Botox Cosmetic: Package Insert / Prescribing Info
Package insert / product label
Generic name: onabotulinumtoxinA
Dosage form: injection, powder, lyophilized, for solution
Drug class: Skeletal muscle relaxants
J Code (medical billing code): J0585 (Per unit, injection)
Medically reviewed by Drugs.com. Last updated on Nov 4, 2024.
On This Page
- Indications and Usage
- Dosage and Administration
- Dosage Forms and Strengths
- Contraindications
- Warnings and Precautions
- Adverse Reactions/Side Effects
- Drug Interactions
- Use In Specific Populations
- Overdosage
- Description
- Clinical Pharmacology
- Nonclinical Toxicology
- Clinical Studies
- How Supplied/Storage and Handling
- Patient Counseling Information
- Medication Guide
Highlights of Prescribing Information
BOTOX® Cosmetic (onabotulinumtoxinA) for injection,
for intramuscular use
Initial U.S. Approval: 1989
WARNING: DISTANT SPREAD OF TOXIN EFFECT
See full prescribing information for complete boxed warning.
The effects of BOTOX Cosmetic and all botulinum toxin products may spread from the area of injection to produce symptoms consistent with botulinum toxin effects. These symptoms have been reported hours to weeks after injection. Swallowing and breathing difficulties can be life threatening and there have been reports of death. The risk of symptoms is probably greatest in children treated for spasticity but symptoms can also occur in adults, particularly in those patients who have an underlying condition that would predispose them to these symptoms. (5.2)
Recent Major Changes
Indications and Usage for Botox Cosmetic
BOTOX Cosmetic is an acetylcholine release inhibitor and a neuromuscular blocking agent indicated in adult patients for the temporary improvement in the appearance of (1):
- Moderate to severe glabellar lines associated with corrugator and/or procerus muscle activity
- Moderate to severe lateral canthal lines associated with orbicularis oculi activity
- Moderate to severe forehead lines associated with frontalis muscle activity
- Moderate to severe platysma bands associated with platysma muscle activity
Botox Cosmetic Dosage and Administration
- Glabellar Lines Administration: 0.1 mL (4 Units) into each of 5 sites, for a total dose of 20 Units (2.4)
- Lateral Canthal Lines Administration: 0.1 mL (4 Units) into each of 3 sites per side (6 total injection points), for a total of 24 Units (2.4)
- Forehead Lines Administration: 0.1 mL (4 Units) into each of 5 forehead line sites (20 Units) with 0.1 mL (4 Units) into each of 5 glabellar line sites (20 Units), for a recommended total of 40 Units (2.4)
- Platysma Bands Administration: 0.05 mL (2 Units) into each of 4 sites in the upper segment of the platysma muscles, below the jawline on each side and 0.025 mL (1 Unit) into 5 sites on each vertical neck band per side (1 to 2 bands per side) for a total of 26 Units, 31 Units, or 36 Units (18, 23, or 28 injection sites, respectively) (2.4)
- BOTOX Cosmetic is administered by intramuscular injection (2.2)
- Follow dosage and administration recommendations. Do not exceed the maximum recommended cumulative dose in a treatment session for any indication (2.1, 2.2)
- See Preparation and Reconstitution Instructions for information on BOTOX Cosmetic reconstitution, storage, and preparation before injection (2.3)
Dosage Forms and Strengths
For Injection: 50 Units or 100 Units vacuum-dried powder in a single-dose vial for reconstitution (3)
Contraindications
Warnings and Precautions
- Potency Units of BOTOX Cosmetic cannot be compared to or converted into Units of any other preparations of botulinum toxin products (5.1, 11)
- Spread of toxin effects; swallowing and breathing difficulties can lead to death. Seek immediate medical attention if respiratory, speech or swallowing difficulties occur (5.2, 5.7)
- Potential serious adverse reactions after administration of BOTOX for unapproved uses (5.3)
- Adverse event reports have been received involving the cardiovascular system, some with fatal outcomes. Use caution when administering to patients with pre-existing cardiovascular disease. (5.5)
- Concomitant neuromuscular disorder may exacerbate clinical effects of treatment (5.6)
- Use with caution in patients with compromised respiratory function or dysphagia (5.7)
Adverse Reactions/Side Effects
The most common adverse reactions are (6.1):
- Glabellar Lines: eyelid ptosis (3%)
- Lateral Canthal Lines: eyelid edema (1%)
- Forehead Lines: headache (9%) and brow ptosis (2%)
To report SUSPECTED ADVERSE REACTIONS, contact AbbVie at 1-800-678-1605 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Drug Interactions
Patients receiving concomitant treatment of BOTOX Cosmetic and aminoglycosides or other agents interfering with neuromuscular transmission (e.g., curare-like agents), or muscle relaxants, should be observed closely because the effect of BOTOX Cosmetic may be potentiated (7)
See 17 for PATIENT COUNSELING INFORMATION and Medication Guide.
Revised: 10/2024
Full Prescribing Information
WARNING: DISTANT SPREAD OF TOXIN EFFECT
Postmarketing reports indicate that the effects of BOTOX Cosmetic and all botulinum toxin products may spread from the area of injection to produce symptoms consistent with botulinum toxin effects. These may include asthenia, generalized muscle weakness, diplopia, ptosis, dysphagia, dysphonia, dysarthria, urinary incontinence and breathing difficulties. These symptoms have been reported hours to weeks after injection. Swallowing and breathing difficulties can be life threatening and there have been reports of death. The risk of symptoms is probably greatest in children treated for spasticity but symptoms can also occur in adults treated for spasticity and other conditions, particularly in those patients who have an underlying condition that would predispose them to these symptoms. In unapproved uses and in approved indications, cases of spread of effect have been reported at doses comparable to those used to treat cervical dystonia and spasticity and at lower doses. [see Warnings and Precautions (5.2)]
1. Indications and Usage for Botox Cosmetic
BOTOX Cosmetic (onabotulinumtoxinA) is indicated in adult patients for the temporary improvement in the appearance of:
• moderate to severe glabellar lines associated with corrugator and/or procerus muscle activity
• moderate to severe lateral canthal lines associated with orbicularis oculi activity
• moderate to severe forehead lines associated with frontalis muscle activity
• moderate to severe platysma bands associated with platysma muscle activity
2. Botox Cosmetic Dosage and Administration
2.1 Instructions for Safe Use
The potency Units of BOTOX Cosmetic (onabotulinumtoxinA) for injection are specific to the preparation and assay method utilized. BOTOX Cosmetic is not equivalent to other preparations of botulinum toxin products, and therefore, units of biological activity of BOTOX Cosmetic cannot be compared to nor converted into units of any other botulinum toxin products assessed with any other specific assay method [see Warnings and Precautions (5.1) and Description (11)].
Follow indication specific dosage and administration recommendations. Do not exceed the maximum recommended cumulative dose in a treatment session for any indication.
The safe and effective use of BOTOX Cosmetic depends upon proper storage of the product, selection of the correct dose, and proper reconstitution and administration techniques. Physicians administering BOTOX Cosmetic must understand the relevant neuromuscular and structural anatomy of the area involved and any alterations to the anatomy due to prior surgical procedures and disease.
Do not use BOTOX Cosmetic and contact AbbVie (1-800-678-1605) if:
- The tamper evident features on the carton appear to be broken or compromised, or
- The U.S. License number 1889 is not present on the vial label and carton labeling [see How Supplied/Storage and Handling (16)]
2.2 Recommended Dose
The total recommended dose in adult patients by treatment area is shown in Table 1. BOTOX Cosmetic is administered by intramuscular injection.
| Treatment Area | Total Recommended Treatment Dose |
| Glabellar lines | 20 Units in 0.5 mL |
| Lateral canthal lines | 24 Units in 0.6 mL |
| Forehead lines and glabellar lines | 40 Units in 1 mL |
| Platysma bands | One band on each side: 26 Units in 0.65 mL 1 band on one side, 2 bands on the other side: 31 Units in 0.78 mL Two bands on each side: 36 Units in 0.9 mL |
The safety and effectiveness of dosing with BOTOX Cosmetic more frequently than every 3 months have not been clinically evaluated.
