Cortifoam: Package Insert / Prescribing Info
Package insert / product label
Generic name: hydrocortisone acetate
Dosage form: rectal aerosol, foam
Drug class: Topical steroids
Medically reviewed by Drugs.com. Last updated on May 16, 2024.
On This Page
Cortifoam Description
Cortifoam® (hydrocortisone acetate rectal aerosol) 10% Rectal Foam contains hydrocortisone acetate 10% in a base containing propylene glycol, emulsifying wax, polyoxyethylene-10-stearyl ether, cetyl alcohol, methylparaben, propylparaben, trolamine, purified water and inert propellants: isobutane and propane.
Each application delivers approximately 900 mg of foam containing 80 mg of hydrocortisone (90 mg of hydrocortisone acetate).
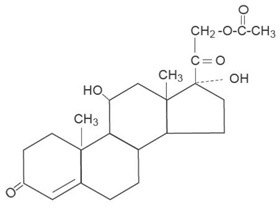
The molecular weight of hydrocortisone acetate is 404.50. It is designated chemically as pregn-4-ene-3,20-dione,21-(acetyloxy)-11,17-dihydroxy-,(11β)-. The empirical formula is C23H32O6 and the structural formula is:
Hydrocortisone acetate, a synthetic adrenocortical steroid, is a white to practically white, odorless, crystalline powder. It is insoluble in water (1 mg/100 mL) and slightly soluble in alcohol and chloroform.
Cortifoam - Clinical Pharmacology
Cortifoam® provides effective topical administration of an anti-inflammatory corticosteroid as adjunctive therapy of ulcerative proctitis. Direct observations of methylene blue-containing foam have shown staining about 10 centimeters into the rectum.
Indications and Usage for Cortifoam
Cortifoam® is indicated as adjunctive therapy in the topical treatment of ulcerative proctitis of the distal portion of the rectum in patients who cannot retain hydrocortisone or other corticosteroid enemas.
Contraindications
Cortifoam® is contraindicated in patients who are hypersensitive to any components of this product.
Local contraindications to the use of intrarectal steroids include obstruction, abscess, perforation, peritonitis, fresh intestinal anastomoses, extensive fistulas and sinus tracts.
Warnings
General
Do not insert any part of the aerosol container directly into the anus. Contents of the container are under pressure. Do not burn or puncture the aerosol container. Do not store at temperatures above 120°F. Because Cortifoam® is not expelled, systemic hydrocortisone absorption may be greater from Cortifoam® than from corticosteroid enema formulations. If there is not evidence of clinical or proctologic improvement within two or three weeks after starting Cortifoam® therapy, or if the patient's condition worsens, discontinue the drug.
Rare instances of anaphylactoid reactions have occurred in patients receiving corticosteroid therapy (see ADVERSE REACTIONS).
Cardio-renal
Corticosteroids can cause elevation of blood pressure, salt and water retention, and increased excretion of potassium. These effects are less likely to occur with the synthetic derivatives except when used in large doses. Dietary salt restriction and potassium supplementation may be necessary. All corticosteroids increase calcium excretion.
Literature reports suggest an apparent association between use of corticosteroids and left ventricular free wall rupture after a recent myocardial infarction; therefore, therapy with corticosteroids should be used with great caution in these patients.
Endocrine
Corticosteroids can produce reversible hypothalamicpituitary adrenal (HPA) axis suppression with the potential for glucocorticosteroid insufficiency after withdrawal of treatment.
Metabolic clearance of corticosteroids is decreased in hypothyroid patients and increased in hyperthyroid patients. Changes in thyroid status of the patient may necessitate adjustment in dosage.
Infections
General
Patients who are on corticosteroids are more susceptible to infections than are healthy individuals. There may be decreased resistance and inability to localize infection when corticosteroids are used. Infection with any pathogen (viral, bacterial, fungal, protozoan or helminthic) in any location of the body may be associated with the use of corticosteroids alone or in combination with other immunosuppressive agents. These infections may be mild to severe. With increasing doses of corticosteroids, the rate of occurrence of infectious complications increases. Corticosteroids may also mask some signs of current infection.
