Hicon Kit: Package Insert / Prescribing Info
Package insert / product label
Generic name: sodium iodide i 131
Dosage form: oral solution, capsules
Drug classes: Antithyroid agents, Therapeutic radiopharmaceuticals
Medically reviewed by Drugs.com. Last updated on Feb 3, 2025.
On This Page
- Indications and Usage
- Dosage and Administration
- Dosage Forms and Strengths
- Contraindications
- Warnings and Precautions
- Adverse Reactions/Side Effects
- Drug Interactions
- Use In Specific Populations
- Overdosage
- Description
- Clinical Pharmacology
- How Supplied/Storage and Handling
- Storage and Handling
- Patient Counseling Information
Highlights of Prescribing Information
HICON® (for the preparation of sodium iodide I 131 solution or sodium iodide I 131 capsules), therapeutic, for oral use.
Initial U.S. Approval: 1971
Recent Major Changes
Indications and Usage for Hicon Kit
HICON® is a radioactive therapeutic agent indicated for the treatment of hyperthyroidism and selected cases of carcinoma of the thyroid. (1)
Hicon Kit Dosage and Administration
- The concentrated sodium iodide I 131 solution USP provided with HICON® must be diluted. (2.2)
- See Full Prescribing Information for important administration instructions and dilution and preparation instructions for sodium iodide l 131 capsules or oral solution. (2.2, 2.4)
- The recommended dose is based on the thyroid gland uptake as well as the size of the gland:
Dosage Forms and Strengths
Vials: Sodium Iodide I 131 Solution [9,250 MBq (250 mCi), 18,500 MBq (500 mCi), and 37,000 MBq (1,000 mCi) at time of calibration] for the preparation of sodium iodide I 131 capsules, therapeutic or sodium iodide I 131 solution, therapeutic. (3)
Contraindications
Warnings and Precautions
- Radiation-induced thyroiditis may cause or worsen hyperthyroidism. Consider pre-treatment with anti-thyroid medications. (5.1)
- Multiple non-thyroid radiation toxicities, including hematopoietic suppression: Individualize dose and monitor for toxicity. (5.2)
- Embryo-Fetal toxicity: May cause severe and irreversible hypothyroidism in the neonate. Verify pregnancy status in females of reproductive potential prior to initiating treatment. Females and males of reproductive potential should use effective contraception. (5.4, 8.1, 8.3)
- Radiation exposure to breast tissue with lactation: Sodium iodide I 131 concentrates in the breast of lactating women. Discontinue breast feeding at least 6 weeks prior to therapy. (5.5, 8.2)
Adverse Reactions/Side Effects
Common adverse reactions reported with therapeutic doses of sodium iodide I 131 include local swelling, radiation sickness, sialadenitis, salivary gland dysfunction, bone marrow depression, lacrimal gland dysfunction, hypothyroidism, hyperthyroidism, thyrotoxic crisis. (6)
To report SUSPECTED ADVERSE REACTIONS, contact Jubilant DraxImage Inc., dba Jubilant RadiopharmaTM at 1-888-633-5343 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Drug Interactions
Use In Specific Populations
See 17 for PATIENT COUNSELING INFORMATION.
Revised: 1/2025
Full Prescribing Information
1. Indications and Usage for Hicon Kit
HICON® is indicated for the treatment of hyperthyroidism and selected cases of thyroid carcinoma.
2. Hicon Kit Dosage and Administration
2.1 Radiation Safety
- HICON® is a radioactive drug. Handle with appropriate safety measures to minimize radiation exposure to the patient and healthcare workers [see Warnings and Precautions (5.7)]:
- Use only by, or under the direction of, physicians who are qualified by specific training and experience in the safe use and handling of radioactive materials, and whose experience and training have been approved by the appropriate governmental agency authorized to license the use of radiopharmaceuticals.
- Use waterproof gloves when handling and administering the product.
- Maintain adequate shielding during the life of the product.
- Measure patient dose with a suitable radioactivity calibration system immediately prior to administration.
2.2 Important Administration Instructions
- Do not directly administer the concentrated sodium iodide I 131 solution USP provided with HICON® to patients. The concentrated sodium iodide I 131 solution USP must be diluted and prepared prior to administration [see Dosage and Administration (2.4)].
- Obtain a pregnancy test in females of reproductive potential prior to administration to verify the absence of pregnancy [see Contraindications (4) and Use in Specific Populations (8.1, 8.3)].
- Instruct patients to fast at least 2 hours before and 2 hours after administration to ensure absorption.
- Instruct patients to hydrate before and after administration of sodium iodide I 131 and to void frequently to enhance urinary elimination of the radioiodide that is not absorbed by the thyroid gland [see Warnings and Precautions (5.2)].
