Aciphex Sprinkle: Package Insert / Prescribing Info
Package insert / product label
Generic name: rabeprazole sodium
Dosage form: capsules, delayed release
Medically reviewed by Drugs.com. Last updated on Feb 4, 2025.
On This Page
- Indications and Usage
- Dosage and Administration
- Dosage Forms and Strengths
- Contraindications
- Adverse Reactions/Side Effects
- Warnings and Precautions
- Drug Interactions
- Use In Specific Populations
- Overdosage
- Description
- Clinical Pharmacology
- Nonclinical Toxicology
- Clinical Studies
- How Supplied/Storage and Handling
- Storage and Handling
- Patient Counseling Information
- Medication Guide
Highlights of Prescribing Information
ACIPHEX ® SPRINKLE™ (rabeprazole sodium delayed-release capsules), for oral use
Initial U.S. Approval: 1999
Recent Major Changes
Warnings and Precautions
- Acute Tubulointerstitial Nephritis (5.3) 11/2020
Indications and Usage for Aciphex Sprinkle
ACIPHEX Sprinkle is a proton-pump inhibitor (PPI) indicated for the treatment of Gastroesophageal Reflux Disease (GERD) in pediatric patients 1 to 11 years of age ( 1).
Aciphex Sprinkle Dosage and Administration
Dosage Regimen ( 2.1) :
The recommended dosage in pediatric patients 1 to 11 years of age for up to 12 weeks is:
- Less than 15 kg: 5 mg once daily with the option to increase to 10 mg once daily, if inadequate response
- 15 kg or more: 10 mg once daily
Administration Recommendations ( 2.2) :
- Take dose 30 minutes before a meal
- Do not swallow the capsule whole
- Open an ACIPHEX Sprinkle capsule and sprinkle granule contents on a spoonful of soft food or liquid (e.g., applesauce). Food or liquid should be at or below room temperature.
- Do not chew or crush the granules
- Take entire dose within 15 minutes of preparation
Dosage Forms and Strengths
Delayed-Release Capsules: 5 mg and 10 mg ( 3).
Contraindications
Adverse Reactions/Side Effects
Most common adverse reactions (>5%) are vomiting, abdominal pain, diarrhea, headache, and nausea (6.1). (5)
(5)
To report SUSPECTED ADVERSE REACTIONS, contact Aytu Therapeutics, LLC. at 855 298-8246 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch (5)
Warnings and Precautions
- Gastric Malignancy: In adults, symptomatic response to therapy with rabeprazole does not preclude the presence of gastric malignancy. Consider additional follow-up and diagnostic testing (5.1).
- Use with Warfarin: Monitor for increases in INR and prothrombin time (5.2, 7).
- Tubulointerstitial Nephritis: Discontinue treatment and evaluate patients (5.3).
- Clostridium difficile-Associated Diarrhea: PPI therapy may be associated with increased risk (5.4).
- Bone Fracture: Long-term and multiple daily dose PPI therapy may be associated with an increased risk for osteoporosis-related fractures of the hip, wrist, or spine (5.5).
- Cutaneous and Systemic Lupus Erythematosus: Mostly cutaneous; new onset or exacerbation of existing disease; discontinue ACIPHEX Sprinkle and refer to specialist for evaluation (5.6).
- Cyanocobalamin (Vitamin B-12) Deficiency: Daily long-term use (e.g., longer than 3 years) may lead to malabsorption or a deficiency of cyanocobalamin (5.7).
- Hypomagnesemia: Reported rarely with prolonged treatment with PPIs (5.8).
- Interaction with Methotrexate: Concomitant use with PPIs may elevate and/or prolong serum concentrations of methotrexate and/or its metabolite, possibly leading to toxicity. With high dose methotrexate administration, consider a temporary withdrawal of ACIPHEX Sprinkle (5.9, 7).
- Fundic Gland Polyps: Risk increases with long-term use, especially beyond one year. Use the shortest duration of therapy (5.10).
Drug Interactions
See full prescribing information for a list of clinically important drug interactions ( 7).
Use In Specific Populations
Pediatric Use: Use is not recommended for the treatment of GERD in pediatric patients younger than 1 year of age; efficacy not demonstrated ( 8.4).
See 17 for PATIENT COUNSELING INFORMATION and Medication Guide.
Revised: 12/2020
Full Prescribing Information
1. Indications and Usage for Aciphex Sprinkle
ACIPHEX Sprinkle is indicated for treatment of Gastroesophageal Reflux Disease (GERD) in pediatric patients 1 to 11 years of age for up to 12 weeks.
2. Aciphex Sprinkle Dosage and Administration
2.1 Dosage Regimen
ACIPHEX Sprinkle is recommended for up to 12 weeks in pediatric patients 1 to 11 years of age and is dosed by body weight:
- Less than 15 kg: 5 mg once daily with the option to increase to 10 mg once daily, if inadequate response.
- 15 kg or more: 10 mg once daily.
2.2 Administration Recommendations
- Take the dose 30 minutes before a meal.
- Do not swallow the capsule whole.
- Open a capsule and sprinkle entire contents on a small amount of soft food (e.g., applesauce, fruit or vegetable based baby food, or yogurt) or empty contents into a small amount of liquid (e.g., infant formula, apple juice, or pediatric electrolyte solution). Food or liquid should be at or below room temperature.
- Do not chew or crush the granules.
- Take the entire dose within 15 minutes of preparation.
- Do not store mixture for future use.
- Take a missed dose as soon as possible. If it is almost time for the next dose, skip the missed dose and go back to the normal schedule. Do not take 2 doses at the same time.
3. Dosage Forms and Strengths
ACIPHEX Sprinkle is provided as:
- 5 mg: transparent blue and opaque white No. 2 capsule imprinted with "↑" on the capsule cap and "ACX 5mg" on the capsule body.
- 10 mg: transparent yellow and opaque white No. 2 capsule imprinted with "↑" on the capsule cap and "ACX 10mg" on the capsule body.
4. Contraindications
- ACIPHEX Sprinkle is contraindicated in patients with known hypersensitivity to rabeprazole, substituted benzimidazoles, or to any component of the formulation. Hypersensitivity reactions may include anaphylaxis, anaphylactic shock, angioedema, bronchospasm, acute tubulointerstitial nephritis, and urticaria [see Warnings and Precautions (5.3), Adverse Reactions (6)].
- PPIs, including ACIPHEX Sprinkle, are contraindicated with rilpivirine-containing products [see Drug Interactions (7)].
6. Adverse Reactions/Side Effects
The following serious adverse reactions are described below and elsewhere in labeling:
Acute Tubulointerstitial Nephritis [see Warnings and Precautions (5.3)]
Clostridium difficile-Associated Diarrhea [see Warnings and Precautions (5.4)]
Bone Fracture [see Warnings and Precautions (5.5)]
Cutaneous and Systemic Lupus Erythematosus [see Warnings and Precautions (5.6)]
Cyanocobalamin (Vitamin B-12) Deficiency [see Warnings and Precautions (5.7)]
Hypomagnesemia [see Warnings and Precautions (5.8)]
Fundic Gland Polyps [see Warnings and Precautions (5.10)]
6.1 Clinical Studies Experience
Because clinical trials are conducted under varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
The efficacy of ACIPHEX Sprinkle was established in a two-part, randomized, multicenter, double-blind, parallel-group study of 127 pediatric patients 1 to 11 years of age with a history of at least one GERD symptom within the 3 months before screening and a positive esophagogastroduodenoscopy (EGD; Hetzel-Dent Endoscopic Classification System, Grade ≥1 and Histological Features of Reflux Esophagitis Scale, Grade >0). The two-part study consisted of a 12-week treatment period in patients with endoscopically-proven GERD followed by a 24-week, double-blinded extension study. Subjects had a mean age of 6 years (range: 1 to 11 years) and 44% (56/127) were female and 56% (71/127) were male. Of the 127 subjects enrolled, 78% (99/127) were white, 10% (13/127) were black, and 2% (3/127) were Asian.
