Meperidine Injection: Package Insert / Prescribing Info
Package insert / product label
Generic name: meperidine hydrochloride
Dosage form: injection
Drug class: Opioids (narcotic analgesics)
J Code (medical billing code): J2175 (Per 100 mg, injection)
Medically reviewed by Drugs.com. Last updated on Apr 15, 2024.
On This Page
- Indications and Usage
- Dosage and Administration
- Dosage Forms and Strengths
- Contraindications
- Warnings and Precautions
- Adverse Reactions/Side Effects
- Drug Interactions
- Use In Specific Populations
- Drug Abuse and Dependence
- Overdosage
- Description
- Clinical Pharmacology
- Nonclinical Toxicology
- How Supplied/Storage and Handling
- Patient Counseling Information
Highlights of Prescribing Information
MEPERIDINE HYDROCHLORIDE injection, for subcutaneous, intramuscular, and intravenous use, CII
Initial U.S. Approval: 1942
WARNING: SERIOUS AND LIFE-THREATENING RISKS FROM USE OF MEPERIDINE HYDROCHLORIDE INJECTION
See full prescribing information for complete boxed warning.
- Meperidine Hydrochloride Injection exposes users to risks of addiction, abuse, and misuse, which can also lead to overdose and death. Assess patient's risk before prescribing and reassess regularly for these behaviors and conditions. (5.1)
- Serious, life-threatening, or fatal respiratory depression may occur with the use of Meperidine Hydrochloride Injection, especially during initiation or following a dosage increase. To reduce the risk of respiratory depression, proper dosing and titration of Meperidine Hydrochloride are essential (5.2)
- Concomitant use of opioids with benzodiazepines or other central nervous system (CNS) depressants, including alcohol, may result in profound sedation, respiratory depression, coma, and death. Reserve concomitant prescribing for use in patients for whom alternative treatment options are inadequate. (5.3, 7).
- If opioid use is required for an extended period of time in a pregnant woman, advise the patient of the risk of Neonatal Opioid Withdrawal Syndrome, which may be life-threatening if not recognized and treated. Ensure that management by neonatology experts will be available at delivery. (5.4)
- Concomitant use with CYP3A4 inhibitors (or discontinuation of CYP3A4 inducers) can result in fatal overdose of meperidine. (5.5, 7)
- Concomitant use of Meperidine Hydrochloride Injection with Monoamine oxidase (MAO) inhibitors can result in coma, severe respiratory depression, cyanosis and hypotension. Use of Meperidine Hydrochloride Injection with MAO inhibitors is contraindicated. (4, 5.6, 7)
Recent Major Changes
Indications and Usage for Meperidine Injection
Meperidine Hydrochloride Injection is indicated for preoperative medication, support of anesthesia, for obstetrical analgesia, and for the management of pain severe enough to require an opioid analgesic and for which alternative treatments are inadequate. (1)
Limitations of Use (1)
Because of the risks of addiction, abuse, and misuse with opioids, which can occur at any dosage or duration (5.1), reserve Meperidine Hydrochloride Injection for use in patients for whom alternative treatment options [e.g., non-opioid analgesics or opioid combination products]:
- Have not been tolerated, or are not expected to be tolerated
- Have not provided adequate analgesia, or are not expected to provide adequate analgesia
Meperidine Hydrochloride Injection should not be used for an extended period of time unless the pain remains severe enough to require an opioid analgesic and for which alternative treatment options continue to be inadequate.
Use of Meperidine Hydrochloride Injection for an extended period of time may increase the risk of toxicity (e.g., seizures) from the accumulation of the meperidine metabolite, normeperidine.
Meperidine Injection Dosage and Administration
- Meperidine Hydrochloride should be prescribed only by healthcare professionals who are knowledgeable about the use of opioids and how to mitigate the associated risks (2.1)
- Use the lowest effective dosage for the shortest duration consistent with individual patient treatment goals. Reserve titration to higher doses of Meperidine Hydrochloride Injection for patients in whom lower doses are insufficiently effective and in whom the expected benefits of using a higher dose opioid clearly outweigh the substantial risks. (2.1, 5)
- Many acute pain conditions (e.g., the pain that occurs with a number of surgical procedures or acute musculoskeletal injuries) require no more than a few days of an opioid analgesic. Clinical guidelines on opioid prescribing for some acute pain conditions are available. (2.1)
- Initiate the dosing regimen for each patient individually, taking into account the patient’s underlying cause and severity of pain, prior analgesic treatment and response, and risk factors for addiction, abuse, and misuse. (2.1, 5.2)
- Respiratory depression can occur at any time during opioid therapy, especially when initiating and following dosage increases with Meperidine Hydrochloride Injection. Consider this risk when selecting an initial dose and when making dose adjustments. (2.2, 5.3)
- For Relief of Pain:
Titrate the dose based upon the individual patients’ response to their initial dose of Meperidine Hydrochloride Injection (2.2,5) - Adults: 50 mg to 150 mg intramuscularly or subcutaneously every 3 to 4 hours. (2.2)
Children: 0.5 mg/lb to 0.8 mg/lb intramuscularly or subcutaneously up to the adult dose every 3 to 4 hours. (2.2) - Preoperative Medication:
Adults: 50 mg to 150 mg intramuscularly or subcutaneously, 30 to 90 minutes before beginning anesthesia. (2.3)
Children: 0.5 mg/lb to 1 mg/lb intramuscularly or subcutaneously up to the adult dose, 30 to 90 minutes before beginning anesthesia. (2.3) - Obstetrical Analgesia:
50 mg to 100 mg intramuscularly or subcutaneously; may be repeated at 1 to 3 hour intervals. (2.4) - Do not abruptly discontinue Meperidine Hydrochloride Injection abruptly in a physically dependent patient. (2.2)
Dosage Forms and Strengths
-
Single Dose vials: 25 mg/mL, 50 mg/mL and 100 mg/mL. (3)
Contraindications
- Significant respiratory depression. (4)
- Acute or severe bronchial asthma in an unmonitored setting or in absence of resuscitative equipment. (4)
- Concurrent use of monoamine oxidase inhibitors (MAOIs) or use of MAIOs within the last 14 days. (7)
- Known or suspected gastrointestinal obstruction, including paralytic ileus. (4)
- Hypersensitivity to meperidine or to any other ingredients of the product. (4)
Warnings and Precautions
- Opioid-Induced Hyperalgesia and Allodynia: Opioid-Induced Hyperalgesia (OIH) occurs when an opioid analgesic paradoxically causes an increase in pain, or an increase in sensitivity to pain. If OIH is suspected, carefully consider appropriately decreasing the dose of the current opioid analgesic or opioid rotation. (5.7)
- Serotonin Syndrome with Concomitant Use of Serotonergic Drugs: Potentially life-threatening condition could result from concomitant serotonergic drug administration. Discontinue Meperidine Hydrochloride Injection if serotonin syndrome is suspected. (5.8)
- Life-Threatening Respiratory Depression in Patients with Chronic Pulmonary Disease or in Elderly, Cachectic, or Debilitated Patients: Monitor closely, particularly during initiation and titration. (5.9)
- Adrenal Insufficiency: If diagnosed, treat with physiologic replacement of corticosteroids, and wean patient off of the opioid. (5.10)
- Severe Hypotension: Monitor during dosage initiation and titration. Avoid use of Meperidine Hydrochloride Injection in patients with circulatory shock. (5.11)
- Risks of Use in Patients with Increased Intracranial Pressure, Brain Tumors, Head Injury, or Impaired Consciousness: Monitor for sedation and respiratory depression. Avoid use of Meperidine Hydrochloride Injection in patients with impaired consciousness or coma. (5.12)
Adverse Reactions/Side Effects
Most common adverse reactions were lightheadedness, dizziness, sedation, nausea, vomiting and sweating. (6)
To report SUSPECTED ADVERSE REACTIONS, contact Hikma Pharmaceuticals USA Inc. at 1-877-845-0689, or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Drug Interactions
- Mixed Agonist/Antagonist and Partial Agonist Opioid Analgesics: Avoid use with Meperidine Hydrochloride Injection because they may reduce analgesic effect of Meperidine Hydrochloride Injection or precipitate withdrawal symptoms. (7)
Use In Specific Populations
Pregnancy: May cause fetal harm. (8.1)
Geriatric Patients: Use caution during dose selection, starting at the low end of the dosing range while carefully monitoring for side effects. (8.5)
See 17 for PATIENT COUNSELING INFORMATION.