2.3 Preparation and Reconstitution Instructions
BOTOX Cosmetic is supplied in single-dose 50 Units and 100 Units per vial. Prior to intramuscular injection, reconstitute each vacuum-dried vial of BOTOX Cosmetic with sterile, preservative-free 0.9% Sodium Chloride Injection USP (see Table 2). Draw up the proper amount of diluent in the appropriate size needle and syringe to obtain a reconstituted solution at a concentration of 4 Units/0.1 mL.
| Vial | Amount of Diluent* Added | Resulting Dose Units per 0.1 mL |
| 50 Units | 1.25 mL | 4 Units |
| 100 Units | 2.5 mL | 4 Units |
*Preservative-free 0.9% Sodium Chloride Injection, USP Only
Slowly inject the diluent into the vial. Discard the vial if a vacuum does not pull the diluent into the vial. Gently mix BOTOX Cosmetic with the saline by rotating the vial. Record the date and time of reconstitution on the space on the label. Administer BOTOX Cosmetic within 24 hours after reconstitution. During this time period, store reconstituted BOTOX Cosmetic in a refrigerator at 2°C to 8°C (36°F to 46°F). Do not freeze reconstituted BOTOX Cosmetic. BOTOX Cosmetic vials are for single-dose only. Discard any remaining solution.
Reconstituted BOTOX Cosmetic is clear, colorless to slightly yellow solution, and free of particulate matter. Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration and whenever the solution and the container permit. Do not use if the solution is cloudy or contains flakes or particles.
2.4 Administration
Draw properly reconstituted toxin into the sterile syringe, preferably a tuberculin syringe, and expel any air bubbles in the syringe barrel (see Table 3). Remove the needle used to reconstitute the product and attach a 30-33 gauge needle. Confirm the patency of the needle.
| Treatment Area | Amount of Reconstituted Toxin to Draw |
| Glabellar lines | At least 0.5 mL |
| Lateral canthal lines | At least 0.6 mL |
| Forehead lines and glabellar lines | At least 1 mL |
| Platysma bands |
|
Glabellar Lines
An effective dose for facial lines is determined by gross observation of the patient’s ability to activate the superficial muscles injected.
In order to reduce the complication of ptosis, take the following steps:
- Avoid injection near the levator palpebrae superioris, particularly in patients with larger brow depressor complexes.
- Place lateral corrugator injections at least 1 cm above the bony supraorbital ridge.
- Ensure the injected volume/dose is accurate and where feasible kept to a minimum.
- Do not inject toxin closer than 1 cm above the central eyebrow.
Inject 4 Units (0.1 mL) of reconstituted BOTOX Cosmetic intramuscularly into each of 5 sites, 2 in each corrugator muscle and 1 in the procerus muscle for a total dose of 20 Units (see Figure 1). Typically, the initial doses of reconstituted BOTOX Cosmetic induce chemical denervation of the injected muscles one to two days after injection, increasing in intensity during the first week.
The duration of effect of BOTOX Cosmetic for glabellar lines is approximately 3-4 months.
Figure 1:
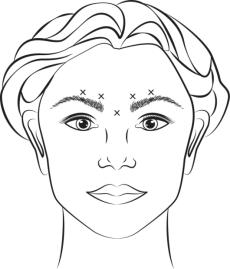
Lateral Canthal Lines
Give injections with the needle bevel tip up and oriented away from the eye. Inject 4 Units (0.1 mL) of reconstituted BOTOX Cosmetic into 3 sites per side (6 total injection points) in the lateral orbicularis oculi muscle for a total of 24 Units (0.6 mL) (12 Units per side). Administer the first injection (A) approximately 1.5-2.0 cm temporal to the lateral canthus and just temporal to the orbital rim. If the lines in the lateral canthal region are above and below the lateral canthus, inject per Figure 2. Alternatively, if the lines in the lateral canthal region are primarily below the lateral canthus, inject per Figure 3.
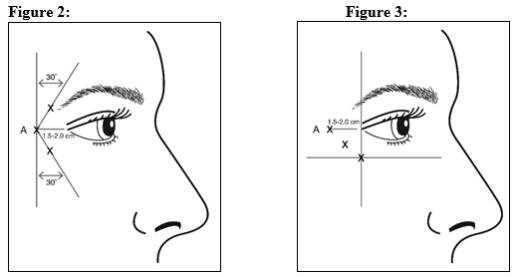
For simultaneous treatment with glabellar lines, the dose is 24 Units for lateral canthal lines and 20 Units for glabellar lines (see Glabellar Lines Administration and Figure 1), with a total dose of 44 Units.
Forehead Lines in Conjunction with Glabellar Lines
Treat forehead lines in conjunction with glabellar lines (see Glabellar Lines Administration and Figure 1) to minimize the potential for brow ptosis. The recommended total dose for treatment of forehead lines (20 Units [0.5 mL]) in conjunction with glabellar lines (20 Units [0.5 mL]) is 40 Units (1 mL).
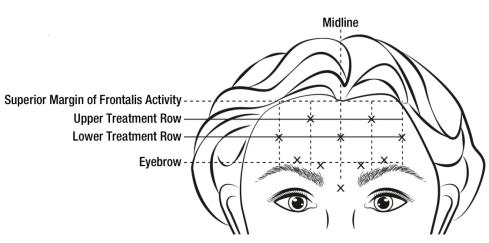
When identifying the location of the appropriate injection sites in the frontalis muscle, assess the overall relationship between the size of the subject’s forehead, and the distribution of frontalis muscle activity.
Locate the following horizontal treatment rows by light palpation of the forehead at rest and maximum eyebrow elevation:
- Superior Margin of Frontalis Activity: approximately 1 cm above the most superior forehead crease
- Lower Treatment Row: midway between the superior margin of frontalis activity and the eyebrow, at least 2 cm above the eyebrow
- Upper Treatment Row: midway between the superior margin of frontalis activity and lower treatment row
Inject 4 Units (0.1 mL) of reconstituted BOTOX Cosmetic into 5 sites in the frontalis muscle, for a total of 20 Units (0.5 mL). Place the 5 injections at the intersection of the horizontal treatment rows with the following vertical landmarks (see Figure 4):
- On the lower treatment row at the midline of the face, and 0.5 – 1.5 cm medial to the palpated temporal fusion line (temporal crest); repeat for the other side.
- On the upper treatment row, midway between the lateral and medial sites on the lower treatment row; repeat for the other side.
Figure 4:
For simultaneous treatment with lateral canthal lines, the total dose is 64 Units, comprised of 20 Units for forehead lines, 20 Units for glabellar lines, and 24 Units for lateral canthal lines (see Lateral Canthal Lines Administration and Figures 2 and 3).
Platysma Bands
Using an appropriately sized sterile syringe, needle, and aseptic technique, inject 2 Units (0.05 mL) of reconstituted BOTOX Cosmetic into 4 sites in the upper segment of platysma muscle, below the jawline on each side. For each side, administer the 4 jawline injections to the upper platysma muscle approximately 1 to 2 cm inferior and parallel to the lower mandibular border. Ensure the anterior injection site is in line with the oral commissure, and the posterior injection is slightly anterior to the angle of the mandible. Administer the remaining 2 injections equidistant (approximately 1 to 2 cm apart) between the anterior and posterior injection points (see Figures 5 and 6).
In addition, inject 1 Unit (0.025 mL) of reconstituted BOTOX Cosmetic into 5 sites along each vertical neck band, 1 to 2 vertical neck bands per side. For each vertical neck band identified, 1 to 2 per side, distribute 5 injections vertically approximately 1 to 2 cm apart (see Figures 5 and 6). Ensure the most superior injection site is approximately 1 to 2 cm inferior to the jawline injections.
Depending on platysma band severity, the total dose may be 26 Units (1 band/side), 31 Units (1 band one side, 2 bands other side), or 36 Units (2 bands/side) (see Table 4 and Figures 5 and 6 below).
Figure 5: Injection Sites for Platysma Band (2 Bands)
 | Figure 6: Injection Sites for Platysma Band (1 Band)
 |
Administer all platysma muscle injections superficially and intramuscularly with the needle perpendicular to the surface of the skin. For vertical neck band injections, identify each band while the patient is contracting their platysma. Gently pinch the band to isolate the muscle from nearby anatomical structures during administration (see Table 4).
