Venous Insufficiency
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
Venous insufficiency is a condition that prevents blood from flowing out of your legs and back to your heart. Veins contain valves that help blood flow in one direction. Venous insufficiency means the valves do not close correctly or fully. Blood flows back and pools in your leg. This can cause problems such as varicose veins. Venous insufficiency may also be called chronic venous insufficiency or venous stasis.
DISCHARGE INSTRUCTIONS:
Seek care immediately if:
- You have a wound that does not heal or is infected.
- You have an injury that has broken your skin and caused your varicose veins to bleed.
- Your leg is swollen and hard.
- You have pain in your leg that does not go away or gets worse.
- Your legs or feet are turning blue or black.
- Your leg feels warm, tender, and painful. It may look swollen and red.
Call your doctor if:
- You have a fever.
- You have varicose veins and they are painful.
- You have new or worsening leg pain, swelling, or redness.
- You have new or worsening ulcers or other sores on your leg.
- You have questions or concerns about your condition or care.
Related medications
Medicines:
- Medicines may be given treat a bacterial infection or to reduce swelling or itching. You may need to apply a topical medicine to a skin ulcer.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Manage venous insufficiency:
- Wear a compression device as directed. Examples include pressure stockings, intermittent pneumatic compression, and sequential compression devices. A compression device puts pressure on your lower legs to help keep blood from pooling in your leg veins. Your healthcare provider can prescribe the right device for you. Do not buy over-the-counter devices unless your provider says it is okay. They may not fit correctly or may have elastic that cuts off your circulation. Ask your provider when to start wearing a compression device and how long to wear it.
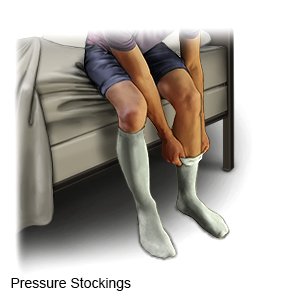
- Do not sit or stand for long periods of time. If you have to sit for a long time, flex and extend your legs, feet, and ankles. Do this about 10 times every 30 minutes to help keep blood flowing. If you have to stand for a long time, take breaks and sit with your legs elevated.
- Elevate your legs. Elevate your legs above the level of your heart to reduce swelling. Your healthcare provider may recommend that you keep your legs elevated for 30 minutes at a time. You may need to do this 3 to 4 times per day, or more if your healthcare provider recommends.

- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can cause blood vessel damage. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
- Reach or maintain a healthy weight. Extra weight can make venous insufficiency worse. Ask your healthcare provider what a healthy weight is for you. He or she can help you create a weight loss plan if you need to lose weight.
- Exercise as directed. Walking can help increase blood flow in your calves. Ask your healthcare provider how much exercise you need each day and which exercises are best for you.

- Care for your skin. Keep your skin clean. Do not use any soaps or lotions that may dry your skin. For example, do not use products that contain fragrance or alcohol. If you have a skin ulcer, your healthcare provider may recommend a wet-to-dry bandage. To do this, apply a wet bandage to your wound and allow it to dry. This will help remove drainage from your wound each time you change the bandage. Your healthcare provider will tell you how often to change your bandage and which kind of bandage to use. Check your wound for signs of infection, such as swelling or pus.
- Go to physical therapy (PT) as directed. A physical therapist can help you increase movement and range of motion in your legs.
Follow up with your doctor as directed:
Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