- Instruct patients to maintain a low-iodide diet two weeks prior to radioiodide administration and continue for several days during the uptake or imaging process [see Warnings and Precautions (5.8) and Drug Interactions (7)].
- Instruct patients to discontinue the anti-thyroid therapy three days before administration of sodium iodide I 131 [see Warnings and Precautions (5.8) and Drug Interactions (7)].
- For patients with a history of renal impairment, evaluate renal function for therapeutic planning and consider dosimetry [see Use in Specific Populations (8.6)].
- Obtain a complete blood count within one month of therapy. If patients show leukopenia or thrombocytopenia, dosimetry should be used to determine a safe sodium iodide I 131 activity, while delivering less than 2 Gy to the bone marrow [see Warnings and Precautions (5.2)].
2.3 Recommended Dosage and Administration
Individualization of Therapy
The recommended dose for orally administered sodium iodide I 131 capsules or solution is based on the thyroid gland uptake as well as the size of the gland. Thyroidal uptake and size should be determined by the physician prior to treatment and may be useful in calculating the therapeutic dose to be administered to the individual patient.
Treatment of Hyperthyroidism
The recommended dose is 148 MBq to 370 MBq (4 mCi to 10 mCi) administered orally. Toxic nodular goiter may require a larger dose.
Treatment of Thyroid Carcinoma
The recommended dose is 1,100 MBq to 3,700 MBq (30 mCi to 100 mCi) administered orally. For subsequent ablation of metastases, the recommended dose is 3,700 MBq to 7,400 MBq (100 mCi to 200 mCi) administered orally.
2.4 Dilution and Preparation Instructions
Drug Handling
- Wear waterproof gloves throughout the entire handling and administration procedure.
- Make all transfers of radioactive solutions with an adequately shielded syringe or remote handling equipment and maintain adequate shielding around the vial during the useful life of the radioactive product.
Preparation of Dilute Sodium Iodide I 131 Solution
- Using the calibration date and radionuclide concentration on the label of the product vial, calculate the required volume to produce the necessary dose in MBq or mCi.
- Using a shielded syringe, remove the required volume.
- Using the shielded syringe, transfer the required volume to a suitably shielded receiving vial.
- Add the solution diluent to the receiving vial to produce a final dose of the desired volume.
- The recommended diluent is Purified Water USP containing 0.2% sodium thiosulfate USP as a reducing agent. Acidic diluents should not be used as they may cause the pH to drop below 7.5 and stimulate the volatilization of Iodine I 131 hydriodic acid.
- Present the dose in a shielded container for administration to the patient with a straw.
Preparation of Sodium Iodide I 131 Capsules
- HICON® includes one LARGE gelatin capsule and one SMALL gelatin capsule for each dose prepared. Each LARGE capsule is empty, and each SMALL capsule contains approximately 300 mg of dibasic sodium phosphate anhydrous USP as the absorbing buffer.
- Using the calibration date and radionuclide concentration on the label of the product vial, calculate the required volume to produce the necessary dose in MBq or mCi.
- Open one LARGE capsule supplied with HICON® by pulling apart the capsule into two pieces as illustrated below:
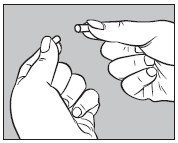
-
Insert an unopened SMALL capsule supplied with HICON® into the bottom half of the empty LARGE capsule as illustrated below:
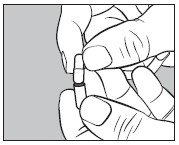
- With an appropriate syringe, withdraw the required volume of sodium iodide I 131 solution USP (maximum 150 microliters) from the vial as illustrated below:
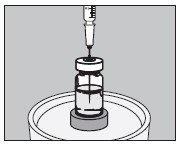
- Inject into the center of the SMALL capsule through the top as illustrated below and wait for 30 seconds to allow the solution to be absorbed by the absorbing buffer:
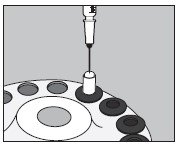
- Slip the upper half of the LARGE capsule over the bottom half to completely cover the SMALL capsule and push down gently until locked as illustrated below:
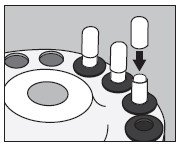
- Measure the patient dose in a suitable radioactivity calibration system immediately prior to administration.
- Prepared capsules may be stored in a suitable polypropylene container and placed inside a lead pot until use, within seven days.
2.5 Radiation Dosimetry
- The biokinetic modeling and radiation dose distributions associated with thyroid uptake of iodide I 131 depend on dietary intake of stable iodide and presume normal production of thyroid hormone. Table 1 shows a range of uptake percentages in an average adult (73.7 kg reference model). Table 1 is not intended to be used for treatment planning.
