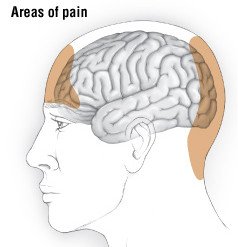
Tension headache
Medically reviewed by Drugs.com. Last updated on Jun 17, 2025.
What is a Tension headache?

Tension headaches are the most common type of headache. These headaches are not caused by disease. They are often considered to be "normal" headaches. Other names for tension headaches are ordinary headaches, muscle tension headaches, and stress headaches.
The International Headache Society has suggested that doctors use the term tension-type headaches because so many different names have been used for tension headaches. Typically tension-type headache causes mild to moderate pain, usually on both sides of the head. There is a pressing or tightening sensation. It is not pulsating and is not accompanied by nausea. The headache does not get worse with routine physical activity.
The society has defined different categories based upon how frequently tension-type headaches occur and how persistent they are:
- infrequent episodes of tension-type headache
- less than 12 episodes per year
- each episode may last from 30 minutes to seven days
- frequent episodes of tension-type headache
- between one and 14 episodes per month on average
- each episode may last from 30 minutes to seven days
- chronic (persistent) tension-type headache
- at least 15 episodes per month on average
- the headache lasts for hours and it may be continuous
- mild nausea may occur some of the time.
The exact cause of tension headaches is unknown. But there appear to be several contributing factors.
In part, they result from changes in how the nerves of the head, neck and shoulders sense pain. They are also caused by changes in the brain's interpretation of the pain signals sent from the muscles in the head and neck. Emotional stress and muscular tension also probably act as triggers.
Symptoms
The main symptom of a tension headache is a sense of tightness around the head. This is sometimes described as a "tight hat-band" or "vise" sensation.
Neck and shoulder muscles are often tense and sore to the touch. The person may have trouble concentrating and difficulty sleeping.
A person can have both migraine and tension-type headaches. And the symptoms of tension-type headaches and migraine headaches can overlap. For example, both types of headaches may be made worse by bright lights or loud noises. In general, migraine headaches tend to be throbbing. Tension-type headaches cause a more constant pain. But the pain of a migraine or tension-type headache can be steady or throbbing or alternate between the two.
|
|
Diagnosis
There is no specific test to confirm the diagnosis of a tension-type headache. The diagnosis is determined by your description of the headache, other medical history and a normal physical examination.
A computed tomography (CT) scan or magnetic resonance imaging (MRI) scan of the head may be ordered. These imaging tests may be used to investigate headache pain that is associated with unexpected or unusual symptoms.
Expected duration
An episodic tension-type headache may last only 30 minutes. But it may linger for as long as seven days.
A chronic tension-type headache typically lasts for part or all of the day for most days of the week. The pain can also be continuous. The intensity of pain may fluctuate during that time.
Prevention
Relaxation techniques and avoidance of stressful situations may help to prevent tension-type headaches. Many things can trigger a tension-type headache. Identifying and correcting one or more triggers may reduce headache frequency and severity.
Drugs used to treat this and similar conditions
Treatment
Infrequent episodic tension-type headaches. Over-the-counter pain relievers are convenient, effective and relatively safe. Examples include aspirin, acetaminophen (Tylenol) or ibuprofen (Advil, Motrin). Some people get more pain relief with combination products containing caffeine.
The use of any over-the-counter pain reliever should be limited to no more than two or three days per week. If pain medications are used more frequently, "rebound" headaches may occur on the days that medications are not taken.
Frequent episodic and chronic tension-type headaches. These headaches are more difficult to treat. Rebound headaches are common when pain relievers are stopped. Therapy to prevent the headache before it starts is a better strategy than taking pain relievers after the headache is present. Your doctor may suggest a trial of one of the medications used to prevent frequent migraine attacks, such as a beta-blocker (metoprolol or propranolol) or an antidepressant (amitriptyline or venlafaxine).
Some people are able to treat their tension-type headaches without medications. You can apply an ice compress, heating pad or massage to any tight areas in the neck and shoulders.
Relaxation techniques and deep-breathing exercises may help to decrease the frequency and severity of headaches. Some people get relief with biofeedback or acupuncture.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
When to call a professional
Most headaches are harmless. It's reassuring if you are able to relieve your headache without medications or with only occasional use of a pain reliever.
Headaches are rarely caused by a serious medical problem. However, you should call or visit your doctor if you have:
- a headache that occurs after a head injury
- a headache accompanied by fever or vomiting
- a headache associated with
- blurred vision
- difficulty speaking
- numbness or weakness of the arms or legs
- headaches that are increasing in intensity or frequency over time
- a "thunderclap" headache or headache associated with loss of consciousness
- headaches that require daily use of pain-relieving medications.
Prognosis
Infrequent episodic tension-type headaches can usually be treated successfully with pain relieving medication. But finding the right combination of therapies to relieve frequent episodic and chronic tension-type headaches may take several months. Over time most people will have fewer and less severe headaches.
Additional info
National Institute of Neurological Disorders and Stroke
https://www.ninds.nih.gov/
National Headache Foundation
https://www.headaches.org/
American Migraine Foundation
https://americanmigrainefoundation.org/
Learn more about Tension headache
- Advil Dosage Charts for Infants and Children
- Dosage Charts for Infants and Children
- Motrin Dosage Charts for Infants and Children
- Top 9 Things You Must Know About Naproxen
- Tylenol Dosage Charts for Infants and Children
- What are the risks of mixing pain medications and alcohol?
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.