Oxytrol: Package Insert / Prescribing Info
Package insert / product label
Generic name: oxybutynin
Dosage form: patch
Drug class: Urinary antispasmodics
Medically reviewed by Drugs.com. Last updated on Jun 7, 2024.
On This Page
- Indications and Usage
- Dosage and Administration
- Dosage Forms and Strengths
- Contraindications
- Warnings and Precautions
- Adverse Reactions/Side Effects
- Drug Interactions
- Use In Specific Populations
- Overdosage
- Description
- Clinical Pharmacology
- Nonclinical Toxicology
- Clinical Studies
- How Supplied/Storage and Handling
- Patient Counseling Information
Highlights of Prescribing Information
OXYTROL® (oxybutynin transdermal system)
Initial U.S. Approval: 1975
Recent Major Changes
Dosage and Administration (2) 5/2024
Indications and Usage for Oxytrol
OXYTROL is a muscarinic antagonist indicated for the treatment of overactive bladder in men with symptoms of urge urinary incontinence, urgency, and frequency. (1)
Oxytrol Dosage and Administration
- Apply OXYTROL transdermal system twice weekly (every 3 to 4 days) to dry, intact skin on the abdomen, hip, or buttocks. (2)
- Select a new application site with each new transdermal system to avoid re-application to the same site within 7 days. (2)
- Do not divide or cut the transdermal system into pieces. Do not use if the transdermal system is damaged.
Dosage Forms and Strengths
Transdermal system: 3.9 mg/day (3)
Contraindications
Warnings and Precautions
- Urinary Retention: Use caution in patients with clinically significant bladder outflow obstruction because of the risk of urinary retention. (5.1)
- Gastrointestinal Disorders: Use caution in patients with gastrointestinal obstructive disorders or decreased intestinal motility because of the risk of gastric retention. Use caution in patients with gastroesophageal reflux and/or those taking drugs that can cause or exacerbate esophagitis. (5.2)
- Central Nervous System Effects: Somnolence has been reported with products containing oxybutynin. Advise patients not to drive or operate heavy machinery until they know how OXYTROL affects them. (5.3)
- Angioedema: Angioedema has been reported with oral oxybutynin use. If symptoms of angioedema occur, discontinue OXYTROL and initiate appropriate therapy. (5.4)
- Skin Hypersensitivity: Discontinue OXYTROL in patients with skin hypersensitivity. (5.5)
- Myasthenia gravis: Avoid use in patients with myasthenia gravis, a disease characterized by decreased cholinergic activity at the neuromuscular junction. (5.6)
Adverse Reactions/Side Effects
The most common adverse reactions (incidence > 5% and > placebo) are application site reactions and dry mouth. (6.1)
To report SUSPECTED ADVERSE REACTIONS, contact AbbVie, Inc. at 1-800-678-1605 or contact the FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Drug Interactions
Other Anticholinergics (muscarinic antagonists): Concomitant use with other anticholinergic agents may increase the frequency and/or severity of dry mouth, constipation, blurred vision, and other anticholinergic pharmacological effects. (7.1)
See 17 for PATIENT COUNSELING INFORMATION and FDA-approved patient labeling.
Revised: 5/2024
Full Prescribing Information
1. Indications and Usage for Oxytrol
OXYTROL is a muscarinic antagonist indicated for the treatment of overactive bladder in men with symptoms of urge urinary incontinence, urgency, and frequency.
2. Oxytrol Dosage and Administration
OXYTROL 3.9 mg/day should be applied to dry, intact skin on the abdomen, hip, or buttock twice weekly (every 3 or 4 days). A new application site should be selected with each new transdermal system to avoid re-application to the same site within 7 days. Do not divide or cut the transdermal system into pieces. Do not use if the transdermal system is damaged.
4. Contraindications
The use of OXYTROL is contraindicated in the following conditions:
- Urinary retention
- Gastric retention
- Uncontrolled narrow-angle glaucoma
- Known serious hypersensitivity reaction to OXYTROL, oxybutynin, or to any of the components of OXYTROL [see Warnings and Precautions (5.5)].
5. Warnings and Precautions
5.1 Urinary Retention
Administer OXYTROL with caution in patients with clinically significant bladder outflow obstruction because of the risk of urinary retention [see Contraindications (4)].
5.2 Risks in Patients with Gastrointestinal Disorders
Administer OXYTROL with caution to patients with gastrointestinal obstructive disorders because of the risk of gastric retention [see Contraindications (4)].
OXYTROL, like other anticholinergic drugs, may decrease gastrointestinal motility and should be used with caution in patients with conditions such as ulcerative colitis or intestinal atony.
OXYTROL should be used with caution in patients who have hiatus hernia/gastroesophageal reflux and/or who are concurrently taking drugs (such as bisphosphonates) that can cause or exacerbate esophagitis.
5.3 Central Nervous System Effects
Products containing oxybutynin are associated with anticholinergic central nervous system (CNS) effects. A variety of CNS anticholinergic effects have been reported, including headache, dizziness, somnolence, confusion and hallucinations [see Adverse Events (6.2)]. Patients should be monitored for signs of anticholinergic CNS effects, particularly after beginning treatment. Advise patients not to drive or operate heavy machinery until they know how OXYTROL affects them. If a patient experiences anticholinergic CNS effects, drug discontinuation should be considered.
5.4 Angioedema
Angioedema requiring hospitalization and emergency medical treatment has occurred with the first or subsequent doses of oral oxybutynin. In the event of angioedema, OXYTROL should be discontinued and appropriate therapy promptly provided.
