Esomeprazole Injection: Package Insert / Prescribing Info
Package insert / product label
Generic name: esomeprazole sodium
Dosage form: injection, powder, lyophilized, for solution
Drug class: Proton pump inhibitors
Medically reviewed by Drugs.com. Last updated on Oct 30, 2023.
On This Page
- Indications and Usage
- Dosage and Administration
- Dosage Forms and Strengths
- Contraindications
- Warnings and Precautions
- Adverse Reactions/Side Effects
- Drug Interactions
- Use In Specific Populations
- Overdosage
- Description
- Clinical Pharmacology
- Nonclinical Toxicology
- Clinical Studies
- How Supplied/Storage and Handling
- Patient Counseling Information
Highlights of Prescribing Information
ESOMEPRAZOLE SODIUM for Injection, for intravenous use
Initial U.S. Approval: 2005
Indications and Usage for Esomeprazole Injection
Esomeprazole sodium for injection is a proton pump inhibitor (PPI) indicated for the:
- Short-term treatment of Gastroesophageal Reflux Disease (GERD) with erosive esophagitis (EE) in adults and pediatric patients 1 month to 17 years of age, as an alternative to oral therapy when oral esomeprazole is not possible or appropriate. (1.1)
- Risk reduction of rebleeding of gastric or duodenal ulcers following therapeutic endoscopy for acute bleeding gastric or duodenal ulcers in adults. (1.2)
Esomeprazole Injection Dosage and Administration
GERD with Erosive Esophagitis(2.1):
- The recommended adult dosage is either 20 mg or 40 mg once daily by intravenous injection (no less than 3 minutes) or intravenous infusion (10 minutes to 30 minutes) for up to 10 days.
- The recommended pediatric dosage is based upon age and weight. See full prescribing information.
Risk Reduction of Rebleeding of Gastric and Duodenal Ulcers(2.2):
- The recommended adult dosage is 80 mg administered as an intravenous infusion over 30 minutes, followed by a continuous infusion of 8 mg/hour for a total treatment duration of 72 hours.
Dosage Adjustment for Hepatic Impairment(2.3):
- See full prescribing information for dosage adjustment by severity of impairment and by indication.
Preparation and Administration(2.4,2.5):
- See full prescribing information for preparation and administration instructions by indication.
Dosage Forms and Strengths
For Injection: 40 mg of esomeprazole as a lyophilized powder in a single-dose vial for reconstitution. (3)
Contraindications
Warnings and Precautions
- Gastric Malignancy:In adults, symptomatic response to therapy with esomeprazole sodium for injection does not preclude the presence of gastric malignancy. Consider additional follow-up and diagnostic testing. (5.1)
- Acute Tubulointerstitial Nephritis:Discontinue treatment and evaluate patients. (5.2)
- Clostridium difficile-Associated Diarrhea: PPI therapy may be associated with increased risk. (5.3)
- Bone Fracture:Long-term and multiple daily dose PPI therapy may be associated with an increased risk for osteoporosis-related fractures of the hip, wrist or spine. (5.4)
- Severe Cutaneous Adverse Reactions: Discontinue at the first signs or symptoms of severe cutaneous adverse reactions or other signs of hypersensitivity and consider further evaluation. (5.5)
- Cutaneous and Systemic Lupus Erythematosus:Mostly cutaneous; new onset or exacerbation of existing disease; discontinue esomeprazole sodium for injection and refer to specialist for evaluation. (5.6)
- Interaction with Clopidogrel:Avoid concomitant use of esomeprazole sodium for injection (5.7,7)
- Hypomagnesemia and Mineral Metabolism:Reported rarely with prolonged treatment with PPIs. (5.8)
- Interaction with St. John’s Wort or Rifampin:Avoid concomitant use of esomeprazole sodium for injection (5.9,7)
- Interactions with Diagnostic Investigations for Neuroendocrine Tumors:Increased chromogranin A (CgA) levels may interfere with diagnostic investigations for neuroendocrine tumors; temporarily stop esomeprazole sodium for injection at least 14 days before assessing CgA levels. (5.10,7)
- Interaction with Methotrexate:Concomitant use with PPIs may elevate and/or prolong serum concentrations of methotrexate and/or its metabolite, possibly leading to toxicity. With high dose methotrexate administration, consider a temporary withdrawal of esomeprazole sodium for injection (5.11,7)
- Fundic Gland Polyps: Risk increases with long-term use, especially beyond one year. Use the shortest duration of therapy . (5.12)
Adverse Reactions/Side Effects
Most common adverse reactions (≥1%) are: headache, flatulence, nausea, abdominal pain, injection site reaction, diarrhea, dry mouth, dizziness/vertigo, constipation and pruritus. (6.1)
To report SUSPECTED ADVERSE REACTIONS, contact Slate Run Pharmaceuticals, LLC at 1-888-341-9214 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Drug Interactions
See full prescribing information for a list of clinically important drug interactions. (7)
See 17 for PATIENT COUNSELING INFORMATION.
Revised: 10/2022
Full Prescribing Information
1. Indications and Usage for Esomeprazole Injection
1.1 Treatment of Gastroesophageal Reflux Disease (GERD) with Erosive Esophagitis (EE)
Esomeprazole sodium for injection is indicated for the short-term treatment of GERD with EE in adults and pediatric patients 1 month to 17 years, inclusively as an alternative to oral therapy when oral esomeprazole is not possible or appropriate.
1.2 Risk Reduction of Rebleeding of Gastric or Duodenal Ulcers following Therapeutic Endoscopy in Adults
Esomeprazole sodium for injection is indicated for risk reduction of rebleeding of gastric or duodenal ulcers following therapeutic endoscopy for acute bleeding gastric or duodenal ulcers in adults.
2. Esomeprazole Injection Dosage and Administration
2.1 Dosage for GERD with EE
Adult Patients
The recommended adult dosage is either 20 mg or 40 mg esomeprazole sodium for injection given once daily by intravenous injection (over at least 3 minutes) or intravenous infusion (10 minutes to 30 minutes) for up to 10 days [see Dosage and Administration (2.4)].
Pediatric Patients
The recommended dosage for pediatric patients is based on age and body weight as shown in Table 1 below. Administer as an intravenous infusion over 10 to 30 minutes once daily for up to 10 days [see Dosage and Administration (2.4)] .
|
Age and Body Weight |
Dosage Regimen |
|
|
1 month to less than 1 year of age |
0.5 mg/kg once daily |
|
|
1 year to 17 years |
less than 55 kg |
10 mg once daily |
|
55 kg or greater |
20 mg once daily |
|
Completion of Treatment
- The safety and effectiveness of esomeprazole sodium for injection for more than 10 days have not been demonstrated.
- As soon as oral therapy is possible or appropriate, discontinue intravenous therapy with esomeprazole sodium for injection and continue with oral esomeprazole therapy.
2.2 Dosage for Risk Reduction of Rebleeding of Gastric or Duodenal Ulcers following Therapeutic Endoscopy in Adults
The recommended adult dosage is 80 mg esomeprazole sodium for injection administered as an intravenous infusion over 30 minutes followed by a continuous infusion of 8 mg/hour for a total treatment duration of 72 hours (i.e., includes initial 30-minute loading dose plus 71.5 hours of continuous infusion) [see Dosage and Administration (2.5)] .
Intravenous therapy is aimed solely at the acute initial management of bleeding gastric or duodenal ulcers and does not constitute full treatment. Administer oral acid-suppressive therapy following intravenous therapy for a full course of treatment.
2.3 Dosage Adjustment for Hepatic Impairment
GERD with EE
For patients with severe hepatic impairment (Child-Pugh Class C), the maximum dosage is 20 mg once daily [see Use in Specific Populations (8.6)] .
Risk Reduction of Rebleeding of Gastric or Duodenal Ulcers following Therapeutic Endoscopy in Adults
For patients with mild to moderate hepatic impairment (Child-Pugh Classes A and B, respectively), administered 80 mg as an intravenous infusion over 30 minutes, followed by a continuous infusion of 6 mg/hour for 71.5 hours.
For patients with severe hepatic impairment (Child-Pugh Class C), administered 80 mg as an intravenous infusion over 30 minutes, followed by a continuous infusion of 4 mg/hour for 71.5 hours [see Use in Specific Populations (8.6)] .
2.4 Preparation and Administration Instructions for GERD with EE
Do not administer esomeprazole sodium for injection concomitantly with any other medications through the same intravenous site and/or tubing.
Oral antacids may be used during treatment with esomeprazole sodium for injection
Intravenous Injection Over At Least 3 Minutes in Adult Patients
- Reconstitute esomeprazole sodium for injection with 5 mL of 0.9% Sodium Chloride Injection, USP.
- Withdraw the desired dose of the reconstituted esomeprazole sodium for injection solution for a 20 mg or 40 mg dose.
- Discard any unused portion of esomeprazole sodium for injection solution remaining in the vial.
- Inspect the reconstituted esomeprazole sodium for injection solution visually for particulate matter and discoloration prior to and during administration.
