Novolin R: Package Insert / Prescribing Info
Package insert / product label
Generic name: regular human insulin
Dosage form: injection, solution
Drug class: Insulin
J Code (medical billing code): J1815 (Per 5 units, injection)
Medically reviewed by Drugs.com. Last updated on Aug 14, 2025.
On This Page
- Indications and Usage
- Dosage and Administration
- Dosage Forms and Strengths
- Contraindications
- Warnings and Precautions
- Adverse Reactions/Side Effects
- Drug Interactions
- Use In Specific Populations
- Overdosage
- Description
- Clinical Pharmacology
- Nonclinical Toxicology
- How Supplied/Storage and Handling
- Patient Counseling Information
- Warnings
Highlights of Prescribing Information
NOVOLIN® R (insulin human) injection, for subcutaneous or intravenous use
Initial U.S. Approval: 1991
Indications and Usage for Novolin R
NOVOLIN R is a short-acting human insulin indicated to improve glycemic control in adults and pediatric patients with diabetes mellitus (1).
Novolin R Dosage and Administration
- •
- See Full Prescribing Information for important administration instructions. (2.1)
- •
- Subcutaneous injection: inject subcutaneously 30 minutes before a meal into the abdominal area, buttocks, thigh or the upper arm. Rotate injection sites to reduce risk of lipodystrophy and localized cutaneous amyloidosis. (2.2)
- •
- Intravenous use: administer intravenously ONLY under medical supervision at concentrations from 0.05 unit/mL to 1 unit/mL in infusion systems using polypropylene infusion bags. (2.2)
- •
- Individualize dose based on route of administration, metabolic needs, blood glucose monitoring results and glycemic control goal. (2.3)
- •
- NOVOLIN R given by subcutaneous injection should generally be used in regimens with an intermediate- or long-acting insulin. (2.3)
- •
- Can be mixed with NOVOLIN N. (2.5)
Dosage Forms and Strengths
Contraindications
Warnings and Precautions
- •
- Never share a NOVOLIN R FlexPen or syringe between patients, even if the needle is changed. (5.1)
- •
- Hyperglycemia or Hypoglycemia with Changes in Insulin Regimen: Make changes to a patient’s insulin regimen (e.g., insulin strength, manufacturer, type, injection site or method of administration) under close medical supervision with increased frequency of blood glucose monitoring. (5.2)
- •
- Hypoglycemia: May be life-threatening. Increase frequency of blood glucose monitoring with changes to: insulin dosage, co-administered glucose lowering medications, meal pattern, physical activity; in patients with renal or hepatic impairment or with hypoglycemia unawareness. (5.3)
- •
- Hypoglycemia Due to Medication Errors: Accidental mix-ups between insulin products can occur. Instruct patients to check insulin labels before injection. (5.4)
- •
- Hypersensitivity Reactions: Severe, life-threatening, generalized allergy, including anaphylaxis, can occur. Discontinue NOVOLIN R, monitor, and treat if indicated. (5.5)
- •
- Hypokalemia: May be life-threatening. Monitor potassium levels in patients at risk for hypokalemia and treat if indicated. (5.6)
- •
- Fluid Retention and Heart Failure with Concomitant Use of Thiazolidinediones (TZDs): Observe for signs and symptoms of heart failure; consider dosage reduction or discontinuation if heart failure occurs. (5.7)
Adverse Reactions/Side Effects
Adverse reactions observed with NOVOLIN R include hypoglycemia, allergic reactions, injection site reactions, lipodystrophy, weight gain and edema (6).
To report SUSPECTED ADVERSE REACTIONS, contact Novo Nordisk Inc. at 1-800-727-6500 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Drug Interactions
See 17 for PATIENT COUNSELING INFORMATION and FDA-approved patient labeling.
Revised: 11/2022
Full Prescribing Information
1. Indications and Usage for Novolin R
NOVOLIN R is indicated to improve glycemic control in adults and pediatric patients with diabetes mellitus.
2. Novolin R Dosage and Administration
2.1 Important Administration Instructions
Always check insulin labels before administration [see Warnings and Precautions (5.4)].
- •
- Inspect NOVOLIN R visually before use. It should appear clear and colorless. Do not use NOVOLIN R if particulate matter or coloration is seen.
- •
- Use of NOVOLIN R in insulin pumps is not recommended because of the risk of precipitation.
2.2 Route of Administration
Subcutaneous Administration
- •
- Inject NOVOLIN R subcutaneously approximately 30 minutes prior to the start of a meal into the abdominal area, buttocks, thigh, or the upper arm.
- •
- Rotate injection sites within the same region from one injection to the next to reduce the risk of lipodystrophy and localized cutaneous amyloidosis. Do not inject into areas of lipodystrophy or localized cutaneous amyloidosis [see Warnings and Precautions (5.2), Adverse Reactions (6)].
Intravenous Administration
- •
- Administer NOVOLIN R intravenously ONLY under medical supervision with close monitoring of blood glucose and potassium levels to reduce the risk of hypoglycemia and hypokalemia [see Warnings and Precautions (5.3, 5.6) and How Supplied/Storage and Handling (16.2)].
- •
- Dilute NOVOLIN R to concentrations from 0.05 unit/mL to 1 unit/mL insulin in infusion systems using polypropylene infusion bags. NOVOLIN R is stable in infusion fluids such as 0.9% sodium chloride, 5% dextrose, or 10% dextrose with 40 mmol/L potassium chloride. Intravenous infusion bags are stable at room temperature for 24 hours.
2.3 Dosage Information
- •
- Individualize and adjust the dosage of NOVOLIN R based on route of administration, the individual's metabolic needs, blood glucose monitoring results and glycemic control goal.
- •
- NOVOLIN R given by subcutaneous injection should generally be used in regimens that include an intermediate or long-acting insulin.
- •
- During changes to a patient’s insulin regimen, increase the frequency of blood glucose monitoring [see Warnings and Precautions (5.2)].
- •
- Dosage adjustments may be needed with changes in physical activity, changes in meal patterns (i.e., macronutrient content or timing of food intake), changes in renal or hepatic function or during acute illness [see Warnings and Precautions (5.2, 5.3) and Use in Specific Populations (8.6,8.7)].
- •
- Dosage adjustment may be needed when switching from another insulin to NOVOLIN R [see Warnings and Precautions (5.2)].
2.4 Dosage Adjustment due to Drug Interactions
- •
- Dosage adjustment may be needed when NOVOLIN R is co-administered with certain drugs [see Drug Interactions (7)].
3. Dosage Forms and Strengths
- Injection: 100 units/mL (U-100), a clear and colorless solution available as:
- •
- 10 mL multiple-dose vial
- •
- 3 mL single-patient-use NOVOLIN R FlexPen prefilled pen
4. Contraindications
NOVOLIN R is contraindicated:
- •
- During episodes of hypoglycemia
- •
- In patients with hypersensitivity to NOVOLIN R or any of its excipients
5. Warnings and Precautions
5.1 Never Share a NOVOLIN R FlexPen or Syringe between Patients
NOVOLIN R FlexPen must never be shared between patients, even if the needle is changed. Patients using NOVOLIN R vials must never share needles or syringes with another person. Sharing poses a risk for transmission of blood-borne pathogens.