5.5 Skin Hypersensitivity
Patients who develop skin hypersensitivity to OXYTROL should discontinue drug treatment.
5.6 Exacerbation of Symptoms of Myasthenia Gravis
Avoid use of OXYTROL in patients with myasthenia gravis, a disease characterized by decreased cholinergic activity at the neuromuscular junction. If experiencing exacerbation of symptoms of myasthenia gravis, oxybutynin-containing product should be discontinued and appropriate therapy promptly provided.
6. Adverse Reactions/Side Effects
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
The safety of OXYTROL was evaluated in a total of 417 patients who participated in two clinical efficacy and safety studies and an open-label extension. Additional safety information was collected in earlier phase trials. In the two pivotal studies, a total of 246 patients received OXYTROL during the 12-week treatment periods. A total of 411 patients entered the open-label extension and of those, 65 patients and 52 patients received OXYTROL for at least 24 weeks and at least 36 weeks, respectively.
No deaths were reported during treatment. No serious adverse events related to treatment were reported.
Adverse reactions reported in the pivotal trials are summarized in Tables 1 and 2 below.
| Table 1: Number (%) of adverse reactions occurring in ≥ 2% of OXYTROL-treated patients and greater in the OXYTROL group than in the placebo group (Study 1). | ||||
| Adverse Reaction | Placebo
(N = 132) | OXYTROL (3.9 mg/day)
(N = 125) |
||
| N | % | N | % | |
| Application site pruritus | 8 | 6.1% | 21 | 16.8% |
| Dry mouth | 11 | 8.3% | 12 | 9.6% |
| Application site erythema | 3 | 2.3% | 7 | 5.6% |
| Application site vesicles | 0 | 0.0% | 4 | 3.2% |
| Diarrhea | 3 | 2.3% | 4 | 3.2% |
| Dysuria | 0 | 0.0% | 3 | 2.4% |
| Table 2: Number (%) of adverse reactions occurring in ≥ 2% of OXYTROL-treated patients and greater in the OXYTROL group than in the placebo group (Study 2). | ||||
| Adverse Reaction | Placebo
(N = 117) | OXYTROL (3.9 mg/day)
(N = 121) |
||
| N | % | N | % | |
| Application site pruritus | 5 | 4.3% | 17 | 14.0% |
| Application site erythema | 2 | 1.7% | 10 | 8.3% |
| Dry mouth | 2 | 1.7% | 5 | 4.1% |
| Constipation | 0 | 0.0% | 4 | 3.3% |
| Application site rash | 1 | 0.9% | 4 | 3.3% |
| Application site macules | 0 | 0.0% | 3 | 2.5% |
| Abnormal vision | 0 | 0.0% | 3 | 2.5% |
Most adverse reactions were described as mild or moderate in intensity. Severe application site reactions were reported by 6.4% of OXYTROL-treated patients in Study 1 and by 5.0% of OXYTROL-treated patients in Study 2.
Adverse reactions that resulted in discontinuation were reported by 11.2% of OXYTROL-treated patients in Study 1 and 10.7% of OXYTROL-treated patients in Study 2. Most of these discontinuations were due to application site reaction. In the two pivotal studies, no patient discontinued OXYTROL treatment due to dry mouth.
In the open-label extension, the most common treatment-related adverse reactions were: application site pruritus, application site erythema, and dry mouth.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post approval use of OXYTROL. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Nervous System Disorders: Memory impairment, dizziness, somnolence, confusion
Psychiatric Disorders: Delirium, hallucinations
Related/similar drugs
7. Drug Interactions
No specific drug-drug interaction studies have been performed with OXYTROL.
7.1 Other Anticholinergics
The concomitant use of OXYTROL with other anticholinergic drugs, or with other agents that produce dry mouth, constipation, somnolence, and/or other anticholinergic-like effects may increase the frequency and/or severity of such effects. Anticholinergic agents may potentially alter the absorption of some concomitantly administered drugs due to anticholinergic effects on gastrointestinal motility.
8. Use In Specific Populations
8.1 Pregnancy
Risk Summary
There are no studies with topical or oral oxybutynin use in pregnant women to inform a drug associated risk for birth defects or miscarriage. No adverse developmental outcomes were observed in animal reproduction studies when oxybutynin chloride was administered to pregnant rats and rabbits during organogenesis at approximately 50 and 1 times, respectively, the maximum human dose based on body surface area (see Data).
In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2-4% and 15-20% respectively.
Data
Animal Data
Subcutaneous administration of oxybutynin chloride to rats at doses up to 25 mg/kg (approximately 50 times the human exposure based on surface area) and to rabbits at doses up to 0.4 mg/kg (approximately 1 times the human exposure based on body surface area) throughout the period of organogenesis revealed no evidence of harm to the fetus.
8.2 Lactation
Risk Summary
There is no information on the presence of oxybutynin in human milk, the effects on the breastfed child, or the effects on milk production. The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for OXYTROL and any potential adverse effects on the breastfed child from OXYTROL or from the underlying maternal condition.
8.4 Pediatric Use
The safety and efficacy of OXYTROL in pediatric patients have not been established.
8.5 Geriatric Use
Forty-nine percent of OXYTROL-treated patients in the clinical studies were at least 65 years of age. No overall differences in safety or effectiveness were observed between these patients and younger patients, and other reported clinical experience has not identified differences in response between elderly and younger patients, but greater sensitivity of some older individuals cannot be ruled out [see Clinical Pharmacology (12.3)].