- Administer as an intravenous injection over no less than 3 minutes.
- Flush the intravenous line with either 0.9% Sodium Chloride Injection, USP, Lactated Ringer’s Injection, USP or 5% Dextrose Injection, USP both prior to and after administration of esomeprazole sodium for injection
Intravenous Infusion Over 10 Minutes to 30 Minutes in Adult and Pediatric Patients
- Reconstitute the contents of one vial of esomeprazole sodium for injection with 5 mL of 0.9% Sodium Chloride Injection, USP, Lactated Ringer’s Injection, USP or 5% Dextrose Injection, USP.
- Further dilute the resulting solution with 45 mL of 0.9% Sodium Chloride Injection, USP, Lactated Ringer’s Injection, USP or 5% Dextrose Injection, USP to a final concentration of 0.8 mg/mL.
- Withdraw the desired dose of the reconstituted esomeprazole sodium for injection solution for an adult or pediatric dose.
- Discard any unused portion of esomeprazole sodium for injection solution remaining in the vial.
- Inspect the reconstituted esomeprazole sodium for injection solution visually for particulate matter and discoloration prior to and during administration.
- Administer intravenously over 10 minutes to 30 minutes.
- Flush the intravenous line with either 0.9% Sodium Chloride Injection, USP, Lactated Ringer’s Injection, USP or 5% Dextrose Injection, USP both prior to and after administration of esomeprazole sodium for injection
Storage
Store the final (diluted) esomeprazole sodium for injection solution at room temperature up to 30°C (86°F) and administer within the designated time period as listed in Table 2 below.
|
Diluent |
Administer within: |
|
0.9% Sodium Chloride Injection, USP |
12 hours |
|
Lactated Ringer’s Injection, USP |
12 hours |
|
5% Dextrose Injection, USP |
6 hours |
2.5 Preparation and Administration Instructions for Risk Reduction of Rebleeding of Gastric or Duodenal Ulcers in Adults
Do not administer esomeprazole sodium for injection concomitantly with any other medications through the same intravenous site and/or tubing.
Oral antacids may be used during treatment with esomeprazole sodium for injection.
Loading Dose (80 mg)
- Reconstitute each of two 40 mg vials of esomeprazole sodium for injection with 5 mL of 0.9% Sodium Chloride Injection, USP.
- Further dilute the resulting solution in 100 mL 0.9% Sodium Chloride Injection, USP.
- Inspect the reconstituted esomeprazole sodium for injection solution visually for particulate matter and discoloration prior to and during administration.
- Administer intravenously over 30 minutes.
- Flush the intravenous line with either 0.9% Sodium Chloride Injection, USP, Lactated Ringer’s Injection, USP or 5% Dextrose Injection, USP both prior to and after administration of esomeprazole sodium for injection
Continuous Infusion
- Reconstitute each of two 40 mg vials of esomeprazole sodium for injection with 5 mL of 0.9% Sodium Chloride Injection, USP.
- Further dilute the reconstituted esomeprazole sodium for injection solution in 100 mL 0.9% Sodium Chloride Injection, USP.
- Inspect the reconstituted esomeprazole sodium for injection solution visually for particulate matter and discoloration prior to and during administration.
- Administer intravenously as a continuous infusion at a rate of 8 mg/hour for 71.5 hours.
- Flush the intravenous line with either 0.9% Sodium Chloride Injection, USP, Lactated Ringer’s Injection, USP or 5% Dextrose Injection, USP both prior to and after administration of esomeprazole sodium for injection
Storage
- Store the final (diluted) esomeprazole sodium for injection solution at room temperature up to 30°C (86°F) and administer within 12 hours.
3. Dosage Forms and Strengths
For Injection: 40 mg of esomeprazole as a white to off-white lyophilized powder in a single-dose vial for reconstitution.
4. Contraindications
- Esomeprazole sodium for injection is contraindicated in patients with known hypersensitivity to substituted benzimidazoles or to any component of the formulation. Hypersensitivity reactions may include anaphylaxis, anaphylactic shock, angioedema, bronchospasm, acute tubulointerstitial nephritis, and urticaria [see Warnings and Precautions (5.2), Adverse Reactions (6.2)] .
- Proton pump inhibitors (PPIs), including esomeprazole sodium for injection, are contraindicated in patients receiving rilpivirine-containing products [see Drug Interactions (7)] .
5. Warnings and Precautions
5.1 Presence of Gastric Malignancy
In adults, symptomatic response to therapy with esomeprazole sodium for injection does not preclude the presence of gastric malignancy. Consider additional follow-up and diagnostic testing in adult patients who have suboptimal response or an early symptomatic relapse after completing treatment with a PPI. In older patients also consider an endoscopy.
5.2 Acute Tubulointerstitial Nephritis
Acute tubulointerstitial nephritis (TIN) has been observed in patients taking PPIs and may occur at any point during PPI therapy. Patients may present with varying signs and symptoms from symptomatic hypersensitivity reactions to non-specific symptoms of decreased renal function (e.g., malaise, nausea, anorexia). In reported case series, some patients were diagnosed on biopsy and in the absence of extra-renal manifestations (e.g., fever, rash or arthralgia). Discontinue esomeprazole sodium for injection and evaluate patients with suspected acute TIN [see Contraindications (4)] .
5.3 Clostridium difficile-Associated Diarrhea
Published observational studies suggest that PPI therapy like esomeprazole sodium for injection may be associated with an increased risk of Clostridium difficile-associated diarrhea, especially in hospitalized patients. This diagnosis should be considered for diarrhea that does not improve [see Adverse Reactions (6.2)] .
Patients should use the lowest dose and shortest duration of PPI therapy appropriate to the condition being treated.
5.4 Bone Fracture
Several published observational studies suggest that proton pump inhibitor (PPI) therapy may be associated with an increased risk for osteoporosis-related fractures of the hip, wrist, or spine. The risk of fracture was increased in patients who received high-dose, defined as multiple daily doses, and long-term PPI therapy (a year or longer). Patients should use the lowest dose and shortest duration of PPI therapy appropriate to the condition being treated. Patients at risk for osteoporosis-related fractures should be managed according to established treatment guidelines [see Dosage and Administration (2.1, 2.2), Adverse Reactions (6.2)].
5.5 Severe Cutaneous Adverse Reactions
Severe cutaneous adverse reactions, including Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN), drug reaction with eosinophilia and systemic symptoms (DRESS), and acute generalized exanthematous pustulosis (AGEP) have been reported in association with the use of PPIs [seeAdverse Reactions (6.2)] .
Discontinue esomeprazole sodium for injection at the first signs or symptoms of severe cutaneous adverse reactions or other signs of hypersensitivity and consider further evaluation.
5.6 Cutaneous and Systemic Lupus Erythematosus
Cutaneous lupus erythematosus (CLE) and systemic lupus erythematosus (SLE) have been reported in patients taking PPIs, including esomeprazole. These events have occurred as both new onset and an exacerbation of existing autoimmune disease. The majority of PPI-induced lupus erythematosus cases were CLE.
The most common form of CLE reported in patients treated with PPIs was subacute CLE (SCLE) and occurred within weeks to years after continuous drug therapy in patients ranging from infants to the elderly. Generally, histological findings were observed without organ involvement.
Systemic lupus erythematosus (SLE) is less commonly reported than CLE in patients receiving PPIs. PPI associated SLE is usually milder than non-drug induced SLE. Onset of SLE typically occurred within days to years after initiating treatment primarily in patients ranging from young adults to the elderly. The majority of patients presented with rash; however, arthralgia and cytopenia were also reported.
Avoid administration of PPIs for longer than medically indicated. If signs or symptoms consistent with CLE or SLE are noted in patients receiving esomeprazole sodium for injection, discontinue the drug and refer the patient to the appropriate specialist for evaluation. Most patients improve with discontinuation of the PPI alone in 4 to 12 weeks. Serological testing (e.g., ANA) may be positive and elevated serological test results may take longer to resolve than clinical manifestations.
5.7 Interaction with Clopidogrel
Avoid concomitant use of esomeprazole sodium for injection with clopidogrel. Clopidogrel is a prodrug. Inhibition of platelet aggregation by clopidogrel is entirely due to an active metabolite. The metabolism of clopidogrel to its active metabolite can be impaired by use with concomitant medications, such as esomeprazole, that inhibit CYP2C19 activity. Concomitant use of clopidogrel with 40 mg esomeprazole reduces the pharmacological activity of clopidogrel. When using esomeprazole sodium for injection consider alternative anti-platelet therapy [see Drug Interactions (7)].
5.8 Hypomagnesemia and Mineral Metabolism
Hypomagnesemia, symptomatic and asymptomatic, has been reported rarely in patients treated with PPIs for at least three months, in most cases after a year of therapy. Serious adverse events include tetany, arrhythmias, and seizures. Hypomagnesemia may lead to hypocalcemia and/or hypokalemia and may exacerbate underlying hypocalcemia in at-risk patients. In most patients, treatment of hypomagnesemia required magnesium replacement and discontinuation of the PPI.