5.2 Hyperglycemia or Hypoglycemia with Changes in Insulin Regimen
Changes in an insulin regimen (e.g., insulin strength, manufacturer, type, injection site or method of administration) may affect glycemic control and predispose to hypoglycemia [see Warnings and Precautions (5.3)] or hyperglycemia. Repeated insulin injections into areas of lipodystrophy or localized cutaneous amyloidosis have been reported to result in hyperglycemia; and a sudden change in the injection site (to an unaffected area) has been reported to result in hypoglycemia [see Adverse Reactions (6)].
Make any changes to a patient’s insulin regimen under close medical supervision with increased frequency of blood glucose monitoring. Advise patients who have repeatedly injected into areas of lipodystrophy or localized cutaneous amyloidosis to change the injection site to unaffected areas and closely monitor for hypoglycemia. For patients with type 2 diabetes, dosage adjustments of concomitant anti-diabetic products may be needed.
5.3 Hypoglycemia
Hypoglycemia is the most common adverse reaction of all insulins, including NOVOLIN R. Severe hypoglycemia can cause seizures, may lead to unconsciousness, may be life threatening or cause death. Hypoglycemia can impair concentration ability and reaction time; this may place the patient and others at risk in situations where these abilities are important (e.g., driving or operating other machinery).
Hypoglycemia can happen suddenly and symptoms may differ in each patient and change over time in the same patient. Symptomatic awareness of hypoglycemia may be less pronounced in patients with longstanding diabetes in patients with diabetic neuropathy, in patients using medications that block the sympathetic nervous system (e.g., beta-blockers) [see Drug Interactions (7)], or in patients who experience recurrent hypoglycemia.
Risk Factors for Hypoglycemia
The risk of hypoglycemia after an injection is related to the duration of action of the insulin and, in general, is highest when the glucose lowering effect of the insulin is maximal. As with all insulins, the glucose lowering effect time course of NOVOLIN R may vary in different individuals or at different times in the same individual and depends on many conditions, including the area of injection as well as the injection site blood supply and temperature [see Clinical Pharmacology (12.2)]. Other factors which may increase the risk of hypoglycemia include changes in meal pattern (e.g., macronutrient content or timing of meals), changes in level of physical activity, or changes to concomitant drugs [see Drug Interactions (7)]. Patients with renal or hepatic impairment may be at higher risk of hypoglycemia [see Use in Specific Populations (8.6, 8.7)].
Risk Mitigation Strategies for Hypoglycemia
Patients and caregivers must be educated to recognize and manage hypoglycemia. Self-monitoring of blood glucose plays an essential role in the prevention and management of hypoglycemia. In patients at higher risk for hypoglycemia and patients who have reduced symptomatic awareness of hypoglycemia, increased frequency of blood glucose monitoring is recommended.
5.4 Hypoglycemia Due to Medication Errors
Accidental mix-ups between NOVOLIN R and other insulin products have been reported. To avoid medication errors between NOVOLIN R and other insulins, instruct patients to always check the insulin label before each injection.
5.5 Hypersensitivity Reactions
Severe, life-threatening, generalized allergy, including anaphylaxis, can occur with NOVOLIN R. Generalized allergy to insulin may manifest as a whole body rash (including pruritus), dyspnea, wheezing, hypotension, tachycardia, or diaphoresis. If hypersensitivity reactions occur, discontinue NOVOLIN R; treat per standard of care and monitor until symptoms and signs resolve. NOVOLIN R is contraindicated in patients who have had hypersensitivity reactions to insulin human injection or its excipients.
5.6 Hypokalemia
All insulins, including NOVOLIN R, cause a shift in potassium from the extracellular to intracellular space, possibly leading to hypokalemia. Untreated hypokalemia may cause respiratory paralysis, ventricular arrhythmia, and death. Monitor potassium levels in patients at risk for hypokalemia if indicated (e.g., patients using potassium-lowering medications, patients taking medications sensitive to serum potassium concentration).
5.7 Fluid Retention and Heart Failure with Concomitant Use of PPAR-gamma agonists
Thiazolidinediones (TZDs), which are peroxisome proliferator-activated receptor (PPAR)-gamma agonists, can cause dose-related fluid retention when used in combination with insulin. Fluid retention may lead to or exacerbate heart failure. Patients treated with insulin, including NOVOLIN R, and a PPAR-gamma agonist should be observed for signs and symptoms of heart failure. If heart failure develops, it should be managed according to current standards of care, and discontinuation or dose reduction of the PPAR-gamma agonist must be considered.
6. Adverse Reactions/Side Effects
The following adverse reactions are also discussed elsewhere in the labeling:
- •
- Hypoglycemia [see Warnings and Precautions (5.3)]
- •
- Medication Errors [see Warnings and Precautions (5.4)]
- •
- Hypersensitivity Reactions [see Warnings and Precautions (5.5)]
- •
- Hypokalemia [see Warnings and Precautions (5.6)]
Adverse Reactions from Clinical Studies or Postmarketing Reports
The following additional adverse reactions have been identified during clinical studies or from postmarketing reports with use of NOVOLIN R. Because some of these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or to establish a causal relationship to drug exposure.
Adverse reactions associated with insulin initiation and glucose control intensification
Intensification or rapid improvement in glucose control has been associated with a transitory, reversible ophthalmologic refraction disorder, worsening of diabetic retinopathy, and acute painful peripheral neuropathy. Over the long-term, improved glycemic control decreases the risk of diabetic retinopathy and neuropathy.
Hypersensitivity reactions
Severe, life-threatening, generalized allergy, including anaphylaxis.
Hypoglycemia
Hypoglycemia is the most commonly observed adverse reaction in NOVOLIN R.
Hypokalemia
NOVOLIN R can cause a shift in potassium from the extracellular to intracellular space, possibly leading to hypokalemia.
Injection site reactions
NOVOLIN R can cause local injection site reactions including redness, swelling, or itching at the site of injection. These reactions usually resolve in a few days to a few weeks, but in some occasions, may require discontinuation. Localized reactions and generalized myalgias have been reported with the use of metacresol, which is an excipient in NOVOLIN R.
Lipodystrophy
Administration of insulin subcutaneously, including NOVOLIN R, has resulted in lipoatrophy (depression in the skin) or lipohypertrophy (enlargement or thickening of tissue) [see Dosage and Administration (2.2)] in some patients.
Localized Cutaneous Amyloidosis
Localized cutaneous amyloidosis at the injection site has occurred. Hyperglycemia has been reported with repeated insulin injections into areas of localized cutaneous amyloidosis; hypoglycemia has been reported with a sudden change to an unaffected injection site.
Medication Errors
Medication errors in which other insulins have been accidentally substituted for NOVOLIN R have been identified during postapproval use.
Peripheral edema
Insulins, including NOVOLIN R, may cause sodium retention and edema, particularly if previously poor metabolic control is improved by intensified insulin therapy.
Weight gain
Weight gain can occur with insulins, including NOVOLIN R, and has been attributed to the anabolic effects of insulin and the decrease in glucosuria.
Immunogenicity
As with all therapeutic proteins, insulin administration may cause anti-insulin antibodies to form. Increases in titers of anti-insulin antibodies that react with human insulin have been observed in patients treated with NOVOLIN R.