10. Overdosage
The plasma concentration of oxybutynin declines within 1 to 2 hours after removal of transdermal system(s). Patients should be monitored until symptoms resolve. Overdosage with oxybutynin has been associated with anticholinergic effects including CNS excitation, flushing, fever, dehydration, cardiac arrhythmia, vomiting, and urinary retention. Ingestion of 100 mg oral oxybutynin chloride in association with alcohol has been reported in a 13 year old boy who experienced memory loss, and in a 34 year old woman who developed stupor, followed by disorientation and agitation on awakening, dilated pupils, dry skin, cardiac arrhythmia, and retention of urine. Both patients recovered fully with treatment directed at their symptoms.
11. Oxytrol Description
OXYTROL (oxybutynin transdermal system) is designed to deliver oxybutynin over a 3- to 4-day interval after application to intact skin. OXYTROL is available as a 39 cm2 transdermal system containing 36 mg of oxybutynin. OXYTROL has a nominal in vivo delivery rate of 3.9 mg oxybutynin per day through skin of average permeability (inter-individual variation in skin permeability is approximately 20%).
Oxybutynin is an antispasmodic, anticholinergic agent. Oxybutynin is administered as a racemate of R- and S-isomers. Chemically, oxybutynin is d, l (racemic) 4-diethylamino-2-butynyl phenylcyclohexylglycolate. The empirical formula of oxybutynin is C22H31NO3. Its structural formula is:
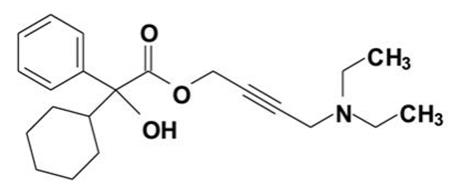
Oxybutynin is a white powder with a molecular weight of 357. It is soluble in alcohol, but relatively insoluble in water.
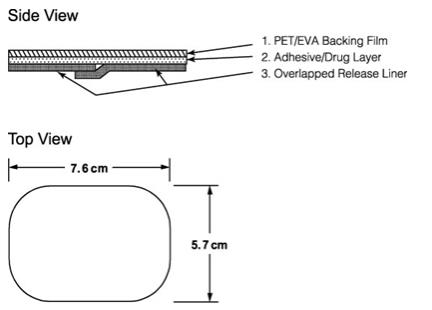
OXYTROL is a matrix-type transdermal system composed of three layers as illustrated in Figure 1. Layer 1 (Backing Film) is a thin flexible polyester/ethylene-vinyl acetate film that provides the matrix transdermal system with occlusivity and physical integrity and protects the adhesive/drug layer. Layer 2 (Adhesive/Drug Layer) is a cast film of acrylic adhesive containing oxybutynin and triacetin, USP. Layer 3 (Release Liner) is two overlapped siliconized polyester strips that are peeled off and discarded by the patient prior to applying the matrix transdermal system.
Figure 1: Side and top views of the OXYTROL transdermal system.
(Not to scale)
12. Oxytrol - Clinical Pharmacology
12.1 Mechanism of Action
The free base form of oxybutynin is pharmacologically equivalent to oxybutynin hydrochloride. Oxybutynin acts as a competitive antagonist of acetylcholine at postganglionic muscarinic receptors, resulting in relaxation of bladder smooth muscle. In patients with conditions characterized by involuntary detrusor contractions, cystometric studies have demonstrated that oxybutynin increases maximum urinary bladder capacity and increases the volume to first detrusor contraction.
Oxybutynin is a racemic (50:50) mixture of R- and S-isomers. Antimuscarinic activity resides predominantly in the R-isomer. The active metabolite, N-desethyloxybutynin, has pharmacological activity on the human detrusor muscle that is similar to that of oxybutynin in in vitro studies.
12.3 Pharmacokinetics
Absorption
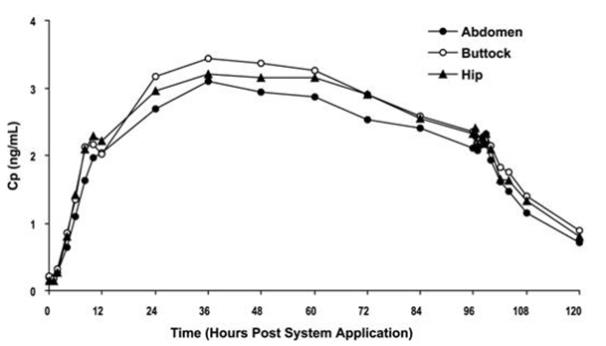
Oxybutynin is transported across intact skin and into the systemic circulation by passive diffusion across the stratum corneum. The average daily dose of oxybutynin absorbed from the 39 cm2 OXYTROL transdermal system is 3.9 mg. The average (SD) nominal dose, 0.10 (0.02) mg oxybutynin per cm2 surface area, was obtained from analysis of residual oxybutynin content of transdermal systems worn over a continuous 4-day period during 303 separate occasions in 76 healthy volunteers. Following application of the first OXYTROL 3.9 mg/day transdermal system, oxybutynin plasma concentrations increase for approximately 24 to 48 hours, reaching average maximum concentrations of 3 to 4 ng/mL. Thereafter, steady concentrations are maintained for up to 96 hours. Absorption of oxybutynin is bioequivalent when OXYTROL is applied to the abdomen, buttocks, or hip. Average plasma concentrations measured during a randomized, crossover study of the three recommended application sites in 24 healthy men and women are shown in Figure 2.