Fungal infections
Corticosteroids may exacerbate systemic fungal infections and therefore should not be used in the presence of such infections unless they are needed to control drug reactions. There have been cases reported in which concomitant use of amphotericin B and hydrocortisone was followed by cardiac enlargement and congestive heart failure (see PRECAUTIONS, Drug Interactions, Amphotericin B injection and potassium-depleting agents).
Special pathogens
Latent disease may be activated or there may be an exacerbation of intercurrent infections due to pathogens, including those caused by Amoeba, Candida, Cryptococcus, Mycobacterium, Nocardia, Pneumocystis, and Toxoplasma.
It is recommended that latent amebiasis or active amebiasis be ruled out before initiating corticosteroid therapy in any patient who has spent time in the tropics or in any patient with unexplained diarrhea.
Similarly, corticosteroids should be used with great care in patients with known or suspected Strongyloides (thread worm) infestation. In such patients, corticosteroid-induced immunosuppression may lead to Strongyloides hyperinfection and dissemination with widespread larval migration, often accompanied by severe enterocolitis and potentially fatal gram-negative septicemia.
Corticosteroids should not be used in cerebral malaria.
Tuberculosis
If corticosteroids are indicated in patients with latent tuberculosis or tuberculin reactivity, close observation is necessary as reactivation of the disease may occur. During prolonged corticosteroid therapy, these patients should receive chemoprophylaxis.
Vaccination
Administration of live or live, attenuated vaccines is contraindicated in patients receiving immunosuppressive doses of corticosteroids. Killed or inactivated vaccines may be administered. However, the response to such vaccines cannot be predicted. Immunization procedures may be undertaken in patients who are receiving corticosteroids as replacement therapy, e.g., for Addison's disease.
Viral infections
Chickenpox and measles can have a more serious or even fatal course in pediatric and adult patients on corticosteroids. In pediatric and adult patients who have not had these diseases, particular care should be taken to avoid exposure. The contribution of the underlying disease and/or prior corticosteroid treatment to the risk is also not known. If exposed to chickenpox, prophylaxis with varicella zoster immune globulin (VZIG) may be indicated. If exposed to measles, prophylaxis with immunoglobulin (IG) may be indicated. (See the respective package inserts for complete VZIG and IG prescribing information.) If chickenpox develops, treatment with antiviral agents should be considered.
Ophthalmic
Use of corticosteroids may produce posterior subcapsular cataracts, glaucoma with possible damage to the optic nerves, and may enhance the establishment of secondary ocular infections due to bacteria, fungi, or viruses. If a patient presents with symptoms such as blurred vision or other visual disturbances, the patient should be considered for referral to an ophthalmologist for evaluation. The use of oral corticosteroids is not recommended in the treatment of optic neuritis and may lead to an increase in the risk of new episodes. Corticosteroids should not be used in active ocular herpes simplex.
Precautions
General
The lowest possible dose of corticosteroid should be used to control the condition under treatment. When reduction in dosage is possible, the reduction should be gradual.
Since complications of treatment with glucocorticoids are dependent on the size of the dose and the duration of treatment, a risk/benefit decision must be made in each individual case as to dose and duration of treatment and as to whether daily or intermittent therapy should be used.
Kaposi's sarcoma has been reported to occur in patients receiving corticosteroid therapy, most often for chronic conditions. Discontinuation of corticosteroids may result in clinical improvement.
Cardio-renal
As sodium retention with resultant edema and potassium loss may occur in patients receiving corticosteroids, these agents should be used with caution in patients with congestive heart failure, hypertension, or renal insufficiency.
Endocrine
Drug-induced secondary adrenocortical insufficiency may be minimized by gradual reduction of dosage. This type of relative insufficiency may persist for months after discontinuation of therapy; therefore, in any situation of stress occurring during that period, hormone therapy should be reinstituted. Since mineralocorticoid secretion may be impaired, salt and/or a mineralocorticoid should be administered concurrently.