To reduce injection-related complications, administer injection at least 1 cm inferior to the lower mandibular border. Do not inject into structures deep to the platysma muscle, particularly in the anterior region of the neck.
| Platysma Bands Presentation | Jawline Injections | Neck Band Injections | Total Number of Injection Sites | Total Dose |
| 1 band on each side | 2 Units (0.05 mL) into 4 sites per side (total of 8 sites and 16 Units) | 1 Unit (0.025 mL) into 5 sites per band (total of 10 sites and 10 Units) | 18 sites | 26 Units (0.65 mL) |
| 1 band on one side,
2 bands on the other side | 2 Units (0.05 mL) into 4 sites per side (total of 8 sites and 16 Units) | 1 Unit (0.025 mL) into 5 sites per band (total of 15 sites and 15 Units) | 23 sites | 31 Units (0.78 mL) |
| 2 bands on each side | 2 Units (0.05 mL) into 4 sites per side (total of 8 sites and 16 Units) | 1 Unit (0.025 mL) into 5 sites per band (total of 20 sites and 20 Units) | 28 sites | 36 Units (0.9 mL) |
3. Dosage Forms and Strengths
- For injection: 50 Units, vacuum-dried powder in a single-dose vial for reconstitution
- For injection: 100 Units, vacuum-dried powder in a single-dose vial for reconstitution
4. Contraindications
4.1 Known Hypersensitivity to Botulinum Toxin
BOTOX Cosmetic is contraindicated in individuals with known hypersensitivity to any botulinum toxin preparation or to any of the components in the formulation [see Warnings and Precautions (5.4)].
5. Warnings and Precautions
5.1 Lack of Equivalency Between Botulinum Toxin Products
The potency Units of BOTOX Cosmetic are specific to the preparation and assay method utilized. BOTOX Cosmetic is not equivalent to other preparations of botulinum toxin products, and therefore, Units of biological activity of BOTOX Cosmetic cannot be compared to nor converted into Units of any other botulinum toxin products assessed with any other specific assay method [see Description (11)].
5.2 Spread of Toxin Effect
Postmarketing safety data from BOTOX Cosmetic and other approved botulinum toxins suggest that botulinum toxin effects may, in some cases, be observed beyond the site of local injection. The symptoms are consistent with the mechanism of action of botulinum toxin and may include asthenia, generalized muscle weakness, diplopia, ptosis, dysphagia, dysphonia, dysarthria, urinary incontinence, and breathing difficulties. These symptoms have been reported hours to weeks after injection. Swallowing and breathing difficulties can be life threatening and there have been reports of death related to spread of toxin effects. The risk of symptoms is probably greatest in children treated for spasticity but symptoms can also occur in adults treated for spasticity and other conditions, and particularly in those patients who have an underlying condition that would predispose them to these symptoms. In unapproved uses and in approved indications, symptoms consistent with spread of toxin effect have been reported at doses comparable to or lower than doses used to treat cervical dystonia and spasticity. Advise patients or caregivers to seek immediate medical care if swallowing, speech or respiratory disorders occur.
No definitive serious adverse event reports of distant spread of toxin effect associated with dermatologic use of BOTOX/BOTOX Cosmetic at the labeled dose of 20 Units (for glabellar lines), 24 Units (for lateral canthal lines), 40 Units (for forehead lines with glabellar lines), 44 Units (for simultaneous treatment of lateral canthal lines and glabellar lines), 64 Units (for simultaneous treatment of lateral canthal lines, glabellar lines, and forehead lines), or 100 Units (for severe primary axillary hyperhidrosis) have been reported.
No definitive serious adverse event reports of distant spread of toxin effect associated with BOTOX for blepharospasm at the recommended dose (30 Units and below), strabismus, or chronic migraine at the labeled doses have been reported.
5.3 Serious Adverse Reactions with Unapproved Use
Serious adverse reactions, including excessive weakness, dysphagia, and aspiration pneumonia, with some adverse reactions associated with fatal outcomes, have been reported in patients who received BOTOX injections for unapproved uses. In these cases, the adverse reactions were not necessarily related to distant spread of toxin, but may have resulted from the administration of BOTOX to the site of injection and/or adjacent structures. In several of the cases, patients had pre-existing dysphagia or other significant disabilities. There is insufficient information to identify factors associated with an increased risk for adverse reactions associated with the unapproved uses of BOTOX. The safety and effectiveness of BOTOX for unapproved uses have not been established.
5.4 Hypersensitivity Reactions
Serious and/or immediate hypersensitivity reactions have been reported. These reactions include anaphylaxis, serum sickness, urticaria, soft tissue edema, and dyspnea. If such a reaction occurs, discontinue further injection of BOTOX Cosmetic and immediately institute appropriate medical therapy. One fatal case of anaphylaxis has been reported in which lidocaine was used as the diluent, and consequently the causal agent cannot be reliably determined.
5.5 Cardiovascular System
There have been reports following administration of BOTOX/BOTOX Cosmetic of adverse events involving the cardiovascular system, including arrhythmia and myocardial infarction, some with fatal outcomes. Some of these patients had risk factors including pre-existing cardiovascular disease. Use caution when administering to patients with pre-existing cardiovascular disease.
5.6 Increased Risk of Clinically Significant Effects with Pre-Existing Neuromuscular Disorders
Patients with neuromuscular disorders may be at increased risk of clinically significant effects including generalized muscle weakness, diplopia, ptosis, dysphonia, dysarthria, severe dysphagia and respiratory compromise from onabotulinumtoxinA [see Warnings and Precautions (5.2, 5.7)]. Monitor individuals with peripheral motor neuropathic diseases, amyotrophic lateral sclerosis or neuromuscular junction disorders (e.g., myasthenia gravis or Lambert-Eaton syndrome) when given botulinum toxin.
5.7 Dysphagia and Breathing Difficulties
Treatment with BOTOX and other botulinum toxin products can result in swallowing or breathing difficulties. Patients with pre-existing swallowing or breathing difficulties may be more susceptible to these complications. In most cases, this is a consequence of weakening of muscles in the area of injection that are involved in breathing or oropharyngeal muscles that control swallowing or breathing [see Warnings and Precautions (5.2)].
Deaths as a complication of severe dysphagia have been reported after treatment with botulinum toxin. Dysphagia may persist for several months, and require use of a feeding tube to maintain adequate nutrition and hydration. Aspiration may result from severe dysphagia and is a particular risk when treating patients in whom swallowing or respiratory function is already compromised.
Treatment with botulinum toxins may weaken neck muscles that serve as accessory muscles of ventilation. This may result in a critical loss of breathing capacity in patients with respiratory disorders who may have become dependent upon these accessory muscles. There have been postmarketing reports of serious breathing difficulties, including respiratory failure.
Patients with smaller neck muscle mass and patients who require bilateral injections into the sternocleidomastoid muscle for the treatment of cervical dystonia have been reported to be at greater risk for dysphagia. Limiting the dose injected into the sternocleidomastoid muscle may reduce the occurrence of dysphagia. Injections into the levator scapulae may be associated with an increased risk of upper respiratory infection and dysphagia.
Patients treated with botulinum toxin may require immediate medical attention should they develop problems with swallowing, speech or respiratory disorders. These reactions can occur within hours to weeks after injection with botulinum toxin [see Warnings and Precautions (5.2)].
5.8 Pre-existing Conditions at the Injection Site
Use caution when BOTOX Cosmetic treatment is used in the presence of inflammation at the proposed injection site(s), ptosis, or when excessive weakness or atrophy is present in the targeted muscle(s).
5.9 Corneal Exposure and Ulceration in Patients Treated with BOTOX for Blepharospasm
Reduced blinking from injection of botulinum toxin products in or near the orbicularis oculi muscle can lead to corneal exposure, persistent corneal epithelial defect, and corneal ulceration, especially in patients with VII nerve disorders.
Employ vigorous treatment of any corneal epithelial defect. This may require protective drops, ointment, therapeutic soft contact lenses, or closure of the eye by patching or other means.
5.10 Dry Eye in Patients Treated with BOTOX Cosmetic
There have been reports of dry eye associated with BOTOX Cosmetic injection in or near the orbicularis oculi muscle. If symptoms of dry eye (e.g., eye irritation, photophobia, or visual changes) persist, consider referring patients to an ophthalmologist [see Warnings and Precautions (5.9)].
5.11 Spatial Disorientation, Double Vision or Past-Pointing in Patients Treated for Strabismus
Inducing paralysis in one or more extraocular muscles may produce spatial disorientation, double vision or past pointing. Covering the affected eye may alleviate these symptoms.