In the study, patients less than 15 kg body weight received either 5 mg or 10 mg ACIPHEX Sprinkle and patients 15 kg or greater body weight received 10 mg ACIPHEX Sprinkle. In this study, some patients were treated for 36 weeks. The most common adverse reactions leading to discontinuation were vomiting, abdominal pain, diarrhea, and nausea. The most common adverse reactions from the first 12 weeks of treatment are listed in Table 1.
| Adverse Reaction | Patients Less than 15 kg | Patients 15 kg or greater | |
|---|---|---|---|
| 5 mg
(N=21) % | 10 mg
(N=19) % | 10 mg
(N=44) % |
|
| * incidence of adverse reactions ≥9% | |||
| Vomiting | 10 | 11 | 14 |
| Abdominal Pain | 0 | 0 | 16 |
| Diarrhea | 14 | 21 | 9 |
| Headache | 0 | 0 | 9 |
| Nausea | 0 | 0 | 9 |
The safety profile was similar for those patients who received treatment for up to 36 weeks.
Adults and Adolescents Experience with Other Rabeprazole Formulations
The data described below reflect exposure to rabeprazole sodium delayed-release tablets in 1064 adult patients exposed for up to 8 weeks. The studies were primarily placebo- and active-controlled trials in adult patients with Erosive or Ulcerative Gastroesophageal Reflux Disease (GERD), Duodenal Ulcers and Gastric Ulcers. The population had a mean age of 53 years (range 18-89 years) and had a ratio of approximately 60% male: 40% female. The racial distribution was 86% Caucasian, 8% African American, 2% Asian, and 5% other. Most patients received either 10 mg, 20 mg, or 40 mg per day of rabeprazole.
An analysis of adverse reactions appearing in ≥2% of rabeprazole-treated patients (n=1064) and with a greater frequency than placebo (n=89) in controlled North American and European acute treatment trials, revealed the following adverse reactions: pain (3% vs. 1%), pharyngitis (3% vs. 2%), flatulence (3% vs. 1%), infection (2% vs. 1%), and constipation (2% vs. 1%).
Other adverse reactions seen in controlled clinical trials, which do not meet the above criteria (≥2% of rabeprazole-treated patients and greater than placebo) and for which there is a possibility of a causal relationship to rabeprazole, include the following: headache, abdominal pain, diarrhea, dry mouth, dizziness, peripheral edema, hepatic enzyme increase, hepatitis, hepatic encephalopathy, myalgia, and arthralgia.
In a multicenter, open-label study of adolescent patients 12 to 16 years of age with a clinical diagnosis of symptomatic GERD or endoscopically proven GERD, the adverse event profile was similar to that of adults. The adverse reactions reported without regard to relationship to rabeprazole that occurred in ≥2% of 111 patients were headache (9.9%), diarrhea (4.5%), nausea (4.5%), vomiting (3.6%), and abdominal pain (3.6%). The related reported adverse reactions that occurred in ≥2% of patients were headache (5.4%) and nausea (1.8%). There were no adverse reactions reported in this study that were not previously observed in adults.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post approval use of rabeprazole sodium. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Blood and Lymphatic System Disorders: agranulocytosis, hemolytic anemia, leukopenia, pancytopenia, and thrombocytopenia
Ear and Labyrinth Disorders: vertigo
Eye Disorders: blurred vision
Gastrointestinal Disorders: fundic gland polyps
General Disorders and Administration Site Conditions: sudden death
Hepatobiliary Disorders: jaundice
Immune System Disorders: anaphylaxis, angioedema, systemic lupus erythematosus, Stevens-Johnson syndrome, toxic epidermal necrolysis (some fatal)
Infections and Infestations: Clostridium difficile-associated diarrhea
Investigations: Increases in prothrombin time/INR (in patients treated with concomitant warfarin), TSH elevations
Metabolism and Nutrition Disorders: hyperammonemia, hypomagnesemia
Musculoskeletal System Disorders: bone fracture, rhabdomyolysis
Nervous System Disorders: coma
Psychiatric Disorders: delirium, disorientation
Renal and Urinary Disorders: interstitial nephritis
Respiratory, Thoracic and Mediastinal Disorders: interstitial pneumonia
Skin and Subcutaneous Tissue Disorders: severe dermatologic reactions, including bullous and other drug eruptions of the skin; cutaneous lupus erythematosus, erythema multiforme
Related/similar drugs
5. Warnings and Precautions
5.1 Presence of Gastric Malignancy
In adults, symptomatic response to therapy with ACIPHEX does not preclude the presence of gastric malignancy. Consider additional follow-up and diagnostic testing in adult patients who have a suboptimal response or an early symptomatic relapse after completing treatment with a PPI. In older patients, also consider an endoscopy.
5.2 Interaction with Warfarin
Steady state interactions of rabeprazole and warfarin have not been adequately evaluated in patients. There have been reports of increased INR and prothrombin time in patients receiving a proton pump inhibitor and warfarin concomitantly. Increases in INR and prothrombin time may lead to abnormal bleeding and even death. Patients treated with ACIPHEX Sprinkle and warfarin concomitantly may need to be monitored for increases in INR and prothrombin time [see Drug Interactions (7)] .
5.4 Clostridium difficile-Associated Diarrhea
Published observational studies suggest that PPI therapy like ACIPHEX Sprinkle may be associated with an increased risk of Clostridium difficile-associated diarrhea, especially in hospitalized patients. This diagnosis should be considered for diarrhea that does not improve [see Adverse Reactions (6.2)].
Patients should use the lowest dose and shortest duration of PPI therapy appropriate to the condition being treated.
Clostridium difficile-associated diarrhea (CDAD) has been reported with use of nearly all antibacterial agents.
5.3 Acute Tubulointerstitial Nephritis
Acute tubulointerstitial nephritis (TIN) has been observed in patients taking PPIs and may occur at any point during PPI therapy. Patients may present with varying signs and symptoms from symptomatic hypersensitivity reactions to non-specific symptoms of decreased renal function (e.g., malaise, nausea, anorexia). In reported case series, some patients were diagnosed on biopsy and in the absence of extra-renal manifestations (e.g., fever, rash or arthralgia).
Discontinue ACIPHEX Sprinkle and evaluate patients with suspected acute TIN [see Contraindications (4)].
5.5 Bone Fracture
Several published observational studies in adults suggest that PPI therapy may be associated with an increased risk for osteoporosis-related fractures of the hip, wrist, or spine. The risk of fracture was increased in patients who received high-dose, defined as multiple daily doses, and long-term PPI therapy (a year or longer). Patients should use the lowest dose and shortest duration of PPI therapy appropriate to the condition being treated.
Patients at risk for osteoporosis-related fractures should be managed according to established treatment guidelines [see Dosage and Administration (2), Adverse Reactions (6.2)] .
ACIPHEX Sprinkle is indicated for short-term treatment up to 12 weeks. Treatment for longer than 12 weeks is not recommended.
5.6 Cutaneous and Systemic Lupus Erythematosus
Cutaneous lupus erythematosus (CLE) and systemic lupus erythematosus (SLE) have been reported in patients taking PPIs, including rabeprazole. These events have occurred as both new onset and an exacerbation of existing autoimmune disease. The majority of PPI-induced lupus erythematosus cases were CLE.