Gastrointestinal
Steroids should be used with caution in active or latent peptic ulcers, diverticulitis, fresh intestinal anastomoses, and nonspecific ulcerative colitis, since they may increase the risk of a perforation. Where surgery is imminent, it is hazardous to wait more than a few days for a satisfactory response to medical treatment.
Do not employ in immediate or early postoperative period following ileorectostomy.
Signs of peritoneal irritation following gastrointestinal perforation in patients receiving corticosteroids may be minimal or absent.
There is an enhanced effect of corticosteroids in patients with cirrhosis.
Musculoskeletal
Corticosteroids decrease bone formation and increase bone resorption both through their effect on calcium regulation (i.e., decreasing absorption and increasing excretion) and inhibition of osteoblast function. This, together with a decrease in the protein matrix of the bone secondary to an increase in protein catabolism, and reduced sex hormone production, may lead to inhibition of bone growth in pediatric patients and the development of osteoporosis at any age. Special consideration should be given to patients at increased risk of osteoporosis (i.e., postmenopausal women) before initiating corticosteroid therapy.
Neuro-psychiatric
An acute myopathy has been observed with the use of high doses of corticosteroids, most often occurring in patients with disorders of neuromuscular transmission (e.g., myasthenia gravis), or in patients receiving concomitant therapy with neuromuscular blocking drugs (e.g., pancuronium). This acute myopathy is generalized, may involve ocular and respiratory muscles, and may result in quadriparesis. Elevation of creatinine kinase may occur. Clinical improvement or recovery after stopping corticosteroids may require weeks to years.
Psychic derangements may appear when corticosteroids are used, ranging from euphoria, insomnia, mood swings, personality changes, and severe depression to frank psychotic manifestations. Also, existing emotional instability or psychotic tendencies may be aggravated by corticosteroids.
Ophthalmic
Intraocular pressure may become elevated in some individuals. If steroid therapy is continued for more than 6 weeks, intraocular pressure should be monitored.
Information for Patients
Patients should be warned not to discontinue the use of corticosteroids abruptly or without medical supervision, to advise any medical attendants that they are taking corticosteroids and to seek medical advice at once should they develop fever or other signs of infection.
Persons who are on corticosteroids should be warned to avoid exposure to chickenpox or measles. Patients should also be advised that if they are exposed, medical advice should be sought without delay.
Drug Interactions
Aminoglutethimide: Aminoglutethimide may lead to a loss of corticosteroid-induced adrenal suppression.
Amphotericin B injection and potassium-depleting agents: When corticosteroids are administered concomitantly with potassium-depleting agents (i.e., amphotericin B, diuretics), patients should be observed closely for development of hypokalemia. There have been cases reported in which concomitant use of amphotericin B and hydrocortisone was followed by cardiac enlargement and congestive heart failure.
Antibiotics: Macrolide antibiotics have been reported to cause a significant decrease in corticosteroid clearance.
Anticholinesterases: Concomitant use of anticholinesterase agents and corticosteroids may produce severe weakness in patients with myasthenia gravis. If possible, anticholinesterase agents should be withdrawn at least 24 hours before initiating corticosteroid therapy.
Anticoagulants, oral: Coadministration of corticosteroids and warfarin result in inhibition of response to warfarin. Therefore, coagulation indices should be monitored to maintain the desired anticoagulant effect.
Antidiabetics: Because corticosteroids may increase blood glucose concentrations, dosage adjustments of antidiabetic agents may be required.
Antitubercular drugs: Serum concentrations of isoniazid may be decreased.
Cholestyramine: Cholestyramine may increase the clearance of corticosteroids.
Cyclosporine: Increased activity of both cyclosporine and corticosteroids may occur when the two are used concurrently. Convulsions have been reported with this concurrent use.
Digitalis glycosides: Patients on digitalis glycosides may be at increased risk of arrhythmias due to hypokalemia.