For patients expected to be on prolonged treatment or who take PPIs with medications such as digoxin or drugs that may cause hypomagnesemia (e.g., diuretics), health care professionals may consider monitoring magnesium levels prior to initiation of PPI treatment and periodically [see Adverse Reactions (6.2)] .
Consider monitoring magnesium and calcium levels prior to initiation of esomeprazole sodium for injection and periodically while on treatment in patients with a preexisting risk of hypocalcemia (e.g., hypoparathyroidism). Supplement with magnesium and/or calcium, as necessary. If hypocalcemia is refractory to treatment, consider discontinuing the PPI.
5.9 Interaction with St. John’s Wort or Rifampin
Drugs which induce CYP2C19 or CYP3A4 (such as St. John’s Wort or rifampin) can substantially decrease esomeprazole concentrations [see Drug Interactions (7)] . Avoid concomitant use of esomeprazole sodium for injection with St. John’s Wort or rifampin.
5.10 Interactions with Diagnostic Investigations for Neuroendocrine Tumors
Serum chromogranin A (CgA) levels increase secondary to drug-induced decreases in gastric acidity. The increased CgA level may cause false positive results in diagnostic investigations for neuroendocrine tumors. Healthcare providers should temporarily stop esomeprazole treatment at least 14 days before assessing CgA levels and consider repeating the test if initial CgA levels are high. If serial tests are performed (e.g., for monitoring), the same commercial laboratory should be used for testing, as reference ranges between tests may vary [see Drug Interactions (7)] .
5.11 Interaction with Methotrexate
Literature suggests that concomitant use of PPIs with methotrexate (primarily at high dose; see methotrexate prescribing information) may elevate and prolong serum levels of methotrexate and/or its metabolite, possibly leading to methotrexate toxicities. In high-dose methotrexate administration, a temporary withdrawal of the PPI may be considered in some patients [see Drug Interactions (7)] .
5.12 Fundic Gland Polyps
PPI use is associated with an increased risk of fundic gland polyps that increases with long-term use, especially beyond one year. Most PPI users who developed fundic gland polyps were asymptomatic and fundic gland polyps were identified incidentally on endoscopy. Use the shortest duration of PPI therapy appropriate to the condition being treated.
6. Adverse Reactions/Side Effects
The following serious adverse reactions are described below and elsewhere in labeling:
- Acute Tubulointerstitial Nephritis [see Warnings and Precautions (5.2)]
- Clostridium difficile-Associated Diarrhea [see Warnings and Precautions (5.3)]
- Bone Fracture [see Warnings and Precautions (5.4)]
- Severe Cutaneous Adverse Reactions [see Warnings and Precautions (5.5)]
- Cutaneous and Systemic Lupus Erythematosus [see Warnings and Precautions (5.6)]
- Hypomagnesemia and Mineral Metabolism [see Warnings and Precautions (5.8)]
- Fundic Gland Polyps [see Warnings and Precautions (5.12)]
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Symptomatic GERD and EE
Adults
The safety of esomeprazole sodium for injection is based on results from clinical trials conducted in four different populations including healthy subjects (n=204) and patients with bleeding gastric or duodenal ulcers (n=375).
The data described below reflect exposure to esomeprazole sodium for injection in 359 patients in actively-controlled trials: symptomatic GERD with or without a history of EE (n=199) and patients with EE (n=160). The population was 18 to 77 years of age; 45% Male, 52% Caucasian, 17% Black, 3% Asian, and 28% other race. Most patients received doses of either 20 or 40 mg either as an infusion or an injection. Adverse reactions occurring in at least 1% of patients are listed below in Table 3:
|
|
|
Adverse Reactions |
% of patients Esomeprazole Sodium for Injection (n=359) |
|
Headache |
11 |
|
Flatulence |
10 |
|
Nausea |
6 |
|
Abdominal pain |
6 |
|
Diarrhea |
4 |
|
Mouth dry |
4 |
|
Dizziness/vertigo |
3 |
|
Constipation |
3 |
|
Injection site reaction |
2 |
|
Pruritus |
1 |
Intravenous treatment with esomeprazole sodium for injection 20 and 40 mg-administered as an injection or as an infusion was found to have a safety profile similar to that of oral esomeprazole.
Pediatrics
A randomized, open-label, multi-national study to evaluate the pharmacokinetics of repeated intravenous doses of once daily esomeprazole sodium for injection in pediatric patients 1 month to 17 years old, inclusive was performed [see Clinical Pharmacology (12.3)] . The safety results are consistent with the known safety profile of esomeprazole and no unexpected safety signals were identified.
Risk Reduction of Rebleeding of Gastric or Duodenal Ulcers in Adults
The data described in Table 4 below reflect exposure to esomeprazole sodium for injection in 375 patients who presented with endoscopically confirmed gastric or duodenal ulcer bleeding in a placebo-controlled trial. The population was 18 to 98 years old; 68% Male, 87% Caucasian, 1% Black, 7% Asian, and 4% other race. Following endoscopic hemostasis, patients received either placebo or 80 mg esomeprazole sodium for injection as an intravenous infusion over 30 minutes followed by a continuous infusion of 8 mg/hour for a total treatment duration of 72 hours. After the initial 72-hour period, all patients received an oral PPI for 27 days.
|
% of patients |
||
|
Esomeprazole Sodium for Injection (n=375) |
Placebo (n=389) |
|
|
Duodenal ulcer hemorrhage |
4 |
4 |
|
Injection site reaction † |
4 |
1 |
|
Pyrexia |
4 |
3 |
|
Cough |
1 |
0.3 |
|
Dizziness |
1 |
1 |
With the exception of injection site reactions described above, intravenous treatment with esomeprazole sodium for injection administered as an injection or as an infusion was found to have a safety profile similar to that of oral esomeprazole.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of esomeprazole. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Blood and Lymphatic System Disorders:agranulocytosis, pancytopenia;
Eye Disorders:blurred vision;
Gastrointestinal Disorders:pancreatitis; stomatitis; microscopic colitis; fundic gland polyps;
Hepatobiliary Disorders:hepatic failure, hepatitis with or without jaundice;
Immune System Disorders:anaphylactic reaction/shock; systemic lupus erythematosus;
Infections and Infestations:GI candidiasis;
Metabolism and nutritional disorders:hypomagnesemia (may lead to hypocalcemia and/or hypokalemia) [see Warnings and Precautions (5.8)] , hyponatremia;
Musculoskeletal and Connective Tissue Disorders:muscular weakness, myalgia, bone fracture;
Nervous System Disorders:hepatic encephalopathy, taste disturbance;
Psychiatric Disorders:aggression, agitation, depression, hallucination;
Renal and Urinary Disorders:interstitial nephritis;
Reproductive System and Breast Disorders:gynecomastia, erectile dysfunction;
Respiratory, Thoracic and Mediastinal Disorders:bronchospasm;
Skin and Subcutaneous Tissue Disorders:alopecia, erythema multiforme, hyperhidrosis, photosensitivity, Stevens-Johnson syndrome, toxic epidermal necrolysis (TEN, some fatal), drug reaction with eosinophilia and systemic symptoms (DRESS), and acute generalized exanthematous pustulosis (AGEP), cutaneous lupus erythematosus.
Adverse reactions associated with omeprazole may also be expected to occur with esomeprazole sodium for injection. See the full prescribing information for oral omeprazole for complete safety information.
Related/similar drugs
7. Drug Interactions
Tables 5 and 6 include drugs with clinically important drug interactions and interaction with diagnostics when administered concomitantly with esomeprazole and instructions for preventing or managing them.
Consult the labeling of concomitantly used drugs to obtain further information about interactions with PPIs.
|
Antiretrovirals |
|
|
Clinical Impact: |
The effect of PPIs on antiretroviral drugs is variable. The clinical importance and the mechanisms behind these interactions are not always known.