The most common form of CLE reported in patients treated with PPIs was subacute CLE (SCLE) and occurred within weeks to years after continuous drug therapy in patients ranging from infants to the elderly. Generally, histological findings were observed without organ involvement.
Systemic lupus erythematosus (SLE) is less commonly reported than CLE in patients receiving PPIs. PPI associated SLE is usually milder than non-drug induced SLE. Onset of SLE typically occurred within days to years after initiating treatment primarily in patients ranging from young adults to the elderly. The majority of patients presented with rash; however, arthralgia and cytopenia were also reported.
Avoid administration of PPIs for longer than medically indicated. If signs or symptoms consistent with CLE or SLE are noted in patients receiving ACIPHEX Sprinkle, discontinue the drug and refer the patient to the appropriate specialist for evaluation. Most patients improve with discontinuation of the PPI alone in 4 to 12 weeks. Serological testing (e.g. ANA) may be positive and elevated serological test results may take longer to resolve than clinical manifestations.
5.7 Cyanocobalamin (Vitamin B-12) Deficiency
Daily treatment with any acid-suppressing medications over a long period of time (e.g., longer than 3 years) may lead to malabsorption of cyanocobalamin (vitamin B-12) caused by hypo- or achlorhydria. Rare reports of cyanocobalamin deficiency occurring with acid-suppressing therapy have been reported in the literature. This diagnosis should be considered if clinical symptoms consistent with cyanocobalamin deficiency are observed in patients treated with ACIPHEX Sprinkle.
5.8 Hypomagnesemia
Hypomagnesemia, symptomatic and asymptomatic, has been reported rarely in adult patients treated with PPIs for at least three months, in most cases after a year of therapy. Serious adverse events include tetany, arrhythmias, and seizures. In most patients, treatment of hypomagnesemia required magnesium replacement and discontinuation of the PPI.
For patients expected to be on prolonged treatment or who take PPIs with medications such as digoxin or drugs that may cause hypomagnesemia (e.g., diuretics), healthcare professionals may consider monitoring magnesium levels prior to initiation of PPI treatment and periodically [see Adverse Reactions (6.2)] .
ACIPHEX Sprinkle is indicated for short-term treatment of up to 12 weeks. Treatment for longer than 12 weeks is not recommended.
5.9 Interaction with Methotrexate
Literature suggests that concomitant use of PPIs with methotrexate (primarily at high dose; see methotrexate prescribing information) may elevate and prolong serum levels of methotrexate and/or its metabolite, possibly leading to methotrexate toxicities. In high-dose methotrexate administration, a temporary withdrawal of the PPI may be considered in some patients [see Drug Interactions (7)] .
5.10 Fundic Gland Polyps
PPI use is associated with an increased risk of fundic gland polyps that increases with long-term use, especially beyond one year. Most PPI users who developed fundic gland polyps were asymptomatic and fundic gland polyps were identified incidentally on endoscopy. Use the shortest duration of PPI therapy appropriate to the condition being treated.
7. Drug Interactions
Table 2 includes clinically important drug interactions and interaction with diagnostics when administered concomitantly with ACIPHEX Sprinkle and instructions for preventing or managing them.
Consult the labeling of concomitantly used drugs to obtain further information about interactions with PPIs.
| Antiretrovirals | |
| Clinical Impact: | The effect of PPIs on antiretroviral drugs is variable. The clinical importance and the mechanisms behind these interactions are not always known.
|
| Intervention: | Rilpivirine-containing products: Concomitant use with ACIPHEX Sprinkle is contraindicated [see Contraindications (4)] . See prescribing information. |
| Atazanavir: See prescribing information for atazanavir for dosing information. | |
| Nelfinavir: Avoid concomitant use with ACIPHEX Sprinkle. See prescribing information for nelfinavir. | |
| Saquinavir: See the prescribing information for saquinavir and monitor for potential saquinavir toxicities. | |
| Other antiretrovirals: See prescribing information. | |
| Warfarin | |
| Clinical Impact: | Increased INR and prothrombin time in patients receiving PPIs, including rabeprazole, and warfarin concomitantly. Increases in INR and prothrombin time may lead to abnormal bleeding and even death [see Warnings and Precautions (5.2)] . |
| Intervention: | Monitor INR and prothrombin time. Dose adjustment of warfarin may be needed to maintain target INR range. See prescribing information for warfarin. |
| Methotrexate | |
| Clinical Impact: | Concomitant use of rabeprazole with methotrexate (primarily at high dose) may elevate and prolong serum levels of methotrexate and/or its metabolite hydroxymethotrexate, possibly leading to methotrexate toxicities. No formal drug interaction studies of methotrexate with PPIs have been conducted [see Warnings and Precautions (5.9)]. |
| Intervention: | A temporary withdrawal of ACIPHEX Sprinkle may be considered in some patients receiving high-dose methotrexate administration. |
| Digoxin | |
| Clinical Impact: | Potential for increased exposure of digoxin [see Clinical Pharmacology (12.3)]. |
| Intervention: | Monitor digoxin concentrations. Dose adjustment of digoxin may be needed to maintain therapeutic drug concentrations. See prescribing information for digoxin. |
| Drugs Dependent on Gastric pH for Absorption (e.g., iron salts, erlotinib, dasatinib, nilotinib, mycophenolate mofetil, ketoconazole, itraconazole) | |
| Clinical Impact: | Rabeprazole can reduce the absorption of other drugs due to its effect on reducing intragastric acidity. |
| Intervention: | Mycophenolate mofetil (MMF): Co-administration of PPIs in healthy subjects and in transplant patients receiving MMF has been reported to reduce the exposure to the active metabolite, mycophenolic acid (MPA), possibly due to a decrease in MMF solubility at an increased gastric pH. The clinical relevance of reduced MPA exposure on organ rejection has not been established in transplant patients receiving ACIPHEX Sprinkle and MMF. Use ACIPHEX Sprinkle with caution in transplant patients receiving MMF . |
| See the prescribing information for other drugs dependent on gastric pH for absorption. | |
| Tacrolimus | |
| Clinical Impact: | Potentially increased exposure of tacrolimus, especially in transplant patients who are intermediate or poor metabolizers of CYP2C19. |
| Intervention: | Monitor tacrolimus whole blood trough concentrations. Dose adjustment of tacrolimus may be needed to maintain therapeutic drug concentrations. See prescribing information for tacrolimus. |
| Interactions with Investigations of Neuroendocrine Tumors | |
| Clinical Impact: | Serum chromogranin A (CgA) levels increase secondary to PPI-induced decreases in gastric acidity. The increased CgA level may cause false positive results in diagnostic investigations for neuroendocrine tumors. |
| Intervention: | Temporarily stop ACIPHEX Sprinkle treatment at least 14 days before assessing CgA levels and consider repeating the test if initial CgA levels are high. If serial tests are performed (e.g. for monitoring), the same commercial laboratory should be used for testing, as reference ranges between tests may vary. |
| Interaction with Secretin Stimulation Test | |
| Clinical Impact: | Hyper-response in gastrin secretion in adults in response to secretin stimulation test, falsely suggesting gastrinoma. |
| Intervention: | Temporarily stop treatment with ACIPHEX delayed-release tablets at least 14 days before assessing to allow gastrin levels to return to baseline. |
| False Positive Urine Tests for THC | |
| Clinical Impact: | There have been reports of false positive urine screening tests for tetrahydrocannabinol (THC) in patients receiving PPIs. |
| Intervention: | An alternative confirmatory method should be considered to verify positive results. |
8. Use In Specific Populations
8.1 Pregnancy
Risk Summary
There are no available human data on ACIPHEX use in pregnant women to inform the drug associated risk. The background risk of major birth defects and miscarriage for the indicated populations are unknown. However, the background risk in the U.S. general population of major birth defects is 2-4% and of miscarriage is 15-20% of clinically recognized pregnancies. No evidence of adverse developmental effects were seen in animal reproduction studies with rabeprazole administered during organogenesis at 13 and 8 times the human area under the plasma concentration-time curve (AUC) at the recommended dose for GERD, in rats and rabbits, respectively [see Data] .
