Osteoporosis
Medically reviewed by Drugs.com. Last updated on Jan 22, 2024.
What is Osteoporosis?

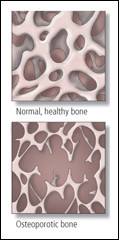
Osteoporosis is a bone disorder. The bones become thinner. They lose some of their strength and are more likely to break. People with osteoporosis have a higher risk of fractures.
Bones can fracture even during everyday movements, such as bending or coughing. The most common osteoporotic fractures occur in the wrist, hip and spine.
Osteoporosis can cause a great deal of suffering, including loss of independence. Death may even occur as the result of complications of an osteoporotic hip fracture.
Osteoporosis is much more common in women than in men. This is because of the hormonal changes that occur during menopause.
Osteoporosis is not a form of arthritis. However, it can cause fractures that lead to arthritis.
|
|
Risk factors
You are more likely to develop osteoporosis if you:
- are female
- are 50 or older
- are postmenopausal
- have a diet low in calcium and/or vitamin D
- have certain medical conditions, such as an intestinal disease that prevents calcium and vitamins from being absorbed, rheumatoid arthritis, or chronic liver disease
- have an overactive thyroid (hyperthyroidism) or take too much thyroid hormone
- lead a sedentary lifestyle
- are thin
- take certain medications, such as prednisone
- are Caucasian or of Asian descent
- smoke
- drink too much alcohol
- have a family history of osteoporosis.
Symptoms
Most people with osteoporosis do not have any symptoms. They do not know they have osteoporosis until they have a bone density test or a fracture.
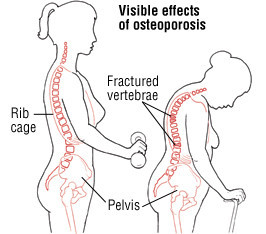
One early sign can be a loss of height caused by curvature or compression of the spine. Curvature or compression is caused by weakened vertebrae (spine bones). The weakened vertebrae develop tiny breaks called compression fractures.
Compression fractures cause the spine bones to collapse vertically. When this happens, the vertebrae become shorter. The shape of each single vertebra goes from a normal rectangle to a more triangular form.
Compression fractures can cause back pain or aching. But the loss of height usually does not cause any symptoms.
|
|
Osteoporosis usually does not cause pain unless a bone is fractured.
Diagnosis
During a physical exam, your doctor may find that you are shorter than you thought you were. Or, your doctor may notice a "dowager's hump." This is a curve of the spine in the upper back that produces a hump.
X-rays may show that your bones are less dense than expected. This could be caused by osteoporosis. But there are also other possible causes, such as not enough vitamin D. Vitamin D deficiency is common and easily diagnosed with a blood test.
Your doctor will suspect osteoporosis if you have had a fragility fracture or other risk factors for the disease.
A bone density test can confirm an osteoporosis diagnosis. Several techniques measure bone density.
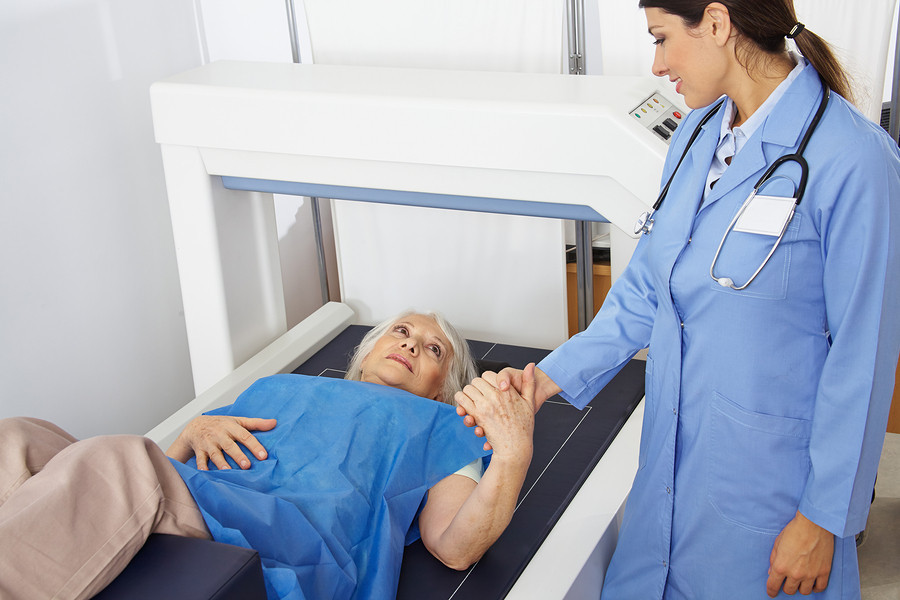
The most accurate bone density test is DEXA (dual-energy X-ray absorptiometry). DEXA takes 10 to 15 minutes and is painless. It uses minimal amounts of radiation and generally is done on the spine and hip.
Other tests are available to screen for osteoporosis, though they are not in widespread use. These include ultrasound of the heel and quantitative computed tomography.
|
|
Expected duration
Osteoporosis is a long-term (chronic) condition. But proper treatment can lead to significant improvements in bone mass. It can decrease the likelihood that a fracture will occur.
Bone mass usually does not return to normal after treatment. But the risk of fracture may decrease dramatically after treatment.
Prevention
You can help to prevent osteoporosis by:
- getting enough calcium and vitamin D
- Eat foods rich in calcium, such as low-fat dairy products, sardines, salmon, green leafy vegetables, and calcium-fortified foods and beverages. Your doctor may also prescribe a calcium supplement.