|
|
Intervention: |
Rilpivirine-containing products:Concomitant use with esomeprazole sodium for injection is contraindicated [see Contraindications (4)] . Atazanavir:See prescribing information for atazanavir for dosing information. Nelfinavir:Avoid concomitant use with esomeprazole sodium for injection. See prescribing information for nelfinavir. Saquinavir:See the prescribing information for saquinavir for monitoring of potential saquinavir-related toxicities. Other antiretrovirals:See prescribing information for specific antiretroviral drugs. |
|
Warfarin |
|
|
Clinical Impact: |
Increased INR and prothrombin time in patients receiving PPIs, including esomeprazole, and warfarin concomitantly. Increases in INR and prothrombin time may lead to abnormal bleeding and even death. |
|
Intervention: |
Monitor INR and prothrombin time and adjust the dose of warfarin, if needed, to maintain the target INR range. |
|
Methotrexate |
|
|
Clinical Impact: |
Concomitant use of esomeprazole with methotrexate (primarily at high dose) may elevate and prolong serum concentrations of methotrexate and/or its metabolite hydroxymethotrexate, possibly leading to methotrexate toxicities. No formal drug interaction studies of high-dose methotrexate with PPIs have been conducted [see Warnings and Precautions (5.11)]. |
|
Intervention: |
A temporary withdrawal of esomeprazole sodium for injection may be considered in some patients receiving high-dose methotrexate. |
|
2C19 Substrates (e.g., clopidogrel, citalopram, cilostazol, diazepam) |
|
|
Clopidogrel |
|
|
Clinical Impact: |
Concomitant use of esomeprazole 40 mg resulted in reduced plasma concentrations of the active metabolite of clopidogrel and a reduction in platelet inhibition [see Clinical Pharmacology (12.3)]. There are no adequate combination studies of a lower dose of esomeprazole or a higher dose of clopidogrel in comparison with the approved dose of clopidogrel . |
|
Intervention: |
Avoid concomitant use with esomeprazole sodium for injection. Consider use of alternative anti-platelet therapy [see Warnings and Precautions (5.7)]. |
|
Citalopram |
|
|
Clinical Impact: |
Increased exposure of citalopram leading to an increased risk of QT prolongation [see Clinical Pharmacology (12.3)] . |
|
Intervention: |
Limit the dose of citalopram to a maximum of 20 mg per day. See prescribing information for citalopram. |
|
Cilostazol |
|
|
Clinical Impact: |
Increased exposure of cilostazol and one of its active metabolites (3,4-dihydro-cilostazol) [see Clinical Pharmacology (12.3)]. |
|
Intervention: |
Consider reducing the dose of cilostazol to 50 mg twice daily. See prescribing information for cilostazol. |
|
Digoxin |
|
|
Clinical Impact: |
Potential for increased exposure of digoxin [see Clinical Pharmacology (12.3)]. |
|
Intervention: |
Monitor digoxin concentrations and adjust the dose, if needed, to maintain therapeutic drug concentrations. See prescribing information for digoxin. |
|
Drugs Dependent on Gastric pH for Absorption (e.g., iron salts, erlotinib, dasatinib, nilotinib, mycophenolate mofetil, ketoconazole/itraconazole) |
|
|
Clinical Impact: |
Esomeprazole can reduce the absorption of other drugs due to its effect on reducing intragastric acidity. |
|
Intervention: |
Mycophenolate mofetil (MMF): Co-administration of omeprazole, of which esomeprazole is an enantiomer, in healthy subjects and in transplant patients receiving MMF has been reported to reduce the exposure to the active metabolite, mycophenolic acid (MPA), possibly due to a decrease in MMF solubility at an increased gastric pH. The clinical relevance of reduced MPA exposure on organ rejection has not been established in transplant patients receiving esomeprazole sodium for injection and MMF. Use esomeprazole sodium for injection with caution in transplant patients receiving MMF [see Clinical Pharmacology (12.3)] . See the prescribing information for other drugs dependent on gastric pH for absorption. |
|
Tacrolimus |
|
|
Clinical Impact: |
Potentially increased exposure of tacrolimus, especially in transplant patients who are intermediate or poor metabolizers of CYP2C19 . |
|
Intervention: |
Monitor tacrolimus whole blood concentrations and consider reducing the dose, if needed, to maintain therapeutic drug concentrations. See prescribing information for tacrolimus. |
|
Interactions with Investigations of Neuroendocrine Tumors |
|
|
Clinical Impact: |
Serum chromogranin A (CgA) levels increase secondary to PPI-induced decreases in gastric acidity. The increased CgA level may cause false positive results in diagnostic investigations for neuroendocrine tumors [see Warnings and Precautions (5.10), Clinical Pharmacology (12.2)]. |
|
Intervention: |
Discontinue esomeprazole sodium for injection at least 14 days before assessing CgA levels and consider repeating the test if initial CgA levels are high. If serial tests are performed (e.g. for monitoring), the same commercial laboratory should be used for testing, as reference ranges between tests may vary. |
|
Interaction with Secretin Stimulation Test |
|
|
Clinical Impact: |
Hyper-response in gastrin secretion in response to secretin stimulation test, falsely suggesting gastrinoma. |
|
Intervention: |
Discontinue esomeprazole sodium for injection 4 weeks prior to testing [see Clinical Pharmacology (12.2)]. |
|
CYP2C19 or CYP3A4 Inducers |
|
|
Clinical Impact: |
Decreased exposure of esomeprazole when used concomitantly with strong inducers [see Clinical Pharmacology (12.3)]. |
|
Intervention: |
St. John’s Wort, rifampin:Avoid concomitant use with esomeprazole sodium for injection [see Warnings and Precautions (5.9)]. Ritonavir-containing products:see prescribing information for specific drugs. |
|
Voriconazole |
|
|
Clinical Impact: |
Increased exposure of esomeprazole [see Clinical Pharmacology (12.3)]. |
|
Intervention: |
Dose adjustment of esomeprazole sodium for injection is not normally required. See prescribing information for voriconazole. |
8. Use In Specific Populations
8.1 Pregnancy
Risk Summary
There are no adequate and well-controlled studies with esomeprazole in pregnant women. Esomeprazole is the s-isomer of omeprazole. Available epidemiologic data fail to demonstrate an increased risk of major congenital malformations or other adverse pregnancy outcomes with first trimester omeprazole use. Reproduction studies in rats and rabbits resulted in dose-dependent embryo-lethality at omeprazole doses that were approximately 3.4 to 34 times an oral human dose of 40 mg (based on a body surface area for a 60 kg person).
Teratogenicity was not observed in animal reproduction studies with administration of oral esomeprazole magnesium in rats and rabbits with doses about 68 times and 42 times, respectively, an oral human dose of 40 mg (based on a body surface area basis for a 60 kg person). Changes in bone morphology were observed in offspring of rats dosed through most of pregnancy and lactation at doses equal to or greater than approximately 34 times an oral human dose of 40 mg. When maternal administration was confined to gestation only, there were no effects on bone physeal morphology in the offspring at any age ( see Data).
The estimated background risks of major birth defects and miscarriage for the indicated population are unknown. All pregnancies have a background risk of birth defect, loss or other adverse outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2% to 4% and 15% to 20%, respectively.
Data
Human Data
Esomeprazole is the S-isomer of omeprazole. Four epidemiological studies compared the frequency of congenital abnormalities among infants born to women who used omeprazole during pregnancy with the frequency of abnormalities among infants of women exposed to H 2-receptor antagonists or other controls.
A population based retrospective cohort epidemiological study from the Swedish Medical Birth Registry, covering approximately 99% of pregnancies, from 1995 to 99, reported on 955 infants (824 exposed during the first trimester with 39 of these exposed beyond first trimester, and 131 exposed after the first trimester) whose mothers used omeprazole during pregnancy. The number of infants exposed in utero to omeprazole that had any malformation, low birth weight, low Apgar score, or hospitalization was similar to the number observed in this population. The number of infants born with ventricular septal defects and the number of stillborn infants was slightly higher in the omeprazole-exposed infants than the expected number in this population.
A population-based retrospective cohort study covering all live births in Denmark from 1996 to 2009, reported on 1,800 live births whose mothers used omeprazole during the first trimester of pregnancy and 837,317 live births whose mothers did not use any proton pump inhibitor. The overall rate of birth defects in infants born to mothers with first trimester exposure to omeprazole was 2.9% and 2.6% in infants born to mothers not exposed to any proton pump inhibitor during the first trimester.
A retrospective cohort study reported on 689 pregnant women exposed to either H 2-blockers or omeprazole in the first trimester (134 exposed to omeprazole) and 1,572 pregnant women unexposed to either during the first trimester. The overall malformation rate in offspring born to mothers with first trimester exposure to omeprazole, an H 2-blocker, or were unexposed was 3.6%, 5.5%, and 4.1% respectively.
A small prospective observational cohort study followed 113 women exposed to omeprazole during pregnancy (89% with first trimester exposures). The reported rate of major congenital malformations was 4% in the omeprazole group, 2% in controls exposed to non-teratogens, and 2.8% in disease paired controls. Rates of spontaneous and elective abortions, preterm deliveries, gestational age at delivery, and mean birth weight were similar among the groups.
Several studies have reported no apparent adverse short-term effects on the infant when single dose oral or intravenous omeprazole was administered to over 200 pregnant women as premedication for cesarean section under general anesthesia.
Animal Data
Omeprazole
Reproductive studies conducted with omeprazole in rats at oral doses up to 138 mg/kg/day (about 34 times an oral human dose of 40 mg on a body surface area basis) and in rabbits at doses up to 69.1 mg/kg/day (about 34 times an oral human dose of 40 mg on a body surface area basis) during organogenesis did not disclose any evidence for a teratogenic potential of omeprazole. In rabbits, omeprazole in a dose range of 6.9 to 69.1 mg/kg/day (about 3.4 to 34 times an oral human dose of 40 mg on a body surface area basis) administered during organogenesis produced dose-related increases in embryo-lethality, fetal resorptions, and pregnancy disruptions. In rats, dose-related embryo/fetal toxicity and postnatal developmental toxicity were observed in offspring resulting from parents treated with omeprazole at 13.8 to 138.0 mg/kg/day (about 3.4 to 34 times an oral human dose of 40 mg on a body surface area basis), administered prior to mating through the lactation period.