- For a thyroid blocked from iodide uptake in the production of hormones, the effective half-life of iodide I 131 is approximately 1.4 hours; for “low” to “high” uptake, the effective half-life of I 131 ranges from approximately 80 hours to 90 hours.
|
||||
| Organ
| Thyroid uptake of I 131 (% administered activity A0) 24 h after oral administration |
|||
| Blocked thyroid (0% A0) | Low uptake†
(16% A0) | Medium uptake†
(26% A0) | High uptake†
(36% A0) |
|
| Adrenals | 0.044 | 0.051 | 0.055 | 0.059 |
| Bone surfaces | 0.03 | 0.089 | 0.12 | 0.16 |
| Brain | 0.021 | 0.093 | 0.13 | 0.17 |
| Breast | 0.02 | 0.038 | 0.048 | 0.058 |
| Gallbladder wall | 0.037 | 0.043 | 0.046 | 0.049 |
| Gastrointestinal tract | ||||
| Esophagus | 0.024 | 0.1 | 0.14 | 0.19 |
| Stomach wall | 0.87 | 0.77 | 0.71 | 0.66 |
| Small intestine wall | 0.035 | 0.033 | 0.032 | 0.032 |
| Colon wall | 0.14 | 0.14 | 0.14 | 0.14 |
| (Upper large intestine wall) | 0.12 | 0.12 | 0.12 | 0.12 |
| (Lower large intestine wall) | 0.17 | 0.17 | 0.17 | 0.16 |
| Heart wall | 0.062 | 0.089 | 0.1 | 0.12 |
| Kidneys | 0.27 | 0.27 | 0.27 | 0.27 |
| Liver | 0.05 | 0.093 | 0.12 | 0.14 |
| Lungs | 0.053 | 0.1 | 0.13 | 0.15 |
| Muscles | 0.026 | 0.084 | 0.12 | 0.15 |
| Ovaries | 0.038 | 0.037 | 0.036 | 0.035 |
| Pancreas | 0.06 | 0.064 | 0.066 | 0.068 |
| Red marrow | 0.031 | 0.072 | 0.095 | 0.12 |
| Salivary glands | 0.27 | 0.22 | 0.19 | 0.16 |
| Skin | 0.019 | 0.043 | 0.057 | 0.071 |
| Spleen | 0.064 | 0.069 | 0.072 | 0.075 |
| Testes | 0.025 | 0.024 | 0.023 | 0.22 |
| Thymus | 0.024 | 0.1 | 0.14 | 0.19 |
| Thyroid | 2.2 | 280‡ | 430‡ | 580‡ |
| Urinary bladder wall | 0.54 | 0.45 | 0.39 | 0.34 |
| Uterus | 0.045 | 0.042 | 0.04 | 0.038 |
| Remaining organs | 0.029 | 0.084 | 0.11 | 0.15 |
|
Effective dose per administered activity (mSv/MBq) | 0.28 | 14‡ | 22‡ | 29‡ |
3. Dosage Forms and Strengths
HICON® is available in 1 mL size, clear vials containing a colorless, aqueous, concentrated Sodium Iodide I 131 Solution USP [9,250 MBq (250 mCi), 18,500 MBq (500 mCi), and 37,000 MBq (1,000 mCi) at time of calibration] for the preparation of sodium iodide I 131 capsules, therapeutic or sodium iodide I 131 solution, therapeutic. Refer to Table 2 for the radioactivity and volume in each vial. Large gelatin capsules (empty) and small gelatin capsules containing approximately 300 mg of dibasic sodium phosphate anhydrous as the absorbing buffer are supplied along with HICON® for the preparation of sodium iodide I 131 capsules, therapeutic.
|
|
| Total Radioactivity*/ Vial |
Solution Volume (mL) / Vial |
| 9,250 MBq (250 mCi) |
0.25 |
| 18,500 MBq (500 mCi) |
0.5 |
|
37,000 MBq (1,000 mCi) | 1 |
4. Contraindications
HICON® is contraindicated in:
- Patients with vomiting and diarrhea [see Warnings and Precautions (5.7)].
- Patients with thyroid malignancies shown to have no iodide update, which include the majority of medullary or anaplastic carcinomas.
- Patients receiving concurrent anti-thyroid therapy [see Warnings and Precautions (5.1) and Drug Interactions (7)].
- Pregnancy [see Warnings and Precautions (5.4), Use in Specific Populations (8.1)].
- Lactation [see Warnings and Precautions (5.5), Use in Specific Populations (8.2)].