Revised: 4/2024
Full Prescribing Information
WARNING: SERIOUS AND LIFE-THREATENING RISKS FROM USE OF MEPERIDINE HYDROCHLORIDE INJECTION
Addiction, Abuse, and Misuse
Because the use of Meperidine Hydrochloride Injection exposes patients and other users to the risks of opioid addiction, abuse, and misuse, which can lead to overdose and death, assess each patient's risk prior to prescribing and reassess all patients regularly for the development of these behaviors and conditions. [see Warnings and Precautions (5.1)].
Life-Threatening Respiratory Depression
Serious, life-threatening, or fatal respiratory depression may occur with use of Meperidine Hydrochloride Injection, especially during initiation or following a dose increase. To reduce the risk of respiratory depression, proper dosing and titration of Meperidine Hydrochloride Injection are essential. [see Warnings and Precautions (5.2)].
Risks From Concomitant Use with Benzodiazepines Or Other CNS Depressants
Concomitant use of opioids with benzodiazepines or other central nervous system (CNS) depressants, including alcohol, may result in profound sedation, respiratory depression, coma, and death. Reserve concomitant prescribing of Meperidine Hydrochloride Injection and benzodiazepines or other CNS depressants for use in patients for whom alternative treatment options are inadequate. [see Warnings and Precautions (5.3), Drug Interactions (7)].
Neonatal Opioid Withdrawal Syndrome (NOWS)
If opioid use is required for an extended period of time in a pregnant woman, advise the patient of the risk of Neonatal Opioid Withdrawal Syndrome, which may be life-threatening if not recognized and treated. Ensure that management by neonatology experts will be available at delivery. [see Warnings and Precautions (5.4)].
Cytochrome P450 3A4 Interaction
The concomitant use of Meperidine Hydrochloride Injection with all cytochrome P450 3A4 inhibitors may result in an increase in meperidine plasma concentrations, which could increase or prolong adverse reactions and may cause potentially fatal respiratory depression. In addition, discontinuation of a concomitantly used cytochrome P450 3A4 inducer may result in an increase in meperidine plasma concentration. Monitor patients receiving Meperidine Hydrochloride Injection and any CYP3A4 inhibitor or inducer. [see Warnings and Precautions (5.5), Drug Interactions (7)].
Concomitant Use of Meperidine Hydrochloride Injection with Monoamine Oxidase (MAO) Inhibitors
Concomitant use of Meperidine Hydrochloride Injection with monoamine oxidase (MAO) inhibitors can result in coma, severe respiratory depression, cyanosis, and hypotension. Use of Meperidine Hydrochloride Injection with MAO inhibitors within last 14 days is contraindicated [see Contraindications (4), Warnings and Precautions (5.6), Drug Interactions (7)].
1. Indications and Usage for Meperidine Injection
Meperidine Hydrochloride Injection is indicated for preoperative medication, support of anesthesia, and obstetrical analgesia.
Meperidine Hydrochloride Injection is indicated for the management of pain severe enough to require an opioid analgesic and for which alternative treatments are inadequate.
Limitations of Use
Because of the risks of addiction, abuse, and misuse with opioids, which can occur at any dosage or duration [see Warnings and Precautions (5.1)], reserve Meperidine Hydrochloride Injection for use in patients for whom alternative treatment options (e.g., non-opioid analgesics or opioid combination products):
- Have not been tolerated or are not expected to be tolerated
- Have not provided adequate analgesia or are not expected to provide adequate analgesia
Meperidine Hydrochloride Injection should not be used for an extended period of time unless the pain remains severe enough to require an opioid analgesic and for which alternative treatment options continue to be inadequate.
Use of Meperidine Hydrochloride Injection for an extended period of time may increase the risk of toxicity (e.g., seizures) from the accumulation of the meperidine metabolite, normeperidine.
2. Meperidine Injection Dosage and Administration
2.1 Important Dosage and Administration Instructions
- Meperidine Hydrochloride Injection should be prescribed only by healthcare professionals who are knowledgeable about the use of opioids and how to mitigate the associated risks.
- Use the lowest effective dosage for the shortest duration of time consistent with individual patient treatment goals [see Warnings and Precautions (5)]. Because the risk of overdose increases as opioid doses increase, reserve titration to higher doses of Meperidine Hydrochloride Injection for patients in whom lower doses are insufficiently effective and in whom the expected benefits of using a higher dose opioid clearly outweigh the substantial risks.
- Many acute pain conditions (e.g., the pain that occurs with a number of surgical procedures or acute musculoskeletal injuries) require no more than a few days of an opioid analgesic. Clinical guidelines on opioid prescribing for some acute pain conditions are available.
- There is variability in the opioid analgesic dose and duration needed to adequately manage pain due both to the cause of pain and to individual patient factors. Initiate the dosing regimen for each patient individually, taking into account the patient's underlying cause and severity of pain, prior analgesic treatment and response, and risk factors for addiction, abuse, and misuse [see Warnings and Precautions (5.1)].
- Respiratory depression can occur at any time during opioid therapy, especially when initiating and following dosage increases with Meperidine Hydrochloride Injection. Consider this risk when selecting an initial dose and when making dose adjustments [see Warnings and Precautions (5)].
- Inspect Meperidine Hydrochloride Injection for particulate matter and discoloration prior to administration. Do not use if color is darker than pale yellow, if it is discolored in any other way, or if it contains a precipitate.
2.2 For Management of Pain
Initial Dosage
Dosage should be adjusted according to the severity of the pain and the response of the patient. While subcutaneous administration is suitable for occasional use, intramuscular administration is preferred when repeated doses are required. If intravenous administration is required, dosage should be decreased and the injection made very slowly, preferably utilizing a diluted solution.
Adults: Initiate treatment in a dosing range of 50 mg to 150 mg intramuscularly or subcutaneously every 3 to 4 hours as needed for pain, and at the lowest dose necessary to achieve adequate analgesia. Elderly patients should usually be given meperidine at the lower end of the dose range and observed closely.
Titration and Maintenance of Therapy
Titrate the dose based upon the individual patient’s response to their initial dose of Meperidine Hydrochloride Injection. Individually titrate Meperidine Hydrochloride Injection to a dose that provides adequate analgesia and minimizes adverse reactions. Continually reevaluate patients receiving Meperidine Hydrochloride Injection to assess the maintenance of pain control, signs and symptoms of opioid withdrawal, and other adverse reactions, as well as to reassess for the development of addiction, abuse, or misuse [see Warnings and Precautions (5.1, 5.15)]. Frequent communication is important among the prescriber, other members of the health and care team, the patient, and the caregiver/family during periods of changing analgesic requirements, including initial titration.
If the level of pain increases after dosage stabilization, attempt to identify the source of increased pain before increasing the Meperidine Hydrochloride Injection dosage. If after increasing the dosage, unacceptable opioid-related adverse reactions are observed (including an increase in pain after a dosage increase), consider reducing the dosage [see Warnings and Precautions (5)]. Adjust the dosage to obtain an appropriate balance between management of pain and opioid-related adverse reactions.
Discontinuation of Meperidine Hydrochloride Injection
When a patient who has been taking Meperidine Hydrochloride Injection regularly and may be physically-dependent no longer requires therapy with Meperidine Hydrochloride Injection, taper the dose gradually, by 25% to 50% every 2 to 4 days, while monitoring carefully for signs and symptoms of withdrawal. If the patient develops these signs or symptoms, raise the dose to the previous level and taper more slowly, either by increasing the interval between decreases, decreasing the amount of change in dose, or both. Do not abruptly discontinue Meperidine Hydrochloride Injection in a physically-dependent patient [see Warnings and Precautions (5.15), Drug Abuse and Dependence (9.3)].
2.3 For Preoperative Medication
2.4 For Support of Anesthesia
Repeated slow intravenous injections of fractional doses (e.g., 10 mg/mL) or continuous intravenous infusion of a more dilute solution (e.g., 1 mg/mL) should be used. The dose should be titrated to the needs of the patient and will depend on the premedication and type of anesthesia being employed, the characteristics of the particular patient, and the nature and duration of the operative procedure. Elderly patients should usually be given meperidine at the lower end of the dose range and observed closely.
2. 5 For Obstetrical Analgesia
The usual dosage is 50 mg to 100 mg intramuscularly or subcutaneously when pain becomes regular, and may be repeated at 1- to 3-hour intervals.
2.6 Dosage Modifications with Concomitant Phenothiazines
The dose of Meperidine Hydrochloride Injection should be proportionately reduced (usually by 25 to 50 percent) when administered concomitantly with phenothiazines and many other tranquilizers since they potentiate the action of Meperidine Hydrochloride Injection.