Esomeprazole
No effects on embryo-fetal development were observed in reproduction studies with esomeprazole magnesium in rats at oral doses up to 280 mg/kg/day (about 68 times an oral human dose of 40 mg on a body surface area basis) or in rabbits at oral doses up to 86 mg/kg/day (about 41 times the human dose on a body surface area basis) administered during organogenesis.
A pre- and postnatal developmental toxicity study in rats with additional endpoints to evaluate bone development was performed with esomeprazole magnesium at oral doses of 14 to 280 mg/kg/day (about 3.4 to 68 times an oral human dose of 40 mg on a body surface area basis). Neonatal/early postnatal (birth to weaning) survival was decreased at doses equal to or greater than 138 mg/kg/day (about 34 times an oral human dose of 40 mg on a body surface area basis). Body weight and body weight gain were reduced and neurobehavioral or general developmental delays in the immediate post-weaning timeframe were evident at doses equal to or greater than 69 mg/kg/day (about 17 times an oral human dose of 40 mg on a body surface area basis). In addition, decreased femur length, width and thickness of cortical bone, decreased thickness of the tibial growth plate and minimal to mild bone marrow hypocellularity were noted at doses equal to or greater than 14 mg/kg/day (about 3.4 times an oral human dose of 40 mg on a body surface area basis). Physeal dysplasia in the femur was observed in offspring of rats treated with oral doses of esomeprazole magnesium at doses equal to or greater than 138 mg/kg/day (about 34 times an oral human dose of 40 mg on a body surface area basis).
Effects on maternal bone were observed in pregnant and lactating rats in a pre- and postnatal toxicity study when esomeprazole magnesium was administered at oral doses of 14 to 280 mg/kg/day (about 3.4 to 68 times an oral human dose of 40 mg on a body surface area basis). When rats were dosed from gestational day 7 through weaning on postnatal day 21, a statistically significant decrease in maternal femur weight of up to 14% (as compared to placebo treatment) was observed at doses equal to or greater than 138 mg/kg/day (about 34 times an oral human dose of 40 mg on a body surface area basis).
A pre- and postnatal development study in rats with esomeprazole strontium (using equimolar doses compared to esomeprazole magnesium study) produced similar results in dams and pups as described above.
A follow up developmental toxicity study in rats with further time points to evaluate pup bone development from postnatal day 2 to adulthood was performed with esomeprazole magnesium at oral doses of 280 mg/kg/day (about 68 times an oral human dose of 40 mg on a body surface area basis) where esomeprazole administration was from either gestational day 7 or gestational day 16 until parturition. When maternal administration was confined to gestation only, there were no effects on bone physeal morphology in the offspring at any age.
8.2 Lactation
Risk Summary
Esomeprazole is the S-isomer of omeprazole and limited data suggest that omeprazole may be present in human milk. There are no clinical data on the effects of esomeprazole on the breastfed infant or on milk production. The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for esomeprazole and any potential adverse effects on the breastfed infant from esomeprazole or from the underlying maternal condition.
8.4 Pediatric Use
The safety and effectiveness of esomeprazole sodium for injection have been established in pediatric patients 1 month to 17 years of age for the short-term treatment of GERD with EE, as an alternative to oral therapy when oral esomeprazole is not possible or appropriate.
Use of esomeprazole sodium for injection in this age group is based on extrapolation of adult efficacy to children and the selection of dose based on exposure-matching of pediatrics to adults supported by the following evidence: a) results observed from a pharmacokinetic (PK) study on esomeprazole sodium for injection in pediatric patients, b) predictions from a population PK model comparing I.V. PK data between adult and pediatric patients, and c) relationship between exposure and pharmacodynamic results obtained from adult I.V. and pediatric oral data and d) PK results from adequate and well-controlled studies that supported the approval of esomeprazole sodium for injection in adults [see Adverse Reactions (6.1), Clinical Pharmacology (12.3), Clinical Studies (14.1)] .
The safety and effectiveness of esomeprazole sodium for injection have not been established in patients less than 1 month of age for the treatment of GERD with EE or for risk reduction of rebleeding of gastric or duodenal ulcer following therapeutic endoscopy.
Juvenile Animal Data
In a juvenile rat toxicity study, esomeprazole was administered with both magnesium and strontium salts at oral doses about 34 to 68 times a daily human dose of 40 mg based on body surface area. Increases in death were seen at the high dose, and at all doses of esomeprazole, there were decreases in body weight, body weight gain, femur weight and femur length, and decreases in overall growth [see Nonclinical Toxicology (13.2)] .
8.5 Geriatric Use
In a clinical trial of patients with bleeding gastric or duodenal ulcers, 52% of 375 patients randomized to esomeprazole sodium for injection were 65 years of age and over. No overall differences in safety and efficacy were observed between the elderly and younger individuals, and other reported clinical experience with esomeprazole sodium for injection and oral esomeprazole has not identified differences in responses between the elderly and younger patients, but greater sensitivity of some older individuals cannot be ruled out.
8.6 Hepatic Impairment
GERD with EE
Exposure to esomeprazole was increased substantially in patients with severe hepatic impairment (Child-Pugh Class C) but not in patients with mild to moderate hepatic impairment (Child-Pugh Classes A and B) compared to patients with normal liver function [see Clinical Pharmacology (12.3)] .
For adult patients, no dosage adjustment is necessary for mild to moderate hepatic impairment. For patients with severe hepatic impairment the maximum recommended dosage is 20 mg once daily [see Dosage and Administration (2.3)] .
Risk Reduction of Rebleeding of Gastric or Duodenal Ulcers following Therapeutic Endoscopy
There are no pharmacokinetic data available for esomeprazole sodium for injection administered as continuous intravenous administration in patients with hepatic impairment. Exposure to intravenous omeprazole, of which esomeprazole is an enantiomer, increased in patients with all degrees of hepatic impairment compared to subjects with normal liver function [see Clinical Pharmacology (12.3)] .
For adult patients, no dosage adjustment of the initial esomeprazole sodium for injection 80 mg loading dose is necessary for patients with any degree of hepatic impairment. Reduce the rate of the continuous infusion to 6 mg/hour for patients with mild to moderate liver impairment (Child-Pugh Classes A and B) and to 4 mg/hour for patients with severe hepatic impairment (Child-Pugh Class C) [see Dosage and Administration (2.3)] .
10. Overdosage
The symptoms described in connection with deliberate esomeprazole overdose (limited experience of doses in excess of 240 mg/day) are transient. Reports of overdosage with omeprazole in humans may also be relevant. Doses ranged up to 2,400 mg (120 times the usual recommended clinical dose). Manifestations were variable, but included confusion, drowsiness, blurred vision, tachycardia, nausea, diaphoresis, flushing, headache, dry mouth, and other adverse reactions similar to those seen at recommended dosages. See the full prescribing information for oral omeprazole for complete safety information. No specific antidote for esomeprazole is known. Since esomeprazole is extensively protein bound, it is not expected to be removed by dialysis. In the event of overdosage, treatment should be symptomatic and supportive.
If over-exposure occurs, call your Poison Control Center at 1-800-222-1222 for current information on the management of poisoning or overdosage.
11. Esomeprazole Injection Description
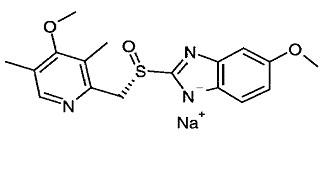
The active ingredient in esomeprazole sodium for injection is ( S)-5-methoxy-2[[(4-methoxy-3,5- dimethyl-2-pyridinyl)-methyl]sulfinyl]-1 H-benzimidazole sodium, a PPI. Esomeprazole is the S-isomer of omeprazole, which is a mixture of the S- and R- isomers. Its empirical formula is C 17H 18N 3O 3SNa with molecular weight of 367.4 g/mol (sodium salt) and 345.4 g/mol (parent compound). Esomeprazole sodium is very soluble in water and freely soluble in ethanol (95%). The structural formula is:
Esomeprazole sodium for injection is supplied as a sterile, lyophilized, white to off-white, porous cake or powder in a 5 mL single-dose vial, intended for intravenous administration after reconstitution with 0.9% Sodium Chloride Injection, USP; Lactated Ringer’s Injection, USP or 5% Dextrose Injection, USP. Esomeprazole sodium for injection contains 40 mg esomeprazole (equivalent to 42.5 mg esomeprazole sodium), edetate disodium 1.5 mg and sodium hydroxide q.s. for pH adjustment. The pH of reconstituted solution of esomeprazole sodium for injection depends on the reconstitution volume and is in the pH range of 9 to 11. The stability of esomeprazole sodium in aqueous solution is strongly pH dependent. The rate of degradation increases with decreasing pH.