Changes in bone morphology were observed in offspring of rats treated with oral doses of a different PPI through most of pregnancy and lactation. When maternal administration was confined to gestation only, there were no effects on bone physeal morphology in the offspring at any age [see Data] .
Data
Animal Data
Embryo-fetal developmental studies have been performed in rats at intravenous doses of rabeprazole during organogenesis up to 50 mg/kg/day (plasma AUC of 11.8 µg•hr/mL, about 13 times the adult human exposure at the recommended oral dose for GERD) and rabbits at intravenous doses up to 30 mg/kg/day (plasma AUC of 7.3 µg•hr/mL, about 8 times the adult human exposure at the recommended oral dose for GERD: 20 mg of rabeprazole delayed-release tablets per day) and have revealed no evidence of harm to the fetus due to rabeprazole.
Administration of rabeprazole to rats in late gestation and during lactation at an oral dose of 400 mg/kg/day (about 195 times the adult human oral dose based on mg/m 2) resulted in decreases in body weight gain of the pups.
A pre- and postnatal developmental toxicity study in rats with additional endpoints to evaluate bone development was performed with a different PPI at about 3.4 to 57 times an oral human dose on a body surface area basis. Decreased femur length, width and thickness of cortical bone, decreased thickness of the tibial growth plate, and minimal to mild bone marrow hypocellularity were noted at doses of this PPI equal to or greater than 3.4 times an oral human dose on a body surface area basis. Physeal dysplasia in the femur was also observed in offspring after in utero and lactational exposure to the PPI at doses equal to or greater than 33.6 times an oral human dose on a body surface area basis. Effects on maternal bone were observed in pregnant and lactating rats in a pre- and postnatal toxicity study when the PPI was administered at oral doses of 3.4 to 57 times an oral human dose on a body surface area basis. When rats were dosed from gestational day 7 through weaning on postnatal day 21, a statistically significant decrease in maternal femur weight of up to 14% (as compared to placebo treatment) was observed at doses equal to or greater than 33.6 times an oral human dose on a body surface area basis.
A follow-up developmental toxicity study in rats with further time points to evaluate pup bone development from postnatal day 2 to adulthood was performed with a different PPI at oral doses of 280 mg/kg/day (about 68 times an oral human dose on a body surface area basis) where drug administration was from either gestational day 7 or gestational day 16 until parturition. When maternal administration was confined to gestation only, there were no effects on bone physeal morphology in the offspring at any age.
8.2 Lactation
Risk Summary
Lactation studies have not been conducted to assess the presence of rabeprazole in human milk, the effects of rabeprazole on the breastfed infant, or the effects of rabeprazole on milk production. Rabeprazole is present in rat milk. The development and health benefits of breastfeeding should be considered along with the mother's clinical need for ACIPHEX Sprinkle and any potential adverse effects on the breastfed infant from ACIPHEX Sprinkle or from the underlying maternal condition.
8.4 Pediatric Use
GERD in Pediatric Patients 1 to 11 Years of Age
The use of ACIPHEX Sprinkle for treatment of GERD in pediatric patients 1 to 11 years of age is supported by a randomized, multicenter, double-blind clinical trial which evaluated two dose levels of ACIPHEX Sprinkle in 127 pediatric patients with endoscopic and histologic evidence of GERD prior to study treatment. Dosing was determined by body weight: Patients weighing 6.0 to 14.9 kg received either 5 or 10 mg of ACIPHEX Sprinkle daily and those weighing 15.0 kg or more received 10 or 20 mg of ACIPHEX Sprinkle daily. After 12 weeks of rabeprazole treatment, 81% of patients demonstrated esophageal mucosal healing on endoscopic assessment. In patients who had esophageal mucosal healing at 12 weeks and elected to continue for 24 more weeks of rabeprazole, 90% retained esophageal mucosal healing at 36 weeks. No prespecified formal hypothesis testing for evaluation of efficacy was conducted. The absence of a placebo group does not allow assessment of sustained efficacy through 36 weeks. There were no adverse reactions reported in this study that were not previously observed in adolescents or adults.
Symptomatic GERD in Infants 1 to 11 Months of Age
The use of ACIPHEX Sprinkle is not recommended because studies conducted do not demonstrate efficacy for the treatment of GERD in pediatric patients younger than 1 year of age.
In a randomized, multicenter, placebo-controlled withdrawal trial, infants 1 to 11 months of age with a clinical diagnosis of symptomatic GERD, or suspected or endoscopically proven GERD, were treated up to 8 weeks in two treatment periods. In the first treatment period (open-label), 344 infants received 10 mg of ACIPHEX Sprinkle for up to 3 weeks. Infants with clinical response were then eligible to enter the second treatment period, which was double-blind and randomized. Two hundred sixty-eight infants were randomized to receive either placebo or 5 mg or 10 mg ACIPHEX Sprinkle.
This study did not demonstrate efficacy based on assessment of frequency of regurgitation and weight-for-age Z-score. Adverse reactions that occurred in ≥5% of patients in any treatment group and with a higher rate than placebo included pyrexia (7%) and increased serum gastrin levels (5%). There were no adverse reactions reported in this study that were not previously observed in adolescents and adults.
Neonates <1 Month and Preterm Infants <44 Weeks Corrected Gestational Age
The use of ACIPHEX Sprinkle is not recommended for the treatment of GERD, based on the risk of prolonged acid suppression and lack of demonstrated safety and effectiveness in neonates. Based on population pharmacokinetic analysis, the median (range) for the apparent clearance (CL/F) was 1.05 L/h (0.0543 to 3.44 L/h) in neonates and 4.46 L/h (0.822 to 12.4 L/h) in patients 1 to 11 months of age following once daily administration of oral ACIPHEX Sprinkle.
Juvenile Animal Data
Studies in juvenile and young adult rats and dogs were performed. In juvenile animal studies rabeprazole sodium was administered orally to rats for up to 5 weeks and to dogs for up to 13 weeks, each commencing on Day 7 post-partum and followed by a 13-week recovery period. Rats were dosed at 5, 25, or 150 mg/kg/day and dogs were dosed at 3, 10, or 30 mg/kg/day. The data from these studies were comparable to those reported for young adult animals. Pharmacologically mediated changes, including increased serum gastrin levels and stomach changes, were observed at all dose levels in both rats and dogs. These observations were reversible over the 13-week recovery periods. Although body weights and/or crown-rump lengths were minimally decreased during dosing, no effects on the development parameters were noted in either juvenile rats or dogs.
When juvenile animals were treated for 28 days with a different PPI at doses equal to or greater than 34 times the daily oral human dose on a body surface area basis, overall growth was affected and treatment-related decreases in body weight (approximately 14%) and body weight gain, and decreases in femur weight and femur length were observed.
8.5 Geriatric Use
No studies with ACIPHEX Sprinkle have been conducted in geriatric patients. ACIPHEX Sprinkle is not indicated for use in patients older than 11 years of age.