Related/similar drugs
7. Drug Interactions
Table 1: Clinically Significant Drug Interactions with NOVOLIN R
|
Drugs that May Increase the Risk of Hypoglycemia |
|
|
Drugs: |
Antidiabetic agents, ACE inhibitors, angiotensin II receptor blocking agents, disopyramide, fibrates, fluoxetine, monoamine oxidase inhibitors, pentoxifylline, pramlintide, salicylates, somatostatin analog (e.g., octreotide), and sulfonamide antibiotics |
|
Intervention: |
Dose adjustment and increased frequency of glucose monitoring may be required when NOVOLIN R is co-administered with these drugs. |
|
Drugs that May Decrease the Blood Glucose Lowering Effect of NOVOLIN R |
|
|
Drugs: |
Atypical antipsychotics (e.g., olanzapine and clozapine), corticosteroids, danazol, diuretics, estrogens, glucagon, isoniazid, niacin, oral contraceptives, phenothiazines, progestogens (e.g., in oral contraceptives), protease inhibitors, somatropin, sympathomimetic agents (e.g., albuterol, epinephrine, terbutaline), and thyroid hormones. |
|
Intervention: |
Dose adjustment and increased frequency of glucose monitoring may be required when NOVOLIN R is co-administered with these drugs. |
|
Drugs that May Increase or Decrease the Blood Glucose Lowering Effect of NOVOLIN R |
|
|
Drugs: |
Alcohol, beta-blockers, clonidine, and lithium salts. Pentamidine may cause hypoglycemia, which may sometimes be followed by hyperglycemia. |
|
Intervention: |
Dose adjustment and increased frequency of glucose monitoring may be required when NOVOLIN R is co-administered with these drugs. |
|
Drugs that May Blunt Signs and Symptoms of Hypoglycemia |
|
|
Drugs: |
Beta-blockers, clonidine, guanethidine, and reserpine |
|
Intervention: |
Increased frequency of glucose monitoring may be required when NOVOLIN R is co-administered with these drugs. |
8. Use In Specific Populations
8.1 Pregnancy
Risk Summary
Available data from published studies over decades have not established an association with human insulin use during pregnancy and major birth defects, miscarriage or adverse maternal or fetal outcomes (see Data). There are risks to the mother and fetus associated with poorly controlled diabetes in pregnancy (see Clinical Considerations). Animal reproduction studies were not performed.
The estimated background risk of major birth defects is 6-10% in women with pre-gestational diabetes with a HbA1c >7 and has been reported to be as high as 20-25% in women with a HbA1c >10. The estimated background risk of miscarriage for the indicated population is unknown. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2-4% and 15-20%, respectively.
Clinical Considerations
Disease-associated maternal and/or embryo/fetal risk
Poorly controlled diabetes in pregnancy increases the maternal risk for diabetic ketoacidosis, pre-eclampsia, spontaneous abortions, preterm delivery, and delivery complications. Poorly controlled diabetes increases the fetal risk for major birth defects, stillbirth, and macrosomia-related morbidity.
Data
Human Data
While available studies cannot definitively establish the absence of risk, published data from retrospective studies, open-label, randomized, parallel studies and meta-analyses have not established an association with human insulin use during pregnancy and major birth defects, miscarriage, or adverse maternal or fetal outcomes. All available studies have methodological limitations including lack of blinding, unclear methods of randomization, and small sample size.
8.2 Lactation
Risk Summary
Available data from published literature suggest that exogenous human insulin products, including NOVOLIN R, are transferred into human milk. There are no adverse reactions reported in the breastfed infants in the literature. There are no data on the effects of exogenous human insulin products, including NOVOLIN R, on milk production. The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for NOVOLIN R and any potential adverse effects on the breastfed infant from NOVOLIN R or from the underlying maternal condition.
8.4 Pediatric Use
NOVOLIN R is indicated to improve glycemic control in pediatric patients with diabetes mellitus.
The dosage of NOVOLIN R must be individualized in pediatric patients based on metabolic needs and frequent monitoring of blood glucose to reduce the risk of hypoglycemia [see Dosage and Administration (2.3) and Warnings and Precautions (5.3)].
8.5 Geriatric Use
In clinical trials 18 of 1285 patients (1.4%) with type 1 diabetes and 151 of 635 patients (24%) with type 2 diabetes treated with NOVOLIN R were ≥65 years of age. Therefore, conclusions are limited regarding the efficacy and safety of NOVOLIN R in patients ≥65 years of age. The effect of age on the pharmacokinetics and pharmacodynamics of NOVOLIN R has not been studied.
Elderly patients using NOVOLIN R, may be at increased risk of hypoglycemia due to co-morbid disease [see Warnings and Precautions (5.3)].
8.6 Renal Impairment
The effect of renal impairment on the pharmacokinetics and pharmacodynamics of NOVOLIN R has not been studied. Patients with renal impairment are at increased risk of hypoglycemia and may require more frequent NOVOLIN R dose adjustment and more frequent blood glucose monitoring [see Warnings and Precautions (5.3)].
8.7 Hepatic Impairment
The effect of hepatic impairment on the pharmacokinetics and pharmacodynamics of NOVOLIN R has not been studied. Patients with hepatic impairment are at increased risk of hypoglycemia and may require more frequent NOVOLIN R dose adjustment and more frequent blood glucose monitoring [see Warnings and Precautions (5.3)].
10. Overdosage
Excess insulin administration may cause hypoglycemia and, particularly when given intravenously, hypokalemia. Mild episodes of hypoglycemia usually can be treated with oral glucose. Adjustments in drug dosage, meal patterns, or exercise may be needed. More severe episodes with coma, seizure, or neurologic impairment can be treated with intramuscular or subcutaneous glucagon or intravenous glucose. Sustained carbohydrate intake and observation may be necessary because hypoglycemia may recur after apparent clinical recovery. Hypokalemia must be corrected appropriately [see Warnings and Precautions (5.3, 5.6)].
11. Novolin R Description
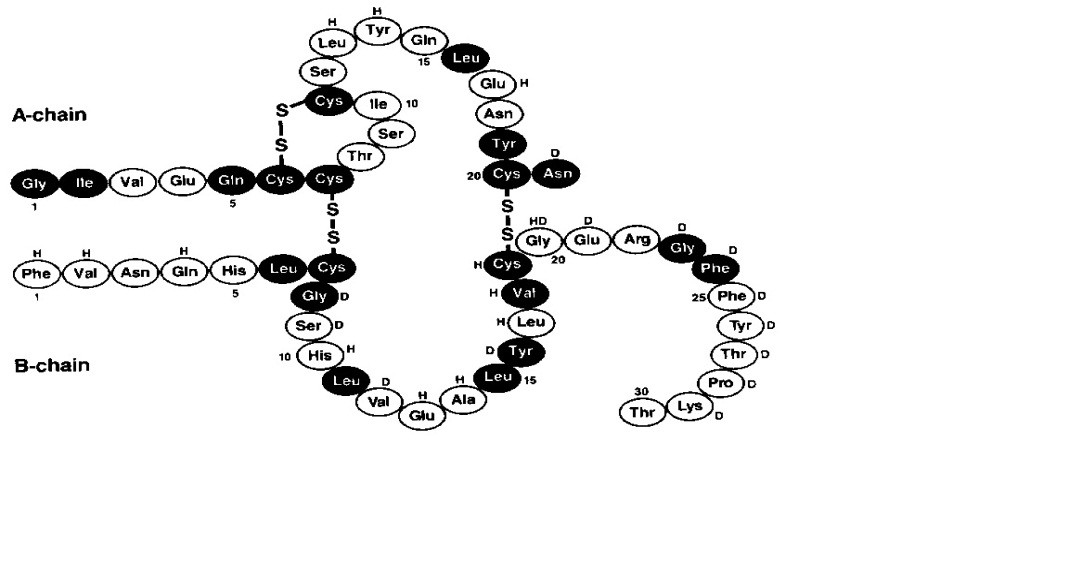
Insulin human is a short-acting human insulin produced by recombinant DNA technology, utilizing Saccharomyces cerevisiae (baker’s yeast) as the production organism and has the empirical formula C257H383N65O77S6 with a molecular weight of 5808 Da.