12. Esomeprazole Injection - Clinical Pharmacology
12.1 Mechanism of Action
Esomeprazole belongs to a class of antisecretory compounds, the substituted benzimidazoles, that suppress gastric acid secretion by specific inhibition of the H+/K+ ATPase enzyme system at the secretory surface of the gastric parietal cell. Esomeprazole is protonated and converted in the acidic compartment of the parietal cell forming the active inhibitor, the achiral sulphenamide. Because this enzyme system is regarded as the acid (proton) pump within the gastric mucosa, esomeprazole has been characterized as a gastric acid-pump inhibitor, in that it blocks the final step of acid production. This effect is dose-related and leads to inhibition of both basal and stimulated acid secretion irrespective of the stimulus.
12.2 Pharmacodynamics
Antisecretory Activity
The effect of esomeprazole on 24-hour intragastric pH in healthy subjects was evaluated in two studies of 20 mg and 40 mg esomeprazole sodium for injection infused intravenously once daily over 30 minutes for 5 days, as shown in Table 7.
|
Esomeprazole Sodium for Injection 20 mg once daily (n=22) |
Esomeprazole Sodium for Injection 40 mg once daily (n=38) |
|
|
% Time Gastric pH>4 (95% CI) |
49.5 41.9-57.2 |
66.2 62.4-70.0 |
Gastric pH was measured over a 24-hour period
The effects of esomeprazole on 24-hour intragastric pH following administration of an intravenous infusion of 80 mg esomeprazole sodium for injection over 30 minutes followed by a continuous infusion of 8 mg/hour for 23.5 hours was evaluated in two studies.
In H. pylori-negative healthy Caucasian subjects (n=24), the % time over 24 hours (95% CI) when the intragastric pH was > 6 and > 7 was 52.3% (40.3, 64.4) and 4.8% (1.8, 7.8), respectively.
In H. pylori-positive (n=8) and H. pylori-negative (n=11) healthy Chinese subjects, the % time over 24 hours (95% CI) when intragastric pH was > 6 and > 7 was 53% (45.6, 60.3) and 15.1% (9.5, 20.7). The percentage of time with intragastric pH > 6 [59% vs. 47%] and with pH > 7 [17% vs. 11%] tended to be larger in the H. pyloripositive subjects compared to H. pylori-negative subjects.
Serum Gastrin Effects
The effect of esomeprazole on serum gastrin concentrations was evaluated in approximately 2,700 patients in clinical trials of oral esomeprazole for up to 8 weeks and in over 1,300 patients treated for up to 12 months. The mean fasting gastrin level increased in a dose-related manner. The increase in serum gastrin concentrations reached a plateau within two to three months of therapy and returned to baseline levels within four weeks after discontinuation of therapy.
Increased gastrin causes enterochromaffin-like cell hyperplasia and increased serum Chromogranin A (CgA) levels. The increased CgA levels may cause false positive results in diagnostic investigations for neuroendocrine tumors [see Warnings and Precautions (5.9)].
Enterochromaffin-like (ECL) Cell Effects
There are no data available on the effects of intravenous esomeprazole on ECL cells.
Human gastric biopsy specimens have been obtained from more than 3,000 patients (both children and adults) treated orally with omeprazole in long-term clinical trials. The incidence of ECL cell hyperplasia in these studies increased with time; however, no case of ECL cell carcinoids, dysplasia, or neoplasia has been found in these patients [see Nonclinical Toxicology (13.1)] .
In over 1,000 patients treated with oral esomeprazole (10 mg, 20 mg or 40 mg/day) for up to 12 months, the prevalence of ECL cell hyperplasia increased with time and dose. No patient developed ECL cell carcinoids, dysplasia, or neoplasia in the gastric mucosa.
Endocrine Effects
Esomeprazole had no effect on thyroid function when given in oral doses of 20 mg or 40 mg for 4 weeks. Other effects of esomeprazole on the endocrine system were assessed in studies of omeprazole. Oral doses of omeprazole 30 mg or 40 mg per day for 2 to 4 weeks had no effect on carbohydrate metabolism, circulating levels of parathyroid hormone, cortisol, estradiol, testosterone, prolactin, cholecystokinin or secretin.
12.3 Pharmacokinetics
Absorption
The pharmacokinetics of esomeprazole in healthy subjects following administration of esomeprazole sodium for injection 20 mg and 40 mg once daily as intravenous infusion over 30 minutes for 5 days are shown in Table 8.
|
Parameter |
Esomeprazole Sodium for Injection 20 mg (n=24) |
Esomeprazole Sodium for Injection 40 mg (n=38) |
|
AUC (micromol*h/L) |
5.1 (4.0:6:6) |
16.2 (14.5:18.2) |
|
C max(micromol/L) |
3.9 (3.2:4.7) |
7.5 (6.9:8.1) |
|
t ½(h) |
1.1 (0.9:1.2) |
1.4 (1.3:1.5) |
Following intravenous administration of esomeprazole sodium for injection in 24 healthy subjects as a loading dose of 80 mg over 30 minutes followed by a continuous infusion of 8 mg/hour for 23.5 hours (for a total of 24 hours), esomeprazole pharmacokinetic parameters [geometric mean value (95% CI)] were as follows: AUC t111.1 micromol*h/L (100.5, 122.7 micromol*h/L), C max15.0 micromol/L (13.5, 16.6 micromol/L), and steady state plasma concentration (C ss) 3.9 micromol/L (3.5, 4.5 micromol/L). In another study of healthy Caucasian subjects administered the same treatment regimen.
Esomeprazole is a time-dependent inhibitor of CYP2C19, resulting in autoinhibition and nonlinear pharmacokinetics. The systemic exposure increases in a more than dose proportional manner after multiple oral doses of esomeprazole. Compared to the first dose, the systemic exposure (C maxand AUC 0-24h) at steady state following once a day dosing increased by 43% and 90%, respectively, compared to after the first dose for the 20 mg dose and increased by 95% and 159%, respectively, for the 40 mg dose.
Distribution
Esomeprazole is 97% bound to plasma proteins. Plasma protein binding is constant over the concentration range of 2 to 20 micromol/L. The apparent volume of distribution at steady state in healthy subjects is approximately 16 L.
Elimination
Metabolism
Esomeprazole is extensively metabolized in the liver by the cytochrome P450 (CYP) enzyme system. The metabolites of esomeprazole lack antisecretory activity. The major part of esomeprazole’s metabolism is dependent upon the CYP2C19 isoenzyme, which forms the hydroxy and desmethyl metabolites. The remaining amount is dependent on CYP3A4 which forms the sulphone metabolite.
Excretion
Esomeprazole is excreted as metabolites primarily in urine but also in feces. Less than 1% of parent drug is excreted in the urine. Esomeprazole is completely eliminated from plasma, and there is no accumulation during once daily administration. The plasma elimination half-life of esomeprazole following intravenous administration of esomeprazole sodium for injection is approximately 1.1 to 1.4 hours and is prolonged with increasing doses.
The plasma clearance (CL) is approximately 5.9 to 7.2 L/h during administration of esomeprazole sodium for injection as an intravenous infusion of 80 mg over 30 minutes followed by a continuous infusion of 8 mg/hour for 23.5 hours.
Specific Populations
Geriatric Patients
The AUC and C maxvalues of esomeprazole were slightly higher (25% and 18%, respectively) in the elderly as compared to younger subjects at steady state. This increase in exposure is not considered clinically relevant.
Pediatric Patients
The pharmacokinetics of esomeprazole were evaluated in 50 pediatric patients birth to 17 years of age, inclusive (of which 44 pediatric patients were 1 month to 17 years) in a randomized, open-label, multi-national, multiple dose study of 20 mg esomeprazole sodium for injection administered as a once-daily 3-minute intravenous injection. Esomeprazole plasma AUC values were 183% and 60% higher in pediatric patients aged 6 to 11 years and 12 to 17 years, respectively, compared to adults.
Subsequent pharmacokinetic analyses predicted the following dosage regimens would achieve comparable steady-state plasma exposures (AUC 0-24) to those observed in adult patients administered 20 mg of esomeprazole sodium for injection once daily: 0.5 mg/kg once daily for pediatric patients 1 month to 11 months of age, 10 mg once daily for pediatric patients 1 year to 17 years with body weight less than 55 kg, and 20 mg once daily for pediatric patients 1 year to 17 years with body weight of 55 kg and greater. Increasing the infusion duration from 3 minutes to 10 minutes or 30 minutes was predicted to produce steady-state C maxvalues that were comparable to those observed in adult patients at the 40 mg and 20 mg esomeprazole sodium for injection doses, respectively [see Use in Specific Populations (8.4)] .
Male and Female Patients
The AUC and C maxvalues of esomeprazole were slightly higher (13%) in females than in males at steady state when dosed orally. Similar differences have been seen for intravenous administration of esomeprazole. This increase in exposure is not considered clinically relevant.
Patients with Renal Impairment
The pharmacokinetics of esomeprazole in patients with renal impairment are not expected to be altered relative to healthy subjects as less than 1% of esomeprazole is excreted unchanged in urine.
