Ovarian Abscess
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is an ovarian abscess?
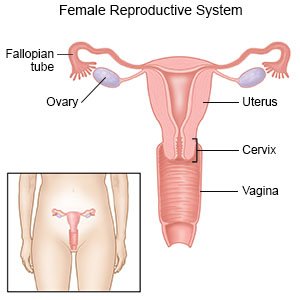
An ovarian abscess is a pus-filled pocket in an ovary. An ovarian abscess is usually caused by bacteria that travel from another part of your body. The bacteria can also travel up your vagina and move into your uterus through your cervix. Bacteria infect the ovary or part of the fallopian tube next to the ovary. An abscess that starts in a fallopian tube and spreads to the ovary is called a tuboovarian abscess (TOA). Less commonly, the abscess can start in the ovary and not involve the fallopian tube.
 |
What increases my risk for an ovarian abscess?
- Pelvic inflammatory disease (PID)
- Unprotected sex, sex with more than one partner, or sex during adolescence
- Anything that weakens your immune system, such as diabetes, HIV/AIDS, or chemotherapy
- Infertility treatment that involved stimulating your ovaries
- Diverticulitis, appendicitis, or inflammatory bowel disease
- An infection in your pelvis after surgery, or an infection that travels through your bloodstream
- Use of an intrauterine device (IUD) to prevent pregnancy
What are the signs and symptoms of an ovarian abscess?
- Pain or ache in your abdomen or pelvis, or pain that worsens with activity or during sex
- Tender area in your lower abdomen
- Heavy monthly periods, spotting, or vaginal bleeding between periods
- Vaginal discharge
- Nausea or vomiting
- Lower back pain
- Fatigue or fever
How is an ovarian abscess diagnosed?
Your healthcare provider will ask about your symptoms and when they started. Tell your healthcare provider about any medical conditions (such as PID) or surgeries you have had. Tell your healthcare provider about any sexually transmitted infections (STIs) that you or your partner may have. You may be given a pregnancy test as well as any of the following:
- A bimanual vaginal exam is used to examine your cervix and ovaries. Your healthcare provider will insert 2 gloved fingers into your vagina and place the other hand on your abdomen. Your healthcare provider will feel for your cervix and ovaries while pressing down lightly on your abdomen. If you feel pain, you may have PID.
- Blood and urine tests may be used to check for infection. The tests may also show if another condition is causing your symptoms.
- A culture or smear test is used to take a sample of discharge from your vagina or cervix to be tested.
- An ultrasound or CT may be used to show pictures of your ovary and abscess. The pictures may help confirm that you have an abscess and how large it is. You may be given contrast liquid before a CT scan to help the abscess show up better. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid.
- Laparoscopy is surgery to look directly at your uterus, ovaries, and fallopian tubes. A scope is put into your abdomen through a small incision. You may have one or more incisions in or below your bellybutton. Ask your healthcare provider for more information about this surgery.
Related medications
How is an ovarian abscess treated?
An ovarian abscess may need to be treated in the hospital. You may need any of the following:
- Antibiotics are given to fight a bacterial infection. You may get antibiotics through an IV for several days.
- Drainage is a procedure used to drain the bacteria from your ovary. Drainage may be done through a needle or during surgery. The area that had the abscess will then be cleaned out.
- A hysterectomy may be needed if the infection spreads from the ovary. You may need to have one or both ovaries removed. Your fallopian tubes and uterus may also need to be removed. A hysterectomy will prevent you from being able to become pregnant. Talk to your healthcare provider about other treatment options if you want to have children.
- Surgery may be used to remove the abscess. Surgery will be necessary if the abscess ruptures. A ruptured ovarian abscess is a life-threatening emergency that needs immediate treatment.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
What can I do to manage an ovarian abscess?
- Do not have sex until your healthcare provider says it is okay. You will need to finish treatment before it is safe to have sex.
- Do not have unprotected sex. Always use a latex condom. Do not have sex while you or your partners are being treated for an STI.
- Talk to your sex partners. If you have an STI, tell your recent partners. Tell them to see a healthcare provider for testing and treatment. This will help stop the spread of infection to others or back to you.
When should I seek immediate care?
- You have sudden, severe abdominal or pelvic pain.
- Your heartbeat or breathing is faster than normal for you.
- You have heavy vaginal bleeding and feel lightheaded.
- You have new or worsening pain.
When should I contact my healthcare provider?
- You have nausea or are vomiting.
- Your pain does not get better even after you take pain medicine.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Ovarian Abscess
- Antibiotic Resistance: The Top 10 List
- Antibiotics 101: Common Names, Types & Their Uses
- Antibiotics For UTI Treatment - What Are My Options?
- Antibiotics and Birth Control Pill Interactions
- Anticholinergic Drugs to Avoid in the Elderly
- Can You Drink Alcohol with Antibiotics?
- Common Side Effects from Antibiotics, and Allergies and Reactions
- Why Don’t Antibiotics Kill Viruses?
Treatment options
Care guides
- Pelvic Inflammatory Disease
- Sexually Transmitted Diseases
- Sexually Transmitted Diseases in Adolescents
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
