H Pylori (Helicobacter Pylori) Infection
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is a Helicobacter pylori (H. pylori) infection?
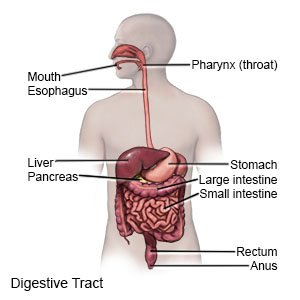
H. pylori bacteria infect the lining of the stomach and upper intestine. People are usually infected with the bacteria as children but do not have symptoms until they are adults.
 |
What are the signs and symptoms of an H. pylori infection?
Most people who are infected with H. pylori do not develop symptoms. If you do, your symptoms may come and go and last for minutes or hours. You may feel better for a short time after you eat food or take medicine. You may have any of the following:
- Dull or burning pain in your stomach or throat
- Nausea, vomiting, bloating, or burping
- Loss of appetite or weight loss
- Pain at night or with an empty stomach
How is an H. pylori infection diagnosed?
- A urea breath test means you will swallow pudding, liquid, or a capsule that contains a chemical. Then you will breathe into a container. Your breath sample will be tested for a reaction to the chemical that confirms H. pylori infection.
- Bowel movement or blood samples may be tested for infection.
- Endoscopy is a procedure that may be done if your healthcare provider thinks you have an ulcer. The provider will use a scope to see the inside of your stomach. A scope is a soft, flexible tube with a light and tiny camera on the end. It is passed down your throat and into your stomach. Samples of your stomach tissue may be removed and tested for H. pylori infection.
How is an H. pylori infection treated?
It is important to treat the infection. H. pylori may lead to changes in the cells of your esophagus or stomach. The cells are changed into intestine cells. This is a condition called intestinal metaplasia that increases your risk for cancer of the esophagus or stomach. The following are often used together to treat an infection:
- Antibiotics help kill the bacteria. You may need to take this medicine for 10 to 14 days. Your healthcare provider will prescribe at least 2 antibiotics at the same time.
- Antiulcer medicines help decrease the amount of acid that is normally made by the stomach. These help relieve pain and heal or prevent ulcers.
- Bismuth is a liquid or tablet that may be used to decrease heartburn, upset stomach, or diarrhea. It may also decrease swelling in your stomach and help treat the infection if other medicines do not work. It also protects ulcers from stomach acid so they can heal.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
How can I prevent or manage an H. pylori infection?
- Wash your hands often. Infection can happen through contact with infected bowel movement, vomit, or saliva. Use soap and warm water. Use an alcohol-based gel if soap and water are not available. Clean your hands before you eat and after you use the bathroom. Clean your hands after you change a baby's diaper.

- Handle food properly. Infection can happen if you drink water that is not clean or eat food that is not washed or cooked properly. Rinse food well before you cook or eat it. Cook food all the way through. Proper handling will help kill any bacteria that may be on your food.
- Drink clean water from a safe source. Only drink water that has been filtered or purified.
- Ask about NSAIDs. NSAIDs, such as ibuprofen, can cause stomach bleeding and kidney problems if not taken correctly. Your healthcare provider may tell you to avoid these medicines because they can make your symptoms worse.
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can worsen your symptoms. Ask your provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your provider before you use these products.
- Do not drink alcohol. Alcohol may worsen your symptoms of heartburn. Alcohol also increases the risk for cancer of the esophagus or stomach. Ask your provider for information if you currently drink alcohol and need help to quit.
Related medications
When should I seek immediate care?
- You have bloody bowel movements, bloody vomit, or vomit that looks like coffee grounds.
- You have sudden, sharp stomach pain that does not go away or spreads to your back.
When should I call my doctor?
- Your symptoms do not improve with treatment.
- You feel full after eating only a small amount of food.
- You lose weight without trying.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about H Pylori Infection
Treatment options
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