5. Warnings and Precautions
5.1 Radiation-induced Thyroiditis
Sodium iodide I 131 may cause thyroiditis with gland enlargement and release of thyroid hormone, which may cause or aggravate hyperthyroidism, thyroid storm and thyrotoxic cardiac disease [see Adverse Reactions (6)]. When treating hyperthyroidism, consider pre-treatment anti-thyroid medication to help deplete the thyroid hormone content within the gland. Discontinue the anti-thyroid medication at least three days before administration of sodium iodide I 131 [see Drug Interactions (7)]. Consider a beta-blocker pre or post-treatment to minimize the risk of hyperthyroidism and thyroid storm.
Thyroiditis may cause gland enlargement resulting in tenderness and swelling of the neck, pain on swallowing, sore throat, and cough; which may occur approximately the third day after sodium iodide I 131 administration. Consider management with pain-reliever or anti-inflammatory medications.
5.2 Radiation-induced Toxicities
Sodium Iodide I 131 may cause radiation induced toxicities [see Adverse Reactions (6)]:
- Dose-dependent fatalities (bone marrow suppression, malignancy).
- Dose-dependent hematopoietic suppression which manifests as a transient thrombocytopenia or neutropenia 3 to 5 weeks following sodium iodide I 131 administrations, may lead to increased susceptibility to infections or bleeding.
- Salivary gland toxicity: sialadenitis, xerostomia.
- Lacrimal gland toxicity: conjunctivitis, xerophthalmia, and epiphora.
- Increased risk of developing new solid tumors and leukemias.
Obtain a complete blood count within one month of therapy. If patients show leukopenia or thrombocytopenia, dosimetry should be used to determine a safe sodium iodide I 131 activity, while delivering less than 2 Gy to the bone marrow.
Advise good hydration for one week following sodium iodide I 131 administration and stimulate salivary flow via a sialagogue (e.g. sugar-free candy or gum, pilocarpine, and ascorbic acid) to reduce radiation exposure to the salivary glands.
Advise patients to void frequently after administration of radioiodide to enhance excretion.
5.3 Hypersensitivity Reactions
Hypersensitivity reactions including anaphylaxis may occur in patients who receive sodium iodide I 131. Although iodide is not considered an allergen, hypersensitivity reactions may occur in relation with excipients or chemical component of the capsule, such as sodium thiosulfate. Obtain and document an allergy history, particularly a sulfite allergy. Emergency resuscitation equipment and personnel should be immediately available [see Adverse Reactions (6)].
5.4 Embryo-Fetal Toxicity
HICON® is contraindicated in pregnancy because sodium iodide I 131 crosses the placenta and fetal exposure can lead to neonatal hypothyroidism. Multiple reports in the published literature describe hypothyroidism in the neonates following in utero exposure to sodium iodide I 131. Some cases of neonatal hypothyroidism were severe and irreversible. Verify pregnancy status of females of reproductive potential prior to initiating HICON® treatment. Advise females and males of reproductive potential to use effective contraception during treatment with HICON® and for at least 6 months after the last dose [see Use in Specific Populations (8.1, 8.3)].
5.5 Increased Radiation Exposure to Breast Tissue with Lactation
HICON® is contraindicated in lactating women because sodium iodide I 131 concentrates in the breast via the increased expression of the sodium iodide symporter in breast tissue with lactation. The literature describes moderate to marked radioiodine uptake in the breast tissue for 5 to 32 weeks post cessation of breast feeding. Advise lactating women to discontinue breast feeding at least 6 weeks prior to administration of sodium iodide I 131 to allow sufficient time for involution to occur and to avoid excess concentration of sodium iodide I 131 in breast tissue. Consider administration of drugs to suppress lactation. Consider diagnostic scintigraphy before administration of sodium iodide I 131 to assess the persistence of uptake by breast tissue. If sodium iodide I 131 is administered in the postpartum period, the lactating mother should not breastfeed the infant [see Use in Specific Populations (8.2)].
5.6 Transient Infertility
Transient dose-related impairment of testicular function in men and transient ovarian insufficiency in women has been reported after sodium iodide I 131 therapy. Sperm banking for men may be considered prior to administration of HICON® for thyroid carcinoma [see Use in Specific Populations (8.3)].
5.7 Radiation Exposure to Other Individuals
Household Contacts
Instruct patients to follow radiation safety precautions after receiving HICON® to minimize the radiation contamination of other persons or the environment. Patients should avoid close contact with others, especially pregnant women and children, and take care to avoid contamination of other persons or the environment with body fluids.
Patients and Healthcare Providers
HICON® contributes to a patient’s overall long-term cumulative radiation exposure, which is associated with an increased risk of cancer. Follow safe handling and administration to minimize radiation exposure to the patient and healthcare providers.
5.8 Risk of Decreased Effectiveness of Therapy
Certain food or drugs may alter the thyroid uptake of sodium iodide I 131 and diminish its effectiveness. Recent intake of stable iodide in any form, or the use of thyroid or anti-thyroid drugs may diminish thyroid uptake of sodium iodide I 131 [see Drug Interactions (7)].
