Peptic ulcer
Medically reviewed by Drugs.com. Last updated on Jun 10, 2025.
What is a peptic ulcer?

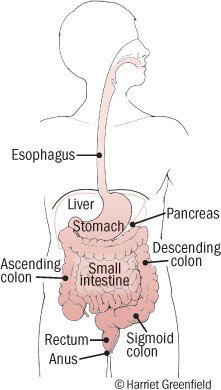
A peptic ulcer is a sore or hole that forms in the lining of the stomach or nearby small intestine.
The word "peptic" refers to the digestive tract. An ulcer in the lining of the stomach is a gastric ulcer. An ulcer in the first part of the small intestine is a duodenal ulcer.
|
|
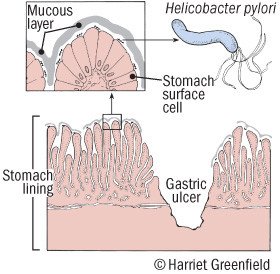
The lining of the stomach is a layer of special cells and mucus. Mucus prevents the stomach and duodenum from being damaged by acid and digestive enzymes.
If there is a break in the lining (such as an ulcer), the tissue under the lining can be damaged by the enzymes and corrosive acid. If the ulcer is small, there may be few symptoms. The wound can heal on its own.
If the ulcer is deep, it can cause serious pain or bleeding. Rarely, acids in the digestive juices may eat completely through the stomach or duodenum wall (called a perforated ulcer).
Peptic ulcers are very common. They become more common as people age.
The bacterium Helicobacter pylori is believed to cause most peptic ulcers. This bacterium causes inflammation in the stomach lining. This probably makes the lining vulnerable. But only a minority of people infected with H. pylori develop ulcers.
|
|
Another common cause of peptic ulcers is the use of nonsteroidal anti-inflammatory drugs (NSAIDs). Examples of NSAIDs include aspirin, ibuprofen (Advil, Motrin), and naproxen (Aleve, Naprosyn).
NSAIDs block the formation of some prostaglandins. Prostaglandins are chemicals that normally help protect against ulcers. With less prostaglandins, ulcers are more likely to form.
Besides H. pylori and NSAID use, several factors can increase your risk of developing a peptic ulcer. Risk factors include
- family history
- smoking (particularly if you are infected withH. pylori)
- excessive alcohol use.
However, contrary to popular belief, stress and spicy foods do not seem to increase the risk of ulcers.
Symptoms of peptic ulcer
Most people with ulcers complain of a burning or gnawing pain in the upper abdomen. This typically occurs when the stomach is empty. These symptoms may be worse at night or upon waking. However, some people's pain may worsen when they eat.
Other symptoms include
- nausea
- vomiting
- loss of appetite
- bloating
- burping
- weight loss.
Some of these symptoms may be relieved by taking over-the-counter antacids or avoiding spicy or acidic foods.
In general, symptoms worsen as an ulcer grows, or if more than one ulcer develops. Some people with mild disease don't have any symptoms.
In more severe cases, ulcers may bleed or extend deep into the wall of the stomach or intestine. Bleeding from large ulcers can be life-threatening. Blood may appear in the vomit. It may appear either red or black or resemble coffee grounds. Blood also may appear in the stools, which often have a tarlike consistency with a black or maroon color.
Peritonitis is an inflammation of the abdominal cavity, and may be due to chemicals leaking out of the stomach or small intestine, infection, or both. It may develop if the ulcer eats completely through the wall of the stomach or intestine and represents a medical emergency.
Diagnosing peptic ulcer
If your health care professional suspects that you have a peptic ulcer, he or she may recommend one of the following tests:
- A blood antibody test for evidence of H. pylori infection. This test is widely available and simple to do. If the test is positive, treatment might be given without more invasive tests. However, the H. pylori blood test is not always accurate. The test results may remain positive for years after an H. pylori infection has been treated. Also, the test cannot tell whether an H. pylori infection has caused an ulcer.
- A stool test for the presence of H. pylori antigen. This test is more specific than the blood antibody test.