8.6 Hepatic Impairment
Administration of rabeprazole sodium delayed-release tablets to adult patients with mild to moderate hepatic impairment (Child-Pugh Class A and B, respectively) resulted in increased exposure and decreased elimination [see Clinical Pharmacology (12.3)] . No dosage adjustment of ACIPHEX Sprinkle is necessary in patients with mild to moderate hepatic impairment. There is no information in patients with severe hepatic impairment (Child-Pugh Class C). Avoid use of ACIPHEX Sprinkle in patients with severe hepatic impairment; however, if treatment is necessary, monitor patients for adverse reactions [see Warnings and Precautions (5), Adverse Reactions (6)] .
10. Overdosage
Seven reports of accidental overdosage with rabeprazole have been received. The maximum reported overdose was 80 mg. There were no clinical signs or symptoms associated with any reported overdose. Patients with Zollinger-Ellison syndrome have been treated with up to 120 mg rabeprazole once daily. No specific antidote for rabeprazole is known. Rabeprazole is extensively protein bound and is not readily dialyzable.
In the event of overdosage, treatment should be symptomatic and supportive.
If over-exposure occurs, call your Poison Control Center at 1-800-222-1222 for current information on the management of poisoning or overdosage.
11. Aciphex Sprinkle Description
The active ingredient in ACIPHEX Sprinkle delayed-release capsules is rabeprazole sodium, which is a proton pump inhibitor. It is a substituted benzimidazole known chemically as 2-[[[4-(3-methoxypropoxy)-3-methyl-2-pyridinyl]-methyl]sulfinyl]-1 H–benzimidazole sodium salt. It has an empirical formula of C 18H 20N 3NaO 3S and a molecular weight of 381.42. Rabeprazole sodium is a white to slightly yellowish-white solid. It is very soluble in water and methanol, freely soluble in ethanol, chloroform, and ethyl acetate and insoluble in ether and n-hexane. The stability of rabeprazole sodium is a function of pH; it is rapidly degraded in acid media, and is more stable under alkaline conditions. The structural figure is:
Figure 1
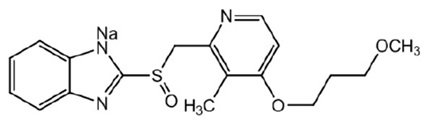
ACIPHEX Sprinkle is available for oral administration as 5 mg and 10 mg rabeprazole sodium delayed-release capsules containing enteric coated granules.
ACIPHEX Sprinkle contains granules of rabeprazole sodium in a hard hypromellose capsule. Inactive ingredients are colloidal silicon dioxide, diacetylated monoglycerides, ethylcellulose, hydroxypropyl cellulose, hypromellose phthalate, magnesium oxide, magnesium stearate, mannitol, talc, titanium dioxide, carrageenan, potassium chloride, FD&C Blue No. 2 Aluminum Lake (in the 5 mg capsule), FD&C Yellow, No. 6 (in the 10 mg capsule), and gray printing ink.
12. Aciphex Sprinkle - Clinical Pharmacology
12.1 Mechanism of Action
Rabeprazole belongs to a class of antisecretory compounds (substituted benzimidazole proton-pump inhibitors) that do not exhibit anticholinergic or histamine H 2-receptor antagonist properties, but suppress gastric acid secretion by inhibiting the gastric H +, K +ATPase at the secretory surface of the gastric parietal cell. Because this enzyme is regarded as the acid (proton) pump within the parietal cell, rabeprazole has been characterized as a gastric proton-pump inhibitor. Rabeprazole blocks the final step of gastric acid secretion.
In gastric parietal cells, rabeprazole is protonated, accumulates, and is transformed to an active sulfenamide. When studied in vitro, rabeprazole is chemically activated at pH 1.2 with a half-life of 78 seconds. It inhibits acid transport in porcine gastric vesicles with a half-life of 90 seconds.
12.3 Pharmacokinetics
Absorption
After oral administration to healthy adults of 10 mg ACIPHEX Sprinkle (delayed-release capsules opened and granules sprinkled on one tablespoon [15 mL] of applesauce) under fasting condition, median time (T max) to peak plasma concentrations (C max) of rabeprazole was 2.5 hours and ranged 1.0 to 6.5 hours. The plasma half-life of rabeprazole ranges from 1 to 2 hours.
In healthy adults, a concomitant high fat meal delayed the absorption of rabeprazole from ACIPHEX Sprinkle (granules sprinkled on one tablespoon (15 mL) of applesauce) resulting in the median T max of 4.5 hours and decreased the C max and AUC last on average by 55% and 33%, respectively [see Dosage and Administration (2.2)].
When 10 mg ACIPHEX Sprinkle (granules) administered under fasting conditions to healthy adults on one tablespoon (15 mL) of applesauce, one tablespoon (15 mL) of yogurt, or when mixed with a small amount (5 mL) of liquid infant formula; the type of soft food did not significantly affect T max, C max and AUC of rabeprazole.
Elimination
Metabolism: Rabeprazole is extensively metabolized. A significant portion of rabeprazole is metabolized via systemic nonenzymatic reduction to a thioether compound. Rabeprazole is also metabolized to sulphone and desmethyl compounds via cytochrome P450 in the liver. The thioether and sulphone are the primary metabolites measured in human plasma. These metabolites were not observed to have significant antisecretory activity. In vitro studies have demonstrated that rabeprazole is metabolized in the liver primarily by cytochromes P450 3A (CYP3A) to a sulphone metabolite and cytochrome P450 2C19 (CYP2C19) to desmethyl rabeprazole. CYP2C19 exhibits a known genetic polymorphism due to its deficiency in some sub-populations (e.g., 3 to 5% of Caucasians and 17 to 20% of Asians). Rabeprazole metabolism is slow in these sub-populations, therefore, they are referred to as poor metabolizers of the drug.
Excretion: Following a single 20 mg oral dose of 14C-labeled rabeprazole, approximately 90% of the drug was eliminated in the urine, primarily as thioether carboxylic acid; its glucuronide, and mercapturic acid metabolites. The remainder of the dose was recovered in the feces. Total recovery of radioactivity was 99.8%. No unchanged rabeprazole was recovered in the urine or feces.
Specific Populations
Pediatric Patients: In patients with GERD 1 to 11 years of age, following once daily administration of ACIPHEX Sprinkle at doses from 0.14 to 1 mg/kg, the median time to peak plasma concentration ranged from 2 to 4 hours and the half-life was about 2.5 hours. No appreciable accumulation was noted following 5 days of dosing compared to exposure after a single dose.
Based on population pharmacokinetic analysis, over the body weight range from 7 to 77 kg, the apparent rabeprazole clearance increased from 8.0 to 13.5 L/hr, an increase of 69%.
The mean estimated total exposure i.e., AUC after a 10 mg dose of ACIPHEX Sprinkle in patients with GERD 1 to 11 years of age is comparable to AUC after 10 mg rabeprazole sodium delayed-release tablet in adults.
Male and Female Patients and Racial or Ethnic Groups: In analyses of adult data adjusted for body mass and height, rabeprazole pharmacokinetics showed no clinically significant differences between male and female subjects. In studies that used different formulations of rabeprazole, AUC 0-∞ values for healthy Japanese men were approximately 50 to 60% greater than values derived from pooled data from healthy men in the United States.
Patients with Renal Impairment: In 10 adult patients with stable end-stage renal disease requiring maintenance hemodialysis (creatinine clearance ≤5 mL/min/1.73 m 2), no clinically significant differences were observed in the pharmacokinetics of rabeprazole after administration of rabeprazole 20 mg delayed-release tablets when compared to 10 healthy adult subjects.
