What Is Insulin
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is insulin?
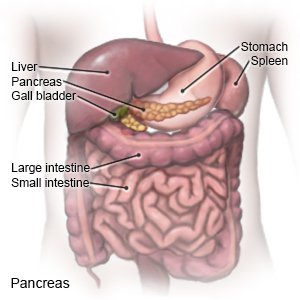
Insulin is a hormone made by the pancreas. Insulin helps remove sugar from your blood. This helps lower your blood sugar level. You may need to take insulin if your pancreas is not making enough. You may need to take insulin if your body cannot use insulin correctly.
 |
What are the different types of insulin?
Several types of insulin are used to lower blood sugar levels. The type tells you how fast the insulin starts to work or how long it lasts in your body. Your diabetes care team provider will help you find the insulin that is right for you:
- Rapid-acting insulin starts to work within 15 minutes. Use this insulin immediately before or after you eat.
- Short-acting, or regular, insulin starts to work within 30 minutes. Use this insulin 30 to 45 minutes before you eat.
- Intermediate-acting insulin starts to work 2 to 4 hours after you use it. It reaches the highest level in your blood about 6 to 8 hours after you use it. This type of insulin helps control your blood sugar level between meals. It is commonly used in the morning, at bedtime, or both.
- Long-acting insulin starts to work 2 to 4 hours after you use it. It can last 24 hours or more in your body. This type of insulin is often used in the morning or at bedtime. It helps control your blood sugar level throughout the day.
- Premixed insulin is a mixture of 2 types of insulin. It usually includes one type to help control your blood sugar level at meals. The other type helps control your blood sugar level between meals and while you sleep.
How is insulin given?
- A needle and syringe are used to inject insulin under the skin. Insulin needles come in different sizes. Ask your diabetes care team provider which needle is best for you. Use the correct size insulin syringe to make sure you get the right dose of insulin.
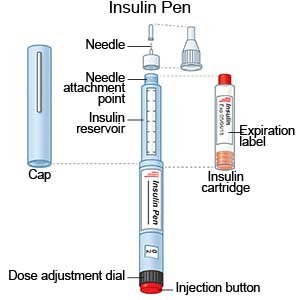
- An insulin pen is used to inject insulin under the skin. It looks like a regular pen but has a short needle on one end. An insulin pen has enough insulin in it for a few injections. Some pens have a cartridge of insulin. You change the cartridge when it is empty. Other pens are thrown away when the case is empty. Change the needle with each dose.
- Insulin jet injectors use strong air pressure to spray insulin through the skin. No needles are used with injectors. Ask your provider how to use your injector.
- An insulin injection port is a tube on your skin. Insulin is injected through the port. The port can stay in place for several days.
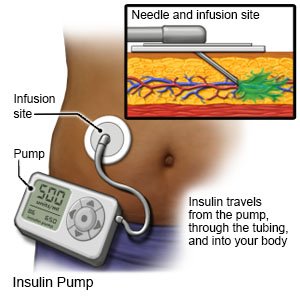
- An insulin pump is worn outside of your body. The pump gives insulin through a small tube attached to a needle under your skin. The pump can give you a constant amount of insulin throughout the day and night. It can also be programmed to give you a dose of insulin with meals.
- Inhaled insulin is powdered insulin that you breathe in from an inhaler device into your mouth. This insulin is only for adults.
Related medications
How should I store insulin and insulin supplies?
Follow the storage directions on the label or package insert that came with the insulin. The following are general guidelines:
- Always keep your insulin and insulin supplies out of the reach of children and animals. Extra insulin can be dangerous for a person who does not need it. Do not share insulin or insulin supplies with anyone.
- Store insulin in the refrigerator or at room temperature. If you store your insulin at room temperature, keep it in a cool, dry place.
- Do not store insulin in the freezer, direct sunlight, or a car. Throw away insulin that has been frozen or exposed to very warm temperatures (above 85°F, or 29.4°C).
- If you travel, keep the insulin in a cool pack. This will help make sure the temperature of the insulin stays below 86°F (30°C). Do not leave insulin in direct sunlight.
How should I throw away insulin and needles?
Do not use your insulin if you see clumps or color changes. Cloudy insulin that has small, white, particles that will not mix should be thrown away. Clear insulin that looks cloudy should be thrown away.
- Ask how to throw away insulin you did not use. Your diabetes care team provider will teach you how to do this safely. You may need to mix it with something before you put it in the trash. This helps make sure no one can use it. Directions will depend on the kind of insulin device used to give insulin.
- Check the expiration date on your insulin bottle before each use. Do not use insulin beyond its expiration date.
- Always throw away your used needles in a hard-sided container with a lid. Some examples include a metal coffee can or laundry detergent bottle.
When should I call my doctor or diabetes care team provider?
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