Figure 2: Average plasma oxybutynin concentrations (Cp) in 24 healthy male and female volunteers during single-dose application of OXYTROL 3.9 mg/day to the abdomen, buttock, and hip (Transdermal System removal at 96 hours).
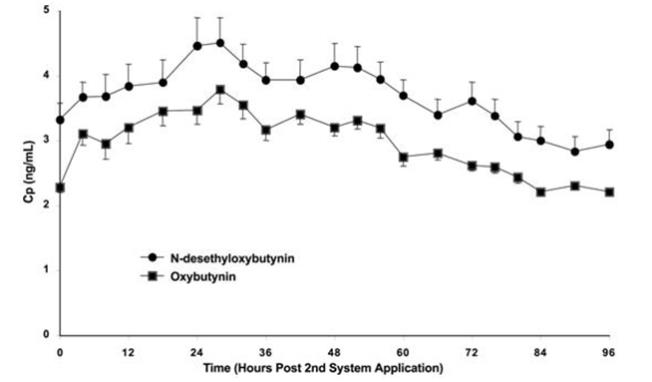
Steady-state conditions are reached during the second OXYTROL application. Average steady-state plasma concentrations were 3.1 ng/mL for oxybutynin and 3.8 ng/mL for N-desethyloxybutynin (Figure 3). Table 3 provides a summary of pharmacokinetic parameters of oxybutynin in healthy volunteers after single and multiple applications of OXYTROL.
Figure 3: Average (SEM) steady-state oxybutynin and N-desethyloxybutynin plasma concentrations (Cp) measured in 13 healthy volunteers following the second transdermal system application in a multiple-dose, randomized, crossover study.
| Table 3: Mean (SD) oxybutynin pharmacokinetic parameters from single and multiple dose studies in healthy men and women volunteers after application of OXYTROL on the abdomen. | ||||
| Dosing | Oxybutynin | |||
| Cmax (SD)
(ng/mL) | Tmax1
(hr) | Cavg (SD)
(ng/mL) | AUC (SD)
(ng/mLxh) |
|
| Single | 3.0 (0.8) | 48 | - | 245 (59)2 |
| 3.4 (1.1) | 36 | - | 279 (99)2 | |
| Multiple | 6.6 (2.4) | 10 | 4.2 (1.1) | 408 (108)3 |
| 4.2 (1.0) | 28 | 3.1 (0.7) | 259 (57)4 | |
| 1Tmax given as median 2AUCinf 3AUC0-96 4AUC0-84 |
||||
Distribution
Oxybutynin is widely distributed in body tissues following systemic absorption. The volume of distribution was estimated to be 193 L after intravenous administration of 5 mg oxybutynin chloride.
Metabolism
Oxybutynin is metabolized primarily by the cytochrome P450 enzyme systems, particularly CYP3A4, found mostly in the liver and gut wall. Metabolites include phenylcyclohexylglycolic acid, which is pharmacologically inactive, and N-desethyloxybutynin, which is pharmacologically active.
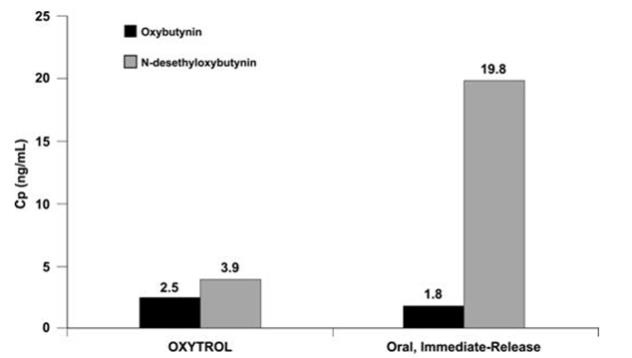
After oral administration of oxybutynin, pre-systemic first-pass metabolism results in an oral bioavailability of approximately 6% and higher plasma concentration of the N-desethyl metabolite compared to oxybutynin (see Figure 4). The plasma concentration area under the time-concentration curve (AUC) ratio of N-desethyl metabolite to parent compound following a single 5 mg oral dose of oxybutynin chloride was 11.9:1.
Transdermal administration of oxybutynin bypasses first-pass gastrointestinal and hepatic metabolism, reducing the formation of the N-desethyl metabolite (see Figure 4). Only small amounts of CYP3A4 are found in skin, limiting pre-systemic metabolism during transdermal absorption. The resulting plasma concentration AUC ratio of N-desethyl metabolite to parent compound following multiple OXYTROL applications was 1.3:1.
Figure 4: Average plasma concentrations (Cp) measured after a single, 96-hour application of the OXYTROL 3.9 mg/day transdermal system (AUCinf/96) and a single, 5 mg, oral immediate-release dose of oxybutynin chloride (AUCinf/8) in 16 healthy male and female volunteers.
Following intravenous administration, the elimination half-life of oxybutynin is approximately 2 hours. Following removal of OXYTROL, plasma concentrations of oxybutynin and N-desethyloxybutynin decline with an apparent half-life of approximately 7 to 8 hours.
Excretion
Oxybutynin is extensively metabolized by the liver, with less than 0.1% of the administered dose excreted unchanged in the urine. Also, less than 0.1% of the administered dose is excreted as the metabolite N-desethyloxybutynin.
Specific Populations:
Geriatric: The pharmacokinetics of oxybutynin and N-desethyloxybutynin were similar in older and younger patients.
Pediatric: The pharmacokinetics of oxybutynin and N-desethyloxybutynin were not evaluated in individuals younger than 18 years of age.
