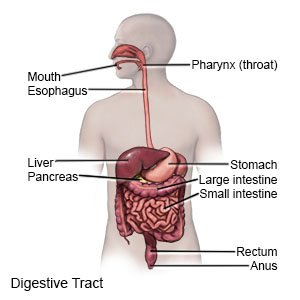
Colostomy creation
is surgery to remove parts of your colon that are injured or diseased. The surgery brings part of your colon (bowel) to the surface of your abdomen. This creates a small opening in your abdomen called a stoma. Bowel movements pass through the stoma and into a pouch that is attached to your abdomen.
 |
Types of colostomy:
Your healthcare provider will choose a colostomy type based on the reasons for the surgery and your general health. Types of colostomies include the following:
- An ascending colostomy has the stoma placed on the right side of your abdomen. Liquid bowel movements pass through the stoma.
- A transverse colostomy has the stoma placed in your upper abdomen on the middle or right side. Bowel movements that pass through the stoma are loose or soft. Sometimes you will have 2 stomas next to each other. This is called a loop colostomy. One stoma will pass bowel movements and the other may pass mucus.
- A descending or sigmoid colostomy has the stoma placed on the lower left side of your abdomen. Firm bowel movements pass through the stoma.
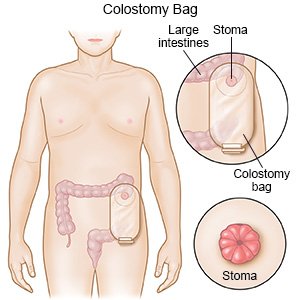
What will happen when you meet with an ostomy specialist:
Bring a family member or friend with you to learn how to help you. Write down any questions you may have so you will remember to ask them during your meetings.
- The ostomy specialist will talk with you about lifestyle changes that happen with a colostomy.
- The specialist will explain how to prevent problems such as bowel movement leakage. You will learn stoma care to prevent a rash or infection around the stoma.
- The specialist will talk about the supplies you will need for your colostomy. The specialist will show you how to change the ostomy bag. You will also be shown how to irrigate the colostomy. Irrigation is a procedure to empty your bowel by putting liquid into your stoma.
- The specialist may also talk about your nutrition, bathing, and other activities after surgery.
- You may meet other people who have a colostomy.
How to prepare for your surgery:
- In the weeks before your surgery you will need to do the following:
- Stop taking blood thinning medicines. This includes NSAIDs, such as ibuprofen and aspirin. Your healthcare provider will tell you other medicines to stop taking.
- Meet with your surgeon or ostomy specialist. Your surgeon or specialist will talk with you about the best place for your stoma. A pen or a small disc is used to mark the stoma site on your abdomen. Your surgeon or specialist will ask you to sit, lie down, stand, and bend. This helps position the stoma to prevent leaks and skin problems. It will also help your stoma better fit your clothes and ostomy bag.
- You may be given an antibiotic to prevent an infection. You may need to begin the antibiotic a few days before your surgery.
- Healthcare providers will tell you to stop eating solid foods for 2 to 3 days before surgery. This helps empty your colon before surgery. Ask which foods and drinks are okay. You may be told not to eat raw vegetables or meats such as beef or pork.
- You may be able to only have clear liquids the day before your surgery. You may need a laxative or enema to completely clean out your colon the night before surgery.
What will happen during your surgery:
- General anesthesia will keep you asleep and pain-free during the surgery. For open surgery, your surgeon will make 1 long incision in the middle of your abdomen. For laparoscopic surgery, 3 to 4 small incisions are made on your abdomen. The laparoscopic tools are placed inside the incisions, and your abdomen is filled with carbon dioxide (a gas). The gas lifts the abdominal muscles away from the colon and other organs during surgery. Your surgeon will cut through the muscles in your abdomen to the colon. Your surgeon will carefully check your colon for disease or injury.
- Your surgeon will cut your colon into 2 or more parts. Diseased or injured parts of your colon may be removed. One end of your colon will be pushed through an opening on your abdomen. The end will be stitched to the skin on your abdomen to create a stoma. The other part of your colon may be stitched closed or a second stoma will be made. You may have a rod placed under the stoma to keep it above your skin if the colostomy has 2 openings. The other incisions are closed with stitches or staples. Your surgeon will attach a pouch around your stoma to collect fluids and bandage your incisions.
- Your rectum and anus may be removed. This will leave a surgery area called a posterior wound. You will have bandages or pads to collect any drainage from the wound.
What to expect after your surgery:
You will be monitored until you are fully awake. You will have to stay in the hospital for up to a week. During your stay you will learn how to take care of your stoma and the skin around it. You will also learn how to use the ostomy supplies.