4. Contraindications
Meperidine Hydrochloride Injection is contraindicated in patients with:
- Significant respiratory depression [see Warnings and Precautions (5.2)]
- Acute or severe bronchial asthma in an unmonitored setting or in the absence of resuscitative equipment [see Warnings and Precautions (5.2)]
- Concomitant use of monoamine oxidase inhibitors (MAOIs) or use of MAOIs within the last 14 days [see Warnings and Precautions (5.6), Drug Interactions (7)]
- Known or suspected gastrointestinal obstruction, including paralytic ileus [see Warnings and Precautions (5.13)]
- Hypersensitivity to meperidine (e.g., anaphylaxis) [see Adverse Reactions (6)]
5. Warnings and Precautions
5.1 Addiction, Abuse, and Misuse
Meperidine Hydrochloride Injection contains meperidine, a Schedule II controlled substance. As an opioid, Meperidine Hydrochloride Injection exposes users to the risks of addiction, abuse, and misuse [see Drug Abuse and Dependence (9)].
Although the risk of addiction in any individual is unknown, it can occur in patients appropriately prescribed Meperidine Hydrochloride Injection. Addiction can occur at recommended dosages and if the drug is misused or abused.
Assess each patient's risk for opioid addiction, abuse, or misuse prior to prescribing Meperidine Hydrochloride Injection, and monitor all patients receiving Meperidine Hydrochloride Injection for the development of these behaviors and conditions. Risks are increased in patients with a personal or family history of substance abuse (including drug or alcohol abuse or addiction) or mental illness (e.g., major depression). The potential for these risks should not, however, prevent the proper management of pain in any given patient. Patients at increased risk may be prescribed opioids such as Meperidine Hydrochloride Injection, but use in such patients necessitates intensive counseling about the risks and proper use of Meperidine Hydrochloride Injection along with intensive monitoring for signs of addiction, abuse, and misuse.
Opioids are sought for nonmedical use and are subject to diversion from legitimate prescribed use. Strategies to reduce these risks include prescribing the drug in the smallest appropriate quantity. Contact local state professional licensing board or state-controlled substances authority for information on how to prevent and detect abuse or diversion of this product.
5.2 Life-Threatening Respiratory Depression
Serious, life-threatening, or fatal respiratory depression has been reported with the use of opioids, even when used as recommended. Respiratory depression, if not immediately recognized and treated, may lead to respiratory arrest and death. Management of respiratory depression may include close observation, supportive measures, and use of opioid antagonists, depending on the patient's clinical status [see Overdosage (10)]. Carbon dioxide (CO2) retention from opioid-induced respiratory depression can exacerbate the sedating effects of opioids.
While serious, life-threatening, or fatal respiratory depression can occur at any time during the use of Meperidine Hydrochloride Injection, the risk is greatest during the initiation of therapy or following a dosage increase.
To reduce the risk of respiratory depression, proper dosing and titration of Meperidine Hydrochloride Injection are essential [see Dosage and Administration (2.3)]. Overestimating the Meperidine Hydrochloride Injection dosage when converting patients from another opioid product can result in a fatal overdose with the first dose.
Opioids can cause sleep-related breathing disorders including central sleep apnea (CSA) and sleep-related hypoxemia. Opioid use increases the risk of CSA in a dose-dependent fashion. In patients who present with CSA, consider decreasing the opioid dosage using best practices for opioid taper [See Dosage and Administration (2.1)].
5.3 Risks from Concomitant Use with Benzodiazepines or Other CNS Depressants
Profound sedation, respiratory depression, coma, and death may result from the concomitant use of Meperidine Hydrochloride Injection with benzodiazepines and/or other CNS depressants, including alcohol (e.g., non- benzodiazepine sedatives/hypnotics, anxiolytics, tranquilizers, muscle relaxants, general anesthetics, antipsychotics, other opioids). Because of these risks, reserve concomitant prescribing of these drugs for use in patients for whom alternative treatment options are inadequate.
Observational studies have demonstrated that concomitant use of opioid analgesics and benzodiazepines increases the risk of drug-related mortality compared to use of opioid analgesics alone. Because of similar pharmacological properties, it is reasonable to expect similar risk with the concomitant use of other CNS depressant drugs with opioid analgesics [see Drug Interactions (7)].
If the decision is made to prescribe a benzodiazepine or other CNS depressant concomitantly with an opioid analgesic, prescribe the lowest effective dosages and minimum durations of concomitant use. In patients already receiving an opioid analgesic, prescribe a lower initial dose of the benzodiazepine or other CNS depressant than indicated in the absence of an opioid, and titrate based on clinical response. If an opioid analgesic is initiated in a patient already taking a benzodiazepine or other CNS depressant, prescribe a lower initial dose of the opioid analgesic, and titrate based on clinical response. Monitor patients closely for signs and symptoms of respiratory depression and sedation.
Advise both patients and caregivers about the risks of respiratory depression and sedation when Meperidine Hydrochloride Injection is used with benzodiazepines or other CNS depressants (including alcohol and illicit drugs). Advise patients not to drive or operate heavy machinery until the effects of concomitant use of the benzodiazepine or other CNS depressant have been determined. Screen patients for risk of substance use disorders, including opioid abuse and misuse, and warn them of the risk for overdose and death associated with the use of additional CNS depressants including alcohol and illicit drugs [see Drug Interactions (7)].
5.4 Neonatal Opioid Withdrawal Syndrome
Use of Meperidine Hydrochloride Injection for an extended period of time during pregnancy can result in withdrawal in the neonate. Neonatal opioid withdrawal syndrome, unlike opioid withdrawal syndrome in adults, may be life-threatening if not recognized and treated, and requires management according to protocols developed by neonatology experts. Observe newborns for signs of neonatal opioid withdrawal syndrome and manage accordingly. Advise pregnant women using opioids for an extended period of time of the risk of neonatal opioid withdrawal syndrome and ensure that management by neonatology experts will be available at delivery [see Use in Specific Populations (8.1)].
5.5 Risks of Concomitant Use or Discontinuation of Cytochrome P450 3A4 Inhibitors and Inducers
Concomitant use of Meperidine Hydrochloride Injection with a CYP3A4 inhibitor, such as macrolide antibiotics (e.g., erythromycin), azole-antifungal agents (e.g., ketoconazole), and protease inhibitors (e.g., ritonavir), may increase plasma concentrations of meperidine and prolong opioid adverse reactions, which may cause potentially fatal respiratory depression [see Warnings and Precautions (5.2)], particularly when an inhibitor is added after a stable dose of Meperidine Hydrochloride Injection is achieved. Similarly, discontinuation of a CYP3A4 inducer, such as rifampin, carbamazepine, and phenytoin, in Meperidine Hydrochloride Injection-treated patients may increase meperidine plasma concentrations and prolong opioid adverse reactions. When using Meperidine Hydrochloride Injection with CYP3A4 inhibitors or discontinuing CYP3A4 inducers in Meperidine Hydrochloride Injection-treated patients, monitor patients closely at frequent intervals and consider dosage reduction of Meperidine Hydrochloride Injection until stable drug effects are achieved [see Drug Interactions (7)].
Concomitant use of Meperidine Hydrochloride Injection with CYP3A4 inducers or discontinuation of a CYP3A4 inhibitor could decrease meperidine plasma concentrations, decrease opioid efficacy or, possibly, lead to a withdrawal syndrome in a patient who had developed physical dependence to meperidine. When using Meperidine Hydrochloride Injection with CYP3A4 inducers or discontinuing CYP3A4 inhibitors, monitor patients closely at frequent intervals and consider increasing the opioid dosage if needed to maintain adequate analgesia or if symptoms of opioid withdrawal occur [see Drug Interactions (7)].
5.6 Fatal Interaction with Monoamine Oxidase Inhibitors
Meperidine is contraindicated in patients who are receiving monoamine oxidase (MAO) inhibitors or those who have recently received such agents. Therapeutic doses of meperidine have occasionally precipitated unpredictable, severe, and occasionally fatal reactions in patients who have received such agents within 14 days. The mechanism of these reactions is unclear but may be related to a pre-existing hyperphenylalaninemia. Some have been characterized by coma, severe respiratory depression, cyanosis, and hypotension, and have resembled the syndrome of acute narcotic overdose. Serotonin syndrome with agitation, hyperthermia, diarrhea, tachycardia, sweating, tremors and impaired consciousness may also occur. In other reactions the predominant manifestations have been hyperexcitability, convulsions, tachycardia, hyperpyrexia, and hypertension.