Gender: There were no significant differences in the pharmacokinetics of oxybutynin in healthy male and female volunteers following application of OXYTROL.
Race: Available data suggest that there are no significant differences in the pharmacokinetics of oxybutynin based on race in healthy volunteers following administration of OXYTROL. Japanese volunteers demonstrated a somewhat lower metabolism of oxybutynin to N-desethyloxybutynin compared to Caucasian volunteers.
13. Nonclinical Toxicology
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
A 24-month study in rats at dosages of oxybutynin chloride of 20, 80 and 160 mg/kg showed no evidence of carcinogenicity. These doses are approximately 6, 25 and 50 times the maximum exposure in humans taking an oral dose based on body surface area.
Oxybutynin chloride showed no increase of mutagenic activity when tested in Schizosaccharomyces pompholiciformis, Saccharomyces cerevisiae, and Salmonella typhimurium test systems. Reproduction studies with oxybutynin chloride in the mouse, rat, hamster, and rabbit showed no definite evidence of impaired fertility.
14. Clinical Studies
The efficacy and safety of OXYTROL were evaluated in patients with urge urinary incontinence in two controlled studies and one open-label extension. Study 1 was a placebo controlled study, comparing the safety and efficacy of OXYTROL at dose levels of 1.3, 2.6, and 3.9 mg/day to placebo in 520 patients. Open-label treatment was available for patients completing the study. Study 2 was a study comparing the safety and efficacy of OXYTROL 3.9 mg/day versus active and placebo controls in 361 patients.
Study 1 was a randomized, double-blind, placebo-controlled, parallel group study of three dose levels of OXYTROL conducted in 520 patients. The 12-week double-blind treatment included an OXYTROL dose of 3.9 mg/day or matching placebo. An open-label, dose titration treatment extension allowed continued treatment for up to an additional 40 weeks for patients completing the double-blind period. The majority of patients were Caucasian (91%) and female (92%) with a mean age of 61 years (range, 20 to 88 years). Entry criteria required that patients have urge or mixed incontinence (with a predominance of urge), urge incontinence episodes of ≥ 10 per week, and ≥ 8 micturitions per day. The patient’s medical history and a urinary diary during the treatment-free baseline period confirmed the diagnosis of urge incontinence. Approximately 80% of patients had no prior pharmacological treatment for incontinence. Changes in weekly incontinence episodes, urinary frequency, and urinary void volume between placebo and active treatment groups are summarized in Table 4.
| Table 4: Mean and median change from baseline to end of treatment (Week 12 or last observation carried forward) in incontinence episodes, urinary frequency, and urinary void volume in patients treated with OXYTROL 3.9 mg/day or placebo for 12 weeks (Study 1). | ||||
| Parameter | Placebo
(N = 127) | OXYTROL 3.9 mg/day
(N = 120) |
||
| Mean (SD) | Median | Mean (SD) | Median | |
| Weekly Incontinence Episodes | ||||
| Baseline | 37.7 (24.0) | 30 | 34.3 (18.2) | 31 |
| Reduction | 19.2 (21.4) | 15 | 21.0 (17.1) | 19 |
| p value vs. placebo | - | 0.0265* | ||
| Daily Urinary Frequency | ||||
| Baseline | 12.3 (3.5) | 11 | 11.8 (3.1) | 11 |
| Reduction | 1.6 (3.0) | 1 | 2.2 (2.5) | 2 |
| p value vs. placebo | - | 0.0313* | ||
| Urinary Void Volume (mL) | ||||
| Baseline | 175.9 (69.5) | 166.5 | 171.6 (65.1) | 168 |
| Increase | 10.5 (56.9) | 5.5 | 31.6 (65.6) | 26 |
| p value vs. placebo | - | 0.0009** | ||
| *Comparison significant if p < 0.05 **Comparison significant if p ≤ 0.0167 |
||||
Study 2 was a randomized, double-blind, study of OXYTROL 3.9 mg/day versus active and placebo controls conducted in 361 patients. The 12-week double-blind treatment included an OXYTROL dose of 3.9 mg/day, an active comparator, and placebo. The majority of patients were Caucasian (95%) and female (93%) with a mean age of 64 years (range, 18 to 89 years). Entry criteria required that all patients have urge or mixed incontinence (with a predominance of urge) and had achieved a beneficial response from the anticholinergic treatment they were using at the time of study entry. The average duration of prior pharmacological treatment was greater than 2 years. The patient’s medical history and a urinary diary during the treatment-free baseline period confirmed the diagnosis of urge incontinence. Changes in daily incontinence episodes, urinary frequency, and urinary void volume between placebo and active treatment groups are summarized in Table 5.
| Table 5: Mean and median change from baseline to end of treatment (Week 12 or last observation carried forward) in incontinence episodes, urinary frequency, and urinary void volume in patients treated with OXYTROL 3.9 mg/day or placebo for 12 weeks (Study 2). | ||||
| Parameter | Placebo
(N = 117) | OXYTROL 3.9 mg/day
(N = 121) |
||
| Mean (SD) | Median | Mean (SD) | Median | |
| Daily Incontinence Episodes | ||||
| Baseline | 5.0 (3.2) | 4 | 4.7 (2.9) | 4 |
| Reduction | 2.1 (3.0) | 2 | 2.9 (3.0) | 3 |
| p value vs. placebo | - | 0.0137* | ||
| Daily Urinary Frequency | ||||
| Baseline | 12.3 (3.3) | 12 | 12.4 (2.9) | 12 |
| Reduction | 1.4 (2.7) | 1 | 1.9 (2.7) | 2 |
| p value vs. placebo | - | 0.1010* | ||
| Urinary Void Volume (mL) | ||||
| Baseline | 175.0 (68.0) | 171.0 | 164.8 (62.3) | 160 |
| Increase | 9.3 (63.1) | 5.5 | 32.0 (55.2) | 24 |
| P value vs placebo | - | 0.0010* | ||
| *Comparison significant if p < 0.05 | ||||
In a controlled clinical trial of skin sensitization, none of the 103 test subjects demonstrated skin hypersensitivity to OXYTROL.