5.12 Human Albumin and Transmission of Viral Diseases
This product contains albumin, a derivative of human blood. Based on effective donor screening and product manufacturing processes, it carries a remote risk for transmission of viral diseases and variant Creutzfeldt-Jakob disease (vCJD). There is a theoretical risk for transmission of Creutzfeldt-Jakob disease (CJD), which would also be considered remote. No cases of transmission of viral diseases, CJD or vCJD have ever been identified for licensed albumin or albumin contained in other licensed products.
6. Adverse Reactions/Side Effects
The following adverse reactions to BOTOX Cosmetic (onabotulinumtoxinA) for injection are discussed in greater detail in other sections of the labeling:
- Spread of Toxin Effects [see Warnings and Precautions (5.2)]
- Hypersensitivity [see Contraindications (4.1) and Warnings and Precautions (5.4)]
- Dysphagia and Breathing Difficulties [see Warnings and Precautions (5.7)]
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, the adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
BOTOX and BOTOX Cosmetic contain the same active ingredient in the same formulation, but have different labeled Indications and Usage. Therefore, adverse events observed with the use of BOTOX also have the potential to be observed with the use of BOTOX Cosmetic.
In general, adverse reactions occur within the first week following injection of BOTOX Cosmetic and while in many cases are transient, may have a duration of several months or longer. Localized pain, infection, inflammation, tenderness, swelling, erythema, and/or bleeding/bruising may be associated with the injection. Needle-related pain and/or anxiety may result in vasovagal responses (including e.g., syncope, hypotension), which may require appropriate medical therapy.
Local weakness of the injected muscle(s) represents the expected pharmacological action of botulinum toxin. However, weakness of nearby muscles may also occur due to spread of toxin [see Warnings and Precautions (5.2)].
Glabellar Lines
Table 5 lists selected adverse reactions reported by ≥1% of BOTOX Cosmetic treated subjects (N=405) aged 18 to 75 who were evaluated in the randomized, placebo-controlled clinical studies to assess the use of BOTOX Cosmetic in the improvement of the appearance of glabellar lines.
| Adverse Reactions by System Organ Class | BOTOX Cosmetic
(N=405) | Placebo
(N=130) |
| General Disorders and Administration Site Conditions Facial pain | 6 (1%) | 0 (0%) |
| Nervous System Disorders Facial paresis | 5 (1%) | 0 (0%) |
| Eye Disorders Eyelid ptosis | 13 (3%) | 0 (0%) |
| Musculoskeletal and Connective Tissue Disorders Muscular Weakness | 6 (1%) | 0 (0%) |
Lateral Canthal Lines
Table 6 lists selected adverse reactions reported within 90 days following injection by ≥1% of BOTOX Cosmetic treated subjects (N=526) aged 18 to 75 who were evaluated in two randomized, double-blind, placebo-controlled clinical studies to assess the use of BOTOX Cosmetic in the improvement of the appearance of lateral canthal lines alone.
| Adverse Reactions by System Organ Class | BOTOX Cosmetic 24 Units
(N=526) | Placebo
(N=530) |
| Eye disorders Eyelid edema |
5 (1%) |
0 (0%) |
Forehead Lines
Table 7 lists selected adverse reactions reported by ≥1% of BOTOX Cosmetic treated subjects (N=665) aged 18 to 77 who were evaluated in two randomized, double-blind, placebo-controlled clinical studies to assess the use of BOTOX Cosmetic in the improvement of the appearance of forehead lines with glabellar lines.
| Adverse Reactions by System Organ Class | BOTOX Cosmetic
(20 Units forehead lines with 20 Units glabellar lines) (N=665) | Placebo
(N=315) |
| Nervous System Disorders Headache | 58 (9%) | 17 (5%) |
| Eye Disorders Eyelid ptosis | 12 (2%) | 1 (0%) |
| Skin and Subcutaneous Tissue Disorders Brow ptosis Skin tightness | 13 (2%) 10 (2%) | 0 (0%) 0 (0%) |
There were no additional adverse drug reactions reported with the simultaneous treatment of forehead lines, glabellar lines, and lateral canthal lines.
Platysma Bands
The safety of BOTOX Cosmetic (26 Units, 31 Units, or 36 Units) was evaluated in two double-blind, placebo-controlled, clinical trials with 407 BOTOX Cosmetic-treated subjects and 425 subjects receiving placebo.
The safety profile of BOTOX Cosmetic treatment of platysma bands is consistent with the known safety profile of BOTOX Cosmetic for other indications.
6.2 Postmarketing Experience
Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
There have been spontaneous reports of death, sometimes associated with dysphagia, pneumonia, and/or other significant debility or anaphylaxis, after treatment with botulinum toxin [see Warnings and Precautions (5.4, 5.7)].
There have also been reports of adverse events involving the cardiovascular system, including arrhythmia and myocardial infarction, some with fatal outcomes. Some of these patients had risk factors including cardiovascular disease.
New onset or recurrent seizures have also been reported, typically in patients who are predisposed to experiencing these events.
The following adverse reactions by System Organ Class have been identified during post-approval use of BOTOX/BOTOX Cosmetic:
Ear and labyrinth disorders
Hypoacusis; tinnitus; vertigo
Eye disorders
Diplopia; dry eye; eyelid edema; lagophthalmos; strabismus; visual disturbances; vision blurred
Gastrointestinal disorders
Abdominal pain; diarrhea; dry mouth; nausea; vomiting
General disorders and administration site conditions
Denervation; malaise; pyrexia
Metabolism and nutrition disorders
Anorexia
Musculoskeletal and connective tissue disorders
Localized muscle twitching/involuntary muscle contractions; Mephisto sign; muscle atrophy; myalgia
Nervous system disorders
Brachial plexopathy; dysarthria; facial palsy; hypoaesthesia; localized numbness; myasthenia gravis; paresthesia; peripheral neuropathy; radiculopathy; syncope
Respiratory, thoracic and mediastinal disorders
Aspiration pneumonia; dyspnea; respiratory depression and/or respiratory failure
Skin and subcutaneous tissue disorders
Alopecia, including madarosis; hyperhidrosis; pruritus; skin rash (including erythema multiforme, dermatitis psoriasiform, and psoriasiform eruption)
Related/similar drugs
7. Drug Interactions
No formal drug interaction studies have been conducted with BOTOX Cosmetic (onabotulinumtoxinA) for injection.
7.1 Aminoglycosides and Other Agents Interfering with Neuromuscular Transmission
Co-administration of BOTOX Cosmetic and aminoglycosides or other agents interfering with neuromuscular transmission (e.g., curare-like compounds) should only be performed with caution as the effect of the toxin may be potentiated.
7.2 Anticholinergic Drugs
Use of anticholinergic drugs after administration of BOTOX Cosmetic may potentiate systemic anticholinergic effects.
7.3 Other Botulinum Neurotoxin Products
The effect of administering different botulinum neurotoxin products at the same time or within several months of each other is unknown. Excessive neuromuscular weakness may be exacerbated by administration of another botulinum toxin prior to the resolution of the effects of a previously administered botulinum toxin.
8. Use In Specific Populations
8.1 Pregnancy
Risk Summary
There are no studies or adequate data from postmarketing surveillance on the developmental risk associated with use of BOTOX Cosmetic in pregnant women.
In animal studies, administrations of BOTOX Cosmetic during pregnancy resulted in adverse effects on fetal growth (decreased fetal body weight and skeletal ossification) at clinically relevant doses, which were associated with maternal toxicity [see Data].
The background risk of major birth defects and miscarriage for the indicated populations is unknown. All pregnancies have a background risk of birth defect, loss or other adverse outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriages in clinically recognized pregnancies is 2-4% and 15-20%, respectively.
Data
Animal Data
When BOTOX Cosmetic (4, 8, or 16 Units/kg) was administered intramuscularly to pregnant mice or rats two times during the period of organogenesis (on gestation days 5 and 13), reductions in fetal body weight and decreased fetal skeletal ossification were observed at the two highest doses. The no-effect dose for developmental toxicity in these studies (4 Units/kg) is approximately 4 times the average high human dose for glabellar lines, lateral canthal lines, and forehead lines of 64 Units on a body weight basis (Units/kg).
When BOTOX Cosmetic was administered intramuscularly to pregnant rats (0.125, 0.25, 0.5, 1, 4, or 8 Units/kg) or rabbits (0.063, 0.125, 0.25, or 0.5 Units/kg) daily during the period of organogenesis (total of 12 doses in rats, 13 doses in rabbits), reduced fetal body weights and decreased fetal skeletal ossification were observed at the two highest doses in rats and at the highest dose in rabbits. These doses were also associated with significant maternal toxicity, including abortions, early deliveries, and maternal death. The developmental no-effect doses in these studies of 1 Unit/kg in rats is approximately equal the average high human dose of 64 Units based on Units/kg, and the developmental no-effect dose of 0.25 Units/kg in rabbits is less than the average high human dose based on Units/kg.