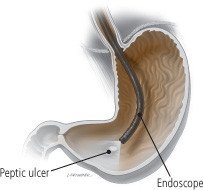
- An esophagogastroduodenoscopy (EGD or endoscopy). A flexible, lighted tube with a tiny camera on the end is passed through your throat into your stomach and intestines. This allows your doctor to examine the walls of the stomach and duodenum. The doctor may snip off a small piece of the lining of the stomach for a biopsy that is closely examined under a microscope. A biopsy can show whether there is an ongoing infection with H. pylori. It can also check to make sure an ulcer did not form because of cancer.
|
|
- An upper-gastrointestinal (GI) series. This test is rarely done today because endoscopy is generally a better test. An upper GI series involves a series of x-rays taken after you drink a chalky liquid that coats the esophagus, stomach, and upper part of the intestine.
- Other tests for H. pylori. Another test to detect the bacteria is called a urea breath test. You swallow a substance containing carbon (which may have a small amount of radioactivity). A positive breath test suggests that H. pylori is present in your stomach.
Stool samples can be tested for proteins that are associated with the bacteria.
Sometimes, more than one test is needed to diagnose your condition.
Expected duration of peptic ulcer
Ulcers caused by a medication (such as an NSAID) should begin healing shortly after you stop taking the drug. Anti-acid medicine may be used for two to six weeks to help healing and relieve pain.
Ulcers caused by H. pylori usually heal after the bacteria are killed. Typically, you will take antibiotics along with acid-suppressing medicine for two weeks. Then you may take acid-suppressing medication for another four to eight weeks. An ulcer related to H. pylori can temporarily heal without antibiotics. But it is common for an ulcer to recur or for another ulcer to form nearby if the bacteria are not killed.
Gastric ulcers tend to heal more slowly than duodenal ulcers. Uncomplicated gastric ulcers take up to two or three months to heal completely. Duodenal ulcers take about six weeks to heal.
Preventing peptic ulcer
Infection with H. pylori is extremely common. It is probably spread from person to person. Crowded living space appears to be a risk factor. Good hygiene may limit the spread of H. pylori somewhat. This includes washing your hands thoroughly before eating and after using the bathroom.
Recurrent ulcers from H. pylori can usually be prevented if you get appropriate treatment for your first ulcer. This should include antibiotics that kill the bacteria.
You may reduce your risk of developing a peptic ulcer by
- not smoking
- avoiding excessive alcohol use
- limiting the dose and duration of NSAIDs.
Drugs used to treat this and similar conditions
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Treating peptic ulcer
For ulcers caused by H. pylori, treatment requires a combination of medications. The goals of treatment are to
- kill H. pylori bacteria in the body
- reduce the amount of acid in the stomach
- protect the lining of the stomach and intestines.
Treatment of H. pylori may include a four-drug regimen for 10 to 14 days, such as bismuth, metronidazolem, tetracycline, and a proton pump inhibitor (PPI) such as lansoprazole or omeprazole.
An example of a three-drug approach includes rifabutin, amoxicillin, and a PPI.
Your doctor will prescribe a specific regimen based on convenience, cost and any allergies you have. A month or two after completion of treatment, testing for H. pylori (usually by breath or stool tests) can confirm elimination of the bacteria; if the test remains positive, another course of treatment may be recommended.
If your ulcer occurred while you were using a nonsteroidal anti-inflammatory drug (NSAID), you will need to stop taking it. Healing will begin almost immediately. Your doctor also will recommend medications to reduce acid damage during healing. These may include antacids to neutralize gastric acids. Medications that decrease the amount of acid produced by the stomach may also be used. Examples include H2 blockers (such as famotidine) or a PPI.
Emergency treatment may be needed if an ulcer causes serious bleeding. Usually, this treatment is done through an endoscope. Acid-blocking medications may be given intravenously (injected into a vein). Blood transfusions may be necessary if the bleeding is severe.
In rare circumstances, surgery may be needed to treat a perforated or bleeding peptic ulcer. Surgery for peptic ulcer disease may involve closing a bleeding artery.
Surgery is rarely needed for peptic ulcer treatment these days because treatments for H. pylori infections and other causes of peptic ulcer disease are so successful.
When to call a professional
Call for medical advice if you have continuing abdominal pain or indigestion. Also call if you need to take antacids frequently to prevent these symptoms. Seek emergency care if you experience:
- a sudden sharp pain in your abdomen
- bloody or black vomit
- maroon or black stools.
Prognosis
With proper treatment and preventive measures after an initial peptic ulcer, the outlook for peptic ulcers is excellent.
Additional info
National Institute of Diabetes & Digestive & Kidney Disorders
https://www.niddk.nih.gov/
American College of Gastroenterology (ACG)
https://www.acg.gi.org/
American Gastroenterological Association
https://www.gastro.org/
Learn more about Peptic ulcer
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.