Do not use Meperidine Hydrochloride Injection in patients taking MAOIs or within 14 days of stopping such treatment. Intravenous hydrocortisone or prednisolone have been used to treat severe reactions, with the addition of intravenous chlorpromazine in those cases exhibiting hypertension and hyperpyrexia. The usefulness and safety of narcotic antagonists in the treatment of these reactions is unknown.
5.7 Opioid-Induced Hyperalgesia and Allodynia
Opioid-Induced Hyperalgesia (OIH) occurs when an opioid analgesic paradoxically causes an increase in pain, or an increase in sensitivity to pain. This condition differs from tolerance, which is the need for increasing doses of opioids to maintain a defined effect [see Dependence (9.3)]. Symptoms of OIH include (but may not be limited to) increased levels of pain upon opioid dosage increase, decreased levels of pain upon opioid dosage decrease, or pain from ordinarily non-painful stimuli (allodynia). These symptoms may suggest OIH only if there is no evidence of underlying disease progression, opioid tolerance, opioid withdrawal, or addictive behavior.
Cases of OIH have been reported, both with short-term and longer-term use of opioid analgesics. Though the mechanism of OIH is not fully understood, multiple biochemical pathways have been implicated. Medical literature suggests a strong biologic plausibility between opioid analgesics and OIH and allodynia. If a patient is suspected to be experiencing OIH, carefully consider appropriately decreasing the dose of the current opioid analgesic or opioid rotation (safely switching the patient to a different opioid moiety) [see Dosage and Administration (2), Warnings and Precautions (5.15)].
5.8 Serotonin Syndrome with Concomitant Use of Serotonergic Drugs
Cases of serotonin syndrome, a potentially life-threatening condition, have been reported during concomitant use of meperidine with serotonergic drugs. Serotonergic drugs include selective serotonin reuptake inhibitors (SSRIs), serotonin and norepinephrine reuptake inhibitors (SNRIs), tricyclic antidepressants (TCAs), triptans, 5-HT3 receptor antagonists, drugs that affect the serotonergic neurotransmitter system (e.g., mirtazapine, trazodone, tramadol), certain muscle relaxants (i.e., cyclobenzaprine, metaxalone), and drugs that impair metabolism of serotonin (including MAO inhibitors, both those intended to treat psychiatric disorders and also others, such as linezolid and intravenous methylene blue) [see Drug Interactions (7)]. This may occur within the recommended dosage range.
Serotonin syndrome symptoms may include mental status changes (e.g., agitation, hallucinations, coma), autonomic instability (e.g., tachycardia, labile blood pressure, hyperthermia), neuromuscular aberrations (e.g., hyperreflexia, incoordination, rigidity), and/or gastrointestinal symptoms (e.g., nausea, vomiting, diarrhea) and can be fatal. The onset of symptoms generally occurs within several hours to a few days of concomitant use but may occur later than that. Discontinue Meperidine Hydrochloride Injection if serotonin syndrome is suspected.
5.9 Life-Threatening Respiratory Depression in Patients with Chronic Pulmonary Disease or in Elderly, Cachectic, or Debilitated Patients
The use of Meperidine Hydrochloride Injection in patients with acute or severe bronchial asthma in an unmonitored setting or in the absence of resuscitative equipment is contraindicated.
Patients with Chronic Pulmonary Disease: Meperidine Hydrochloride Injection-treated patients with significant chronic obstructive pulmonary disease or cor pulmonale, and those with a substantially decreased respiratory reserve, hypoxia, hypercapnia, or pre-existing respiratory depression are at increased risk of decreased respiratory drive including apnea, even at recommended dosages of Meperidine Hydrochloride Injection [see Warnings and Precautions (5.2)].
Elderly, Cachectic, or Debilitated Patients: Life-threatening respiratory depression is more likely to occur in elderly, cachectic, or debilitated patients because they may have altered pharmacokinetics or altered clearance compared to younger, healthier patients [see Warnings and Precautions (5.2)].
Monitor such patients closely, particularly when initiating and titrating Meperidine Hydrochloride Injection and when Meperidine Hydrochloride Injection is given concomitantly with other drugs that depress respiration [see Warnings and Precautions (5.2)].
Alternatively, consider the use of non-opioid analgesics in these patients.
5.10 Adrenal Insufficiency
Cases of adrenal insufficiency have been reported with opioid use, more often following greater than one month of use. Presentation of adrenal insufficiency may include non-specific symptoms and signs including nausea, vomiting, anorexia, fatigue, weakness, dizziness, and low blood pressure. If adrenal insufficiency is suspected, confirm the diagnosis with diagnostic testing as soon as possible. If adrenal insufficiency is diagnosed, treat with physiologic replacement doses of corticosteroids. Wean the patient off of the opioid to allow adrenal function to recover and continue corticosteroid treatment until adrenal function recovers. Other opioids may be tried as some cases reported use of a different opioid without recurrence of adrenal insufficiency. The information available does not identify any particular opioids as being more likely to be associated with adrenal insufficiency.
5.11 Severe Hypotension
Meperidine Hydrochloride Injection may cause severe hypotension including orthostatic hypotension and syncope in ambulatory patients. There is increased risk in patients whose ability to maintain blood pressure has already been compromised by a reduced blood volume or concurrent administration of certain CNS depressant drugs (e.g., phenothiazines or general anesthetics) [see Drug Interactions (7)]. Monitor these patients for signs of hypotension after initiating or titrating the dosage of Meperidine Hydrochloride Injection. In patients with circulatory shock, Meperidine Hydrochloride Injection may cause vasodilation that can further reduce cardiac output and blood pressure. Avoid the use of Meperidine Hydrochloride Injection in patients with circulatory shock.
5.12 Risks of Use in Patients with Increased Intracranial Pressure, Brain Tumors, Head Injury, or Impaired Consciousness
In patients who may be susceptible to the intracranial effects of CO2 retention (e.g., those with evidence of increased intracranial pressure or brain tumors), Meperidine Hydrochloride Injection may reduce respiratory drive, and the resultant CO2 retention can further increase intracranial pressure. Monitor such patients for worsening of signs of increasing intracranial pressure. Monitor such patients for signs of sedation and respiratory depression, particularly when initiating therapy with Meperidine Hydrochloride Injection.
Opioids may also obscure the clinical course in a patient with a head injury. Avoid the use of Meperidine Hydrochloride Injection in patients with impaired consciousness or coma.
5.13 Risks of Use in Patients with Gastrointestinal Conditions
Meperidine Hydrochloride Injection is contraindicated in patients with known or suspected gastrointestinal obstruction, including paralytic ileus.
The meperidine in Meperidine Hydrochloride Injection may cause spasm of the sphincter of Oddi. Opioids may cause increases in serum amylase. Monitor patients with biliary tract disease, including acute pancreatitis, for worsening symptoms.
5.14 Increased Risk of Seizures in Patients with Seizure Disorders
The meperidine in Meperidine Hydrochloride Injection may increase the frequency of seizures in patients with seizure disorders and may increase the risk of seizures occurring in other clinical settings associated with seizures. Monitor patients with a history of seizure disorders for worsened seizure control during Meperidine Hydrochloride Injection therapy. Prolonged meperidine use may increase the risk of toxicity (e.g., seizures) from the accumulation of the meperidine metabolite, normeperidine.
5.15 Withdrawal
Avoid the use of mixed agonist/antagonist (e.g., pentazocine, nalbuphine, and butorphanol) or partial agonist (e.g., buprenorphine) analgesics in patients who are receiving a full opioid agonist analgesic, including Meperidine Hydrochloride Injection. In these patients, mixed agonist/antagonist and partial agonist analgesics may reduce the analgesic effect and/or precipitate withdrawal symptoms.
When discontinuing Meperidine Hydrochloride Injection, gradually taper the dosage [see Dosage and Administration (2.4)]. Do not abruptly discontinue Meperidine Hydrochloride Injection [see Drug Abuse and Dependence (9.3)].
5.16 Risks of Driving and Operating Machinery
Meperidine Hydrochloride Injection may impair the mental or physical abilities needed to perform potentially hazardous activities such as driving a car or operating machinery. Warn patients not to drive or operate dangerous machinery unless they are tolerant to the effects of Meperidine Hydrochloride Injection and know how they will react to the medication.
5.17 Risks in Patients with Pheochromocytoma
In patients with pheochromocytoma, meperidine has been reported to provoke hypertension.