6. Adverse Reactions/Side Effects
The following clinically significant adverse reactions are described below and elsewhere in labeling:
- Radiation-induced Thyroiditis [see Warnings and Precautions (5.1)].
- Radiation-induced Toxicities [see Warnings and Precautions (5.2)].
- Hypersensitivity Reactions [see Warnings and Precautions (5.3)].
- Embryo-Fetal Toxicity [see Warnings and Precautions (5.4), Use in Specific Populations (8.1)].
- Increased Radiation Exposure to Breast Tissue with Lactation [see Warnings and Precautions (5.5), Use in Specific Populations (8.2)].
- Transient Infertility [see Warnings and Precautions (5.6), Use in Specific Populations (8.3)].
- Radiation Exposure to Other Individuals [see Warnings and Precautions (5.7)].
- Risk of Decreased Effectiveness of Therapy [see Warnings and Precautions (5.8)].
6.1 Postmarketing Experience
The following adverse reactions have been reported during post-approval use of sodium iodide I 131 (Table 3). Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
| System Organ Class*
| Symptoms*
|
| Cardiac disorders | Chest pain, tachycardia |
| Congenital, familial and genetic disorders | Chromosomal abnormalities, congenital hypothyroidism |
| Endocrine disorders | Hyperthyroidism, hypoparathyroidism, hypothyroidism, thyrotoxic crisis |
| Eye disorders | Lacrimal gland dysfunction |
| Gastrointestinal disorders | Gastritis, nausea, salivary gland dysfunction, sialadenitis, vomiting |
| General disorders and administration site conditions | Local swelling of thyroid or sites of iodide avid tumor |
| Hematologic and lymphatic disorders including fatalities | Anemia, blood dyscrasia, bone marrow depression, leukopenia, thrombocytopenia |
| Immune system disorders | Bronchospasm |
| Neoplasms benign, malignant and unspecified (including cysts and polyps) | Acute leukemia, solid cancer |
| Nervous system disorders | †Cerebral edema, headache |
| Respiratory, thoracic and mediastinal disorders | ‡Pulmonary fibrosis, ‡radiation pneumonitis |
| Skin and subcutaneous tissue disorders | Hives, itching, rash |
Related/similar drugs
7. Drug Interactions
- Concomitant use of bone marrow depressants may enhance the depression of the hematopoietic system caused by the use of large doses of sodium iodide I 131 [see Warnings and Precautions (5.2)].
- Many drugs and iodide-containing foods interfere with the accumulation of radioiodide by the thyroid. Review the patient’s history, current medications, and recent diagnostic tests prior to the administration of sodium iodide I 131 [see Warnings and Precautions (5.8)].
- Advise patients to maintain a low-iodide diet two weeks prior to radioiodide administration and continue for several days during the uptake or imaging process and to discontinue taking the following products before they undergo the procedure as shown in Table 4.
| Type of Medication | Recommended time of withdrawal
|
| Thionamide medications (e.g., propylthiouracil, methimazole, carbimazole) | 3 days |
| Multivitamins containing iodide | 10 days |
| Natural or synthetic thyroid hormones
triiodothyronine thyroxine | 2 weeks 4 weeks |
| Iodide-containing foods: iodized salt, dairy products, egg yolks, seafood, turkey and liver | 2 weeks |
| Kelp, agar, carrageenan, Lugol solution | 3 weeks |
| Saturated solution of potassium iodide | 3 weeks |
| Topical iodide (e.g., surgical skin preparation) | 3 weeks |
| Intravenous radiographic contrast agents
Water soluble Lipophilic | 2 months 6 months |
| Amiodarone | 6 months |
8. Use In Specific Populations
8.1 Pregnancy
Risk Summary
HICON® is contraindicated in pregnancy because fetal exposure can lead to neonatal hypothyroidism, which in some cases is severe and irreversible [See Warnings and Precautions (5.4)]. Data from the published literature describe reports of neonatal thyroid abnormalities after fetal exposure; including agenesis of the thyroid and hypothyroidism (see Clinical Considerations, Data). No animal reproductive studies have been conducted.
Clinical Considerations
Fetal/ Neonatal Adverse Reactions
A fetus exposed to sodium iodide I 131 can develop neonatal hypothyroidism. Delay in diagnosis of neonatal hypothyroidism after exposure to sodium iodide I 131 in utero can result in severe sequelae such as cognitive impairment and delayed bone age. Monitor thyroid function in any infant born after in utero exposure to sodium iodide I 131.