Estrogens, including oral contraceptives: Estrogens may decrease the hepatic metabolism of certain corticosteroids, thereby increasing their effect.
Hepatic Enzyme Inducers (e.g., barbiturates, phenytoin, carbamazepine, rifampin): Drugs which induce hepatic microsomal drug metabolizing enzyme activity may enhance the metabolism of corticosteroids and require that the dosage of the corticosteroid be increased.
Ketoconazole: Ketoconazole has been reported to decrease the metabolism of certain corticosteroids by up to 60%, leading to an increased risk of corticosteroids side effects.
Nonsteroidal anti-inflammatory agents (NSAIDS): Concomitant use of aspirin (or other nonsteroidal anti-inflammatory agents) and corticosteroids increases the risk of gastrointestinal side effects. Aspirin should be used cautiously in conjunction with corticosteroids in hypoprothrombinemia. The clearance of salicylates may be increased with concurrent use of corticosteroids.
Skin tests: Corticosteroids may suppress reactions to skin tests.
Vaccines: Patients on prolonged corticosteroid therapy may exhibit a diminished response to toxoids and live or inactivated vaccines due to inhibition of antibody response. Corticosteroids may also potentiate the replication of some organisms contained in live attenuated vaccines. Routine administration of vaccines or toxoids should be deferred until corticosteroid therapy is discontinued if possible (see WARNINGS, Infections, Vaccination).
Carcinogenesis, Mutagenesis, Impairment of Fertility
No adequate studies have been conducted in animals to determine whether corticosteroids have a potential for carcinogenesis or mutagenesis.
Steroids may increase or decrease motility and number of spermatozoa in some patients.
Pregnancy
Teratogenic Effects
Corticosteroids have been shown to be teratogenic in many species when given in doses equivalent to the human dose. Animal studies in which corticosteroids have been given to pregnant mice, rats, and rabbits have yielded an increased incidence of cleft palate in the offspring. There are no adequate and well-controlled studies in pregnant women. Corticosteroids should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus. Infants born to mothers who have received corticosteroids during pregnancy should be carefully observed for signs of hypoadrenalism.
Nursing Mothers
Systemically administered corticosteroids appear in human milk and could suppress growth, interfere with endogenous corticosteroid production, or cause other untoward effects. Caution should be exercised when corticosteroids are administered to a nursing woman.
Geriatric Use
No overall differences in safety or effectiveness were observed between elderly subjects and younger subjects, and other reported clinical experience has not identified differences in responses between the elderly and younger patients, but greater sensitivity of some older individuals cannot be ruled out.
Adverse Reactions/Side Effects
(listed alphabetically, under each subsection)
To report SUSPECTED ADVERSE REACTIONS, contact Meda Pharmaceuticals Inc. at 1-877-848-6608 or
FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Allergic reactions: Anaphylactoid reaction, anaphylaxis, angioedema.
Cardiovascular: Bradycardia, cardiac arrest, cardiac arrhythmias, cardiac enlargement, circulatory collapse, congestive heart failure, fat embolism, hypertension, hypertrophic cardiomyopathy in premature infants, myocardial rupture following recent myocardial infarction (see WARNINGS), pulmonary edema, syncope, tachycardia, thromboembolism, thrombophlebitis, vasculitis.
Dermatologic: Acne, allergic dermatitis, cutaneous and subcutaneous atrophy, dry scaly skin, ecchymoses and petechiae, edema, erythema, hyperpigmentation, hypopigmentation, impaired wound healing, increased sweating, rash, sterile abscess, striae, suppressed reactions to skin tests, thin fragile skin, thinning scalp hair, urticaria.
Endocrine: Decreased carbohydrate and glucose tolerance, development of cushingoid state, glycosuria, hirsutism, hypertrichosis, increased requirements for insulin or oral hypoglycemic agents in diabetes, manifestations of latent diabetes mellitus, menstrual irregularities, secondary adrenocortical and pituitary unresponsiveness (particularly in times of stress, as in trauma, surgery, or illness), suppression of growth in pediatric patients.