5.18 Risk of Use in Patients with Atrial Flutter and Other Supraventricular Tachycardias
Meperidine Hydrochloride Injection should be used with caution in patients with atrial flutter and other supraventricular tachycardias because of a possible vagolytic action which may produce a significant increase in the ventricular response rate.
5.19 Intravenous Use
If necessary, meperidine may be given intravenously, but the injection should be given very slowly, preferably in the form of a diluted solution. Rapid intravenous injection of narcotic analgesics, including meperidine, increases the incidence of adverse reactions; severe respiratory depression, apnea, hypotension, peripheral circulatory collapse, and cardiac arrest have occurred. Meperidine should not be administered intravenously unless a narcotic antagonist and the facilities for assisted or controlled respiration are immediately available. When meperidine is given parenterally, especially intravenously, the patient should be lying down.
6. Adverse Reactions/Side Effects
The following serious adverse reactions are described, or described in greater detail, in other sections:
- Addiction, Abuse, and Misuse [see Warnings and Precautions (5.1)]
- Life-Threatening Respiratory Depression [see Warnings and Precautions (5.2)]
- Interactions with Benzodiazepines or Other CNS Depressants [see Warnings and Precautions (5.3)]
- Neonatal Opioid Withdrawal Syndrome [see Warnings and Precautions (5.4)]
- Opioid-Induced Hyperalgesia and Allodynia [see Warnings and Precautions (5.7)]
- Serotonin Syndrome with Concomitant Use of Serotonergic Drugs [see Warnings and Precautions (5.8)]
- Adrenal Insufficiency [see Warnings and Precautions (5.10)]
- Severe Hypotension [see Warnings and Precautions (5.11)]
- Gastrointestinal Adverse Reactions [see Warnings and Precautions (5.13)]
- Seizures [see Warnings and Precautions (5.14)]
- Withdrawal [see Warnings and Precautions (5.15)]
The following adverse reactions associated with the use of meperidine were identified in clinical studies or postmarketing reports. Because some of these reactions were reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
The major hazards of meperidine, as with other opioid analgesics, are respiratory depression and, to a lesser degree, circulatory depression; respiratory arrest, shock, and cardiac arrest have occurred.
The most frequently observed adverse reactions include lightheadedness, dizziness, sedation, nausea, vomiting, and sweating. These effects seem to be more prominent in ambulatory patients and in those who are not experiencing severe pain. In such individuals, lower doses are advisable. Some adverse reactions in ambulatory patients may be alleviated if the patient lies down.
Other adverse reactions include:
Nervous System: Mood changes (e.g. euphoria, dysphoria), weakness, headache, agitation, tremor, involuntary muscle movements (e.g. muscle twitches, myoclonus), severe convulsions, transient hallucinations and disorientation, confusion, delirium, visual disturbances. Inadvertent injection about a nerve trunk may result in sensory-motor paralysis which is usually, though not always, transitory.
Gastrointestinal: Dry mouth, constipation, biliary tract spasm.
Cardiovascular: Flushing of the face, tachycardia, bradycardia, palpitation, hypotension [see Warnings and Precautions (5.18)], syncope, phlebitis following intravenous injection.
Genitourinary: Urinary retention.
Allergic:. Pruritus, urticaria, other skin rashes, wheal and flare over the vein with intravenous injection.
Hypersensitivity reactions, anaphylaxis.
Histamine release leading to hypotension and/or tachycardia, flushing, sweating, and pruritus.
Other: Pain at injection site; local tissue irritation and induration following subcutaneous injection, particularly when repeated; antidiuretic effect.
Serotonin syndrome: Cases of serotonin syndrome, a potentially life-threatening condition, have been reported during concomitant use of opioids with serotonergic drugs.
Adrenal insufficiency: Cases of adrenal insufficiency have been reported with opioid use, more often following greater than one month of use.
Androgen deficiency: Cases of androgen deficiency have occurred with chronic use of opioids for an extended period of time [see Clinical Pharmacology (12.2)].
Hyperalgesia and Allodynia: Cases of hyperalgesia and allodynia have been reported with opioid therapy of any duration [see Warnings and Precautions (5.7)].
Hypoglycemia: Cases of hypoglycemia have been reported in patients taking opioids. Most reports were in patients with at least one predisposing risk factor (e.g., diabetes).
Related/similar drugs
7. Drug Interactions
Table 1 includes clinically significant drug interactions with Meperidine Hydrochloride Injection.
| Monoamine Oxidase Inhibitors (MAOIs) | |
| Clinical Impact: | Meperidine is contraindicated in patients who are receiving monoamine oxidase (MAO) inhibitors or those who have recently received such agents. Therapeutic doses of meperidine have occasionally precipitated unpredictable, severe, and occasionally fatal reactions in patients who have received such agents within 14 days. The mechanism of these reactions is unclear, but may be related to a pre-existing hyperphenylalaninemia. Some have been characterized by coma, severe respiratory depression, cyanosis, and hypotension, and have resembled the syndrome of acute narcotic overdose. Serotonin syndrome with agitation, hyperthermia, diarrhea, tachycardia, sweating, tremors and impaired consciousness may also occur. In other reactions the predominant manifestations have been hyperexcitability, convulsions, tachycardia, hyperpyrexia, and hypertension. [see Warnings and Precautions (5.6)]. |
| Intervention: | Do not use Meperidine Hydrochloride Injection in patients taking MAOIs or within 14 days of stopping such treatment.
Intravenous hydrocortisone or prednisolone have been used to treat severe reactions, with the addition of intravenous chlorpromazine in those cases exhibiting hypertension and hyperpyrexia. The usefulness and safety of narcotic antagonists in the treatment of these reactions is unknown. |
| Examples: | Phenelzine, tranylcypromine, linezolid |
| Inhibitors of CYP3A4 and CYP2B6 | |
| Clinical Impact: | The concomitant use of Meperidine Hydrochloride Injection and CYP3A4 or CYP2B6 inhibitors can increase the plasma concentration of meperidine, resulting in increased or prolonged opioid effects. These effects could be more pronounced with concomitant use of Meperidine Hydrochloride Injection and CYP2B6 and CYP3A4 inhibitors, particularly when an inhibitor is added after a stable dose of Meperidine Hydrochloride Injection is achieved [see Warnings and Precautions (5.5)].
After stopping a CYP3A4 inhibitor, as the effects of the inhibitor decline, the meperidine plasma concentration will decrease [see Clinical Pharmacology (12.3)], resulting in decreased opioid efficacy or a withdrawal syndrome in patients who had developed physical dependence to meperidine. |
| Intervention: | If concomitant use is necessary, consider dosage reduction of Meperidine Hydrochloride Injection until stable drug effects are achieved. Monitor patients for respiratory depression and sedation at frequent intervals.
If a CYP3A4 or CYP2B6 inhibitor is discontinued, consider increasing the Meperidine Hydrochloride Injection dosage until stable drug effects are achieved. Monitor for signs of opioid withdrawal. |
| Examples: | Macrolide antibiotics (e.g., erythromycin), azole-antifungal agents (e.g. ketoconizole), protease inhibitors (e.g., ritonavir) |
| CYP3A4 and CYP2B6 Inducers | |
| Clinical Impact: | The concomitant use of Meperidine Hydrochloride Injection and CYP3A4 inducers, or CYP2B6 inducers can decrease the plasma concentration of meperidine [see Clinical Pharmacology (12.3)], resulting in decreased efficacy or onset of a withdrawal syndrome in patients who have developed physical dependence to meperidine [see Warnings and Precautions (5.5)].