When pregnant rats received single intramuscular injections (1, 4, or 16 Units/kg) at three different periods of development (prior to implantation, implantation, or organogenesis), no adverse effects on fetal development were observed. The developmental no-effect level for a single maternal dose in rats (16 Units/kg) is approximately 16 times the average high human dose of 64 Units based on Units/kg.
8.2 Lactation
Risk Summary
There are no data on the presence of BOTOX Cosmetic in human or animal milk, the effects on the breastfed child, or the effects on milk production.
The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for BOTOX Cosmetic and any potential adverse effects on the breastfed infant from BOTOX Cosmetic or from the underlying maternal conditions.
8.4 Pediatric Use
The safety and effectiveness of BOTOX Cosmetic have not been established in pediatric patients.
8.5 Geriatric Use
Glabellar Lines
In the two initial glabellar lines clinical studies of BOTOX Cosmetic, the responder rates appeared to be higher for subjects younger than age 65 than for subjects 65 years or older [see Clinical Studies (14)].
Lateral Canthal Lines
In the two lateral canthal lines clinical studies of BOTOX Cosmetic, the responder rates appeared to be higher for subjects younger than age 65 than for subjects 65 years or older.
Forehead Lines
In the two forehead lines clinical studies of BOTOX Cosmetic, the responder rates appeared to be higher for subjects younger than age 65 than for subjects 65 years or older.
Platysma Bands
In the two platysma bands clinical studies of BOTOX Cosmetic, 3.6% of subjects (13 subjects) treated with BOTOX Cosmetic were 65 years or older. Although the responder rates appeared to be higher for subjects younger than age 65 than for subjects 65 years or older, clinical studies of BOTOX Cosmetic did not include sufficient numbers of subjects 65 years or older to determine whether they respond differently from younger subjects.
10. Overdosage
Excessive doses of BOTOX Cosmetic (onabotulinumtoxinA) for injection may be expected to produce neuromuscular weakness with a variety of symptoms.
Symptoms of overdose are likely not to be present immediately following injection. Should accidental injection or oral ingestion occur or overdose be suspected, consider patients for further medical evaluation and immediately institute appropriate medical therapy, which may include hospitalization. The patient should be medically supervised for several weeks for signs and symptoms of systemic muscular weakness which could be local, or distant from the site of injection [see Boxed Warning and Warnings and Precautions (5.2, 5.7)].
If the musculature of the oropharynx and esophagus are affected, aspiration may occur which may lead to development of aspiration pneumonia. If the respiratory muscles become paralyzed or sufficiently weakened, intubation and assisted respiration may be necessary until recovery takes place. Supportive care could involve the need for a tracheostomy and/or prolonged mechanical ventilation, in addition to other general supportive care.
In the event of overdose, antitoxin raised against botulinum toxin is available from the Centers for Disease Control and Prevention (CDC) in Atlanta, GA. However, the antitoxin will not reverse any botulinum toxin-induced effects already apparent by the time of antitoxin administration. In the event of suspected or actual cases of botulinum toxin poisoning, please contact your local or state Health Department to process a request for antitoxin through the CDC. If you do not receive a response within 30 minutes, please contact the CDC directly at 1-770-488-7100. More information can be obtained at http://www.cdc.gov/mmwr/preview/mmwrhtml/mm5232a8.htm.
11. Botox Cosmetic Description
BOTOX Cosmetic (onabotulinumtoxinA) for injection, is a sterile, vacuum-dried purified botulinum toxin type A, produced from fermentation of Hall strain Clostridium botulinum type A intended for intramuscular use. It is purified from the culture solution by dialysis and a series of acid precipitations to a complex consisting of the neurotoxin, and several accessory proteins. The complex is dissolved in sterile sodium chloride solution containing Albumin Human and is sterile filtered (0.2 microns) prior to filling and vacuum-drying.
The primary release procedure for BOTOX Cosmetic uses a cell-based potency assay to determine the potency relative to a reference standard. The assay is specific to AbbVie’s products BOTOX and BOTOX Cosmetic. One Unit of BOTOX Cosmetic corresponds to the calculated median intraperitoneal lethal dose (LD50) in mice. Due to specific details of this assay such as the vehicle, dilution scheme and laboratory protocols, Units of biological activity of BOTOX Cosmetic cannot be compared to nor converted into Units of any other botulinum toxin or any toxin assessed with any other specific assay method. The specific activity of BOTOX Cosmetic is approximately 20 Units/nanogram of neurotoxin complex.
Each vial of BOTOX Cosmetic contains either 50 Units of Clostridium botulinum type A neurotoxin complex, 0.25 mg of Albumin Human, and 0.45 mg of sodium chloride; or 100 Units of Clostridium botulinum type A neurotoxin complex, 0.5 mg of Albumin Human, and 0.9 mg of sodium chloride in a sterile, vacuum-dried form without a preservative.
12. Botox Cosmetic - Clinical Pharmacology
12.1 Mechanism of Action
BOTOX Cosmetic blocks neuromuscular transmission by binding to acceptor sites on motor nerve terminals, entering the nerve terminals, and inhibiting the release of acetylcholine. This inhibition occurs as the neurotoxin cleaves SNAP-25, a pre-synaptic protein integral to the successful docking and release of acetylcholine from vesicles situated within nerve endings. When injected intramuscularly at therapeutic doses, BOTOX Cosmetic produces partial chemical denervation of the muscle resulting in a localized reduction in muscle activity. In addition, the muscle may atrophy, axonal sprouting may occur, and extrajunctional acetylcholine receptors may develop. There is evidence that reinnervation of the muscle may occur, thus slowly reversing muscle denervation produced by BOTOX Cosmetic.
12.2 Pharmacodynamics
No formal pharmacodynamic studies have been conducted with BOTOX Cosmetic (onabotulinumtoxinA) for injection.
12.3 Pharmacokinetics
Using currently available analytical technology, it is not possible to detect BOTOX Cosmetic in the peripheral blood following intramuscular injection at the recommended doses.
12.6 Immunogenicity
Since BOTOX Cosmetic is a therapeutic protein, there is a potential for immunogenicity. The detection of antibody formation is highly dependent on the sensitivity and specificity of the assay. Additionally, the observed incidence of antibody (including neutralizing antibody) positivity in an assay may be influenced by several factors including assay methodology, sample handling, timing of sample collection, concomitant medications, and underlying disease. For these reasons, comparison of the incidence of antibodies to BOTOX Cosmetic in the studies described below with the incidence of antibodies in other studies or to other products may be misleading.
In three Lateral Canthal Line trials, 916 subjects (517 subjects at 24 Units and 399 subjects at 44 Units) treated with BOTOX Cosmetic had specimens analyzed for antibody formation. Among the 916 BOTOX Cosmetic treated subjects, 14 subjects (1.5%) developed binding antibodies and no subjects (0%) developed the presence of neutralizing antibodies.
The data reflect the subjects whose test results were considered positive or negative for neutralizing activity to BOTOX Cosmetic in a mouse protection assay.
The critical factors for neutralizing antibody formation have not been well characterized. The results from some studies suggest that botulinum toxin injections at more frequent intervals or at higher doses may lead to greater incidence of antibody formation. The potential for antibody formation may be minimized by injecting with the lowest effective dose given at the longest feasible intervals between injections.
13. Nonclinical Toxicology
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Long term studies in animals have not been performed to evaluate carcinogenic potential of BOTOX Cosmetic.
BOTOX Cosmetic was negative in a battery of in vitro (microbial reverse mutation assay, mammalian cell mutation assay, and chromosomal aberration assay) and in vivo (micronucleus assay) genetic toxicologic assays.
In fertility studies of BOTOX Cosmetic (4, 8, or 16 Units/kg) in which either male or female rats were injected intramuscularly prior to mating and on the day of mating (3 doses, 2 weeks apart for males, 2 doses, 2 weeks apart for females) to untreated animals, reduced fertility was observed in males at the intermediate and high doses and in females at the high dose. The no-effect doses for reproductive toxicity (4 Units/kg in males, 8 Units/kg in females) are approximately 4-8 times the average high human dose for glabellar lines, lateral canthal lines, and forehead lines of 64 Units on a body weight basis (Units/kg).