Data
Human Data
Sodium iodide I 131 crosses the placenta and the fetal thyroid begins to concentrate iodide during the 10th to 12th week of gestation. In literature reports of maternal exposures to sodium iodide I 131 at doses of 333 MBq to 8,325 MBq (9 mCi to 225 mCi) during 4 to 26 weeks gestational age, the most common adverse outcomes were hypothyroid infants and children.
8.2 Lactation
Risk Summary
HICON® is contraindicated during lactation because I 131 concentrates in the breast during lactation via the increased expression of the sodium iodide symporter in breast tissue and can lead to hypothyroidism in the infant through breastfeeding. If sodium iodide I 131 is administered postpartum, breastfeeding should not be restarted for the remainder of the postpartum period. In addition, to minimize the absorbed radiation dose to the breast tissue, breastfeeding and breast-pumping should be discontinued for at least 6 weeks before administration of sodium iodide I 131 [see Data and Warnings and Precautions (5.5)].
Infants exposed to sodium iodide I 131 through breast milk are at risk for development of hypothyroidism because sodium iodide I 131 is distributed into breast milk and may reach concentrations equal to or greater than concentrations in maternal plasma (see Data).
Data
Published literature describes sodium iodide I 131 transfer into breast milk and uptake by the thyroid of the breastfed infant. The amount of sodium Iodide I 131 detected in the breast milk at 36 to 48 hours after administration is 1% to 27% of the injected dose (with injected doses between 1.1 MBq (0,0297 mCi) to 5,143 MBq (139 mCi)).
8.3 Female and Males of Reproductive Potential
HICON® is contraindicated in pregnancy because of the risk of fetal hypothyroidism [see Warnings and Precautions (5.4) and Use in Specific Populations (8.1)].
Pregnancy Testing
Obtain a pregnancy test in females of reproductive potential and verify the absence of pregnancy within 24 hours prior to administration of treatment [see Dosage and Administration (2.2)].
Contraception
Advise females and males of reproductive potential to use effective contraception during treatment with HICON® and for at least six months after the last dose of HICON®.
Infertility
Females
Fertility may be impaired with HICON® treatment. Transient amenorrhea and ovarian insufficiency have been observed after sodium iodide I 131 therapy in females. The literature describes reports of transient menstrual cycle irregularities, including amenorrhea, and ovarian failure in females treated with cumulative doses of 1,000 MBq to 59,000 MBq (27 mCi to 1,595 mCi) sodium iodide I 131. In a published literature analysis, the effects on fertility occurred in up to 30% of women treated with sodium iodide I 131, and may resolve 12 months after treatment.
Males
Fertility may be impaired with HICON® treatment. Discuss sperm banking for males who are expected to receive a high cumulative dose of sodium iodide I 131. Transient dose-related impairment of testicular function after sodium iodide I 131 therapy has been reported in the published literature. The literature describes reports of males treated with sodium iodide I 131 at doses of 370 MBq to 22,000 MBq (10 mCi to 595 mCi) resulting in transiently impaired testicular function (including spermatogenesis). The risk of persistent testicular dysfunction increases after administration of repeated or high cumulative radioiodide exposure.
8.4 Pediatric Use
The safety and effectiveness of HICON® have not been established in pediatric patients. Pediatric patients are at an increased lifetime risk for malignancy from radiation exposure.
8.5 Geriatric Use
Clinical experience has not identified differences in safety or effectiveness in geriatric patients compared to younger patients. However, elderly patients are more likely to have decreased renal function and radiation exposure is greater in patients with impaired renal function [see Use in Specific Populations (8.6), Clinical Pharmacology (12.3)].
8.6 Renal Impairment
HICON® is primarily excreted by the kidneys. Renal function impairment decreases excretion of sodium iodide I 131 and increases the radiation exposure and risk of radiation toxicity. For patients with a history of renal impairment, evaluate renal function for therapeutic planning and consider dosimetry. Sodium Iodide I 131 is dialyzable. Hemodialysis can be used to reduce total body radiation exposure [see Clinical Pharmacology (12.3)].
10. Overdosage
In case of exposure to a radioactive dose of sodium iodide I 131 exceeding the intended therapeutic dose, provide general supportive care, promote frequent voiding, monitor for bone marrow and thyroid suppression. Consider administering a thyroid blocking agent (e.g. potassium iodide (KI) or perchlorate) promptly within 4 to 6 hours after the exposure. Assess the benefit of administering a thyroid blocking agent against the risk of failure of sodium iodide I 131 therapy. Appropriate replacement therapy is recommended if hypothyroidism occurs.
11. Hicon Kit Description
11.1 Chemical Characteristics
HICON®, a radioactive therapeutic agent, provides a concentrated solution of sodium iodide I 131 with a radioconcentration of 37,000 MBq/mL (1,000 mCi/mL). Each mL of the concentrated solution contains 37,000 MBq (1,000 mCi) of no-carrier-added sodium iodide I 131, disodium edetate dihydrate USP as a stabilizer, sodium thiosulfate pentahydrate USP as a reducing agent, and dibasic sodium phosphate anhydrous USP. The pH of the concentrated solution is between 7.5 and 10.
