Emphysema
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is emphysema?
Emphysema is a long-term lung disease. Emphysema is part of a group of lung diseases called chronic obstructive pulmonary disease (COPD). Emphysema damages the alveoli (air sacs) in your lungs. This makes it hard for your lungs to send oxygen to the rest of your body.
 |
What increases my risk for emphysema?
- Smoking, or secondhand smoke
- A past lung infection or lung condition
- Irritants such as dust, chemicals, or air pollution
- A genetic condition called alpha-1 antitrypsin (AAT) deficiency
What are the signs and symptoms of emphysema?
You may have any of the following, depending on how severe your emphysema is:
- Shortness of breath that gets worse with activity, such as climbing stairs
- A cough with or without sputum
- A bluish tint to your skin, lips, or nails
- Weight loss without trying
- Barrel chest (rounded, bulging chest)
- Wheezing
How is emphysema diagnosed?
Your healthcare provider will ask about your symptoms and listen to your lungs. Your provider will ask if you smoke or are exposed to smoke, air pollution, dust, or chemicals.
- Blood tests measure the amount of oxygen, acids, and carbon dioxide in your blood. They will also show if you have an infection.
- A chest x-ray may show any changes or problems in your lungs.
- Pulmonary function tests (PFTs) measure how well your lungs exchange gases and how much air your lungs can hold. PFTs can also show if your lungs respond to certain medicines.
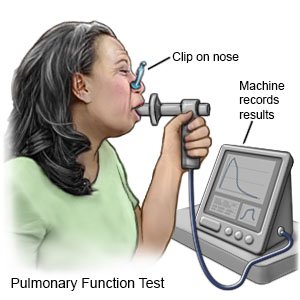
How is emphysema treated?
- Medicines may open your airways, decrease swelling and inflammation in your lungs, or treat an infection. You may need 2 or more medicines. A short-acting medicine relieves symptoms quickly. Long-acting medicines will control or prevent symptoms. Ask your provider how to use your medicines safely.
- Extra oxygen may help you breathe easier and feel more alert if your oxygen level is low.
- Surgery or a procedure may be done if other treatments do not work. Ask your provider about surgery or procedure options.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Related medications
What is an exacerbation of emphysema?
An exacerbation is when your symptoms suddenly get worse. You may have a harder time breathing, your cough may get worse, and you may cough up more sputum. You may have a fever, an increased heart rate, or feel more tired. An exacerbation may be caused by a lung infection, air pollution, or other lung irritants. Sometimes the cause of an exacerbation is not known.
How can I help prevent an exacerbation?
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can cause lung damage. Ask your provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your provider before you use these products.
- Avoid irritants when possible. Wear protective gear if your workplace has dust or chemicals that bother you. Avoid secondhand smoke. Stay inside when air quality is poor. Cover your mouth and nose when you are outside in cold weather or poor air quality.
- Go to pulmonary rehabilitation (rehab), as directed. Pulmonary rehab is a program to help you manage your symptoms and improve your quality of life. It may include nutritional counseling and exercise to strengthen your lungs.
- Get recommended vaccines. Get the flu vaccine as soon as recommended each year, usually in September or October. Get all recommended COVID-19 vaccine doses and booster shots. The pneumonia vaccine may also be recommended. Ask about other vaccines you may need, and when to get them.
- Prevent the spread of germs. Avoid people who are sick. Cover your mouth when you cough. Cough into a tissue or the bend of your elbow so you do not spread germs from your hands. Wash your hands often. Use soap and water. Wash your hands after you use the bathroom, change a child's diapers, or sneeze. Wash before you prepare or eat food.

- Eat a variety of healthy foods. Healthy foods include fruits, vegetables, whole-grain breads, low-fat dairy products, beans, lean meats, and fish. You may need to eat foods that have extra calories, fat, vitamins, or calcium. Ask your provider if you need to be on a special diet.

What can I do to manage my symptoms?
- Check your oxygen level as directed. You may need to check your blood oxygen level with a device called a pulse oximeter. The device shows your heart rate and the percentage of oxygen in your blood. You may be given an oxygen level goal for when you are at rest and another goal for activity. Your provider can tell you how often to check during the day.

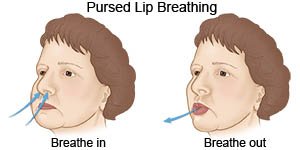
- Use pursed-lip breathing. Pursed-lip breathing can be used any time you feel short of breath. It can also be helpful before you start an activity.
- Count to 2 while you take a deep breath in through your nose.
- Slowly breathe out through your mouth with your lips slightly puckered. You should make a quiet hissing sound as you breathe out.
- Repeat this exercise 4 or 5 times a day. When you are used to doing pursed-lip breathing, you can use it any time you need more air.
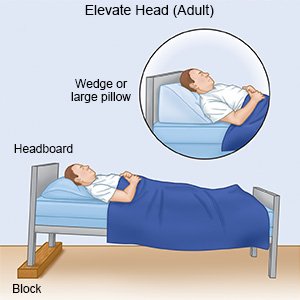
- Rest or sleep with your head elevated. This will help keep your airway open. Use foam wedges or elevate the head of your bed. Use a device that will tilt your whole body, or bend your body at the waist. The device should not bend your body at the upper back or neck.
Call your local emergency number (911 in the US) if:
- You have any of the following signs of a heart attack:
- Squeezing, pressure, or pain in your chest
- You may also have any of the following:
- Discomfort or pain in your back, neck, jaw, stomach, or arm
- Shortness of breath
- Nausea or vomiting
- Lightheadedness or a sudden cold sweat
When should I seek immediate care?
- You have shortness of breath that is so severe you cannot talk.
- You cough up blood.
- You are confused, dizzy, or feel like you may pass out.
When should I call my doctor or pulmonologist?
- You have trouble reaching your oxygen level goal.
- You have a fever.
- You have trouble doing your usual activities because it is hard to breathe.
- You need to use your inhalers or take breathing treatments more often than usual.
- You cough up more sputum than is normal for you.
- You wheeze more than is normal for you.
- Your legs or ankles are swollen.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Emphysema
Treatment options
Care guides
Symptoms and treatments
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