Figure 1: Structural formula of NOVOLIN R
NOVOLIN R (insulin human) injection is a sterile, clear and colorless solution for subcutaneous or intravenous use. Each mililiter of NOVOLIN R contains 100 units of insulin human, and glycerin (16 mg), metacresol (3 mg), zinc (approximately 21 mcg/mL) and Water for Injection. Hydrochloric acid 2N and sodium hydroxide 2N may be added during manufacture to adjust pH. The pH is 7.0 to 7.8.
12. Novolin R - Clinical Pharmacology
12.1 Mechanism of Action
The primary activity of insulin, including NOVOLIN R is the regulation of glucose metabolism. Insulins lower blood glucose by stimulating peripheral glucose uptake, especially by skeletal muscle and fat, and by inhibiting hepatic glucose production. Insulin inhibits lipolysis and proteolysis, and enhances protein synthesis.
12.2 Pharmacodynamics
NOVOLIN R is a short-acting insulin. The time course of insulin action (i.e., glucose lowering) may vary considerably in different individuals, within the same individual, and different doses. When injected subcutaneously, the glucose-lowering effect of NOVOLIN R begins approximately 30 minutes post-dose, is maximal between 1.5 and 3.5 hours post-dose and terminates approximately 8 hours post-dose. The onset of action of NOVOLIN R, when administered intravenously, is more rapid in comparison to the subcutaneous administration. When injected subcutaneously, NOVOLIN R has a slower onset of action and longer duration of action compared to the rapid-acting insulin analogs.
12.3 Pharmacokinetics
After single subcutaneous administration of 0.1 unit/kg of NOVOLIN R to healthy subjects, peak insulin concentrations occurred between 1.5 to 2.5 hours post-dose. On average, insulin concentrations returned to baseline at around 5 hours post-dose.
The effects of gender, age, obesity, renal and hepatic impairment on the pharmacodynamics and pharmacokinetics of NOVOLIN R have not been studied.
13. Nonclinical Toxicology
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Standard 2-year carcinogenicity studies in animals have not been performed to evaluate the carcinogenic potential of NOVOLIN R.
NOVOLIN R is not mutagenic in the following in vitro tests: The chromosomal aberration assay in human lymphocytes, the micronucleus assay in mouse polychromatic erythrocytes, and the mutation frequency assay in Chinese hamster cells.
Standard reproduction and teratology studies in animals, including fertility assessments have not been conducted with NOVOLIN R.
16. How is Novolin R supplied
16.1 How Supplied
NOVOLIN R (insulin human) injection is 100 units/mL (U-100), a clear and colorless solution available as:
|
10 mL multiple-dose vial |
NDC 0169-1833-11 |
|
|
ReliOn® brand |
NDC 0169-1833-02 |
|
|
3 mL single-patient-use FlexPen |
NDC 0169-3003-15 |
|
|
ReliOn® brand |
NDC 0169-3003-25 |
The NOVOLIN R FlexPen dials in 1-unit increments.
16.2 Storage and Handling
- Dispense in the original sealed carton with the enclosed Instructions for Use.
- •
- Do not freeze.
- •
- Do not use if it has been frozen.
- •
- Do not use after the expiration date.
- •
- Do not expose to excessive heat or light.
NOVOLIN R FlexPen must never be shared between patients, even if the needle is changed. Always remove and discard the needle after each injection from the NOVOLIN R FlexPen and store without a needle attached.
Patients using NOVOLIN R vials must never share needles or syringes with another person. Always use a new disposable syringe or needle for each injection to prevent contamination.
Table 2: Storage Conditions and Expiration Dates for NOVOLIN R
|
Not In-use (Unopened) Refrigerated (36°F - 46°F [2°C - 8°C]) |
Not In-use (Unopened ) Room Temperature (see temperature below) |
In-use (Opened) Room Temperature (see temperature below) |
|
|
10 mL multiple-dose vial |
Until expiration date |
42 days up to 77°F (25°C) |
42 days up to 77°F (25°C) (Do not refrigerate) |
|
3 mL single-patient-use FlexPen |
Until expiration date |
28 days up to 86°F (30°C) |
28 days up to 86°F (30°C) (Do not refrigerate) |
Intravenous infusion bags prepared as indicated [see Dosage and Administration (2.2)] are stable at room temperature for 24 hours.
17. Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Patient Information and Instructions for Use).
Never Share a NOVOLIN R FlexPen or Syringe between Patients
Advise patients using NOVOLIN R vials or FlexPen not to share needles, syringes or FlexPen with another person. Sharing poses a risk for transmission of blood-borne pathogens [see Warnings and Precautions (5.1)].
Hyperglycemia or Hypoglycemia
Inform patients that hypoglycemia is the most common adverse reaction with insulin. Instruct patients on self-management procedures including glucose monitoring, proper injection technique, and management of hypoglycemia and hyperglycemia, especially at initiation of NOVOLIN R therapy. Instruct patients on handling of special situations such as intercurrent conditions (illness, stress, or emotional disturbances), an inadequate or skipped insulin dose, inadvertent administration of an increased insulin dose, inadequate food intake, and skipped meals. Instruct patients on the management of hypoglycemia [see Warnings and Precautions (5.3)].
Inform patients that their ability to concentrate and react may be impaired as a result of hypoglycemia. Advise patients who have frequent hypoglycemia or reduced or absent warning signs of hypoglycemia to use caution when driving or operating machinery.
Advise patients that changes in insulin regimen can predispose to hyperglycemia or hypoglycemia and that changes in insulin regimen should be made under close medical supervision [see Warnings and Precautions (5.2).
Hypoglycemia due to Medication Errors
Instruct patients to always check the insulin label before each injection to avoid mix-ups between insulin products [see Warnings and Precautions (5.4)].
Hypersensitivity Reactions
Advise patients that hypersensitivity reactions have occurred with NOVOLIN R. Inform patients on the symptoms of hypersensitivity reactions and to seek medical attention if they occur [see Warnings and Precautions (5.5)].
Novolin®, FlexPen® and Novo Nordisk® are registered trademarks of Novo Nordisk A/S.
ReliOn® is a registered trademark of Walmart Inc. and is used under license by Novo Nordisk Inc.
Patent Information: http://novonordisk-us.com/products/product-patents.html
© 2022 Novo Nordisk
Manufactured by:
Novo Nordisk Inc.
800 Scudders Mill Road
Plainsboro, New Jersey 08536
1-800-727-6500
U.S. License Number 1261
For information about NOVOLIN R contact:
Novo Nordisk Inc.
800 Scudders Mill Road
Plainsboro, New Jersey 08536
www.novonordisk-us.com
1-800-727-6500 (Se habla español)
Patient Package Insert
Patient Information
NOVOLIN® R (NO-voe-lin)
(insulin human) injection for subcutaneous or intravenous use
Do not share your Novolin R FlexPen or syringes with other people, even if the needle has been changed. You may give other people a serious infection, or get a serious infection from them.
What is Novolin R?
Novolin R is a man-made insulin that is used to control high blood sugar in adults and children with diabetes mellitus.