14. Clinical Studies
14.1 Glabellar Lines
Two randomized, multi-center, double-blind, placebo-controlled studies of identical design were conducted to evaluate BOTOX Cosmetic for use in the temporary improvement of the appearance of moderate to severe glabellar facial lines. The studies enrolled healthy adults (ages 18 to 75) with glabellar lines of at least moderate severity at maximum frown. Subjects were excluded if they had ptosis, deep dermal scarring, or an inability to substantially lessen glabellar lines even by physically spreading them apart. Subjects received a single treatment with BOTOX Cosmetic (N=405, combined studies) or placebo (N=132, combined studies). Injection volume was 0.1 mL/injection site, for a dose/injection site in the active treatment groups of 4 Units. Subjects were injected intramuscularly in five sites, 1 in the procerus muscle and 2 in each corrugator supercilii muscle, for a total dose in the active treatment groups of 20 Units.
The co-primary efficacy endpoints were the investigator’s rating of glabellar line severity at maximum frown and the subject’s global assessment of change in appearance of glabellar lines, both at Day 30 post-injection. For the investigator rating, using a 4-point grading scale (0=none, 3=severe) a responder was defined as having a severity grade of 0 or 1. For the subject’s global assessment of change, the ratings were from +4 (complete improvement) to -4 (very marked worsening). A responder was defined as having a grade of at least +2 (moderate improvement). After completion of the randomized studies, subjects were offered participation in an open label, repeat treatment study to assess the safety of repeated treatment sessions.
The combined results of these two efficacy studies are presented here. The mean age was 46 years, with 32 subjects (6%) ≥65 years of age. Most of the subjects were women (82%), and White (84%). At baseline, 210 subjects (39%) had glabellar line severity scores at rest of moderate or severe.
In these studies, the severity of glabellar lines was reduced for up to 120 days in the BOTOX Cosmetic group compared to the placebo group as measured both by investigator rating of glabellar line severity at maximum frown (Table 8), and by subject’s global assessment of change in appearance of glabellar lines (Table 9).
| Day | BOTOX
Cosmetic | Placebo | Differencea |
| 7 | 74% 299/405 | 6% 8/132 | 68% (62, 74) |
| 30b | 80% 325/405 | 3% 4/132 | 77% (72, 82) |
| 60 | 70% 283/403 | 2% 2/130 | 69% (64, 74) |
| 90 | 48% 192/403 | 2% 3/128 | 45% (40, 51) |
| 120 | 25% 102/403 | 2% 2/128 | 24% (19, 29) |
a 95% confidence intervals are shown in parenthesis
b Day 30: Co-Primary Efficacy Time point, p<0.001
| Day | BOTOX Cosmetic | Placebo | Differencea |
| 7 | 82% 334/405 | 9% 12/132 | 73% (68, 80) |
| 30b | 89% 362/405 | 7% 9/132 | 83% (77, 88) |
| 60 | 82% 330/403 | 4% 5/130 | 78% (73, 83) |
| 90 | 63% 254/403 | 3% 4/128 | 60% (54, 66) |
| 120 | 39% 157/403 | 1% 1/128 | 38% (33, 43) |
a 95% confidence intervals are shown in parenthesis
b Day 30: Co-Primary Efficacy Time point, p<0.001
In the subset of subjects with resting severity scores of moderate or severe, the investigator assessment of a resting severity of mild or none at Day 30 was also achieved by more BOTOX Cosmetic treated subjects (74%, 119/161) than placebo treated subjects (20%, 10/49).
Analysis of the limited number of subjects 65 years or older suggested a lower treatment-associated response compared to subjects less than 65 years of age (Table 10).
| Assessment | Age Group | BOTOX Cosmetic (N=405) | Placebo (N=132) | Differencea |
| Investigators (maximal frown) | <65 | 83% 316/382 | 2% 2/123 | 81% (77, 86) |
| Subjects | <65 | 91% 346/382 | 7% 8/123 | 84% (79, 90) |
| Investigators (maximal frown) | ≥65 | 39% 9/23 | 22% 2/9 | 17% (-17, 51) |
| Subjects | ≥65 | 70% 16/23 | 11% 1/9 | 58% (31, 86) |
a 95% confidence intervals are shown in parenthesis
Exploratory analyses by gender suggested that responder rates in the BOTOX Cosmetic treated group were higher for women than for men for both the investigator assessment (Day 30; 85% of 334 women, 59% of 71 men) and the Subject Assessment (Day 30; 93% of women, 72% of men). In the limited number of subjects that identified as other races (n=64 in the BOTOX Cosmetic treated group) the responder rates were similar to those observed in White subjects.
14.2 Lateral Canthal Lines
Two multicenter, randomized, double-blind, placebo-controlled studies evaluated BOTOX Cosmetic (N=833, randomized to receive any BOTOX Cosmetic treatment or N=529 randomized to receive placebo) for the temporary improvement in the appearance of moderate to severe lateral canthal lines (LCL). Study 1 assessed BOTOX Cosmetic treatment of LCL alone; Study 2 also assessed simultaneous treatment of LCL and glabellar lines (GL). Both studies enrolled healthy adults with moderate to severe LCL at maximum smile at baseline; Study 2 also required subjects to have moderate to severe GL at maximum frown at baseline.
In the 5-month Study 1, subjects were randomized to receive a single blinded treatment of 24 Units/0.6 mL (12 Units per side) consisting of 4 Units/0.1 mL into 3 sites of each orbicularis oculi muscle with either BOTOX Cosmetic (N=222) or placebo (N=223).
In the 7-month Study 2, subjects were randomized to receive either BOTOX Cosmetic in the LCL region and placebo in the GL region (24 Units; N=306), or BOTOX Cosmetic in the LCL and GL regions (44 Units [24 Units for LCL and 20 Units for GL]; N=305), or placebo in the LCL and GL regions (0 Units; N=306). Subjects received the same 24 Units regimen for LCL as in Study 1, and the labeled 20 Units (5 injections, 4 Units per site) for GL. Subjects received the same treatment at days 1 and 120.
The primary efficacy measure was the assessment of LCL severity at maximum smile using the 4-point Facial Wrinkle Scale with Photonumeric Guide (FWS; 0=none, 1= mild, 2=moderate, 3=severe). The FWS assessment was performed independently by both investigators and subjects. The primary timepoint was day 30 following the first treatment, as compared to baseline.
The primary efficacy response definition was a composite ≥2-grade improvement from baseline in LCL severity at maximum smile, assessed by both investigator and subject on a per-subject basis. For Studies 1 and 2, the proportion of responders was statistically significant favoring BOTOX Cosmetic (24 Units [LCL alone] and 44 Units [LCL and GL]) compared to placebo at day 30 (Table 11).
| Study | BOTOX
Cosmetic 24 Units | BOTOX
Cosmetic 24 Units LCL and 20 Units GL | Placebo |
| Study 1 | 26.1% 58/222 | - | 1.3% 3/223 |
| Study 2 | 20.3% 62/306 | 21.3% 65/305 | 0.0% 0/306 |
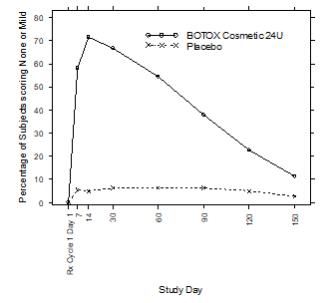
The secondary endpoint of a responder defined as achieving a grade of none or mild for Study 1 as measured by the investigator is presented in Figure 7 below.
Figure 7: Percentage of Subjects with Treatment Success (% of Subjects achieving None or Mild from Baseline) by Visit (Study 1)
14.3 Forehead Lines
Two multicenter, randomized, double-blind, placebo-controlled studies evaluated BOTOX Cosmetic (N=921, randomized to receive any BOTOX Cosmetic treatment or N=257, randomized to receive placebo) for the temporary improvement in the appearance of moderate to severe forehead lines (FHL).
Study 1 assessed BOTOX Cosmetic treatment of FHL with glabellar lines (GL); Study 2 also assessed simultaneous treatment of FHL, GL, and lateral canthal lines [LCL]. Both studies enrolled healthy adults with moderate to severe FHL at maximum eyebrow elevation at baseline and moderate to severe GL at maximum frown at baseline; Study 2 also required subjects to have moderate to severe LCL at maximum smile at baseline.