After stopping a CYP3A4 or CYP2B6 inducer, as the effects of the inducer decline, the meperidine plasma concentration will increase [see Clinical Pharmacology (12.3)], which could increase or prolong both the therapeutic effects and adverse reactions, and may cause serious respiratory depression. |
| Intervention: | If concomitant use is necessary, consider increasing the Meperidine Hydrochloride Injection dosage until stable drug effects are achieved. Monitor for signs of opioid withdrawal. If a CYP3A4 or CYP2B6 inducer is discontinued, consider Meperidine Hydrochloride Injection dosage reduction and monitor for signs of respiratory depression. |
| Examples: | Rifampin, carbamazepine, phenytoin |
| Benzodiazepines and Other Central Nervous System (CNS) Depressants | |
| Clinical Impact: | Due to additive pharmacologic effect, the concomitant use of benzodiazepines or other CNS depressants, including alcohol, can increase the risk of hypotension respiratory depression, profound sedation, coma, and death [see Warnings and Precautions (5.3)]. |
| Intervention: | Reserve concomitant prescribing of these drugs for use in patients for whom alternative treatment options are inadequate. Limit dosages and durations to the minimum required. Follow patients closely for signs of respiratory depression and sedation. |
| Examples: | Benzodiazepines and other sedatives/hypnotics, anxiolytics, tranquilizers, muscle relaxants, general anesthetics, antipsychotics, other opioids, alcohol. |
| Serotonergic Drugs | |
| Clinical Impact: | The concomitant use of opioids with other drugs that affect the serotonergic neurotransmitter system has resulted in serotonin syndrome [see Warnings and Precautions (5.8)]. |
| Intervention: | If concomitant use is warranted, carefully observe the patient, particularly during treatment initiation and dose adjustment. Discontinue Meperidine Hydrochloride Injection if serotonin syndrome is suspected. |
| Examples: | Selective serotonin reuptake inhibitors (SSRIs), serotonin and norepinephrine reuptake inhibitors (SNRIs), tricyclic antidepressants (TCAs), triptans, 5-HT3 receptor antagonists, drugs that affect the serotonin neurotransmitter system (e.g., mirtazapine, trazodone, tramadol), certain muscle relaxants (i.e., cyclobenzaprine, metaxalone), monoamine oxidase (MAO) inhibitors (those intended to treat psychiatric disorders and also others, such as linezolid and intravenous methylene blue). |
| Mixed Agonist/Antagonist and Partial Agonist Opioid Analgesics | |
| Clinical Impact: | May reduce the analgesic effect of Meperidine Hydrochloride Injection and/or precipitate withdrawal symptoms. |
| Intervention: | Avoid concomitant use. |
| Examples: | Butorphanol, nalbuphine, pentazocine, buprenorphine. |
| Muscle Relaxants | |
| Clinical Impact: | Meperidine may enhance the neuromuscular blocking action of skeletal muscle relaxants and produce an increased degree of respiratory depression. |
| Intervention: | Monitor patients for signs of respiratory depression that may be greater than otherwise expected and decrease the dosage of Meperidine Hydrochloride Injection and/or the muscle relaxant as necessary. |
| Diuretics | |
| Clinical Impact: | Opioids can reduce the efficacy of diuretics by inducing the release of antidiuretic hormone. |
| Intervention: | Monitor patients for signs of diminished diuresis and/or effects on blood pressure and increase the dosage of the diuretic as needed. |
| Anticholinergic Drugs | |
| Clinical Impact: | The concomitant use of anticholinergic drugs may increase risk of urinary retention and/or severe constipation, which may lead to paralytic ileus. |
| Intervention: | Monitor patients for signs of urinary retention or reduced gastric motility when Meperidine Hydrochloride Injection is used concomitantly with anticholinergic drugs. |
| Acyclovir | |
| Clinical Impact: | The concomitant use of acyclovir may increase the plasma concentrations of meperidine and its metabolite, normeperidine. |
| Intervention: | If concomitant use of acyclovir and Meperidine Hydrochloride Injection is necessary, monitor patients for respiratory depression and sedation at frequent intervals. |
| Cimetidine | |
| Clinical Impact: | The concomitant use of cimetidine may reduce the clearance and volume of distribution of meperidine also the formation of the metabolite, normeperidine, in healthy subjects. |
| Intervention: | If concomitant use of cimetidine and Meperidine Hydrochloride Injection is necessary, monitor patients for respiratory depression and sedation at frequent intervals. |
8. Use In Specific Populations
8.1 Pregnancy
Risk Summary
Prolonged use of opioid analgesics for an extended period of time during pregnancy may cause neonatal opioid withdrawal syndrome [see Warnings and Precautions (5.4)]. Available data with Meperidine Hydrochloride Injection are insufficient to inform a drug-associated risk for major birth defects and miscarriage or adverse maternal outcomes. There are adverse outcomes reported with fetal exposure to opioid analgesics (see Clinical Considerations). Formal animal reproduction studies have not been conducted with meperidine. Neural tube defects (exencephaly and cranioschisis) have been reported in hamsters administered a single bolus dose of meperidine during a critical period of organogenesis at 0.85 and 1.5 times the total human daily dose of 1200 mg. [see Data]
The background risk of major birth defects and miscarriage for the indicated population is unknown. All pregnancies have a background risk of birth defect, loss or other outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2–4% and 15–20%, respectively.
Clinical Considerations
Fetal/Neonatal Adverse Reactions
Use of opioid analgesics for an extended period of time during pregnancy for medical or nonmedical purposes can result in physical dependence in the neonate and neonatal opioid withdrawal syndrome shortly after birth.
Neonatal opioid withdrawal syndrome presents as irritability, hyperactivity and abnormal sleep pattern, high pitched cry, tremor, vomiting, diarrhea, and failure to gain weight. The onset, duration, and severity of neonatal opioid withdrawal syndrome vary based on the specific opioid used, duration of use, timing and amount of last maternal use, and rate of elimination of the drug by the newborn. Observe newborns for symptoms of neonatal opioid withdrawal syndrome and manage accordingly [see Warnings and Precautions (5.4)].
Labor or Delivery
Opioids cross the placenta and may produce respiratory depression and psycho-physiologic effects in neonates. An opioid antagonist, such as naloxone, must be available for reversal of opioid-induced respiratory depression in the neonate. Meperidine Hydrochloride Injection is not recommended for use in pregnant women during or immediately prior to labor, when other analgesic techniques are more appropriate. Opioid analgesics, including Meperidine Hydrochloride Injection, can prolong labor through actions which temporarily reduce the strength, duration, and frequency of uterine contractions. However, this effect is not consistent and may be offset by an increased rate of cervical dilation, which tends to shorten labor. Monitor neonates exposed to opioid analgesics during labor for signs of excess sedation and respiratory depression.
Data
Animal Data
Formal reproductive and developmental toxicology studies for meperidine have not been completed.
In a published study, neural tube defects (exencephaly and cranioschisis) were noted following subcutaneous administration of meperidine hydrochloride (127 and 218 mg/kg, respectively) on Gestation Day 8 to pregnant hamsters (0.85 and 1.5 times the total daily dose of 1200 mg/day based on body surface area). The findings cannot be clearly attributed to maternal toxicity.
8.2 Lactation
Risk Summary
Meperidine appears in the milk of nursing mothers receiving the drug. The developmental and health benefits of breastfeeding should be considered along with the mother's clinical need for Meperidine Hydrochloride Injection and any potential adverse effects on the breastfed infant from Meperidine Hydrochloride Injection or from the underlying maternal condition.
Clinical Considerations
Monitor infants exposed to Meperidine Hydrochloride Injection through breast milk for excess sedation and respiratory depression. Withdrawal symptoms can occur in breastfed infants when maternal administration of an opioid analgesic is stopped, or when breast-feeding is stopped.
8.3 Females and Males of Reproductive Potential
Infertility
Use of opioids for an extended period of time may cause reduced fertility in females and males of reproductive potential. It is not known whether these effects on fertility are reversible [see Adverse Reactions (6) Clinical Pharmacology (12.2)], Nonclinical Pharmacology (13.1)].
8.4 Pediatric Use
The safety and efficacy of Meperidine Hydrochloride Injection in patients less than 18 years of age have not been established.
The safety and effectiveness of meperidine in pediatric patients has not been established. Literature reports indicate that meperidine has a slower elimination rate in neonates and young infants compared to older children and adults. Neonates and young infants may also be more susceptible to the effects, especially the respiratory depressant effects. If meperidine use is contemplated in neonates or young infants, any potential benefits of the drug need to be weighed against the relative risk of the patient.
8.5 Geriatric Use
Elderly patients (aged 65 years or older) may have increased sensitivity to meperidine. In general, use caution when selecting a dosage for an elderly patient, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function and of concomitant disease or other drug therapy.
Respiratory depression is the chief risk for elderly patients treated with opioids, and has occurred after large initial doses were administered to patients who were not opioid-tolerant or when opioids were co-administered with other agents that depress respiration. Titrate the dosage of Meperidine Hydrochloride Injection slowly in geriatric patients and monitor closely for signs of central nervous system and respiratory depression [see Warnings and Precautions (5.2)].
Meperidine is known to be substantially excreted by the kidney, and the risk of adverse reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to monitor renal function.