Who should not use Novolin R?
Do not use Novolin R if you:
- •
- are having an episode of low blood sugar (hypoglycemia).
- •
- have an allergy to human insulin or any of the ingredients in Novolin R. See the end of this Patient Information leaflet for a complete list of ingredients in Novolin R.
Before using Novolin R, tell your healthcare provider about all of your medical conditions, including if you:
- •
- have liver or kidney problems.
- •
- take other medicines, especially ones called TZDs (thiazolidinediones).
- •
- have heart failure or other heart problems. If you have heart failure, it may get worse while you take TZDs with Novolin R.
- •
- are pregnant or plan to become pregnant. Talk with your healthcare provider about the best way to control your blood sugar if you plan to become pregnant or while you are pregnant.
- •
- are breastfeeding or plan to breastfeed. Novolin R may pass into your breast milk. Talk with your healthcare provider about the best way to feed your baby while using Novolin R.
Tell your healthcare provider about all of the medicines you take, including prescription and over-the-counter medicines, vitamins and herbal supplements.
Before you start using Novolin R, talk to your healthcare provider about low blood sugar and how to manage it.
How should I use Novolin R?
- •
- Read the detailed Instructions for Use that comes with your Novolin R.
- •
- Use Novolin R exactly as your healthcare provider tells you to. Your healthcare provider should tell you how much Novolin R to use and when to use it.
- •
- Use Novolin R about 30 minutes before eating a meal.
- •
- Know the type, strength, and amount of insulin you use. Do not change the type or amount of insulin you use unless your healthcare provider tells you to. The amount of insulin and the best time for you to take your insulin may need to change if you use different types of insulin.
- •
- Check your insulin label each time you give your injection to make sure you are using the correct insulin.
- •
- Inject Novolin R under the skin (subcutaneously) of your stomach area, buttocks, upper legs (thighs), or upper arms. Do not inject Novolin R into your vein (intravenously) or use in an insulin infusion pump. Novolin R may be given into your vein only by your healthcare provider.
- o
- Do not mix Novolin R with any other insulin except Novolin N. If Novolin R is mixed with Novolin N, Novolin R should be drawn into the syringe first. Inject immediately after mixing.
- •
- Change (rotate) your injection sites within the area you choose with each dose to reduce your risk of getting lipodystrophy (pits in skin or thickened skin) and localized cutaneous amyloidosis (skin with lumps) at the injection sites.
- o
- Do not use the exact same spot for each injection.
- o
- Do not inject where the skin has pits, is thickened, or has lumps.
- o
- Do not inject where the skin is tender, bruised, scaly or hard, or into scars or damaged skin.
- •
- Check your blood sugar levels. Ask your healthcare provider what your blood sugars should be and when you should check your blood sugar levels.
Keep Novolin R and all medicines out of the reach of children.
Your dose of Novolin R may need to change because of:
- •
- change in level of physical activity or exercise, weight gain or loss, increased stress, illness, change in diet, or because of other medicines you take.
What should I avoid while using Novolin R?
While using Novolin R do not:
- •
- drive or operate heavy machinery until you know how Novolin R affects you.
- •
- drink alcohol or use prescription or over-the-counter medicines that contain alcohol.
What are the possible side effects of Novolin R?
Novolin R may cause serious side effects that can lead to death, including:
- •
- low blood sugar (hypoglycemia). Signs and symptoms of low blood sugar may include:
- o
- dizziness or lightheadedness, sweating, confusion, headache, blurred vision, slurred speech, shakiness, fast heartbeat, anxiety, irritability or mood changes, hunger.
- o
- Your healthcare provider may prescribe a glucagon emergency kit so that others can give you an injection if your blood sugar becomes too low (hypoglycemia) and you are unable to take sugar by mouth.
- •
- severe allergic reaction (whole body reaction). Get medical help right away if you have any of these signs or symptoms of a severe allergic reaction:
- o
- a rash over your whole body, have trouble breathing, a fast heartbeat, or sweating.
- •
- low potassium in your blood (hypokalemia).
- •
- heart failure. Taking certain diabetes pills called thiazolidinediones or “TZDs” with Novolin R may cause heart failure in some people. This can happen even if you have never had heart failure or heart problems before. If you already have heart failure it may get worse while you take TZDs with Novolin R. Your healthcare provider should monitor you closely while you are taking TZDs with Novolin R. Tell your healthcare provider if you have any new or worse symptoms of heart failure including:
- o
- shortness of breath, swelling of your ankles or feet, sudden weight gain.
- o
- Treatment with TZDs and Novolin R may need to be adjusted or stopped by your healthcare provider if you have new or worse heart failure.
Get emergency medical help if you have:
- •
- severe hypoglycemia needing hospitalization or emergency room care, and be sure to tell the hospital staff the units of Novolin R your healthcare provider has prescribed for you.
- •
- trouble breathing, shortness of breath, fast heartbeat, swelling of your face, tongue, or throat, sweating, extreme drowsiness, dizziness, confusion.
The most common side effects of Novolin R include:
- •
- low blood sugar (hypoglycemia), allergic reactions including reactions at your injection site, skin thickening or pits at the injection site (lipodystrophy), weight gain, and swelling (edema) in hands or feet.
These are not all of the possible side effects of Novolin R. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
General information about the safe and effective use of Novolin R
Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. Do not use Novolin R for a condition for which it was not prescribed. Do not give Novolin R to other people, even if they have the same symptoms you have. It may harm them.
This Patient Information leaflet summarizes the most important information about Novolin R. If you would like more information, talk with your healthcare provider. You can ask your healthcare provider or pharmacist for information about Novolin R that is written for healthcare providers.
For more information about Novolin R, call 1-800-727-6500 or go to www.novonordisk-us.com.
What are the ingredients in Novolin R?
Active ingredient: insulin human
Inactive ingredients: glycerin, metacresol, zinc, Water for Injection. Hydrochloric acid and sodium hydroxide may be added.
Novolin®, FlexPen® and Novo Nordisk® are registered trademarks of Novo Nordisk A/S.
© 2022 Novo Nordisk
Manufactured by:
Novo Nordisk Inc.
800 Scudders Mill Road
Plainsboro, New Jersey 08536
U.S. License Number 1261
For information about Novolin R contact:
Novo Nordisk Inc.
800 Scudders Mill Road
Plainsboro, New Jersey 08536
1-800-727-6500 (Se habla español)
www.novonordisk-us.com
This Patient Information has been approved by the U.S. Food and Drug Administration.
Revised: 11/2022
INSTRUCTIONS FOR USE
Novolin® R
(insulin human)
injection, for subcutaneous use
10 mL multiple-dose vial (100 units/mL, U-100)
Please read the following Instructions for Use carefully before using your Novolin® R 10 mL vial and each time you get a refill. You should read the instructions in this manual even if you have used an insulin 10 mL vial before. There may be new information.
Before starting, gather all of the supplies that you will need to use for preparing and giving your insulin injection.
Never re-use syringes and needles.
How should I use the Novolin R vial?
1. Check to make sure that you have the correct type of insulin. This is especially important if you use different types of insulin.
2. Look at the vial and the insulin. The insulin should be clear and colorless. The tamper-resistant cap should be in place before the first use. If the cap had been removed before your first use of the vial, or if the insulin is cloudy, colored, or contains any particles, do not use it and call Novo Nordisk at 1-800-727-6500.