Patients with Hepatic Impairment
The steady state pharmacokinetics of esomeprazole obtained after administration of 40 mg orally once daily to 4 patients each with mild (Child-Pugh Class A), moderate (Child-Pugh Class B), and severe (Child-Pugh Class C) hepatic impairment were compared to those obtained in 36 male and female GERD patients with normal liver function. In patients with mild and moderate hepatic impairment, the AUCs were within the range that could be expected in patients with normal liver function. In patients with severe hepatic impairment, the AUCs were 2 to 3 times higher than in the patients with normal liver function. [see Use in Specific Populations (8.6)] .
There are no pharmacokinetic data available for esomeprazole administered as continuous intravenous administration in patients with liver impairment. The pharmacokinetics of intravenous omeprazole 80 mg infused over 30 minutes, followed by 8 mg/hour over 47.5 hours in patients with mild (Child-Pugh Class A; n=5), moderate (Child-Pugh Class B; n=4) and severe (Child-Pugh Class C; n=3) liver impairment were compared to those obtained in 24 male and female healthy subjects. In patients with mild and moderate liver impairment, omeprazole clearance and steady state plasma concentration was approximately 35% lower and 50% higher, respectively, than in healthy subjects. In patients with severe liver impairment, the omeprazole clearance was 50% of that in healthy subjects and the steady state plasma concentration was double that in healthy subjects [see Use in Specific Populations (8.6)] .
Drug Interaction Studies
Effect of Esomeprazole/Omeprazole on Other Drugs
In vitroand in vivostudies have shown that esomeprazole is not likely to inhibit CYPs 1A2, 2A6, 2C9, 2D6, 2E1 and 3A4.
Antiretrovirals
For some antiretroviral drugs, such as rilpivirine, atazanavir and nelfinavir, decreased serum concentrations have been reported when given together with omeprazole [see Drug Interactions (7)] .
Rilpivirine:
Following multiple doses of rilpivirine (150 mg, daily) and omeprazole (20 mg, daily), AUC was decreased by 40%, C maxby 40%, and C minby 33% for rilpivirine [see Contraindications (4)] .
Nelfinavir:
Following multiple doses of nelfinavir (1250 mg, twice daily) and omeprazole (40 mg daily), AUC was decreased by 36% and 92%, C maxby 37% and 89% and C minby 39% and 75% respectively for nelfinavir and M8.
Atazanavir:
Following multiple doses of atazanavir (400 mg, daily) and omeprazole (40 mg, daily, 2 hours before atazanavir), AUC was decreased by 94%, C maxby 96%, and C minby 95%.
Saquinavir:
Following multiple dosing of saquinavir/ritonavir (1000/100 mg) twice daily for 15 days with omeprazole 40 mg daily co-administered days 11 to 15. The AUC was increased by 82%, C maxby 75%, and C minby 106%. The mechanism behind this interaction is not fully elucidated.
Clopidogrel
In a crossover study, healthy subjects were administered clopidogrel (300 mg loading dose followed by 75 mg per day as the maintenance dosage for 28 days) alone and with esomeprazole (40 mg orally once daily at the same time as clopidogrel) for 29 days. Exposure to the active metabolite of clopidogrel was reduced by 35% to 40% over this time period when clopidogrel and esomeprazole were administered together. Pharmacodynamic parameters were also measured and demonstrated that the change in inhibition of platelet aggregation was related to the change in the exposure to clopidogrel active metabolite [see Warnings and Precautions (5.7), Drug Interactions (7)] .
Mycophenolate Mofetil
Administration of omeprazole 20 mg twice daily for 4 days and a single 1000 mg dose of MMF approximately one hour after the last dose of omeprazole to 12 healthy subjects in a cross-over study resulted in a 52% reduction in the C maxand 23% reduction in the AUC of MPA [see Drug Interactions (7)] .
Cilostazol
Omeprazole acts as an inhibitor of CYP2C19. Omeprazole, given in doses of 40 mg daily for one week to 20 healthy subjects in cross-over study, increased C maxand AUC of cilostazol by 18% and 26% respectively. The C maxand AUC of one of the active metabolites, 3,4-dihydro-cilostazol, which has 4-7 times the activity of cilostazol, were increased by 29% and 69%, respectively. Co-administration of cilostazol with omeprazole is expected to increase concentrations of cilostazol and the above mentioned active metabolite [see Drug Interactions (7)] .
Diazepam
Co-administration of esomeprazole 30 mg and diazepam, a CYP2C19 substrate, resulted in a 45% decrease in clearance of diazepam. Increased plasma levels of diazepam were observed 12 hours after dosing and onwards. However, at that time, the plasma levels of diazepam were below the therapeutic interval, and thus this interaction is unlikely to be of clinical relevance.
Digoxin
Concomitant administration of omeprazole 20 mg once daily and digoxin in healthy subjects increased the bioavailability of digoxin by 10% (30% in two subjects) [see Drug Interactions (7)] .
Other Drugs
Concomitant administration of esomeprazole and either naproxen (non-selective NSAID) did not identify any clinically relevant changes in the pharmacokinetic profiles of these NSAIDs.
Effect of Other Drugs on Esomeprazole/Omeprazole
St. John’s Wort
In a cross-over study in 12 healthy male subjects, St. John’s Wort (300 mg three times daily for 14 days) significantly decreased the systemic exposure of omeprazole in CYP2C19 poor metabolizers (C maxand AUC decreased by 37.5% and 37.9%, respectively) and extensive metabolizers (C maxand AUC decreased by 49.6% and 43.9%, respectively) [see Drug Interactions (7)] .
Voriconazole
Concomitant administration of omeprazole and voriconazole (a combined inhibitor of CYP2C19 and CYP3A4) resulted in more than doubling of the omeprazole exposure. When voriconazole (400 mg every 12 hours for one day, followed by 200 mg once daily for 6 days) was given with omeprazole (40 mg once daily for 7 days) to healthy subjects, the steady-state C maxand AUC 0-24of omeprazole significantly increased: an average of 2 times (90% CI: 1.8, 2.6) and 4 times (90% CI: 3.3, 4.4), respectively, as compared to when omeprazole was given without voriconazole [see Drug Interactions (7)] .
Other Drugs
Co-administration of esomeprazole with oral contraceptives, diazepam, phenytoin, quinidine, naproxen (non-selective NSAID) did not seem to change the pharmacokinetic profile of esomeprazole.
12.4 Microbiology
Effects on Gastrointestinal Microbial Ecology
Decreased gastric acidity due to any means including proton pump inhibitors, increases gastric counts of bacteria normally present in the gastrointestinal tract. Treatment with proton pump inhibitors may lead to slightly increased risk of gastrointestinal infections such as Salmonellaand Campylobacterand, in hospitalized patients, possibly also Clostridium difficile.
12.5 Pharmacogenomics
CYP2C19, a polymorphic enzyme, is involved in the metabolism of esomeprazole. The CYP2C19*1 allele is fully functional while the CYP2C19*2 and *3 alleles are nonfunctional. There are other alleles associated with no or reduced enzymatic function. Patients carrying two fully functional alleles are extensive metabolizers and those carrying two loss-of-function alleles are poor metabolizers. The systemic exposure to esomeprazole varies with a patient’s metabolism status: poor metabolizers > intermediate metabolizers > extensive metabolizers. Approximately 3% of Caucasians and 15 to 20% of Asians are CYP2C19 poor metabolizers.
Systemic esomeprazole exposures were modestly higher (approximately 17%) in CYP2C19 intermediate metabolizers (IM; n=6) compared to extensive metabolizers (EM; n=17) of CYP2C19. Similar pharmacokinetic differences were noted across these genotypes in a study of Chinese healthy subjects that included 7 EMs and 11 IMs. There is very limited pharmacokinetic information for poor metabolizers (PM) from these studies.
At steady state following once daily administration of esomeprazole sodium for injection 40 mg, the ratio of AUC in Poor Metabolizers to AUC in the rest of the population (EMs) is approximately 1.5. This change in exposure is not considered clinically meaningful.
13. Nonclinical Toxicology
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
The carcinogenic potential of esomeprazole was assessed using omeprazole studies. In two 24-month oral carcinogenicity studies in rats, omeprazole at daily doses of 1.7, 3.4, 13.8, 44.0, and 140.8 mg/kg/day (about 0.4 to 34 times the human dose of 40 mg/day expressed on a body surface area basis) produced gastric ECL cell carcinoids in a dose-related manner in both male and female rats; the incidence of this effect was markedly higher in female rats, which had higher blood levels of omeprazole. Gastric carcinoids seldom occur in the untreated rat. In addition, ECL cell hyperplasia was present in all treated groups of both sexes. In one of these studies, female rats were treated with 13.8 mg omeprazole/kg/day (about 3.4 times the human dose of 40 mg/day on a body surface area basis) for 1 year, then followed for an additional year without the drug. No carcinoids were seen in these rats. An increased incidence of treatment-related ECL cell hyperplasia was observed at the end of 1 year (94% treated vs 10% controls). By the second year the difference between treated and control rats was much smaller (46% vs 26%) but still showed more hyperplasia in the treated group. Gastric adenocarcinoma was seen in one rat (2%). No similar tumor was seen in male or female rats treated for 2 years. For this strain of rat no similar tumor has been noted historically, but a finding involving only one tumor is difficult to interpret. A 78-week oral mouse carcinogenicity study of omeprazole did not show increased tumor occurrence, but the study was not conclusive.
