Hysterosalpingography
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
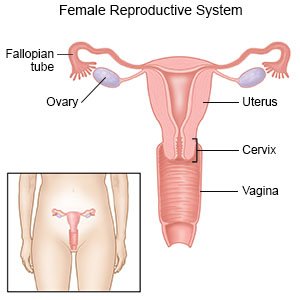
Hysterosalpingography is a procedure to look inside your uterus and fallopian tubes.
 |
DISCHARGE INSTRUCTIONS:
Call your local emergency number (911 in the US) if:
- You have sudden breathing problems, hives, or other signs of an allergic reaction to the contrast liquid.
Seek care immediately if:
- You feel something is bulging into your vagina and not going back.
- You have stomach pain that does not go away even after you take pain medicine.
- You have blood in your urine.
- You have pain when you urinate or have sex.
- You have pus or a foul-smelling odor coming from your vagina.
Related medications
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Call your doctor or gynecologist if:
- You have a fever.
- You have chills, a cough, or feel weak and achy.
- You have nausea or are vomiting.
- Your pads become soaked with blood.
- Your skin is itchy, swollen, or has a rash.
- You are urinating less often than usual.
- You have questions or concerns about your condition or care.
Medicines:
- Prescription pain medicine may be given. Ask your healthcare provider how to take this medicine safely. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your healthcare provider how to prevent or treat constipation.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Vaginal care:
You may need to use sanitary pads for 1 to 2 days if you have some spotting. Some leftover contrast liquid may also come out of your vagina. When you arrive home, carefully wash your vulva with soap and water. Then put on a clean sanitary pad. Change your pad as needed. Ask for more information about vaginal care.
Follow up with your doctor or gynecologist as directed:
Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