3. Wash your hands with soap and water. Clean your injection site with an alcohol swab and let the injection site dry before you inject. Talk with your healthcare provider about how to rotate injection sites and how to give an injection.
4. If you are using a new vial, pull off the tamper-resistant cap.
Wipe the rubber stopper with an alcohol swab.
5. Do not roll or shake the vial. Shaking right before the dose is drawn into the syringe may cause bubbles or foam. This can cause you to draw up the wrong dose of insulin.
6. Pull back the plunger on the syringe until the black tip reaches the marking for the number of units you will inject.
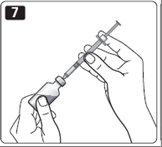
7. Push the needle through the rubber stopper of the vial.
8. Push the plunger all the way in to force air into the vial.
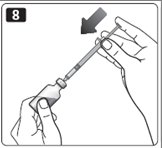
9. Turn the vial and syringe upside down and slowly pull the plunger back to a few units beyond the correct dose.
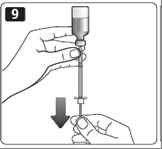
10. If there are any air bubbles, tap the syringe gently with your finger to raise the air bubbles to the top. Then slowly push the plunger to the marking for your correct dose. This process should move any air bubbles present in the syringe back into the vial.
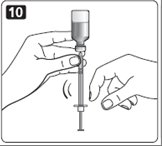
11. Check to make sure you have the right dose of Novolin R in the syringe.
12. Pull the syringe out of the vial’s rubber stopper.
13. Novolin R can be injected under the skin (subcutaneously) of your stomach area, buttocks, upper legs (thighs), or upper arms. Change (rotate) your injection sites within the area you choose for each dose to reduce your risk of getting lipodystrophy (pits in skin or thickened skin) and localized cutaneous amyloidosis (skin with lumps) at the injection sites. For each injection, change (rotate) your injection site within the area of skin that you use. Do not use the same injection site for reach injection. Do not inject where the skin has pits, is thickened, or has lumps. Do not inject where the skin is tender, bruised, scaly or hard, or into scars or damaged skin. Your healthcare provider should tell you if you need to pinch the skin before and while inserting the needle. This can vary from patient to patient so it is important to ask your healthcare provider if you did not receive instructions on pinching the skin. Insert the needle into the skin. Press the plunger of the syringe to inject the insulin. When you are finished injecting the insulin, pull the needle out of your skin. You may see a drop of Novolin R at the needle tip. This is normal and has no effect on the dose you just received. If you see blood after you take the needle out of your skin, press the injection site lightly with a piece of gauze or an alcohol wipe. Do not rub the area.
14. After your injection, do not recap the needle. Place used syringes, needles and used insulin vials in a disposable puncture-resistant sharps container, or some type of hard plastic or metal container with a screw on cap such as a detergent bottle or coffee can.
15. Ask your healthcare provider about the right way to throw away used syringes and needles. There may be state or local laws about the right way to throw away used syringes and needles. Do not throw away used needles and syringes in household trash or recycle.
How should I mix Novolin R with Novolin N?
Different insulins should be mixed only under instruction from a healthcare provider. Do not mix Novolin R with any other type of insulin except Novolin N. Novolin R should be mixed with Novolin N right before use. When you are mixing Novolin R insulin with Novolin N, always draw the Novolin R (clear) insulin into the syringe first.
1. Add together the total number of units of Novolin N and Novolin R that you need to inject. Your total dose of medicine to inject will be the amount of Novolin N and Novolin R in the syringe after drawing up both insulins. For example, if you need 5 units of Novolin N and 2 units of Novolin R, the total dose of insulin in the syringe would be 7 units.
Preparing your Novolin N and Novolin R insulins for injection:
2. Roll the Novolin N vial between your hands until all of the liquid in the vial is cloudy.
3. Pull the plunger of the syringe down so that the dark end is lined up to the number of units needed for your Novolin N. This will draw into the syringe the same amount of air as the Novolin N dose needed.
4. Put the needle through the rubber stopper of the cloudy Novolin N bottle. After you inject the air into the Novolin N vial, remove the needle from the vial but do not withdraw any of the Novolin N insulin. Putting air in the bottle makes it easier to draw the insulin out of the bottle.
5. Pull the plunger of the syringe down to the number of units needed for your Novolin R insulin. After you draw the air into the syringe, inject the air into the Novolin R vial.
Drawing up and mixing your Novolin N and Novolin R insulins for injection:
6. With the needle in place, turn the clear insulin vial of Novolin R upside down and slowly pull the plunger back to a few units beyond the right dose of Novolin R. The tip of the needle must be in the Novolin R liquid to get the full dose and not an air dose.
7. Check the syringe for air bubbles. If you see air bubbles, tap the syringe gently with your finger to raise the air bubbles to the top. Then slowly push the plunger to the marking for your correct dose. This process should move any air bubbles in the syringe back into the vial.
8. After withdrawing the needle from the Novolin R vial, insert the needle into the Novolin N vial.
9. Turn the Novolin N vial upside down with the syringe and needle still in the vial. Slowly pull the plunger back to withdraw your Novolin N dose.
Remember the total dose of medicine in the syringe should be your total dose of Novolin N and Novolin R insulins. (See Step 1 under “How should I mix Novolin R with Novolin N?”)
10. Inject your insulin right away otherwise it might not work properly.
How should I store Novolin® R?
- •
- Do not freeze Novolin R. Do not use Novolin R if it has been frozen.
- •
- Keep Novolin R away from heat or light.
- •
- All unopened vials:
- o
- Store unopened Novolin R vials in the refrigerator at 36°F to 46°F (2°C to 8°C).
- o
- Unopened vials may be used until the expiration date printed on the label, if they have been stored in the refrigerator.
- o
- Unopened vials should be thrown away after 42 days, if they are stored at room temperature up to 77°F (25°C).
- •
- After vials have been opened:
- o
- Opened Novolin R vials can be stored at room temperature up to 77°F (25°C). Do not refrigerate.
- o
- Throw away all opened Novolin R vials after 42 days, even if they still have insulin left in them.
This Patient Instructions for Use has been approved by the Food and Drug Administration.
Manufactured by:
Novo Nordisk Inc.
800 Scudders Mill Road
Plainsboro, New Jersey 08536
1-800-727-6500
U.S. License Number 1261
Revised: 11/2022
INSTRUCTIONS FOR USE
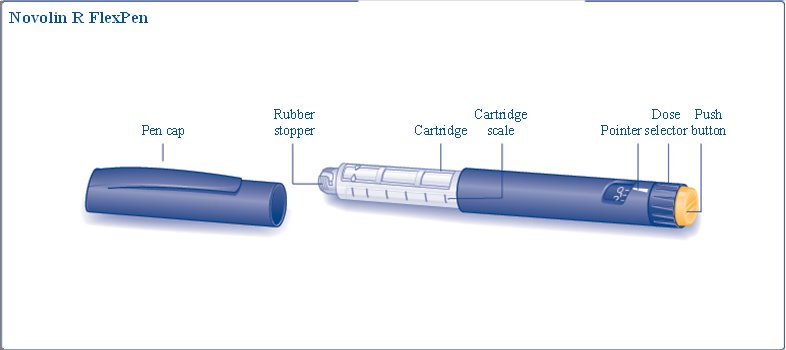
Novolin® R FlexPen®
(insulin human)
injection, for subcutaneous use
Introduction
Please read the following instructions carefully before using your Novolin R FlexPen.