8.6 Hepatic Impairment
Accumulation of meperidine and/or its active metabolite, normeperidine, can also occur in patients with hepatic impairment. Elevated serum levels have been reported to cause central nervous system excitatory effects. Meperidine should therefore be used with caution in patients with hepatic impairment. Titrate the dosage of Meperidine Hydrochloride Injection slowly in patients with hepatic impairment and monitor closely for signs of central nervous system and respiratory depression.
8.7 Renal Impairment
Accumulation of meperidine and/or its active metabolite, normeperidine, can occur in patients with renal impairment. Meperidine should therefore be used with caution in patients with renal impairment. Titrate the dosage of Meperidine Hydrochloride Injection slowly in patients with renal impairment and monitor closely for signs of central nervous system and respiratory depression.
9. Drug Abuse and Dependence
9.1 Controlled Substance
Meperidine Hydrochloride Injection contains meperidine, a Schedule II controlled substance.
9.2 Abuse
Meperidine Hydrochloride Injection contains meperidine, a substance with a high potential for misuse and abuse, which can lead to the development of substance use disorder, including addiction [see Warnings and Precautions (5.1)].
Misuse is the intentional use, for therapeutic purposes, of a drug by an individual in a way other than prescribed by a healthcare provider or for whom it was not prescribed.
Abuse is the intentional, non-therapeutic use of a drug, even once, for its desirable psychological or physiological effects.
Drug addiction is a cluster of behavioral, cognitive, and physiological phenomena that may include a strong desire to take the drug, difficulties in controlling its use(e.g., continuing drug use despite harmful consequences, giving a higher priority to drug use than other activities and obligations), and possible tolerance or physical dependence.
Misuse and abuse of Meperidine Hydrochloride Injection increases risk of overdose, which may lead to central nervous system and respiratory depression, hypotension, seizures, and death. The risk is increased with concurrent abuse of Meperidine Hydrochloride Injection with alcohol and/or other CNS depressants. Abuse of and addiction to opioids in some individuals may not be accompanied by concurrent tolerance and symptoms of physical dependence. In addition, abuse of opioids can occur in the absence of addiction.
All patients treated with opioids require careful and frequent reevaluation for signs of misuse, abuse and addiction, because use of opioid analgesic products carries the risk of addiction even under appropriate medical use. Patients at high risk of Meperidine Hydrochloride Injection abuse include those with a history of prolonged use of any opioid, including products containing meperidine, those with a history of drug or alcohol abuse, or those who use Meperidine Hydrochloride Injection in combination with other abused drugs.
"Drug-seeking" behavior is very common in persons with substance use disorders. Drug-seeking tactics include emergency calls or visits near the end of office hours, refusal to undergo appropriate examination, testing, or referral, repeated "loss" of prescriptions, tampering with prescriptions, and reluctance to provide prior medical records or contact information for other treating health care provider(s). "Doctor shopping" (visiting multiple prescribers to obtain additional prescriptions) is common among people who abuse drugs and people with substance use disorder. Preoccupation with achieving adequate pain relief can be appropriate behavior in a patient with inadequate pain control.
Meperidine Hydrochloride Injection, like other opioids, can be diverted for nonmedical use into illicit channels of distribution. Careful record-keeping of prescribing information, including quantity, frequency, and renewal requests, as required by state and federal law, is strongly advised.
Proper assessment of the patient, proper prescribing practices, periodic re-evaluation of therapy, and proper dispensing and storage are appropriate measures that help to limit abuse of opioid drugs.
Risks Specific to Abuse of Meperidine Hydrochloride Injection
Abuse of Meperidine Hydrochloride Injection poses a risk of overdose and death. The risk is increased with concurrent abuse of Meperidine Hydrochloride Injection with alcohol and other CNS depressants.
Parenteral drug abuse is commonly associated with transmission of infectious diseases such as hepatitis and HIV.
9.3 Dependence
Both tolerance and physical dependence can develop during chronic opioid therapy.
Tolerance is a physiological state characterized by a reduced response to a drug after repeated administration (i.e., a higher dose of a drug is required to produce the same effect that was once obtained at a lower dose).
Physical dependence is a state that develops as a result of a physiological adaptation in response to repeated drug use, manifested by withdrawal signs and symptoms after abrupt discontinuation or a significant dose reduction of a drug.
Withdrawal may be precipitated through the administration of drugs with opioid antagonist activity (e.g., naloxone), mixed agonist/antagonist analgesics (e.g., pentazocine, butorphanol, nalbuphine), or partial agonists (e.g., buprenorphine). Physical dependence may not occur to a clinically significant degree until after several days to weeks of continued use. Meperidine Hydrochloride Injection should not be abruptly discontinued [see Dosage and Administration (2.4)]. If Meperidine Hydrochloride Injection is abruptly discontinued in a physically-dependent patient, a withdrawal syndrome may occur, typically characterized by restlessness, lacrimation, rhinorrhea, perspiration, chills, myalgia, and mydriasis. Other signs and symptoms also may develop, including: irritability, anxiety, backache, joint pain, weakness, abdominal cramps, insomnia, nausea, anorexia, vomiting, diarrhea, or increased blood pressure, respiratory rate, or heart rate.
Infants born to mothers physically dependent on opioids will also be physically-dependent and may exhibit respiratory difficulties and withdrawal signs [see Use in Specific Populations (8.1)].
10. Overdosage
Clinical Presentation
Acute overdose with Meperidine Hydrochloride Injection can be manifested by respiratory depression, somnolence progressing to stupor or coma, skeletal muscle flaccidity, cold and clammy skin, constricted pupils, and, in some cases, pulmonary edema, bradycardia, hypotension, hypoglycemia, partial or complete airway obstruction, atypical snoring, and death. Marked mydriasis rather than miosis may be seen with hypoxia in overdose situations [see Clinical Pharmacology (12.2)]. In severe overdose, particularly by the intravenous route, apnea, circulatory collapse, cardiac arrest, and death may occur.
Accumulation of normeperidine as in chronic use or possibly following introduction of a concomitant CYP3A4 inducer presents as excitatory syndrome including hallucinations, tremors, muscle twitches, dilated pupils, hyperactive reflexes, and convulsions.
Treatment of Overdose
In case of overdose, priorities are the reestablishment of a patent and protected airway and institution of assisted or controlled ventilation, if needed. Employ other supportive measures (including oxygen and vasopressors) in the management of circulatory shock and pulmonary edema as indicated. Cardiac arrest or arrhythmias will require advanced life-support techniques.
The opioid antagonists, such as naloxone, are specific antidotes to respiratory depression resulting from opioid overdose. For clinically significant respiratory or circulatory depression secondary to meperidine overdose, administer an opioid antagonist.
Because the duration of opioid reversal is expected to be less than the duration of action of meperidine in Meperidine Hydrochloride Injection, carefully monitor the patient until spontaneous respiration is reliably re-established. If the response to an opioid antagonist is suboptimal or only brief in nature, administer additional antagonist as directed by the product's prescribing information.
In an individual physically dependent on opioids, administration of the recommended usual dosage of the antagonist will precipitate an acute withdrawal syndrome. The severity of the withdrawal symptoms experienced will depend on the degree of physical dependence and the dose of the antagonist administered. If a decision is made to treat serious respiratory depression in the physically dependent patient, administration of the antagonist should be begun with care and by titration with smaller than usual doses of the antagonist.
11. Meperidine Injection Description
Meperidine Hydrochloride Injection, USP is an opioid agonist, available as a sterile aqueous solution, for intramuscular, subcutaneous or slow intravenous administration.
Each mL contains meperidine hydrochloride, either 25 mg, 50 mg or 100 mg in Water for Injection. Buffered with acetic acid-sodium acetate. pH 3.5-6.0.
The meperidine hydrochloride chemical name is 4-Piperidinecarboxylic acid, 1- methyl-4-phenyl-,ethyl ester, hydrochloride. The molecular weight is 283.79. Its molecular formula is C15H21NO2·HCl, and it has the following chemical structure.
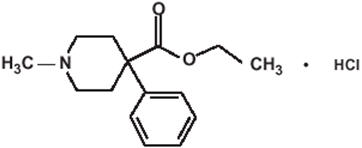
Meperidine hydrochloride is a white crystalline substance with a melting point of 186° C to 189° C. It is readily soluble in water and has a neutral reaction and a slightly bitter taste. The solution is not decomposed by a short period of boiling.
12. Meperidine Injection - Clinical Pharmacology
12.1 Mechanism of Action
Meperidine hydrochloride is an opioid agonist with multiple actions qualitatively similar to those of morphine; the most prominent of these involve the central nervous system and organs composed of smooth muscle. The principal actions of therapeutic value are analgesia and sedation.