Risks of colostomy creation:
- The condition that led to your colostomy may come back, even with treatment. You may develop an infection or bleed more than expected. Surgery may damage nerves or other organs. You may develop a life-threatening blood clot.
- Your stoma may narrow, become blocked, or move too far outside or inside your abdomen. You may develop a hernia (weakness in the muscles in your abdomen). Sometimes the stoma tissue does not get enough blood and the tissue may die. A colon incision may come apart or leak bowel movement fluid into your abdomen. This can cause a life-threatening infection. More surgery and other treatments are needed right away to correct these problems.
Call your local emergency number (911 in the US) if:
- You feel lightheaded, short of breath, and have chest pain.
- You cough up blood.
Related medications
Seek care immediately if:
- You are urinating very little or not at all.
- No bowel movement is passing through your stoma.
- You have pus or a foul-smelling odor coming from your surgery wound or stoma.
- You vomit blood, are bleeding from your stoma, or see blood in your bowel movement. Your bowel movement may look like tar.
- Your abdomen feels hard and tender.
- Your stoma looks gray, purple, dark brown or black.
- Your arm or leg feels warm, tender, and painful. It may look swollen and red.
Call your surgeon or ostomy specialist if:
- You have nausea or are vomiting.
- You have a temperature of 101ºF (38.3ºC) or higher.
- More bowel movement is draining from your stoma than normal. Your bowel movement may look watery or smell very bad.
- The skin around your stoma is red, sore, itchy, swollen, or has a rash.
- Your stoma opening has narrowed or you have drainage from around your stoma.
- Your stoma has moved farther inside or outside of your abdomen. You see bulges under the skin around your stoma.
- You have questions or concerns about your stoma, surgery, medicine, or care.
Medicines:
- Prescription pain medicine may be given. Ask your healthcare provider how to take this medicine safely. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your healthcare provider how to prevent or treat constipation.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Self-care after surgery:
- Do not lift more than 10 pounds for 4 weeks or as directed. Do not bend or twist. This will help your surgery area heal and decrease your risk for a hernia.
- Prevent blood clots and pneumonia. Walk around the inside of your house at least every 2 hours.
- Check your stoma every day. Check for signs of infection, such as redness, swelling, and drainage.
- Do not drive until your healthcare provider says it is okay.
Work with an ostomy specialist:
An ostomy specialist can provide more information on how to care for your colostomy. The specialist will help select the right size and type of pouch for your colostomy to prevent problems. You may need a different size pouch after your stoma heals. The specialist will also know how and where to get the supplies you need, and which supplies are best.
Care for the surgery area and stoma:
Look at the skin around your stoma each time you change your pouch. Your stoma should be pink or red and moist. You may have a small amount of bleeding when you clean your stoma. This is normal. Your stoma will get smaller and become its normal size in about 8 weeks.
- Make sure the skin barrier opening fits well. The skin barrier is the part of the pouch that sticks to the skin of your abdomen. It should be no more than ⅛ of an inch larger than your stoma. If the opening is too large, bowel movement can leak onto your skin and cause irritation. Measure the size of your stoma with the guide that comes with your colostomy supplies. Make sure you cut the skin barrier smaller as your stoma gets smaller.
- Soothe irritated skin. If your skin is red, it may mean that the skin barrier was on too long. It is important to find the cause of your skin irritation. Ask your healthcare provider if you need help finding the cause of your skin irritation.
- Care for your posterior wound. Wash the area with soap and water daily. Use bandages or pads to collect any drainage. Change them daily or if the bandage or pad gets dirty or wet.
Nutrition after colostomy creation:
- Eat a variety of healthy foods. Healthy foods include fruits, vegetables, whole-grain breads, low-fat dairy products, and lean meats. Do not eat foods that give you cramps or diarrhea.

- Limit foods that may cause gas and odor. These include vegetables such as broccoli, cabbage, and cauliflower. Beans, eggs, and fish may also cause gas and odor. Eat slowly and do not use a straw to drink liquids. Yogurt, buttermilk, and fresh parsley may help control odor and gas.
- Drink liquids as directed. Ask your healthcare provider how much liquid to drink each day and which liquids are best for you. This may help reduce constipation.
Follow up with your surgeon or ostomy specialist as directed:
Write down your questions so you remember to ask them during your visits.
For more information:
- National Digestive Diseases Information Clearinghouse (NDDIC)
2 Information Way
Bethesda , MD 20892-3570
Phone: 1- 800 - 891-5389
Web Address: www.digestive.niddk.nih.gov
- United Ostomy Associations of America, Inc.
P.O. Box 512
Northfield , MN 55057-0512
Phone: 1- 800 - 826-0826
Web Address: http://www.ostomy.org
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