Adhesion
Adhesion was periodically evaluated during the pivotal studies. Of the 4,746 OXYTROL evaluations in the trials, 20 (0.4%) were observed at clinic visits to have become completely detached and 35 (0.7%) became partially detached during routine clinic use. Similar to the pharmacokinetic studies, > 98% of the transdermal systems evaluated in the pivotal studies were assessed as being ≥ 75% attached and thus would be expected to perform as anticipated.
16. How is Oxytrol supplied
How Supplied
Unit Dose: Heat sealed pouch containing 1 OXYTROL (oxybutynin transdermal system).
Each 39 cm2 transdermal system imprinted with “OXYTROL 3.9 mg/day” contains 36 mg of oxybutynin for nominal delivery of 3.9 mg oxybutynin per day when dosed in a twice weekly regimen.
Patient Calendar Box of 8 Transdermal Systems (NDC 0023-6153-08)
Storage
Store at 20-25°C (68-77°F). [See USP controlled room temperature.] Protect from moisture and humidity. Do not store outside the sealed pouch. Apply immediately after removal from the protective pouch. Discard used OXYTROL in household trash in a manner that prevents accidental application or ingestion by children, pets, or others.
Keep out of reach of children.
17. Patient Counseling Information
See FDA-Approved Patient Labeling (Patient Information and Instructions for Use)
Administration Instructions
Inform patients that OXYTROL should be applied to dry, intact skin on the abdomen, hip, or buttock and not be applied to areas that have been treated with oils, lotions or powders. OXYTROL should not be exposed to sunlight. Contact with water while bathing, swimming, showering or exercising will not change the effect of OXYTROL.
Do not divide or cut the transdermal system into pieces. Do not use if the transdermal system is damaged.
A new application site should be selected with each new transdermal system to avoid re-application to the same site within 7 days. Inform patients to try to change OXYTROL on the same 2 days each week and that the package of OXYTROL has a calendar checklist printed on the back to remind patients of their schedule. Inform patients to avoid rubbing the area of the transdermal system during bathing, swimming, showering or exercising. Inform patients that details on use of the transdermal system are explained in the Patient Information Leaflet.
Inform patients to discard used OXYTROL in household trash in a manner that prevents accidental application or ingestion by children, pets, or others. Inform patients to keep out of reach of children.
Important Anticholinergic Adverse Reactions
Inform patients that anticholinergic (antimuscarinic) agents, such as OXYTROL, may produce adverse reactions related to anticholinergic pharmacological activity including:
- Urinary retention and constipation.
- Heat prostration (due to decreased sweating) when anticholinergics such as OXYTROL are used in a hot environment.
- Dizziness or blurred vision. Patients should be advised to avoid driving or operating heavy machinery until OXYTROL’s effects have been determined.
- Drowsiness that may be worsened by alcohol.
- Angioedema has been reported with oral oxybutynin use. Patients should be advised to promptly discontinue OXYTROL and seek immediate medical attention if they experience symptoms consistent with angioedema.
Distributed By:
AbbVie, Inc.
North Chicago, IL 60064
© 2024 AbbVie. All rights reserved.
OXYTROL and its design are trademarks of Allergan Sales, LLC, an AbbVie company.
| PATIENT INFORMATION
OXYTROL (OKSEE TROLE) (oxybutynin transdermal system) |
| What is OXYTROL?
OXYTROL is a prescription medicine used to treat overactive bladder in men with symptoms of sudden need to urinate with leaking or wetting accidents (urge urinary incontinence), need to urinate right away (urgency), and a need to urinate often (frequency). OXYTROL is a transdermal system (patch) you apply to your skin. It is not known if OXYTROL is safe and effective in children. |
| Do not use OXYTROL if:
• your bladder does not empty or does not empty completely when you urinate (urinary retention). • your stomach empties slowly or incompletely after a meal (gastric retention). • you have uncontrolled narrow-angle glaucoma (high pressure in your eye). Tell your doctor if you have glaucoma or a family history of glaucoma. • you are allergic to oxybutynin or any of the ingredients in OXYTROL. See the end of this Patient Information leaflet for a complete list of ingredients in OXYTROL. If you have allergies to medical tape products or other skin patches, tell your doctor. |
| Before using OXYTROL, tell your doctor about all of your medical conditions, including if you:
• have problems emptying your bladder completely. • have a gastrointestinal obstruction (blockage in the digestive system). • have ulcerative colitis (inflamed bowels). • have gastroesophageal reflux disease (GERD) or esophagitis (inflamed esophagus, the tube between your mouth and stomach). • have myasthenia gravis (condition that causes muscle weakness). Tell your doctor about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. Using OXYTROL with certain other medicines may affect each other. Using OXYTROL with other medicines can cause serious side effects. Especially tell your doctor if you take: • medicines called “bisphosphonates” to treat osteoporosis • medicines called “anticholinergics” Ask your doctor or pharmacist for a list of these medicines if you are not sure you take any of these medicines. Know the medicines you take. Keep a list of them and show it to your doctor and pharmacist when you get a new medicine. |
| How should I use OXYTROL?
