Urinary Sphincter Replacement
Medically reviewed by Drugs.com. Last updated on Jun 30, 2025.
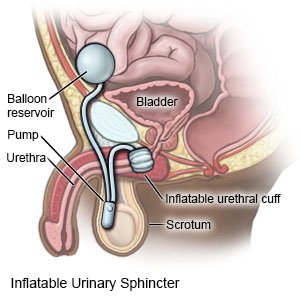
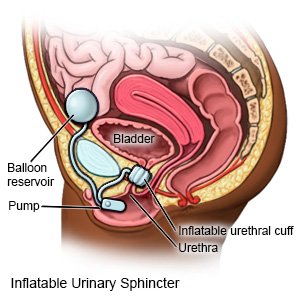
Urinary sphincter replacement is surgery to replace your urinary sphincter with an artificial urinary sphincter (AUS). The urinary sphincter is a muscle that surrounds your urethra. The sphincter squeezes the urethra to keep urine in the bladder until it is time to urinate. An AUS device has a balloon reservoir, a cuff, and a pump. When the AUS is turned on, liquid inside the balloon flows into the cuff. When the cuff is filled, it squeezes your urethra to prevent urine from leaking out of your bladder. To urinate, you press the pump. This relaxes the cuff and allows urine to flow out of your bladder.
 |
 |
DISCHARGE INSTRUCTIONS:
Seek care immediately if:
- You cannot urinate.
- You cannot find the pump to open your AUS.
- Urine is leaking from your surgery area.
Call your doctor or surgeon if:
- You have a fever.
- Your surgery area is red, swollen, or draining pus.
- You have pain when you urinate, or you see blood in your urine.
- You have to press the pump more times than usual to open the AUS.
- Your AUS cuff is on and closed, but you keep leaking urine.
- You do not think you are emptying your bladder completely when you urinate.
- You have questions or concerns about your condition or care.
Medicines:
You may need any of the following:
- Antibiotics help prevent or treat a bacterial infection.
- Prescription pain medicine may be given. Ask your healthcare provider how to take this medicine safely. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your healthcare provider how to prevent or treat constipation.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Related medications
VESIcare
Vesicare is used to treat symptoms of overactive bladder such as incontinence and frequent ...
Myrbetriq
Myrbetriq (mirabegron) is used to treat overactive bladder with symptoms of frequent or urgent ...
Botox
Botox is used cosmetically to reduce facial lines and wrinkles and for medical purposes for ...
OnabotulinumtoxinA
OnabotulinumtoxinA information from Drugs.com, includes OnabotulinumtoxinA side effects ...
Darifenacin
Darifenacin is used for overactive bladder, urinary frequency, urinary incontinence
Solifenacin
Solifenacin (Vesicare) is used to treat overactive bladder symptoms such as frequent or urgent ...
Tolterodine
Tolterodine is used for overactive bladder, urinary frequency, urinary incontinence
Toviaz
Toviaz (fesoterodine) is used to treat overactive bladder with symptoms of urinary frequency ...
Care for the surgery area:
When your healthcare provider says it is okay to bathe, carefully wash the area with soap and water. Dry the area and put on new, clean bandages as directed. Change your bandages when they get wet or dirty.
Activity:
Avoid activities and exercises that put pressure on your genital area. Ask your healthcare provider or surgeon which activities are best for you. Do not have sex for at least 6 weeks after surgery. This gives the surgery area time to heal. Ask when you can return to work and other daily activities.
When to turn off your AUS:
Turn off your AUS as directed. You may need to turn off your AUS at the following times:
- At night to decrease pressure on your urethra and prevent damage
- For procedures that involve your urinary system
- If you are a woman, the last 3 months of pregnancy to prevent cuff damage from the baby's head
Follow up with your doctor or surgeon as directed:
You will need to return to have your surgery area checked and to have the AUS turned on. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