In the 12-month Study 1, subjects were randomized to receive BOTOX Cosmetic 20 Units to the frontalis muscle with 20 Units to the glabellar region (for a total of 40 Units) or placebo in both areas.
In the 12-month Study 2, subjects were randomized to receive BOTOX Cosmetic 20 Units to the frontalis muscle, 20 Units to the glabellar region, and 0 Units to the LCL region (for a total of 40 units) or BOTOX Cosmetic 20 Units to the frontalis muscle, 20 Units to the glabellar region, and 24 Units to the LCL region (for a total of 64 Units) or placebo in all three areas.
The primary efficacy measure was the assessment of FHL severity at maximum eyebrow elevation using the 4-point Facial Wrinkle Scale with Photonumeric Guide (FWS; 0=none, 1= mild, 2=moderate, 3=severe). The FWS assessment was performed independently by both investigators and subjects. The primary timepoint was Day 30 following the first treatment.
The primary efficacy response definition was a composite ≥2-grade improvement from baseline in FHL severity at maximum eyebrow elevation, assessed by both investigator and subject on a per-subject basis. For Studies 1 and 2, the proportion of responders was greater in the BOTOX Cosmetic arms compared to placebo at Day 30 (p<0.0001 for Studies 1 and 2) (Table 12).
| Study | BOTOX Cosmetic (20 Units FHL with 20 Units GL) | BOTOX Cosmetic (20 Units FHL,
20 Units GL, and 24 Units LCL) | Placebo |
| Study 1 | N=290 61% | - | N=101 0% |
| Study 2 | N=318 46% | N=313 53% | N=156 1% |
A total of 165 and 197 subjects received 3 cycles over 1 year of BOTOX Cosmetic 40 Units (20 Units FHL with 20 Units GL) and 64 Units (20 Units FHL, 20 Units GL, and 24 Units LCL), respectively. The response rate for FHL was similar across all treatment cycles.
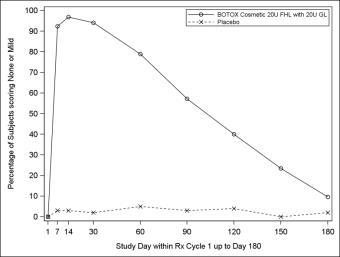
The results for a key secondary endpoint of responders achieving a grade of none or mild on investigator ratings at maximum eyebrow elevation of FHL severity are presented below for Studies 1 and 2.
Figure 8: Percentage of Subjects with Treatment Success (Achieving None or Mild FHL from Baseline at Maximum Eyebrow Elevation) by Visit (Study 1)

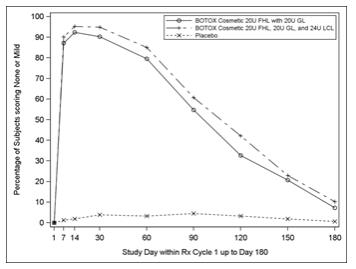
Figure 9: Percentage of Subjects with Treatment Success (Achieving None or Mild FHL from Baseline at Maximum Eyebrow Elevation) by Visit (Study 2)
The results of the Facial Line Satisfaction Questionnaire are presented in Table 13.
| Study 1 | Study 2 | |||
| BOTOX
Cosmetic (20 Units FHL with 20 Units GL) N=289 | Placebo
N=99 | BOTOX
Cosmetic (20 Units FHL with 20 Units GL) N=317 | Placebo
N=155 |
|
| “Very satisfied” | 57% | 1% | 35% | 0% |
| “Mostly satisfied” | 33% | 0% | 47% | 3% |
| “Neither dissatisfied nor satisfied” | 4% | 22% | 9% | 23% |
| “Mostly dissatisfied” | 4% | 21% | 7% | 20% |
| “Very dissatisfied” | 2% | 56% | 2% | 54% |
14.4 Platysma Bands
Two multicenter, randomized, double-blind, placebo-controlled trials (Study M21-309 [NCT04949399] and Study M21-310 [NCT04994535]) evaluated BOTOX Cosmetic (N=408 BOTOX Cosmetic and N=426 placebo) for the temporary improvement in the appearance of moderate to severe platysma bands. Based on baseline severity, subjects were randomized to receive a single treatment of BOTOX Cosmetic (26 Units, 31 Units, or 36 Units), or placebo.
The primary efficacy measure was the assessment of platysma band severity at maximum contraction using the 5-grade clinician platysma band scale by the investigators, and the 5-grade participant platysma band scale by the subjects. For both scales, the 5 grades are 1=Minimal, 2=Mild, 3=Moderate, 4=Severe, 5=Extreme (Table 14). The investigator and subject assessments were performed independently.
| Grade | Severity Description |
| 1 | Minimal; no visible neck bands and no impact to jawline definition |
| 2 | Mild; visible neck bands and no impact to jawline definition |
| 3 | Moderate; 1 visible continuous neck band impacting jawline definition |
| 4 | Severe; 2 visible continuous neck bands impacting jawline definition |
| 5 | Extreme; 3 or more visible neck bands impacting jawline definition |
The primary timepoint was Day 14 after the first treatment. The studies enrolled healthy adults with moderate to severe platysma bands. In these studies, 94% were female, 91% were White, 5% were Asian, 3% were Black or African American; for ethnicity, 86% identified as not Hispanic or Latino. Subjects were 19 to 82 years old, with a mean age of 49 years.
The primary efficacy endpoint was a multi-component endpoint defined as achievement of Grade 1 or 2 (Minimal or Mild) and at least a 2-grade improvement from baseline in platysma band severity at maximum contraction, assessed by both investigator and subject at Day 14 (Table 15).
| Study M21-309 | Study M21-310 | |||||
| BOTOX
Cosmetic 26, 31, or 36 Units (N=199) | Placebo
(N=209) | Differenced | BOTOX
Cosmetic 26, 31, or 36 Units (N=209) | Placebo
(N=217) | Differenced | |
| Multi-component Assessmenta | 32% | 2% | 30% (24%, 37%) | 31% | 0% | 31% (24%, 37%) |
| Individual Components | ||||||
| Investigator Assessmentb | 45% | 4% | - | 42% | 2% | - |
| Subject Assessmentc | 44% | 4% | - | 40% | 3% | - |
- Grade 1 or 2 (Minimal or Mild) and ≥ 2-grade improvement from baseline at maximum contraction on both the investigator and subject assessments at Day 14.
- Grade 1 or 2 (Minimal or Mild) and ≥ 2-grade improvement from baseline at maximum contraction on the investigator assessment at Day 14.
- Grade 1 or 2 (Minimal or Mild) and ≥ 2-grade improvement from baseline at maximum contraction on the subject assessment at Day 14.
- 95% confidence intervals are shown in parentheses.
The percentages of subjects achieving these endpoints over time are shown in Figure 10 (Study M21-309) and Figure 11 (Study M21-310).
Figure 10: Percentages of Subjects Achieving a Grade 1 or 2 (Minimal or Mild) and at Least 2-Grade Improvement from Baseline Based on Both the Investigator and Subject Assessments of Platysma Band Severity at Maximum Contraction Over Time (Study M21-309)
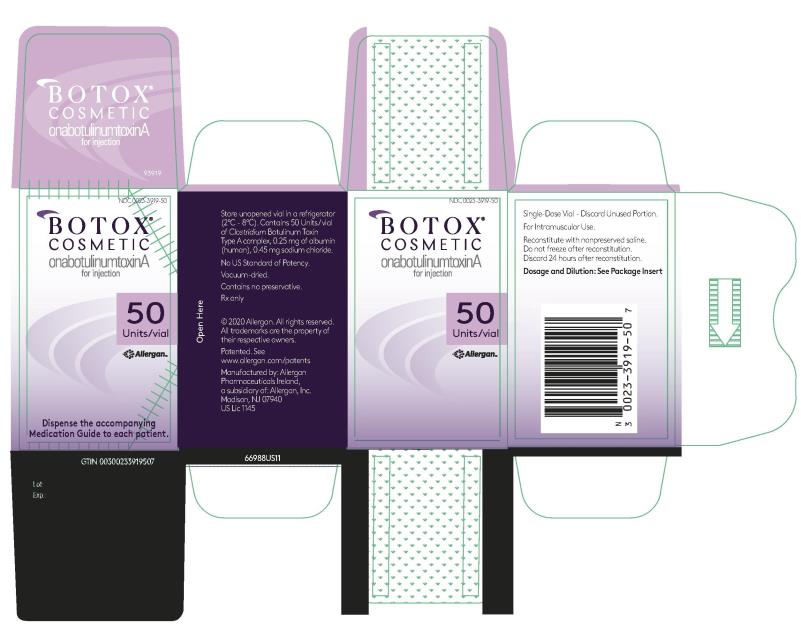
Figure 11: Percentages of Subjects Achieving a Grade 1 or 2 (Minimal or Mild) and at Least 2-Grade Improvement from Baseline Based on Both the Investigator and Subject Assessments of Platysma Band Severity at Maximum Contraction Over Time (Study M21-310)

The results for Appearance of Neck and Lower Face Questionnaire: Satisfaction (Follow-up) Item 5 at Day 14 secondary efficacy endpoints are presented for Studies M21-309 and M21-310 in Table 16.