Do not share your Novolin R FlexPen with other people, even if the needle has been changed. You may give other people a serious infection, or get a serious infection from them.
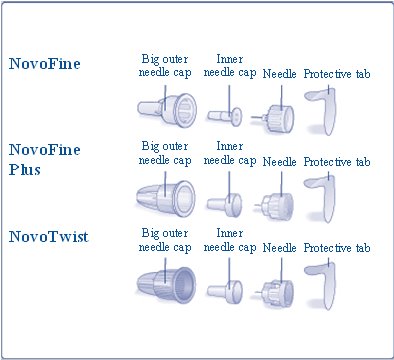
Novolin R FlexPen is a disposable, single-patient-use, dial-a-dose insulin pen. You can select doses from 1 to 60 units in increments of 1 unit. Novolin R FlexPen is designed to be used with NovoFine, NovoFine Plus or NovoTwist needles.
 People who are blind or have vision problems should not use Novolin R FlexPen without help from a person trained to use Novolin R FlexPen.
People who are blind or have vision problems should not use Novolin R FlexPen without help from a person trained to use Novolin R FlexPen.
Getting ready
Make sure you have the following items:
- •
- Novolin R FlexPen
- •
- New NovoFine, NovoFine Plus or NovoTwist needle
- •
- Alcohol swab
- •
- Gauze pad
Preparing your Novolin R FlexPen
Wash your hands with soap and water. Before you start to prepare your injection, check the label to make sure that you are taking the right type of insulin. This is especially important if you take more than 1 type of insulin. Novolin R should look clear and colorless. Do not use your Novolin R FlexPen if the liquid contains particles or is colored.
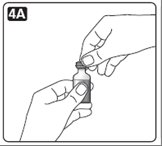
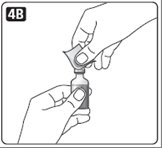
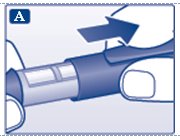
A. Pull off the pen cap (see diagram A).
Wipe the rubber stopper with an alcohol swab.
Attaching the needle
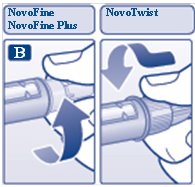
B. Remove the protective tab from a disposable needle.
Screw the needle tightly onto your Novolin R FlexPen. It is important that the needle is put on straight (see diagram B).
Never place a disposable needle on your Novolin R FlexPen until you are ready to take your injection.
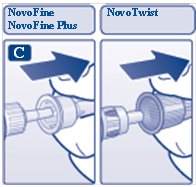
C. Pull off the big outer needle cap (see diagram C).
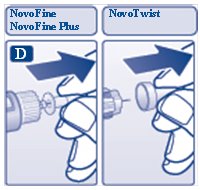
D. Pull off the inner needle cap and dispose of it (see diagram D).
 Always use a new needle for each injection to help ensure sterility and prevent blocked needles. Do not reuse or share your needles with other people. You may give other people a serious infection, or get a serious infection from them.
Always use a new needle for each injection to help ensure sterility and prevent blocked needles. Do not reuse or share your needles with other people. You may give other people a serious infection, or get a serious infection from them.
 Be careful not to bend or damage the needle before use.
Be careful not to bend or damage the needle before use.
 To reduce the risk of unexpected needle sticks, never put the inner needle cap back on the needle.
To reduce the risk of unexpected needle sticks, never put the inner needle cap back on the needle.
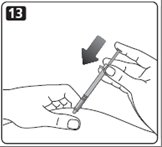
Giving the airshot before each injection
Before each injection small amounts of air may collect in the cartridge during normal use. To avoid injecting air and to make sure you take the right dose of insulin:
E. Turn the dose selector to select 2 units (see diagram E).
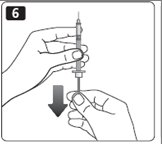
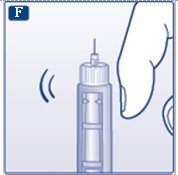
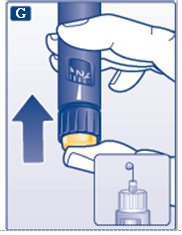
F. Hold your Novolin R FlexPen with the needle pointing up. Tap the cartridge gently with your finger a few times to make any air bubbles collect at the top of the cartridge (see diagram F).
G. Keep the needle pointing upwards, press the push-button all the way in (see diagram G). The dose selector returns to 0.
- A drop of insulin should appear at the needle tip. If not, change the needle and repeat the procedure no more than 6 times.
- If you do not see a drop of insulin after 6 times, do not use the Novolin R FlexPen and contact Novo Nordisk at 1-800-727-6500.
- A small air bubble may remain at the needle tip, but it will not be injected.
Selecting your dose
Check and make sure that the dose selector is set at 0.
H. Turn the dose selector to the number of units you need to inject. The pointer should line up with your dose.
The dose can be corrected either up or down by turning the dose selector in either direction until the correct dose lines up with the pointer (see diagram H). When turning the dose selector, be careful not to press the push-button as insulin will come out.
You cannot select a dose larger than the number of units left in the cartridge.
You will hear a click for every single unit dialed. Do not set the dose by counting the number of clicks you hear.
 Do not use the cartridge scale printed on the cartridge to measure your dose of insulin.
Do not use the cartridge scale printed on the cartridge to measure your dose of insulin.
Giving the injection
Give the injection exactly as shown to you by your healthcare provider. Your healthcare provider should tell you if you need to pinch the skin before injecting. Wipe the skin with an alcohol swab and let the area dry.
Novolin R can be injected under the skin (subcutaneously) of your stomach area, buttocks, upper legs (thighs), or upper arms.
Change (rotate) your injection sites within the area you choose for each dose to reduce your risk of getting lipodystrophy (pits in skin or thickened skin) and localized cutaneous amyloidosis (skin with lumps) at the injection sites. Do not use the same injection site for each injection. Do not inject where the skin has pits, is thickened, or has lumps. Do not inject where the skin is tender, bruised, scaly or hard, or into scars or damaged skin.
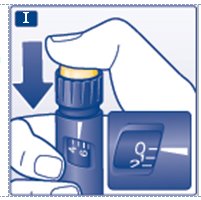
I. Insert the needle into your skin.
- Inject the dose by pressing the push-button all the way in until the 0 lines up with the pointer (see diagram I). Be careful only to push the button when injecting.
- Turning the dose selector will not inject insulin.
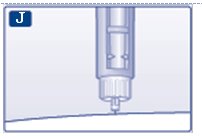
J. Keep the needle in the skin for at least 6 seconds, and keep the push-button pressed all the way in until the needle has been pulled out from the skin (see diagram J). This will make sure that the full dose has been given.
- You may see a drop of insulin at the needle tip. This is normal and has no effect on the dose you just received. If blood appears after you take the needle out of your skin, press the injection site lightly with a gauze pad or an alcohol swab. Do not rub the area.
After the injection
Do not recap the needle. Recapping can lead to a needle stick injury. Remove the needle from the Novolin R FlexPen after each injection and dispose of it. This helps to prevent infection, leakage of insulin, and will help to make sure you inject the right dose of insulin.
If you do not have a sharps container, carefully slip the needle into the outer needle cap. Safely remove the needle and throw it away as soon as you can.
- •
- The used Novolin R FlexPen may be thrown away in your household trash after you have removed the needle.
- •
- Put your used needles in a FDA-cleared sharps disposal container right away after use. Do not throw away (dispose of) loose needles in your household trash.