Esomeprazole was negative in the Ames mutation test, in the in vivorat bone marrow cell chromosome aberration test, and the in vivomouse micronucleus test. Esomeprazole, however, was positive in the in vitrohuman lymphocyte chromosome aberration test. Omeprazole was positive in the in vitrohuman lymphocyte chromosome aberration test, the in vivomouse bone marrow cell chromosome aberration test, and the in vivomouse micronucleus test.
The potential effects of esomeprazole on fertility and reproductive performance were assessed using omeprazole studies. Omeprazole at oral doses up to 138 mg/kg/day in rats (about 34 times the human dose of 40 mg/day on a body surface area basis) was found to have no effect on reproductive performance of parental animals.
13.2 Animal Toxicology and/or Pharmacology
Reproduction Studies
Reproduction studies have been performed in rats at oral doses up to 280 mg/kg/day (about 68 times an oral human dose of 40 mg on a body surface area basis) and in rabbits at oral doses up to 86 mg/kg/day (about 42 times an oral human dose of 40 mg on a body surface area basis) and have revealed no evidence of impaired fertility or harm to the fetus due to esomeprazole [see Use in Specific Populations (8.1)] .
Juvenile Animal Study
A 28-day toxicity study with a 14-day recovery phase was conducted in juvenile rats with esomeprazole magnesium at doses of 70 to 280 mg/kg/day (about 17 to 68 times a daily oral human dose of 40 mg on a body surface area basis). An increase in the number of deaths at the high dose of 280 mg/kg/day was observed when juvenile rats were administered esomeprazole magnesium from postnatal day 7 through postnatal day 35. In addition, doses equal to or greater than 140 mg/kg/day (about 34 times a daily oral human dose of 40 mg on a body surface area basis), produced treatment-related decreases in body weight (approximately 14%) and body weight gain, decreases in femur weight and femur length, and affected overall growth. Comparable findings described above have also been observed in this study with another esomeprazole salt, esomeprazole strontium, at equimolar doses of esomeprazole.
14. Clinical Studies
14.1 Acid Suppression in GERD
Four multicenter, open-label, two-period crossover studies were conducted to compare the pharmacodynamic effects of esomeprazole following intravenous or oral administration on acid suppression in 206 patients with symptoms of GERD with or without erosive esophagitis. Patients were randomized to receive either 20 or 40 mg of esomeprazole sodium for injection or oral esomeprazole once daily for 10 days (Period 1), and then were switched in Period 2 to the other formulation for 10 days, matching their respective dose from Period 1. Esomeprazole sodium for injection 20 mg and 40 mg was administered as a 3-minute injection in two of the studies and as a 15-minute infusion in the other two studies.
The patient population ranged from 18 to 72 years old; 54% were female; 53% Caucasian, 24% Black, 5% Asian, and 17% other race. Basal acid output (BAO) and maximal acid output (MAO) were determined 22 to 24 hours post-dose on Period 1, Day 11; on Period 2, Day 3; and on Period 2, Day 11. BAO and MAO were estimated from 1-hour continuous collections of gastric contents prior to and following (respectively) subcutaneous injection of 6.0 mcg/kg of pentagastrin.
In these studies, after 10 days of once daily administration, esomeprazole sodium for injection 20 mg and 40 mg were similar to the corresponding oral dosage of esomeprazole in their ability to suppress BAO and MAO in these GERD patients (see Table 9 below).
There were no major changes in acid suppression when switching between intravenous and oral dosage forms.
|
Study |
Dose in mg |
Intravenous Administration Method |
BAO in mmol H+/h |
MAO in mmol H+/h |
||
|
Intravenous |
Oral |
Intravenous |
Oral |
|||
|
1 (N=42) |
20 |
3-minute injection |
0.71 (1.24) |
0.69 (1.24) |
5.96 (5.41) |
5.27 (5.39) |
|
2 (N=44) |
20 |
15-minute infusion |
0.78 (1.38) |
0.82 (1.34) |
5.95 (4.00) |
5.26 (4.12) |
|
3 (N=50) |
40 |
3-minute injection |
0.36 (0.61) |
0.31 (0.55) |
5.06 (3.90) |
4.41 (3.11) |
|
4 (N=47) |
40 |
15-minute infusion |
0.36 (0.79) |
0.22 (0.39) |
4.74 (3.65) |
3.52 (2.86) |
14.2 Bleeding Gastric or Duodenal Ulcers
A randomized, double blind, placebo-controlled clinical study was conducted in 764 patients who presented with endoscopically confirmed gastric or duodenal ulcer bleeding. The population was 18 to 98 years old; 68% were male, 87% Caucasian, 1% Black, 7% Asian, and 4% other race. Following endoscopic hemostasis, patients were randomized to either placebo or esomeprazole sodium for injection 80 mg as an intravenous infusion over 30 minutes followed by a continuous infusion of 8 mg/hour for a total of 72 hours. After the initial 72-hour period, all patients received an oral PPI for 27 days. The occurrence of rebleeding within 3 days of randomization was 5.9% in the esomeprazole sodium for injection treated group compared to 10.3% for the placebo group (treatment difference -4.4%; 95% confidence interval: -8.3%, -0.6%; p=0.03). This treatment difference was similar to that observed at Day 7 and Day 30, during which all patients were receiving an oral PPI.
A randomized, double blind, placebo-controlled single-center study conducted in Hong Kong also demonstrated a reduction compared to placebo in the risk of rebleeding within 72 hours in patients with bleeding gastric or duodenal ulcers who received racemic omeprazole, 50% of which is the S-enantiomer esomeprazole.
16. How is Esomeprazole Injection supplied
Esomeprazole sodium for injection is supplied in a single-dose vial as a as a white to off-white lyophilized powder for reconstitution containing 40 mg of esomeprazole.
Esomeprazole sodium for injection is available as follows:
|
NDC Number |
Strength |
Package Size |
|
70436-190-82 |
40 mg esomeprazole |
10 vials |
Storage
Store at 25°C (77°F); excursions permitted to 15° to 30°C (59° to 86°F). [See USP Controlled Room Temperature.] Protect from light. Store in carton until time of use.
Following reconstitution and administration, discard any unused portion of esomeprazole solution [see Dosage and Administration (2.4, 2.5)] .
17. Patient Counseling Information
Adverse Reactions
Advise patients to report to their healthcare provider if they experience any signs or symptoms consistent with:
- Hypersensitivity Reactions [see Contraindications (4)]
- Acute Tubulointerstitial Nephritis [see Warnings and Precautions (5.2)]
- Clostridium difficile-Associated Diarrhea [see Warnings and Precautions (5.3)]
- Bone Fracture [see Warnings and Precautions (5.4)]
- Severe Cutaneous Adverse Reactions [see Warnings and Precautions (5.5)].
- Cutaneous and Systemic Lupus Erythematosus [see Warnings and Precaution (5.6)]
- Hypomagnesemia [see Warnings and Precautions (5.8)]
Drug Interactions
Advise patients to report to their healthcare provider before they start treatment with any of the following:
- Rilpivirine-containing products [see Contraindications (4)]
- Clopidogrel [see Warnings and Precautions (5.7)]
- St. John’s Wort or rifampin [see Warnings and Precautions (5.9)]
- High-dose methotrexate [see Warnings and Precautions (5.11)]
Administration
- Inform patients that antacids may be used while taking esomeprazole sodium for injection
Manufactured by:
Hainan Poly Pharm. Co., Ltd., Guilinyang Economic Development Zone, Haikou, Hainan Province, China 571127
Distributed by:
Slate Run Pharmaceuticals, LLC, Columbus, Ohio 43215
10000344/03
Revised: 10/2023
| ESOMEPRAZOLE SODIUM
esomeprazole sodium injection, powder, lyophilized, for solution |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| Labeler - Slate Run Pharmaceuticals, LLC (039452765) |
| Establishment | |||
| Name | Address | ID/FEI | Business Operations |
|---|---|---|---|
| Hainan Poly Pharm. Co., Ltd. | 654561638 | manufacture(70436-190) , analysis(70436-190) , pack(70436-190) , api manufacture(70436-190) | |
Frequently asked questions
More about esomeprazole
- Check interactions
- Compare alternatives
- Pricing & coupons
- Reviews (276)
- Drug images
- Side effects
- Dosage information
- Patient tips
- During pregnancy
- Support group
- Drug class: proton pump inhibitors
- Breastfeeding
Patient resources
Professional resources
- Esomeprazole monograph
- Esomeprazole (FDA)
- Esomeprazole Capsules (FDA)
- Esomeprazole ODT (FDA)
- Esomeprazole Oral Suspension (FDA)
- Esomeprazole Strontium Capsules (FDA)