| Responses | Study M21-309 | Study M21-310 | ||
| BOTOX Cosmetic
26, 31, or 36 Units (N = 199) | Placebo
(N = 209) | BOTOX Cosmetic
26, 31, or 36 Units (N = 209) | Placebo
(N = 217) |
|
| “Very satisfied” | 31% | 3% | 22% | 2% |
| “Satisfied” | 34% | 9% | 40% | 10% |
| “Neither satisfied nor dissatisfied” | 25% | 31% | 25% | 32% |
| “Dissatisfied” | 7% | 34% | 10% | 29% |
| “Very dissatisfied” | 2% | 24% | 3% | 27% |
16. How is Botox Cosmetic supplied
BOTOX Cosmetic (onabotulinumtoxinA) for injection is a vacuum-dried powder supplied in a single-dose vial in the following sizes:
50 Units: NDC 0023-3919-50
100 Units: NDC 0023-9232-01
BOTOX Cosmetic cartons have features to alert users if contents may have been compromised. Each BOTOX Cosmetic vial label and carton labeling also contain the U.S. License number 1889 [see Dosage and Administration (2.1)].
Do not use the product and contact AbbVie for additional information at 1-800-678-1605 if the labeling is not as described above.
Storage
Store unopened vials of BOTOX Cosmetic in a refrigerator 2°C to 8°C (36ºF to 46ºF). Do not use after the expiration date on the vial. Store reconstituted BOTOX Cosmetic in a refrigerator 2°C to 8°C (36ºF to 46ºF) and administer within 24 hours [see Dosage and Administration (2.3)].
17. Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
Provide a copy of the Medication Guide and review the contents with the patient.
Swallowing, Speaking or Breathing Difficulties, or Other Unusual Symptoms
Advise patients to inform their doctor or pharmacist if they develop any unusual symptoms (including difficulty with swallowing, speaking, or breathing), or if any existing symptom worsens [see Boxed Warning and Warnings and Precautions (5.2, 5.7)].
Ability to Operate Machinery or Vehicles
Advise patients that if loss of strength, muscle weakness, blurred vision, or drooping eyelids occur, avoid driving a car or engaging in other potentially hazardous activities.
Ophthalmic Adverse Reactions
Inform patients that BOTOX Cosmetic injection may cause eye dryness. Advise patients to report symptoms of eye dryness (e.g., eye pain, eye irritation, photosensitivity, or changes in vision) to their doctor.
Manufactured by: AbbVie Inc.
1 N Waukegan Rd. North Chicago, IL 60064
U.S. License number 1889
© 2024 AbbVie. All rights reserved.
BOTOX and its design are trademarks of Allergan, Inc., an AbbVie company.

V4.1USPI3919
Medication Guide
| MEDICATION GUIDE
BOTOX® BOTOX® Cosmetic (Boe-tox) (onabotulinumtoxinA) for injection, for intramuscular, intradetrusor, or intradermal use |
| What is the most important information I should know about BOTOX and BOTOX Cosmetic?
BOTOX and BOTOX Cosmetic may cause serious side effects that can be life threatening, including:
Call your doctor or get medical help right away if you have any of these problems after treatment with BOTOX or BOTOX Cosmetic:
These problems could make it unsafe for you to drive a car or do other dangerous activities. See "What should I avoid while receiving BOTOX or BOTOX Cosmetic?" There has not been a confirmed serious case of spread of toxin effect away from the injection site when BOTOX has been used at the recommended dose to treat chronic migraine, severe underarm sweating, blepharospasm, or strabismus, or when BOTOX Cosmetic has been used at the recommended dose to treat frown lines, crow’s feet lines, forehead lines, or vertical bands connecting the jaw and neck. |
| What are BOTOX and BOTOX Cosmetic?
BOTOX is a prescription medicine that is injected into muscles and used:
|
BOTOX Cosmetic is a prescription medicine for adults that is injected into muscles and used for a short period of time (temporary) to improve the look of:
|
It is not known whether BOTOX is safe and effective in people younger than:
It is not known whether BOTOX and BOTOX Cosmetic are safe and effective to prevent headaches in people with migraine who have 14 or fewer headache days each month (episodic migraine). It is not known whether BOTOX and BOTOX Cosmetic are safe and effective for severe sweating anywhere other than your armpits. It is not known if BOTOX Cosmetic is safe and effective for use more than 1 time every 3 months. |
| Who should not receive BOTOX or BOTOX Cosmetic?
Do not receive BOTOX or BOTOX Cosmetic if you:
|
| What should I tell my doctor before receiving BOTOX or BOTOX Cosmetic?
Tell your doctor about all your medical conditions, including if you:
Especially tell your doctor if you:
Know the medicines you take. Keep a list of your medicines with you to show your doctor and pharmacist each time you get a new medicine. |
How will I receive BOTOX or BOTOX Cosmetic?
|
| What should I avoid while receiving BOTOX or BOTOX Cosmetic?
BOTOX and BOTOX Cosmetic may cause loss of strength or general muscle weakness, vision problems, or dizziness within hours to weeks of taking BOTOX or BOTOX Cosmetic. If this happens, do not drive a car, operate machinery, or do other dangerous activities. See "What is the most important information I should know about BOTOX and BOTOX Cosmetic?" |
| What are the possible side effects of BOTOX and BOTOX Cosmetic?
BOTOX and BOTOX Cosmetic can cause serious side effects. See "What is the most important information I should know about BOTOX and BOTOX Cosmetic?" Other side effects of BOTOX and BOTOX Cosmetic include:
These are not all the possible side effects of BOTOX and BOTOX Cosmetic. For more information, ask your doctor or pharmacist. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
| General information about the safe and effective use of BOTOX and BOTOX Cosmetic:
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. This Medication Guide summarizes the most important information about BOTOX and BOTOX Cosmetic. If you would like more information, talk with your doctor. You can ask your doctor or pharmacist for information about BOTOX and BOTOX Cosmetic that is written for health professionals. |
| What are the ingredients in BOTOX and BOTOX Cosmetic?
Active ingredient: onabotulinumtoxinA Inactive ingredients: human albumin and sodium chloride |
| Manufactured by: AbbVie Inc. 1 N Waukegan Rd. North Chicago, IL 60064 U.S. License Number 1889 © 2024 AbbVie. All rights reserved. BOTOX and its design are trademarks of Allergan, Inc., an AbbVie company. All trademarks are the property of their respective owners.   V8.0MG1145 |
This Medication Guide has been approved by the U.S. Food and Drug Administration Revised: 10/2024
| BOTOX COSMETIC
onabotulinumtoxina injection, powder, lyophilized, for solution |
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
| BOTOX COSMETIC
onabotulinumtoxina injection, powder, lyophilized, for solution |
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
| Labeler - Allergan, Inc. (144796497) |
Biological Products Related to Botox Cosmetic
Find detailed information on biosimilars for this medication.
Frequently asked questions
- Masseter Botox for Jaw Slimming: Benefits, Cost, Side Effects & Results
- Botox Vs Botox Cosmetic: What is the difference?
- What is botulinum toxin used to treat?
- Dysport vs Botox: Key Differences and Effectiveness
More about Botox Cosmetic (onabotulinumtoxinA)
- Check interactions
- Compare alternatives
- Pricing & coupons
- Reviews (12)
- Drug images
- Latest FDA alerts (3)
- Side effects
- Dosage information
- During pregnancy
- FDA approval history
- Drug class: skeletal muscle relaxants
- Breastfeeding
- En español