Patients with Hepatic Impairment: In a single dose study of 10 adult patients with chronic mild to moderate hepatic impairment (Child-Pugh Class A and B, respectively) who were administered a 20 mg dose of rabeprazole sodium delayed-release tablets, AUC 0-24 was approximately doubled, the elimination half-life was 2- to 3-fold higher, and total body clearance was decreased to less than half compared to values in healthy adult men.
In a multiple dose study of 12 adult patients with mild to moderate hepatic impairment administered 20 mg rabeprazole sodium delayed-release tablets once daily for eight days, AUC 0-∞ and C max values increased approximately 20% compared to values in healthy age- and gender-matched subjects. These increases were not statistically significant.
No information exists on rabeprazole disposition in patients with severe hepatic impairment (Child-Pugh Class C) [see Use in Specific Populations (8.6)].
Drug Interaction Studies
Effects of Rabeprazole on Other Drugs
Studies in healthy adult subjects have shown that rabeprazole does not have clinically significant interactions with other drugs metabolized by the CYP450 system, such as theophylline (CYP1A2) given as single oral doses, diazepam (CYP2C9 and CYP3A4) as a single intravenous dose, and phenytoin (CYP2C9 and CYP2C19) given as a single intravenous dose (with supplemental oral dosing). Steady state interactions of rabeprazole and other drugs metabolized by this enzyme system have not been studied in patients.
Clopidogrel: Clopidogrel is metabolized to its active metabolite in part by CYP2C19. A study of healthy adult subjects including CYP2C19 extensive and intermediate metabolizers receiving once daily administration of clopidogrel 75 mg concomitantly with placebo or with 20 mg rabeprazole sodium delayed-release tablets (n=36), for 7 days was conducted. The mean AUC of the active metabolite of clopidogrel was reduced by approximately 12% (mean AUC ratio was 88%, with 90% CI of 81.7 to 95.5%) when rabeprazole sodium delayed-release tablets was co-administered compared to administration of clopidogrel with placebo [see Drug Interactions (7)].
Digoxin: In healthy adult subjects (n=16), co-administration of 20 mg rabeprazole sodium delayed-release tablets with 2.5 mg once daily doses of digoxin at steady state resulted in approximately 29% and 19% increase in mean C max and AUC (0-24) of digoxin [see Drug Interactions (7)].
Ketoconazole: In healthy adult subjects (n=19), co-administration of 20 mg rabeprazole sodium delayed-release tablets at steady state with a single 400 mg oral dose ketoconazole resulted in approximately an average of 31% reduction in both C max and AUC (0-inf) of ketoconazole [see Drug Interactions (7)].
Cyclosporine: In vitro incubations employing human liver microsomes indicated that rabeprazole inhibited cyclosporine metabolism with an IC 50 of 62 micromolar, a concentration that is over 50 times higher than the C max in healthy volunteers following 14 days of dosing with 20 mg of ACIPHEX delayed-release tablets. This degree of inhibition is similar to that by omeprazole at equivalent concentrations.
12.5 Pharmacogenomics
In a clinical study in Japan evaluating rabeprazole sodium delayed-release tablets in Japanese adult patients categorized by CYP2C19 genotype (n=6 per genotype category), gastric acid suppression was higher in poor metabolizers as compared to extensive metabolizers. The clinical relevance of this is not known. This could be due to higher rabeprazole plasma levels in poor metabolizers. Whether or not interactions of rabeprazole sodium with other drugs metabolized by CYP2C19 would be different between extensive metabolizers and poor metabolizers has not been studied.
13. Nonclinical Toxicology
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
In an 88/104-week carcinogenicity study in CD-1 mice, rabeprazole at oral doses up to 100 mg/kg/day did not produce any increased tumor occurrence. The highest tested dose produced a systemic exposure to rabeprazole (AUC) of 1.40 µg•hr/mL which is 1.6 times the adult human exposure (plasma AUC 0-∞ = 0.88 µg•hr/mL) at the recommended dose for GERD (20 mg of rabeprazole sodium delayed-release tablets per day). In a 28-week carcinogenicity study in p53 +/- transgenic mice, rabeprazole at oral doses of 20, 60, and 200 mg/kg/day did not cause an increase in the incidence rates of tumors but produced gastric mucosal hyperplasia at all doses. The systemic exposure to rabeprazole at 200 mg/kg/day is about 17 to 24 times the adult human exposure at the recommended dose for GERD (20 mg of rabeprazole sodium delayed-release tablets per day). In a 104-week carcinogenicity study in Sprague-Dawley rats, males were treated with oral doses of 5, 15, 30, and 60 mg/kg/day and females with 5, 15, 30, 60, and 120 mg/kg/day. Rabeprazole produced gastric enterochromaffin-like (ECL) cell hyperplasia in male and female rats and ECL cell carcinoid tumors in female rats at all doses including the lowest tested dose. The lowest dose (5 mg/kg/day) produced a systemic exposure to rabeprazole (AUC) of about 0.1 µg•hr/mL which is about 0.1 times the adult human exposure at the recommended dose for GERD (20 mg of rabeprazole sodium delayed-release tablets per day). In male rats, no treatment-related tumors were observed at doses up to 60 mg/kg/day producing a rabeprazole plasma exposure (AUC) of about 0.2 µg•hr/mL (0.2 times the adult human exposure at the recommended dose for GERD).
Rabeprazole was positive in the Ames test, the Chinese hamster ovary cell (CHO/HGPRT) forward gene mutation test, and the mouse lymphoma cell (L5178Y/TK+/–) forward gene mutation test. Its demethylated-metabolite was also positive in the Ames test. Rabeprazole was negative in the in vitro Chinese hamster lung cell chromosome aberration test, the in vivo mouse micronucleus test, and the in vivo and ex vivo rat hepatocyte unscheduled DNA synthesis (UDS) tests.
Rabeprazole at intravenous doses up to 30 mg/kg/day (plasma AUC of 8.8 µg•hr/mL, about 10 times the adult human exposure at the recommended dose for GERD) was found to have no effect on fertility and reproductive performance of male and female rats. The recommended dose for GERD in adults is 20 mg per day (rabeprazole sodium delayed-release tablets).
14. Clinical Studies
The use of ACIPHEX Sprinkle in pediatric patients 1 to 11 years of age is supported by a two-part, multicenter, randomized, double-blind, parallel 2 dose arms clinical trial which was conducted in 127 pediatric patients with endoscopic and histologic evidence of GERD prior to study treatment.
Part 1 of the trial was 12 weeks in duration. Patients were randomized to one of two rabeprazole dose levels based on body weight. Patients weighing 6 to 14.9 kg received either 5 or 10 mg ACIPHEX Sprinkle, and those with body weight ≥15 kg received 10 mg ACIPHEX Sprinkle. Part 2 was a 24-week double-blinded extension of Part 1 (on same dose assigned in Part 1). Endoscopic evaluations were performed at 12 weeks (Part 1) and 36 weeks (Part 2) to assess esophageal healing. No prespecified formal hypothesis testing was conducted.
For Part 1, rates of endoscopic healing were calculated and are shown in Table 3.
| Endoscopic
Classification of GERD At Baseline | Healing Rate at 12 weeks
|
||
|---|---|---|---|
| Body Weight Less than 15 kg | Body Weight 15 kg or Greater | ||
| 5 mg dose | 10 mg dose | 10 mg dose | |
| a Hetzel-Dent score ≥2
b Hetzel-Dent score = 1 |
|||
| Erosive a | 88% (7/8) | 83% (5/6) | 71% (12/17) |
| Non-erosive b | 78% (7/9) | 100% (10/10) | 81% (17/21) |
Of the 87 patients with healing in Part 1, 64 patients were enrolled into Part 2. The absence of a placebo group does not allow assessment of sustained efficacy through 36 weeks. Of the 52 patients with available data, healing was observed in 47 (90%) patients at 36 weeks.