• Read the Instructions for Use at the end of this Patient Information leaflet for information on the right way to use OXYTROL. • Use OXYTROL exactly as your doctor tells you to use it. • Put on a new patch of OXYTROL 2 times a week (every 3 to 4 days) according to your doctor’s instructions. • Choose a new skin site for each new patch application. You should not use the same skin site within 7 days. • Wear the patch all the time until it is time to apply a new one. • Wear only 1 patch of OXYTROL at a time. • Try to change the patch on the same 2 days each week. • Your package of OXYTROL has a calendar checklist printed on the back to help you remember your schedule. Mark the schedule you plan to follow. Always change OXYTROL on the 2 days of the week you mark on the calendar. • Contact with water when you are bathing, swimming, showering or exercising will not change the way that OXYTROL works. • Do not divide or cut the patch into pieces. Damaged patches should not be used. |
| What should I avoid while using OXYTROL?
• You should not drink alcohol while using OXYTROL. Drinking alcohol can increase drowsiness that results from OXYTROL use. • OXYTROL can cause dizziness or blurred vision. Do not drive, operate machinery, or do other dangerous activities until you know how OXYTROL affects you. • Do not put OXYTROL on areas that have been treated with oils, lotions, or powders that could keep the patch from sticking well to your skin. Do not expose the patch to sunlight. Wear your patch under clothing. • Avoid rubbing the patch area during bathing, swimming, showering or exercising. |
| What are the possible side effects of OXYTROL?
OXYTROL may cause serious side effects, including: • inability to empty your bladder (urinary retention). OXYTROL may increase your chances of not being able to empty your bladder if you have a blockage at the base of your bladder that decreases or stops the flow of urine into the urethra, the tube that carries urine out of the body (bladder outlet obstruction). Tell your doctor right away if you are unable to empty your bladder. • increased risk of stomach and esophagus problems in certain people. OXYTROL may cause stomach and esophagus problems in people who have a history of stomach or intestinal blockage, ulcerative colitis, intestinal atony, hiatal hernia, gastroesophageal reflux disease, or who are taking certain medicines called bisphosphonates. • central nervous system effects. OXYTROL can cause central nervous system side effects including headache, dizziness, sleepiness, confusion, and seeing or hearing things that are not really there (hallucinations). Your doctor should monitor you for these effects after starting OXYTROL. See “What should I avoid while using OXYTROL.” • swelling (angioedema). The active ingredient in OXYTROL, oxybutynin, can cause swelling around the eyes, lips, genitals, hands or feet. Some people who have taken oxybutynin medicines by mouth have had to be hospitalized. Stop using OXYTROL immediately and get emergency medical treatment right away if you have any of these symptoms. • skin hypersensitivity. You may have skin changes where the patch was placed such as itching, rash, or redness. Tell your doctor if these changes do not go away or bother you. • worsening of myasthenia gravis (condition that causes muscle weakness). OXYTROL may cause worsening of myasthenia gravis symptoms, including muscle weakness and breathing problems. Call your doctor right away if you have any worsening muscle weakness or breathing problems. The most common side effects of OXYTROL include skin reactions where the patch is placed and dry mouth. OXYTROL may cause you to sweat less and may increase your chances of being overheated, having a fever or heat stroke if you are in hot temperatures. Tell your doctor if you have any side effect that bothers you or that does not go away or if you have constipation. These are not all the possible side effects of OXYTROL. For a complete list, ask your doctor or pharmacist. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA- 1088. |
| How should I store OXYTROL?
• Store OXYTROL at room temperature between 68°F to 77°F (20°C to 25°C). • Do not store OXYTROL outside the sealed pouch. • Keep OXYTROL patches in a dry place. • Safely throw away used OXYTROL patches in the household trash. Be careful to prevent accidental exposure of OXYTROL to children or pets. Keep OXYTROL and all medicines out of the reach of children. |
| General information about the safe and effective use of OXYTROL.
Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. Do not use OXYTROL for a condition for which it was not prescribed. Do not give OXYTROL to other people, even if they have the same symptoms you have. It may harm them. You can ask your pharmacist or doctor for information about OXYTROL that is written for health professionals. |
| What are the ingredients of OXYTROL?
Active Ingredient: oxybutynin Inactive Ingredients: flexible polyester/ethylene-vinyl acetate film, acrylic adhesive, triacetin, siliconized polyester film. For more information, go to www.OXYTROL.com or call 1-800-678-1605 |
Instructions for Use
OXYTROL (OKSEE TROLE)
(oxybutynin transdermal system)
Read this Instructions for Use that comes with your OXYTROL before you start using it and each time you get a refill. There may be new information. This information does not take the place of talking to your doctor about your medical condition or treatment.
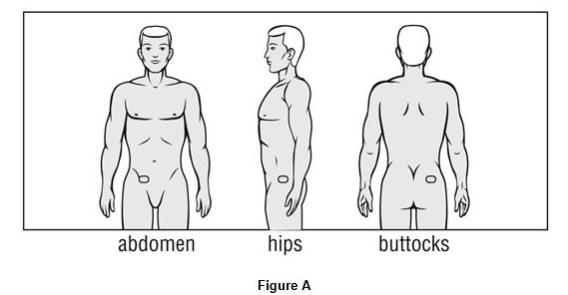
Where to apply OXYTROL:
- Put the patch on a clean, dry, and smooth (fold-free) area of skin on your abdomen (stomach area), hips or buttocks. See Figure A.
