Acute Headache
Medically reviewed by Drugs.com. Last updated on Sep 23, 2025.
AMBULATORY CARE:
An acute headache
is pain or discomfort that may start suddenly and get worse quickly. You may have an acute headache only when you feel stress or eat certain foods. Other acute headache pain can happen every day, and sometimes several times a day. The cause of an acute headache may not be known. It may be triggered by stress, fatigue, hormones, food, or trauma.
Common types of acute headache:
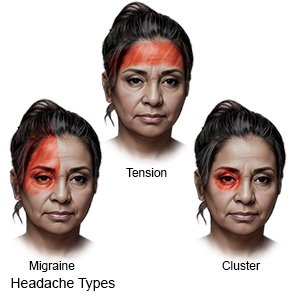
- Tension headache is the most common type of headache. These headaches typically occur in the late afternoon and go away by evening. The pain is usually mild or moderate. You may have problems tolerating bright light or loud noise. The pain is usually across the forehead or in the back of the head, often only on one side. These headaches may occur every day.
- Migraine headaches cause moderate or severe pain. The headache generally lasts from 1 to 3 days and tends to come back. Pain is usually on only one side, but it may change sides. Migraines often occur in the temple, the back of the head, or behind the eye. The pain may throb or be sharp and steady.
- A migraine with aura means you see or feel something before a migraine. You may see a small spot surrounded by bright zigzag lines. Other signs or symptoms may follow the aura.
- Cluster headache pain is usually only on one side. It often causes severe pain, and can last for 30 minutes to 2 hours. These headaches may occur 1 or 2 times each day, more often at night. The pain may wake you.
 |
Seek care immediately if:
- You have severe pain.
- You have numbness or weakness on one side of your face or body.
- You have a headache that occurs after a blow to the head, a fall, or other trauma.
- You have a headache, are forgetful or confused, or have trouble speaking.
- You have a headache, stiff neck, and a fever.
Call your doctor if:
- You have a constant headache and are vomiting.
- You have a headache each day that does not get better, even after treatment.
- You have changes in your headaches, or new symptoms that occur when you have a headache.
- You have questions or concerns about your condition or care.
Related medications
Treatment:
- Medicine may be given to decrease pain. The medicine your healthcare provider recommends will depend on the kind of headaches you have. You will need to take prescription headache medicines as directed to prevent a problem called rebound headache. These headaches happen with regular use of pain relievers for headache disorders. NSAIDs or acetaminophen may help some kinds of headaches.
- Biofeedback may help you learn how to change stress reactions. For example, you learn to slow your heart rate when you become upset. You may also learn to prevent certain headaches by combining heat with relaxation.
- Cognitive behavior therapy, or stress management, may be used with other therapies to prevent headaches.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Manage your symptoms:
- Apply heat or ice on the headache area. Use a heat or ice pack. For an ice pack, you can also put crushed ice in a plastic bag. Cover the pack or bag with a towel before you apply it to your skin. Ice and heat both help decrease pain, and heat helps decrease muscle spasms. Apply heat for 20 to 30 minutes every 2 hours. Apply ice for 15 to 20 minutes every hour. Apply heat or ice for as long and for as many days as directed. You may alternate heat and ice.
- Relax your muscles. Lie down in a comfortable position and close your eyes. Relax your muscles slowly. Start at your toes and work your way up your body.
- Keep a record of your headaches. Write down when your headaches start and stop. Include your symptoms and what you were doing when the headache began. Record what you ate or drank for 24 hours before the headache started. Describe the pain and where it hurts. Keep track of what you did to treat your headache and if it worked.
Prevent an acute headache:
- Avoid anything that triggers an acute headache. Examples include exposure to chemicals, going to high altitude, or not getting enough sleep. Create a regular sleep routine. Go to sleep at the same time and wake up at the same time each day. Do not use electronic devices before bedtime. These may trigger a headache or prevent you from sleeping well.
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can trigger an acute headache or make it worse. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
- Limit alcohol as directed. Alcohol can trigger an acute headache or make it worse. If you have cluster headaches, do not drink alcohol during an episode. For other types of headaches, ask your healthcare provider if it is safe for you to drink alcohol. Ask how much is safe for you to drink, and how often.
- Exercise as directed. Exercise can reduce tension and help with headache pain. Aim for 30 minutes of physical activity on most days of the week. Your healthcare provider can help you create an exercise plan.
- Eat a variety of healthy foods. Healthy foods include fruits, vegetables, low-fat dairy products, lean meats, fish, whole grains, and cooked beans. Your healthcare provider or dietitian can help you create meals plans if you need to avoid foods that trigger headaches.
Follow up with your healthcare provider as directed:
Bring your headache record with you when you see your healthcare provider. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Acute Headache
- Advil Dosage Charts for Infants and Children
- Dosage Charts for Infants and Children
- Motrin Dosage Charts for Infants and Children
- Top 9 Things You Must Know About Naproxen
- Tylenol Dosage Charts for Infants and Children
- What are the risks of mixing pain medications and alcohol?
Treatment options
Care guides
Symptoms and treatments
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