Fluid and electrolyte disturbances: Congestive heart failure in susceptible patients, fluid retention, hypokalemic alkalosis, potassium loss, sodium retention.
Where hypokalemia and other symptoms associated with fluid and electrolyte imbalance call for potassium supplementation and salt poor or salt-free diets, these may be instituted and are compatible with diet requirements for ulcerative proctitis.
Gastrointestinal: Abdominal distention, elevation in serum liver enzyme levels (usually reversible upon discontinuation), hepatomegaly, increased appetite, nausea, pancreatitis, peptic ulcer with possible perforation and hemorrhage, perforation of the small and large intestine (particularly in patients with inflammatory bowel disease), ulcerative esophagitis.
Metabolic: Negative nitrogen balance due to protein catabolism.
Musculoskeletal: Aseptic necrosis of femoral and humeral heads, Charcot-like arthropathy, loss of muscle mass, muscle weakness, osteoporosis, pathologic fracture of long bones, steroid myopathy, tendon rupture, vertebral compression fractures.
Neurologic/Psychiatric: Convulsions, depression, emotional instability, euphoria, headache, increased intracranial pressure with papilledema (pseudotumor cerebri) usually following discontinuation of treatment, insomnia, mood swings, neuritis, neuropathy, paresthesia, personality changes, psychic disorders, vertigo.
Ophthalmic: Blurred vision, exophthalmos, glaucoma, increased intraocular pressure, posterior subcapsular cataracts, rare instances of blindness associated with periocular injections.
Other: Abnormal fat deposits, decreased resistance to infection, hiccups, increased or decreased motility and number of spermatozoa, malaise, moon face, weight gain.
Related/similar drugs
Overdosage
Treatment of acute overdosage is by supportive and symptomatic therapy. For chronic overdosage in the face of severe disease requiring continuous steroid therapy, the dosage of the corticosteroid may be reduced only temporarily, or alternate day treatment may be introduced.
Cortifoam Dosage and Administration
The usual dose is one applicatorful once or twice daily for two or three weeks, and every second day thereafter, administered rectally. Directions for use, below and on the carton, describe how to use the aerosol container and applicator. Satisfactory response usually occurs within five to seven days marked by a decrease in symptoms. Symptomatic improvement in ulcerative proctitis should not be used as the sole criterion for evaluating efficacy. Sigmoidoscopy is also recommended to judge dosage adjustment, duration of therapy, and rate of improvement.
It Should Be Emphasized that Dosage Requirements are Variable and Must Be Individualized on the Basis of the Disease Under Treatment and the Response of the Patient. After a favorable response is noted, the proper maintenance dosage should be determined by decreasing the initial drug dosage in small decrements at appropriate time intervals until the lowest dosage which will maintain an adequate clinical response is reached. Situations which may make dosage adjustments necessary are changes in clinical status secondary to remissions or exacerbations in the disease process, the patient's individual drug responsiveness, and the effect of patient exposure to stressful situations not directly related to the disease entity under treatment. In this latter situation it may be necessary to increase the dosage of the corticosteroid for a period of time consistent with the patient's condition. If after long-term therapy the drug is to be stopped, it is recommended that it be withdrawn gradually rather than abruptly.
Directions For Use
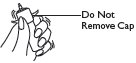
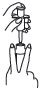
(1) Shake foam container vigorously for 5-10 seconds before each use. Do not remove container cap during use of the product.
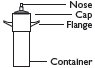
(2) Hold container upright on a level surface and gently place the tip of the applicator onto the nose of the container cap. CONTAINER MUST BE HELD UPRIGHT TO OBTAIN PROPER FLOW OF MEDICATION.
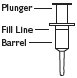
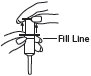
(3) Pull plunger past the fill line on the applicator barrel.
(4) To fill applicator barrel, press down firmly on cap flanges, hold for 1 – 2 seconds and release. Pause 5 – 10 seconds to allow foam to expand in applicator barrel. Repeat until foam reaches fill line. Remove applicator from container cap. Allow some foam to remain on the applicator tip. A burst of air may come out of container with first pump.