The concentrated solution provided with HICON® is used for the preparation of sodium iodide I 131 capsules or sodium iodide I 131 solution of varying strengths for oral administration for therapy.
Sodium iodide I 131 solution is designated chemically as Na 131I and has a molecular weight of 153.99 g/mol. Hard gelatin capsules, provided for the preparation of the sodium iodide I 131 capsules final dosage form, contain approximately 300 mg of dibasic sodium phosphate anhydrous USP as the absorbing buffer.
11.2 Physical Characteristics
Iodide I 131 decays by beta emission and associated gamma emission with a physical half-life of 8.02 days. The principal radiation emissions are listed in Table 5.
| Radiation
| Mean % per Disintegration | Mean Energy (keV) |
| Beta-1 | 2.1% | 69.4 |
| Beta-3 | 7.2% | 96.6 |
| Beta-4 | 89.4% | 191.6 |
| Gamma-7 | 6.1% | 284.3 |
| Gamma-14 | 81.2% | 364.5 |
| Gamma-18 | 7.1% | 637.0 |
11.3 External Radiation
The specific gamma-ray constant for iodide I 131 is 4.26 × 10-13 C•m2•kg-1•MBq-1•s-1 (2.2 R•cm2/mCi•hr). The first half-value thickness of lead (Pb) for iodide I 131 is 0.27 cm. A range of values for the relative attenuation of the radiation emitted by iodide I 131 that results from interposition of various thicknesses of Pb is shown in Table 6. For example, the use of 2.59 cm of Pb will decrease the external radiation exposure by a factor of about 100.
| Shield Thickness (Pb) cm | Coefficient of Attenuation
|
| 0.27 | 0.5 |
| 0.56 | 0.25 |
| 0.99 | 10-1
|
| 2.59 | 10-2
|
| 4.53 | 10-3
|
To correct for physical decay of iodine I 131, the fractions that remain at selected intervals after the time of calibration are shown in Table 7.
|
|||||
| Days
| Fraction Remaining
| Days
| Fraction Remaining
| Days
| Fraction Remaining
|
| 0*
| 1.000 | 11 | 0.388 | 22 | 0.151 |
| 1 | 0.918 | 12 | 0.356 | 23 | 0.138 |
| 2 | 0.842 | 13 | 0.327 | 24 | 0.127 |
| 3 | 0.773 | 14 | 0.300 | 25 | 0.116 |
| 4 | 0.709 | 15 | 0.275 | 26 | 0.107 |
| 5 | 0.651 | 16 | 0.253 | 27 | 0.098 |
| 6 | 0.597 | 17 | 0.232 | 28 | 0.090 |
| 7 | 0.548 | 18 | 0.213 | 29 | 0.083 |
| 8 | 0.503 | 19 | 0.195 | 30 | 0.076 |
| 9 | 0.461 | 20 | 0.179 | ||
| 10 | 0.423 | 21 | 0.164 | ||
12. Hicon Kit - Clinical Pharmacology
12.1 Mechanism of Action
Iodide is actively transported by the sodium-iodide symporter (NIS) protein, in thyroid follicular cells. Iodide is concentrated in follicular cells to levels up to 50 times higher than in the plasma. Iodide is metabolically oxidized by thyroid peroxidase to iodinium (I+) which in turn iodinates tyrosine residues of thyroglobulin (tri or tetra-iodinated tyrosine). The beta emission of I 131 is responsible for the therapeutic effect.
12.2 Pharmacodynamics
The relationship between the extent of iodide I 131 exposure and pharmacologic effects has not been explored in clinical trials.
12.3 Pharmacokinetics
Absorption
Following oral administration of HICON®, 90% of the administered radioactivity of sodium iodide I 131 is systemically absorbed in the first 60 minutes.
Distribution
Following absorption, sodium iodide I 131 is distributed within the extra-cellular space. It is actively transported by the sodium-iodide symporter (NIS) protein, and binds to thyroglobulin resulting in accumulation in the thyroid. The thyroid uptake of iodide is usually increased in hyperthyroidism and in goiter, and is decreased in hypothyroidism. Sodium iodide I 131 also accumulates in the stomach, choroid plexus, salivary glands, breast, liver, gall bladder, and kidneys.
Elimination
Metabolism
In thyroidal follicular cells iodide is oxidized through the action of thyroid peroxidase to iodinium (I+) which in turn iodinates tyrosine residues of thyroglobulin.
