Menorrhagia
Medically reviewed by Drugs.com. Last updated on Sep 23, 2025.
What is menorrhagia?
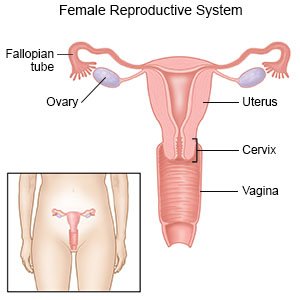
Menorrhagia is heavy menstrual bleeding for more than 7 days or severe menstrual bleeding for less than 7 days. Your menstrual bleeding and cramping are so heavy that you have trouble doing your usual daily activities. Your monthly period may also occur more often, and you may bleed between periods. Menorrhagia is common in adolescence and around menopause.
 |
What causes menorrhagia?
- A hormone imbalance
- Ovaries do not work correctly and cannot produce eggs
- Uterine fibroids or growths (polyps) on the lining of your uterus
- Adenomyosis (thickening of your uterus)
- A pelvic infection or intrauterine device (IUD)
- Complications of pregnancy, such as miscarriage or an ectopic pregnancy
- Conditions such as blood coagulation disorders or uterine cancer
What increases my risk for menorrhagia?
- Obesity
- Not having children
- Use of blood thinner medicine
- Abnormal structure of your reproductive organs
- Family history of endometrial or colon cancer
What are the signs and symptoms of menorrhagia?
- Soaking a pad or tampon every 1 to 2 hours
- Using both a pad and a tampon
- Waking up at night to change your pad or tampon
- Blood clots with your bleeding for more than 1 day
- Abdominal pain or cramps
How is menorrhagia diagnosed?
Your healthcare provider will ask about your symptoms and examine you. Tell him or her how often you change your pad or tampon. He or she may examine you for other signs of bleeding, such as bruises or bleeding gums. He or she may ask if anything relieves your pain, such as heat or medicine. Tell your healthcare provider if you are sexually active or have ever been pregnant. You may need any of the following:
- A blood test will check for pregnancy and the cause of your blood loss. A blood test will also show anemia caused by menorrhagia.
- A pelvic exam and Pap smear may be needed to check the size and shape of your uterus and ovaries. Your healthcare provider gently inserts a warmed speculum into your vagina. A speculum is a tool that opens your vagina to show your cervix.
- A biopsy is a procedure to remove a small piece of tissue from the endometrium. The tissue is sent to a lab for tests.
- An ultrasound may show the cause of your bleeding. Sound waves are used to show pictures on a monitor.
- A hysteroscopy is a procedure to look at your endometrium. The endometrium is the lining inside of your uterus. Your healthcare provider will insert a small tube with a camera at the end into your uterus.
Related medications
How is menorrhagia treated?
- Medicines:
- Iron supplements may be given if your blood iron level decreases because of heavy bleeding.
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. NSAIDs can cause stomach bleeding or kidney problems in certain people. If you take blood thinner medicine, always ask your healthcare provider if NSAIDs are safe for you. Always read the medicine label and follow directions.
- Hormones help slow or stop your bleeding and make your monthly periods more regular. This medicine may be given as birth control pills or an intrauterine device (IUD).
- Surgery and procedures may be needed if medicines do not work or cannot be used. You may need procedures to control bleeding, such as endometrial ablation or a D&C (dilation and curettage). You may need uterine embolization or a hysterectomy. Ask your healthcare provider about these or other procedures you may need.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
How can I manage my symptoms?
- Keep a supply of pads or tampons with you at all times. If possible, stay close to a bathroom.
- Apply heat on your abdomen to decrease pain and cramps. You can use a heating pad on a low setting. Apply heat for 20 to 30 minutes every 2 hours for as many days as directed.
Call your local emergency number (911 in the US) for any of the following:
- You have chest pain and shortness of breath.
- Your heart is fluttering or beating faster than usual for you.
When should I seek immediate care?
- You feel dizzy when you stand.
- You feel confused.
- You have severe abdominal pain, nausea, and vomiting.
- Your skin or the whites of your eyes turn yellow.
When should I call my doctor?
- You need to change your pad or tampon more than 1 time per hour, for several hours in a row.
- You feel more weak and tired than usual.
- You have new coldness in your hands and feet.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Menorrhagia
Treatment options
Care guides
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