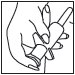
(5) Hold applicator firmly by barrel, making sure thumb and middle finger are positioned securely underneath and resting against barrel wings. Place index finger over the plunger. Gently insert tip into anus. Once in place, push plunger to expel foam, then withdraw applicator.
CAUTION: Do not insert any part of the aerosol container directly into the anus. Apply to anus only with enclosed applicator.
(6) After each use, applicator parts should be pulled apart for thorough cleaning with warm water. The container cap and underlying tip should also be pulled apart and rinsed to help prevent build-up of foam and possible blockage.
How is Cortifoam supplied
Cortifoam® is supplied in an aerosol container with a special rectal applicator. Each applicator delivers approximately 900 mg of foam containing approximately 80 mg of hydrocortisone as 90 mg of hydrocortisone acetate. When used correctly, the aerosol container will deliver a minimum of 14 applications.
NDC 0037-6830-15 15 g
Store at controlled room temperature, 20°-25°C (68°-77°F).
DO NOT REFRIGERATE.
Rx Only
Distributed by:
Meda Pharmaceuticals Inc.
Canonsburg, PA 15317 U.S.A.
© 2024 Mylan Specialty L.P., a Viatris Company
For Medical Inquiries, call toll-free 1-877-848-6608
CORTIFOAM is a registered trademark of Alaven Pharmaceutical LLC, a Viatris Company.
IN-683015-05
141280-0324
PRINCIPAL DISPLAY PANEL - 15 g Label
NDC 0037-6830-15
cortifoam®
(hydrocortisone acetate 10%)
rectal foam
Rx Only
15 g net wt
DIRECTIONS FOR USE
Description: cortifoam® (hydrocortisone acetate) 10% rectal foam contains hydrocortisone acetate 10% in a base containing propylene glycol, emulsifying wax, polyoxyethylene-10-stearyl ether, cetyl alcohol, methylparaben, propyl-paraben, trolamine, purified water and inert propellants: isobutane and propane.
Dosage: One applicatorful once or twice daily for two or three weeks, and every second day thereafter, administered rectally. See back of carton for full directions for use.
Please see package insert for further information. For rectal use only.
117756-0324 UC-683015-05
Caution: Do not insert any part of the aerosol container directly into the anus. Apply to anus only with the enclosed applicator.
WARNINGS: Contents of the container are under pressure. Do not burn or puncture the aerosol container. Do not store at temperatures above 120°F (49°C).
KEEP OUT OF REACH OF CHILDREN.
Store upright at controlled room temperature 20° - 25°C (68° - 77°F).
DO NOT REFRIGERATE
Distributed by: Meda Pharmaceuticals Inc., Canonsburg, PA 15317 U.S.A.
© 2024 Mylan Specialty L.P., a Viatris Company
CORTIFOAM is a registered trademark of Alaven Pharmaceutical LLC, a Viatris company.
| CORTIFOAM
hydrocortisone acetate aerosol, foam |
||||||||||||||||||||||||
|
||||||||||||||||||||||||
|
||||||||||||||||||||||||
|
||||||||||||||||||||||||
|
||||||||||||||||||||||||
|
||||||||||||||||||||||||
|
||||||||||||||||||||||||
| Labeler - Meda Pharmaceuticals Inc. (051229602) |
More about hydrocortisone topical
- Check interactions
- Compare alternatives
- Pricing & coupons
- Reviews (66)
- Drug images
- Side effects
- Dosage information
- During pregnancy
- Drug class: topical steroids
- Breastfeeding
Patient resources
Professional resources
- Hydrocortisone (Topical) monograph
- Hydrocort Lotion (FDA)
- Hydrocortisone (FDA)
- Hydrocortisone 2.5% (FDA)
- Hydrocortisone Butyrate (FDA)
Other brands
Westcort, Anusol-HC Suppositories, Anucort-HC, Proctozone HC, ... +15 more