Atherectomy
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
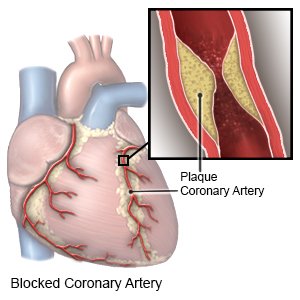
Atherectomy is a procedure used to remove plaque that narrows or blocks your arteries. Plaque is fat, cholesterol, or tissues that build up on the inner artery wall. Blood flow is decreased when plaque builds up and narrows the arteries. Decreased blood flow can cause chest pain or a heart attack.
 |
WHILE YOU ARE HERE:
Before your procedure:
- Informed consent is a legal document that explains the tests, treatments, or procedures that you may need. Informed consent means you understand what will be done and can make decisions about what you want. You give your permission when you sign the consent form. You can have someone sign this form for you if you are not able to sign it. You have the right to understand your medical care in words you know. Before you sign the consent form, understand the risks and benefits of what will be done. Make sure all your questions are answered.
- An IV is a small tube placed in your vein that is used to give you medicine or liquids.
- Local anesthesia is a shot of medicine put into your skin to numb the area and dull the pain. You may still feel pressure or pushing during the procedure, but you should not feel pain.
During your procedure:
A small incision will be made in your groin, arm, or wrist. A catheter will be inserted into your artery and moved to the blockage. You may be given dye so your surgeon can see the blockage clearly. He or she will use a cutting device to remove the plaque from your artery. Your incision will be closed with stitches.
Related medications
After your procedure:
- You will need to lie flat and still for a few hours. Healthcare providers will get you up to walk as soon as possible to help prevent blood clots.
- A bandage or pressure device may be put on your incision area to prevent bleeding.
- Medicines may be given to manage pain or nausea. Antiplatelets, such as aspirin, may be given to help prevent blood clots.
RISKS:
Your artery may be damaged or tear. Your arteries may become completely blocked during the procedure. This stops blood flow and may lead to a heart attack. You may need coronary artery bypass graft surgery. You may get a blood clot in your limb. This may become life-threatening.
CARE AGREEMENT:
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Atherectomy
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