The recommended dosage of ACIPHEX Sprinkle is 5 mg once daily for 12 weeks in patients less than 15 kg with the option to increase to 10 mg once daily if there is an inadequate response. In patients 15 kg or greater, the recommended dosage is 10 mg once daily for 12 weeks.
16. How is Aciphex Sprinkle supplied
ACIPHEX Sprinkle delayed-release capsules (5 mg) are supplied as transparent blue and opaque white capsules containing enteric coated granules. Identification and strength (ACX 5mg) are imprinted on the body of the capsule. An arrow (↑) imprint on the capsule cap indicates direction for opening a capsule.
Bottles of 30 (NDC 23594-205-01)
ACIPHEX Sprinkle delayed-release capsules (10 mg) are supplied as transparent yellow and opaque white capsules containing enteric coated granules. Identification and strength (ACX 10mg) are imprinted on the body of the capsule. An arrow (↑) imprint on the capsule cap indicates direction for opening a capsule.
Bottles of 30 (NDC 23594-210-01)

Distributed and Marketing by Cerecor, Inc. Rockville, MD 20850
ACIPHEX
® is a registered trademark of Eisai R&D Management Co., Ltd;
ACIPHEX
® Sprinkle™ is a trademark of Eisai R&D Management Co., Ltd, each of which is licensed to Cerecor, Inc.
17. Patient Counseling Information
Advise the patient or caregiver to read the FDA-approved patient labeling (Medication Guide).
Acute Tubulointerstitial Nephritis
Advise the patient or caregiver to call the patient’s healthcare provider immediately if they experience signs and/or symptoms associated with acute tubulointerstitial nephritis [see Contraindications (4), Warnings and Precautions (5.3)].
Clostridium difficile-Associated Diarrhea
Advise the patient or caregiver to immediately call the patient’s healthcare provider if they experience diarrhea that does not improve [see Warnings and Precautions (5.4)].
Bone Fracture
Advise the patient or caregiver to report any fractures, especially of the hip, wrist or spine, to the patient’s healthcare provider [see Warnings and Precautions (5.5)].
Cutaneous and Systemic Lupus Erythematosus
Advise the patient or caregiver to immediately call the patient’s healthcare provider for any new or worsening of symptoms associated with cutaneous or systemic lupus erythematosus [see Warnings and Precautions (5.6)]
Cyanocobalamin (Vitamin B-12) Deficiency
Advise the patient or caregiver to report any clinical symptoms that may be associated with cyanocobalamin deficiency to the patient’s healthcare provider if they have been receiving ACIPHEX Sprinkle for longer than 3 years [see Warnings and Precautions (5.7)].
Hypomagnesemia
Advise the patient or caregiver to report any clinical symptoms that may be associated with hypomagnesemia to the patient’s healthcare provider, if they have been receiving ACIPHEX Sprinkle for at least 3 months [see Warnings and Precautions (5.8)].
Drug Interactions
Advise the patient or caregiver to report to the patient’s healthcare provider if they are taking rilpilvirine-containing products [see Contraindications (4)], warfarin or high-dose methotrexate [see Warnings and Precautions (5.2, 5.9)].
Administration
- Take the dose 30 minutes before a meal.
- Do not swallow the capsule whole.
- Open the ACIPHEX Sprinkle capsule and sprinkle the granule contents on a small amount of soft food (e.g., applesauce, fruit or vegetable based baby food, or yogurt) or empty contents into a small amount of liquid (e.g., infant formula, apple juice, or pediatric electrolyte solution). Food or liquid should be at or below room temperature.
- Do not chew or crush the granules.
- Take the entire dose within 15 minutes of preparation.
- Do not store mixture for future use.
- Take a missed dose as soon as possible. If it is almost time for the next dose, skip the missed dose and go back to the normal schedule. Do not take 2 doses at the same time.
Acute Interstitial Nephritis
Advise the patient or caregiver to call the patient’s healthcare provider immediately if they experience signs and/or symptoms associated with acute interstitial nephritis [see Warnings and Precautions (5.3)] .
Clostridium difficile-Associated Diarrhea
Advise the patient or caregiver to immediately call the patient’s healthcare provider if they experience diarrhea that does not improve [see Warnings and Precautions (5.4)] .
Bone Fracture
Advise the patient or caregiver to report any fractures, especially of the hip, wrist or spine, to the patient’s healthcare provider [see Warnings and Precautions (5.5)] .
Cutaneous and Systemic Lupus Erythematosus
Advise the patient or caregiver to immediately call the patient’s healthcare provider for any new or worsening of symptoms associated with cutaneous or systemic lupus erythematosus [see Warnings and Precautions (5.6)]
Cyanocobalamin (Vitamin B-12) Deficiency
Advise the patient or caregiver to report any clinical symptoms that may be associated with cyanocobalamin deficiency to the patient’s healthcare provider if they have been receiving ACIPHEX Sprinkle for longer than 3 years [see Warnings and Precautions (5.7)].
Hypomagnesemia
Advise the patient or caregiver to report any clinical symptoms that may be associated with hypomagnesemia to the patient’s healthcare provider, if they have been receiving ACIPHEX Sprinkle for at least 3 months [see Warnings and Precautions (5.8)].
Drug Interactions
Advise the patient or caregiver to report to the patient’s healthcare provider if they are taking rilpilvirine-containing products [see Contraindications (4)] , warfarin or high-dose methotrexate [see Warnings and Precautions (5.2, 5.9)] .
Administration
- Take the dose 30 minutes before a meal.
- Do not swallow the capsule whole.
- Open the ACIPHEX Sprinkle capsule and sprinkle the granule contents on a small amount of soft food (e.g., applesauce, fruit or vegetable based baby food, or yogurt) or empty contents into a small amount of liquid (e.g., infant formula, apple juice, or pediatric electrolyte solution). Food or liquid should be at or below room temperature.
- Do not chew or crush the granules.
- Take the entire dose within 15 minutes of preparation.
- Do not store mixture for future use.
- Take a missed dose as soon as possible. If it is almost time for the next dose, skip the missed dose and go back to the normal schedule. Do not take 2 doses at the same time.
MEDICATION GUIDE
ACIPHEX® Sprinkle™ (a-se-feks spr-en-kle)
(rabeprazole sodium delayed-release capsules)
What is the most important information I should know about ACIPHEX Sprinkle?
Your child should take ACIPHEX Sprinkle exactly as prescribed, at the lowest dose possible and for the shortest time needed.
ACIPHEX Sprinkle may help your child’s acid-related symptoms, but your child could still have serious stomach problems. Talk with your child’s doctor.
ACIPHEX Sprinkle can cause serious side effects, including:
A type of kidney problem (acute tubulointerstitial nephritis). Some people who take proton pump inhibitor (PPI) medicines, including ACIPHEX Sprinkle, may develop a kidney problem called acute tubulointerstitial nephritis that can happen at any time during treatment with ACIPHEX Sprinkle. Call your child’s doctor right away if your child has a decrease in the amount that they urinate or if they have blood in their urine.
Diarrhea caused by an infection (Clostridium difficile) in your child’s intestines. Call your child’s doctor right away if your child has watery stools or stomach pain that does not go away. Your child may or may not have a fever.
Bone fractures (hip, wrist or spine). Bone fractures in the hip, wrist or spine may happen in people who take multiple daily doses of PPI medicines and for a long period of time (a year or longer). Tell your child’s doctor if your child has a bone fracture, especially in the hip, wrist or spine.