- You may also need to take a vitamin D supplement or a daily multivitamin.
- regularly doing weight-bearing exercises
- not smoking
- avoiding excess alcohol
- limiting the dose and length of time you take medications (such as prednisone) that increase the risk of osteoporosis.
If you are a woman who has recently entered menopause, talk to your doctor about being evaluated for osteoporosis.
Drugs used to treat this and similar conditions
Preventive medications
There are several medications to prevent menopause-related osteoporosis. These include:
- estrogen replacement therapy (not routinely recommended due to the risks of this treatment)
- raloxifene (Evista), tamoxifen (Soltamox), or bazedoxifene-CEE (Duavee, which combines a medication similar to raloxifene with estrogen). Raloxifene and bazedoxifene behave like estrogen on bone to increase bone density.
- alendronate (Fosamax)
- ibandronate (Boniva)
- risedronate (Actonel)
- zoledronic acid (Reclast).
Estrogen slows the breakdown of bone. The loss of estrogen during menopause leads to bone loss. Estrogen therapy helps to counteract this process. However, estrogen replacement therapy has fallen out of favor. That is because of side effects, including an increased risk of heart disease and stroke when taken by women more than 10 years past menopause.
Alendronate, ibandronate, risedronate, and zoledronic acid are bisphosphonates. This family of drugs slows down the breakdown of bone. They can help bone to become thicker.
If a bone density test shows signs of a problem, it may help you to decide whether to begin taking a preventive medication. You should also measure your height every year, especially if you are a woman older than age 40.
Too much thyroid medication may lead to osteoporosis and other medical problems. Monitor thyroid medication regularly if you take it.
If you take prednisone, work with your doctor to reduce the dose to the lowest possible amount or to discontinue the medication.
Treatment
Doctors initially treat osteoporosis by:
- making sure the person gets enough calcium and vitamin D daily (through the diet and supplements)
- recommending weight-bearing exercises
- modifying other risk factors.
For women, many medications are available to treat osteoporosis. These include:
- Bisphosphonates. These are the drugs used most often to treat osteoporosis in postmenopausal women. Bisphosphonates inhibit the breakdown of bone. They may even increase bone density. Most are taken as a tablet by mouth, but some may be given intravenously. Bisphosphonates can cause side effects. These include nausea, abdominal pain, irritation of the esophagus, and difficulty swallowing. One rare but serious side effect is death of the jawbone caused by poor blood supply. Bisphosphonates include:
- alendronate (Fosamax)
- risedronate (Actonel)
- ibandronate (Boniva)
- pamidronate (Aredia)
- xoledronic acid (Reclast, Zometa).
- Selective estrogen receptor modulators (SERMs). SERM s treat osteoporosis by mimicking the effects of estrogen to increase bone density.
- raloxifene (Evista)
- Calcitonin (Miacalcin). Calcitonin is a hormone produced by the thyroid gland. It is given as a nasal spray or by injection. Although calcitonin inhibits bone breakdown, it is not a preferred medication for osteoporosis given the limited information regarding effectiveness compared with other options.
- Teriparatide (Forteo) and abaloparatide (Tymlos). Teriparatide and abaloparatide are forms of parathyroid hormone, which stimulates the growth of new bone. Teriparatide and abaloparatide are given by a daily injection. Long-term treatment (for more than 2 years) is not recommended.
- Denosumab (Prolia). Denosumab is a monoclonal antibody, a type of biological therapy. It is an antibody that targets a protein involved in bone breakdown. By attacking this protein, it helps stop bone loss. Denosumab may cause very low blood calcium levels in people with advanced chronic kidney disease, especially those on dialysis.
- Romosozumab (Evenity). Romosozumab is another monoclonal available for women with very severe osteoporosis, usually considered after a woman has had a fragility fracture. It acts by blocking sclerostin, a protein that inhibits bone formation.
Long-term estrogen therapy can help slow the breakdown of bone. However, it is rarely recommended solely for the prevention or treatment of osteoporosis because the risks usually outweigh the potential benefits. The risks of long-term estrogen therapy include an increased risk of heart disease, stroke, breast cancer, and gallstones.
Among men, advanced age and low levels of testosterone are the most common risk factors for developing osteoporosis. Testing can reveal if testosterone levels are low. In this case, other tests will look for the cause so that treatment can be started, including testosterone therapy. Men also can be treated with a bisphosphonate or teriparatide.
Your doctor will monitor how well your treatment is working. He or she will do this by taking bone density measurements every one to two years.
Treating fractures
If a person with osteoporosis fractures a hip, surgery may be needed. Surgery will realign and stabilize the hip.
A wrist fracture may heal well simply by being put in a cast. Sometimes surgery may be needed to restore proper alignment of the bones.
Other treatments for fracture include pain medication and rest for a short time.
Calcitonin injections may reduce spine pain from a new compression fracture.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
When to call a professional
Review your options for evaluation and treatment with your doctor if you have:
- risk factors for osteoporosis
- had a fracture with little or no trauma.
Prognosis
The outlook for people with osteoporosis is good, especially if the problem is detected and treated early. Bone density, even in severe osteoporosis, generally can be stabilized or improved. The risk of fractures can be substantially reduced with treatment.
People with mild osteoporosis have an excellent outlook. Those who have a fracture can expect their bones to heal normally. The pain usually goes away within a week or two.
In some people, osteoporosis has a clear cause. The outlook is especially good if the cause is identified and corrected.
Additional info
National Institutes of Health
Osteoporosis and Related Bone Diseases
Learn more about Osteoporosis
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.