- Avoid your waistline area, since tight clothing may rub against the patch.
- The areas you choose should not be oily, damaged (cut or scraped), irritated (rashes) or have any other skin problems.
-
Do not put OXYTROL on areas that have been treated with oils, lotions, or powders that could keep the patch from sticking well to your skin.
- When you put on a new patch, use a different area of skin from the most recent patch site. You may find it useful to change the site from one side of your body to the other.
-
Do not use the same area for the patch for at least 7 days. You may choose to try different sites when using OXYTROL to find the sites that are most comfortable for you and where clothing will not rub against it.
- Do not divide or cut the patch into pieces. Damaged patches should not be used.
How to apply OXYTROL:
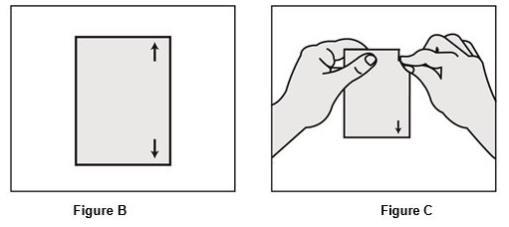
Step 1.
- Each patch is sealed in its own protective pouch. See Figure B.
- When you are ready to put on your OXYTROL patch, tear open the pouch and remove the patch. See Figure C.
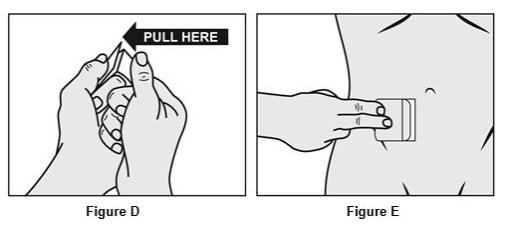
Step 2.
- The sticky adhesive side of the patch is covered by 2 strips of overlapping protective liner. See Figure D.
- Remove the first piece of the protective liner and place the patch, adhesive face down, firmly onto the skin. See Figure E.
Step 3.
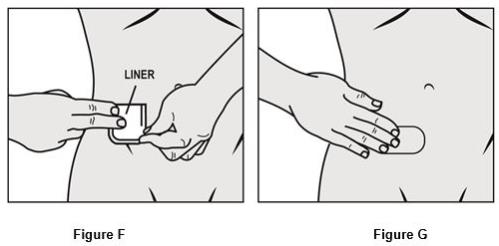
- Bend the patch in half and gently roll the remaining part onto your skin using the tips of your fingers. As you roll the patch in place, the second piece of the protective liner should come off the patch. See Figure F.
- Apply firm pressure over the surface of the patch with your fingers to make sure the patch stays on. See Figure G.
- When putting on the patch, avoid touching the sticky adhesive side.
- Touching the adhesive may cause the patch to fall off early.
- Throw away the protective liners.
- If the patch partly or completely falls off, press it back in place and continue to follow your application schedule.
- If the patch does not stay on, throw it away. Put on a new patch on a different area of skin, and continue to follow your original application schedule.
- If you forget to change your patch after 3 or 4 days, remove the old patch, put on a new patch in a different area of skin and continue to follow your original application schedule.
How to remove OXYTROL:
- When changing your OXYTROL patch, remove the old patch slowly and carefully to avoid damaging your skin.
- After the old patch is removed, fold it in half with the sticky sides together.
-
The patch will still contain some oxybutynin. Throw the patch away so that it cannot be worn or swallowed by another person, child, or pet.
- Gently wash the application site with warm water and a mild soap to remove any adhesive that stays on your skin after removing the patch.
- A small amount of baby oil may also be used to remove any adhesive remaining on your skin. Rings of adhesive that become dirty may need a medical adhesive removal pad that you can get from your pharmacist.
- Alcohol or other dissolving liquids (nail polish remover or other solvents) may cause skin irritation and should not be used.
This Patient Information and Instructions for Use has been approved by the U.S. Food and Drug Administration.
Distributed By:
AbbVie, Inc.
North Chicago, IL 60064
© 2024 AbbVie. All rights reserved.
OXYTROL and its design are trademarks of Allergan Sales, LLC, an AbbVie company.
Revised: 05/2024
PRINCIPAL DISPLAY PANEL
NDC 0023-6153-08
OXYTROL®
Oxybutynin Transdermal System
3.9 mg/day
Nominal delivery of 3.9 mg/day.
Continuous delivery for twice weekly dosing.
Each 39 cm2 system contains 36 mg oxybutynin.
Inactive Components: triacetin, USP; acrylic adhesive;
polyester/ethylene-vinyl acetate film, and siliconized polyester film.
Contains 8 transdermal systems
Keep out of reach of children.
Rx only
| OXYTROL
oxybutynin patch |
|||||||||||||||||||||||||
|
|||||||||||||||||||||||||
|
|||||||||||||||||||||||||
|
|||||||||||||||||||||||||
|
|||||||||||||||||||||||||
|
|||||||||||||||||||||||||
|
|||||||||||||||||||||||||
| Labeler - Allergan, Inc. (144796497) |
More about Oxytrol (oxybutynin)
- Check interactions
- Compare alternatives
- Pricing & coupons
- Reviews (79)
- Side effects
- Dosage information
- During pregnancy
- Drug class: urinary antispasmodics
- En español
Patient resources
Professional resources
Other brands
Ditropan, Ditropan XL, Gelnique