Certain types of lupus erythematosus. Lupus erythematosus is an autoimmune disorder (the body’s immune cells attack other cells or organs in the body). Some people who take PPI medicines, including ACIPHEX Sprinkle, may develop certain types of lupus erythematosus or have worsening of the lupus they already have. Call your child’s doctor right away if they have new or worsening joint pain or a rash on their cheeks or arms that gets worse in the sun.
Talk to your child’s doctor about your child’s risk of serious side effects.
ACIPHEX Sprinkle can have other serious side effects. See “What are the possible side effects of ACIPHEX Sprinkle?”
What is ACIPHEX Sprinkle?
ACIPHEX Sprinkle is a prescription medicine called a proton pump inhibitor (PPI). ACIPHEX Sprinkle reduces the amount of acid in the stomach.
ACIPHEX Sprinkle is used in children 1 year to 11 years of age to treat Gastroesophageal Reflux Disease (GERD) for up to 12 weeks.
ACIPHEX Sprinkle is not effective in treating GERD in children under 1 year of age.
ACIPHEX Sprinkle should not be used to treat GERD in babies younger than 1 month of age.
Your child should not take ACIPHEX Sprinkle if they are:
allergic to rabeprazole, any other PPI medicine, or any of the ingredients in ACIPHEX Sprinkle. See the end of this Medication Guide for a complete list of ingredients.
taking a medicine that contains rilpivirine (EDURANT, COMPLERA, ODEFSEY) used to treat HIV-1 (Human Immunodeficiency Virus).
Before your child takes ACIPHEX Sprinkle, tell your child’s doctor about all of your child’s medical conditions, including if they:
have low magnesium levels in their blood.
have liver problems.
are pregnant or plan to become pregnant. It is not known if ACIPHEX Sprinkle can harm an unborn baby.
are breastfeeding or plan to breastfeed. It is not known if ACIPHEX Sprinkle passes into breast milk. Talk to your child’s doctor about the best way to feed her baby if she takes ACIPHEX Sprinkle.
Tell your child’s doctor about all the medicines your child takes, including prescription and over-the-counter medicines, vitamins, and herbal supplements. Especially tell your child’s doctor if your child takes warfarin (COUMADIN, JANTOVEN) or methotrexate (Otrexup, Rasuvo,Trexall, Xatmep).
How should my child take ACIPHEX Sprinkle?
Your child should take ACIPHEX Sprinkle exactly as prescribed. Your child’s doctor will prescribe the dose that is right for your child.
Your child should take ACIPHEX Sprinkle 1 time each day.
Your child should take ACIPHEX Sprinkle 30 minutes before a meal.
Your child should not swallow the ACIPHEX Sprinkle capsule whole.
Prepare and give a dose of ACIPHEX Sprinkle to your child as follows:
Open the ACIPHEX Sprinkle capsule in the direction that the arrow (↑) on the capsule is pointing. Sprinkle all of the capsule contents onto a small amount of soft food such as applesauce, fruit or vegetable based baby food, or yogurt. You may also empty all of the capsule contents into a small amount of infant formula, apple juice, or a pediatric electrolyte solution. The food or liquid that you use should be at or below room temperature.
Your child should swallow the entire mixture. They should not chew or crush the granules.
Your child should take the entire dose within 15 minutes of preparing it. Do not save it for use later.
If your child misses a dose of ACIPHEX Sprinkle, they should take it as soon as possible. If it is almost time for their next dose, they should not take the missed dose. Your child should take their next dose at their regular time. They should not take 2 doses at the same time.
If your child takes too much ACIPHEX Sprinkle, call your child’s doctor or your poison control center at 1-800-222-1222 right away, or go to the nearest emergency room.
What are the possible side effects of ACIPHEX Sprinkle?
ACIPHEX Sprinkle can cause serious side effects, including:
See “What is the most important information I should know about ACIPHEX Sprinkle?”
Interaction with warfarin. Taking warfarin with a PPI medicine may lead to an increased risk of bleeding and death. If your child takes warfarin, their doctor may check their blood to see if they have an increased risk of bleeding. If your child takes warfarin during treatment with ACIPHEX Sprinkle, tell their doctor right away if they have any signs or symptoms of bleeding, including:
pain, swelling or discomfort
headaches, dizziness, or weakness
unusual bruising (bruises that happen without known cause or that grow in size)
nosebleeds
bleeding gums
bleeding from cuts takes a long time to stop
menstrual bleeding that is heavier than normal
pink or brown urine
red or black stools
coughing up blood
vomiting blood or vomit that looks like coffee grounds
Low vitamin B-12 levels in the body can happen in people who have taken ACIPHEX Sprinkle for a long time (more than 3 years). Tell your child’s doctor if your child has symptoms of low vitamin B-12 levels, including shortness of breath, lightheadedness, irregular heartbeat, muscle weakness, pale skin, feeling tired, mood changes, and tingling or numbness in the arms and legs.
Low magnesium levels in the body can happen in people who have taken ACIPHEX Sprinkle for at least 3 months. Tell your child’s doctor if your child has symptoms of low magnesium levels, including seizures, dizziness, irregular heartbeat, jitteriness, muscle aches or weakness, and spasms of hands, feet or voice.
Stomach growths (fundic gland polyps). People who take PPI medicines for a long time have an increased risk of developing a certain type of stomach growths called fundic gland polyps, especially after taking PPI medicines for more than 1 year.
The most common side effects of ACIPHEX Sprinkle include: vomiting, stomach-area (abdomen) pain, diarrhea, headache, and nausea.
These are not all of the possible side effects of ACIPHEX Sprinkle. Call your child’s doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
How should I store ACIPHEX Sprinkle?
Store ACIPHEX Sprinkle in a dry place at room temperature between 68°F to 77°F (20°C to 25°C).
Keep ACIPHEX Sprinkle and all medicines out of the reach of children.
General Information about the safe and effective use of ACIPHEX Sprinkle.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use ACIPHEX Sprinkle for a condition for which it was not prescribed. Do not give ACIPHEX Sprinkle to other people, even if they have the same symptoms that you have. It may harm them.
You can ask your child’s doctor or pharmacist for information about ACIPHEX Sprinkle that is written for health professionals.
What are the ingredients in ACIPHEX Sprinkle?
Active ingredient: rabeprazole sodium
Inactive ingredients: colloidal silicon dioxide, diacetylated monoglycerides, ethylcellulose, hydroxypropyl cellulose, hypromellose phthalate, magnesium oxide, magnesium stearate, mannitol, talc, titanium dioxide, carrageenan, potassium chloride, FD&C Blue No. 2 Aluminum Lake (in the 5 mg capsule), FD&C Yellow, No. 6 (in the 10 mg capsule), and gray printing ink.
Distributed and Marketed by Aytu Therapeutics, LLC Englewood, CO 80112
ACIPHEX® is a registered trademark of Eisai R&D Management Co., Ltd;
ACIPHEX® Sprinkle™ is a trademark of Eisai R&D Management Co., Ltd, each of which is licensed to Aytu Therapeutics, LLC
For more information, go to www.aciphexsprinkle.com
| ACIPHEX
SPRINKLE
rabeprazole sodium capsule, delayed release |
||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||
| ACIPHEX
SPRINKLE
rabeprazole sodium capsule, delayed release |
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
| Labeler - Aytu Therapeutics, LLC (117244733) |
More about Aciphex Sprinkle (rabeprazole)
- Check interactions
- Compare alternatives
- Imprints, shape & color data
- Side effects
- Dosage information
- During pregnancy or Breastfeeding
- En español