Excretion
Sodium iodide I 131 is excreted in urine and feces. The normal range of urinary excretion is 37% to 75% of the administered dose, varying with the thyroid and renal function of the patient. Fecal excretion is about 10%.
16. How is Hicon Kit supplied
16.1 How Supplied
HICON® provides a concentrated solution of sodium iodide I 131 with a radioconcentration of 37,000 MBq/mL (1,000 mCi/mL). It is supplied in 1 mL clear vials that contain approximately 9,250 MBq (250 mCi), 18,500 MBq (500 mCi), and 37,000 MBq (1,000 mCi) at the time of calibration.
The concentrated solution is intended for use in the preparation of capsules and solutions of varying strengths for oral administration.
| NDC
| Volume of Concentrated Solution
| Total Radioactivity per Vial
|
| 65174-880-25 | 0.25 mL | 9,250 MBq (250 mCi) |
| 65174-880-50 | 0.50 mL | 18,500 MBq (500 mCi) |
| 65174-880-00 | 1 mL | 37,000 MBq (1,000 mCi) |
A minimum of one blister package of 10 empty large hard gelatin capsules and a minimum of one blister package of 10 small hard gelatin capsules containing approximately 300 mg of dibasic sodium phosphate anhydrous as the absorbing buffer are supplied along with HICON® for the preparation of sodium iodide I 131 capsules, therapeutic.
16.2 Storage and Handling
HICON® should be stored between 2 °C and 25 °C (36 °F and 77 °F). Store and dispose of HICON® in compliance with the appropriate regulations of the government agency authorized to license the use of this radionuclide. Use HICON® solution per the expiry date on the lead pot label. Use prepared capsules within 7 days of preparing.
Discard unused capsules after all HICON® solution has been dispensed or expired. New blister packages of hard gelatin capsules are provided with each new shipment of HICON®.
This radiopharmaceutical is approved for use by persons under license by the Nuclear Regulatory Commission or the relevant regulatory authority of an Agreement State.
17. Patient Counseling Information
Radiation Safety Precautions
- Advise patients treated for hyperthyroidism to monitor for and seek medical care for signs and symptoms of
thyrotoxicosis and thyroid storm arising during the post-treatment period. For mild radiation-induced thyroiditis, patients may be advised to consider symptomatic management with pain-relievers or anti-inflammatory medications [see Warnings and Precautions (5.1)]. - Advise patients to hydrate and void frequently and to use a sialagogue after administration of radioiodide to minimize radiation dose [see Warnings and Precautions (5.2)].
- Advise patients to avoid close contact with others, especially pregnant women and children, and to take care to avoid contamination of other persons or the environment with body fluids [see Warnings and Precautions (5.7)].
Embryo-Fetal Toxicity
- Advise female patients of the risk to a fetus [see Warnings and Precautions (5.4), Use in Specific Populations (8.1)].
- Advise females and males of reproductive potential to use effective contraception during treatment with HICON® and for at least 6 months after the last dose [see Warnings and Precautions (5.4), Use in Specific Populations (8.3)].
- Advise female patients to contact their healthcare provider with a known or suspected pregnancy.
Lactation
- Instruct women to stop breastfeeding and breast-pumping for the remainder of the postpartum period after and for at least 6 weeks prior to HICON® administration [see Contraindications (4), Warnings and Precautions (5.5), Use in Specific Populations (8.2)].
Effects on Fertility
- Advise females and males of reproductive potential of the potential for impaired fertility with HICON® treatment and possible use of sperm banking for males of reproductive potential [see Warnings and Precautions (5.6), Use in Specific Populations (8.3)]
Manufactured by:

Jubilant DraxImage Inc., dba Jubilant RadiopharmaTM
16 751 TransCanada Highway
Kirkland, Quebec H9H 4J4 Canada
1-888-633-5343
www.jubilantradiopharma.com
Revised: November 2021
Art Rev.: 2.1
50000000796
HICON® is a registered trademark of Jubilant DraxImage Inc.
Jubilant RadiopharmaTM is a trademark used under license by Jubilant DraxImage Inc.
| HICON
sodium iodide i 131 solution |
||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||
| Labeler - Jubilant DraxImage Inc., dba Jubilant Radiopharma (243604761) |
| Registrant - Jubilant DraxImage Inc., dba Jubilant Radiopharma (243604761) |
| Establishment | |||
| Name | Address | ID/FEI | Business Operations |
|---|---|---|---|
| Jubilant DraxImage Inc., dba Jubilant Radiopharma | 243604761 | ANALYSIS(65174-880) , MANUFACTURE(65174-880) | |
More about Hicon (sodium iodide-i-131)
- Check interactions
- Compare alternatives
- Side effects
- Dosage information
- During pregnancy
- Generic availability
- Drug class: antithyroid agents
- Breastfeeding