12.2 Pharmacodynamics
Effects on the Central Nervous System
Meperidine produces respiratory depression by direct action on brain stem respiratory centers. The respiratory depression involves a reduction in the responsiveness of the brain stem respiratory centers to both increases in carbon dioxide tension and electrical stimulation.
Meperidine causes miosis, even in total darkness. Pinpoint pupils are a sign of opioid overdose but are not pathognomonic (e.g., pontine lesions of hemorrhagic or ischemic origins may produce similar findings). Marked mydriasis rather than miosis may be seen due to hypoxia in overdose situations.
Effects on the Gastrointestinal Tract and Other Smooth Muscle
Meperidine causes a reduction in motility associated with an increase in smooth muscle tone in the antrum of the stomach duodenum. Digestion of food in the small intestine is delayed and propulsive contractions are decreased. Propulsive peristaltic waves in the colon are decreased, while tone may be increased to the point of spasm, resulting in constipation. Other opioid-induced effects may include a reduction in biliary and pancreatic secretions, spasm of sphincter of Oddi, and transient elevations in serum amylase.
Effects of the Cardiovascular System
Meperidine produces peripheral vasodilation which may result in orthostatic hypotension or syncope. Manifestations of histamine release and/or peripheral vasodilation may include pruritus, flushing, red eyes, and sweating and/or orthostatic hypotension.
Effects on the Endocrine System
Opioids inhibit the secretion of adrenocorticotropic hormone (ACTH), cortisol, and luteinizing hormones (LH) in humans [see Adverse Reactions (6)]. They also stimulate prolactin, growth hormone (GH) secretion, and pancreatic secretion of insulin and glucagon.
Use of opioids for an extended period of time may influence the hypothalamic-pituitary-gonadal axis, leading to androgen deficiency that may manifest as low libido, impotence, erectile dysfunction, amenorrhea, or infertility. The causal role of opioids in the clinical syndrome of hypogonadism is unknown because the various medical, physical, lifestyle, and psychological stressors that may influence gonadal hormone levels have not been adequately controlled for in studies conducted to date [see Adverse Reactions (6)].
Effects on the Immune System
Opioids have been shown to have a variety of effects on components of the immune system in in vitro and animal models. The clinical significance of these findings is unknown. Overall, the effects of opioids appear to be modestly immunosuppressive.
Concentration–Efficacy Relationships
The minimum effective analgesic concentration will vary widely among patients, especially among patients who have been previously treated with potent agonist opioids. The minimum effective analgesic concentration of meperidine for any individual patient may increase over time due to an increase in pain, the development of a new pain syndrome and/or the development of analgesic tolerance [see Dosage and Administration (2.1, 2.2)].
Meperidine, in 60 mg to 80 mg parenteral doses, is approximately equivalent in analgesic effect to 10 mg of morphine. The onset of action is slightly more rapid than with morphine, and the duration of action is slightly shorter. Meperidine is significantly less effective by the oral than by the parenteral route, but the exact ratio of oral to parenteral effectiveness is unknown.
Concentration–Adverse Reaction Relationships
There is a relationship between increasing meperidine plasma concentration and increasing frequency of dose-related opioid adverse reactions such as nausea, vomiting, CNS effects, and respiratory depression. In opioid-tolerant patients, the situation may be altered by the development of tolerance to opioid-related adverse reactions [see Dosage and Administration (2.1, 2.2)].
12.3 Pharmacokinetics
Elimination
The half-life of meperidine is 2 to 5 hours, and the half-life of normeperidine is 15 to 30 hours.
Metabolism
Meperidine is metabolized through biotransformation. In vitro data show meperidine is metabolized to normeperidine in liver mainly by CYP3A4 and CYP2B6.
Hepatic Impairment
The elimination half-life is 3 to 8 hours in healthy volunteers and is 1.3 to 2 times greater in post-operative or cirrhotic patients.
Age
In clinical studies reported in the literature, changes in several pharmacokinetic parameters with increasing age have been observed. The initial volume of distribution and steady-state volume of distribution may be higher in elderly patients than in younger patients. The free fraction of meperidine in plasma may be higher in patients over 45 years of age than in younger patients.
Drug Interactions Studies
Phenytoin: The hepatic metabolism of meperidine may be enhanced by phenytoin. Concomitant administration resulted in reduced half-life and bioavailability with increased clearance of meperidine in healthy subjects; however, blood concentrations of normeperidine were increased [see Drug Interactions, (7)].
Ritonavir: Plasma concentrations of the active metabolite normeperidine may be increased by ritonavir [see Drug Interactions, (7)].
Acyclovir: Plasma concentrations of meperidine and its metabolite, normeperidine, may be increased by acyclovir [see Drug Interactions, (7)].
Cimetidine: Cimetidine reduced the clearance and volume of distribution of meperidine and also the formation of the metabolite, normeperidine, in healthy subjects [see Drug Interactions, (7)].
13. Nonclinical Toxicology
16. How is Meperidine Injection supplied
For Parenteral Use
Meperidine Hydrochloride Injection, USP is clear and colorless and is available in the following packages:
25 mg/mL
1 mL Single Dose vials packaged in 25s (NDC 0641-6052-25)
50 mg/mL
1 mL Single Dose vials packaged in 25s (NDC 0641-6053-25)
100 mg/mL
1 mL Single Dose vials packaged in 25s (NDC 0641-6054-25)
Store at 20° to 25°C (68° to 77°F), excursions permitted to 15° to 30°C (59° to 86°F) [See USP Controlled Room Temperature].
17. Patient Counseling Information
Addiction, Abuse, and Misuse
Inform patients that the use of Meperidine Hydrochloride Injection, even when taken as recommended, can result in addiction, abuse, and misuse, which can lead to overdose and death [see Warnings and Precautions (5.1)]. Instruct patients not to share Meperidine Hydrochloride Injection with others and to take steps to protect Meperidine Hydrochloride Injection from theft or misuse.
Life-Threatening Respiratory Depression
Inform patients of the risk of life-threatening respiratory depression, including information that the risk is greatest when Meperidine Hydrochloride Injection or when the dosage is increased, and that it can occur even at recommended dosages [see Warnings and Precautions (5.2)].
Hyperalgesia and Allodynia
Advise patients to inform their healthcare provider if they experience symptoms of hyperalgesia, including worsening pain, increased sensitivity to pain, or new pain [see Warnings and Precautions (5.7), Adverse Reactions (6)].
Serotonin Syndrome
Inform patients that opioids could cause a rare but potentially life-threatening condition resulting from concomitant administration of serotonergic drugs. Warn patients of the symptoms of serotonin syndrome and to seek medical attention right away if symptoms develop. Instruct patients to inform their health care provider if they are taking, or plan to take serotonergic medications [see Warnings and Precautions (5.7), Drug Interactions (7)].
Constipation
Advise patients of the potential for severe constipation, including management instructions and when to seek medical attention [see Adverse Reactions (6), Clinical Pharmacology (12.1)].
PRINCIPAL DISPLAY PANEL
NDC 0641-6052-01 Rx only
Meperidine
HCl Injection, USP
25 mg/mL CII
For IM, SC or
slow IV use
Do not use
if precipitated
1 mL Vial

NDC 0641-6052-25 Rx only
Meperidine
HCl Injection, USP
25 mg/mL CII
For Intramuscular, Subcutaneous
or slow Intravenous use
25 x 1 mL Single Dose Vials

| MEPERIDINE HYDROCHLORIDE
meperidine hydrochloride injection |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| MEPERIDINE HYDROCHLORIDE
meperidine hydrochloride injection |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| MEPERIDINE HYDROCHLORIDE
meperidine hydrochloride injection |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| Labeler - Hikma Pharmaceuticals USA Inc. (946499746) |
| Establishment | |||
| Name | Address | ID/FEI | Business Operations |
|---|---|---|---|
| Hikma Pharmaceuticals USA Inc. | 946499746 | analysis(0641-6053, 0641-6054, 0641-6052) , label(0641-6053, 0641-6054, 0641-6052) , manufacture(0641-6053, 0641-6054, 0641-6052) , pack(0641-6053, 0641-6054, 0641-6052) | |
Frequently asked questions
More about meperidine
- Check interactions
- Compare alternatives
- Pricing & coupons
- Reviews (101)
- Drug images
- Side effects
- Dosage information
- During pregnancy
- Drug class: Opioids (narcotic analgesics)
- Breastfeeding
- En español