- •
- If you do not have a FDA-cleared sharps disposal container, you may use a household container that is:
- o
- made of a heavy-duty plastic
- o
- can be closed with a tight-fitting, puncture-resistant lid, without sharps being able to come out
- o
- upright and stable during use
- o
- leak-resistant
- o
- properly labeled to warn of hazardous waste inside the container
- •
- When your sharps disposal container is almost full, you will need to follow your community guidelines for the right way to dispose of your sharps disposal container. There may be state or local laws about how you should throw away used needles and syringes. For more information about safe sharps disposal, and for specific information about sharps disposal in the state that you live in, go to the FDA’s website at: http://www.fda.gov/safesharpsdisposal.
Do not dispose of your used sharps disposal container in your household trash unless your community guidelines permit this. Do not recycle your used sharps disposal container.
- •
- When there is not enough medicine left in your Novolin R FlexPen for your prescribed dose, the Novolin R FlexPen may be thrown away in your household trash after you have removed the needle. The Novolin R FlexPen prevents the cartridge from being completely emptied. It is designed to deliver 300 units.
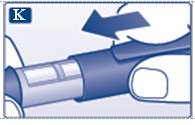
K. Put the pen cap on the Novolin R FlexPen and store the Novolin R FlexPen without the needle attached (see diagram K). Storing without the needle attached helps prevent leaking, blocking of the needle, and air from entering the Pen.
How should I store Novolin R FlexPen?
- •
- Do not freeze Novolin R. Do not use Novolin R if it has been frozen.
- •
- Keep Novolin R away from heat and light.
- •
- Until first use:
- o
- Store unused Novolin R FlexPen in the refrigerator at 36°F to 46°F (2°C to 8°C).
- o
- Unused Novolin R FlexPen may be used until the expiration date printed on the label, if kept in the refrigerator at 36°F to 46°F (2°C to 8°C).
- o
- Unused Novolin R FlexPen stored at room temperature should be thrown away after 28 days.
- •
- In-use:
- o
- Store the Novolin R FlexPen you are currently using out of the refrigerator at room temperature up to 86°F (30°C) for up to 28 days.
- o
- The Novolin R FlexPen you are using should be thrown away after 28 days, even if it still has insulin left in it.
- o
- Store the Novolin R FlexPen without the needle attached.
Maintenance
For the safe and proper use of your Novolin R FlexPen be sure to handle it with care. Avoid dropping your Novolin R FlexPen as it may damage it. If you are concerned that your Novolin R FlexPen is damaged, use a new one. You can clean the outside of your Novolin R FlexPen by wiping it with a damp cloth. Do not soak or wash your Novolin R FlexPen as it may damage it. Do not refill your Novolin R FlexPen.
 Remove the needle from Novolin R FlexPen after each injection. This helps to ensure sterility, prevent leakage of insulin, and will help to make sure you inject the right dose of insulin for future injections.
Remove the needle from Novolin R FlexPen after each injection. This helps to ensure sterility, prevent leakage of insulin, and will help to make sure you inject the right dose of insulin for future injections.
 Be careful when handling used needles to avoid needle sticks and transfer of infectious diseases.
Be careful when handling used needles to avoid needle sticks and transfer of infectious diseases.
 Keep your Novolin R FlexPen and needles out of the reach of children.
Keep your Novolin R FlexPen and needles out of the reach of children.
 Use Novolin R FlexPen as directed to treat your diabetes.
Use Novolin R FlexPen as directed to treat your diabetes.
 Do not share your Novolin R FlexPen or needles with other people. You may give other people a serious infection, or get a serious infection from them.
Do not share your Novolin R FlexPen or needles with other people. You may give other people a serious infection, or get a serious infection from them.
 Always use a new needle for each injection.
Always use a new needle for each injection.
 Novo Nordisk is not responsible for harm due to using this insulin pen with products not recommended by Novo Nordisk.
Novo Nordisk is not responsible for harm due to using this insulin pen with products not recommended by Novo Nordisk.
 As a precautionary measure, always carry a spare insulin delivery device in case your Novolin R FlexPen is lost or damaged.
As a precautionary measure, always carry a spare insulin delivery device in case your Novolin R FlexPen is lost or damaged.
 Remember to keep the disposable Novolin R FlexPen with you. Do not leave it in a car or other location where it can get too hot or too cold.
Remember to keep the disposable Novolin R FlexPen with you. Do not leave it in a car or other location where it can get too hot or too cold.
This Instructions for Use has been approved by the U.S. Food and Drug Administration.
Manufactured by:
Novo Nordisk Inc.
800 Scudders Mill Road
Plainsboro, New Jersey 08536
1-800-727-6500
U.S. License Number 1261
Revised: 11/2022
PRINCIPAL DISPLAY PANEL – 10 mL Vial
NDC 0169-1833-11
Novolin® R
(insulin human) injection
100 units/mL (U-100)
For subcutaneous or intravenous use
10 mL multiple-dose vial
Novo Nordisk®
Principal Display Panel – 10 mL Vial ReliOn
NDC 0169-1833-02
Novolin®R
(insulin human) injection
100 units/mL (U-100)
For subcutaneous or intravenous use
10 mL multiple-dose vial
ReliOn®
PRINCIPAL DISPLAY PANEL - 3 mL FlexPen
- NDC 0169-3003-15 List 300315
Novolin®R
FlexPen®
(insulin human) injection
For Single Patient Use Only
100 units/mL (U-100)
5 x 3 mL Prefilled Pens
For subcutaneous use only
Recommended for use with NovoFine®, NovoFine®
Plus or NovoTwist® disposable needles.
Store unopened pens refrigerated at 36°F to 46°F
(2°C to 8°C) in the original carton to protect from
light until expiration date or first use.
Do not freeze. After first use, store at room
temperature (up to 86°F [30°C]), discard after 28 days.
Dispense in this sealed carton.
- R
novo nordisk®
Principal Display Panel – 3 mL FlexPen ReliOn
- NDC 0169-3003-25 List 300325
Novolin® R
FlexPen®
(insulin human) injection
For Single Patient Use Only
100 units/mL (U-100)
5 x 3 mL Prefilled Pens
For subcutaneous use only
Recommended for use with NovoFine®, NovoFine®
Plus or NovoTwist® disposable needles.
Store unopened pens refrigerated at 36°F to 46°F
(2°C to 8°C) in the original carton to protect from
light until expiration date or first use.
Do not freeze. After first use, store pen at
room temperature (up to 86°F [30°C]), discard
after 28 days.
Dispense in this sealed carton.
- R
ReliOn®
| NOVOLIN
R
human insulin injection, solution |
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
| NOVOLIN
R
human insulin injection, solution |
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
| Labeler - Novo Nordisk (622920320) |
Frequently asked questions
- Is Novolin the same as Humulin?
- How and where should I inject insulin?
- Can Trulicity be used with insulin?
- What are the different types of insulin?
- What is the difference between regular insulin and lispro (Humalog)?
- How long can Humulin be unrefrigerated?
- Is Humulin fast or long-acting insulin?
- How long does Humulin last?
- Can regular and lispro insulin (Humalog) be mixed?
More about Novolin R (insulin regular)
- Check interactions
- Compare alternatives
- Pricing & coupons
- Reviews (6)
- Side effects
- Dosage information
- During pregnancy
- Drug class: insulin
- En español
Patient resources
Professional resources
Other brands
Humulin R, Humulin R U-500 (Concentrated)