Peptic Ulcer
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is a peptic ulcer?
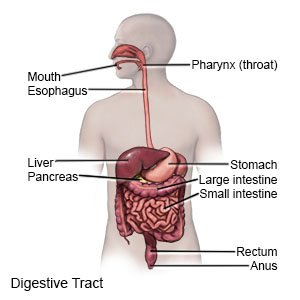
A peptic ulcer is an open sore in the lining of your stomach, intestine, or esophagus. Peptic ulcers have different names, depending on their location. Gastric ulcers are peptic ulcers in the stomach. Duodenal ulcers are peptic ulcers in the small intestine. Esophageal ulcers are peptic ulcers in the esophagus. Peptic ulcers may be a short-term or long-term problem.
 |
What causes or increases my risk for a peptic ulcer?
- Bacteria in the stomach called Helicobacter pylori (H. pylori)
- Certain medicines, such as NSAIDs or aspirin
- Zollinger-Ellison syndrome
- Cigarettes or alcohol
- Physical stress, such as from a burn or severe illness
- A family history of peptic ulcers
What are the signs and symptoms of a peptic ulcer?
- Burning or pain in your upper abdomen 1 to 3 hours after you eat or when your stomach is empty
- Pain that is worse at night or that comes and goes for weeks
- Pain that is relieved or worse when you eat or take antacid medicine
- Nausea, vomiting, or burping
- Red or black bowel movements from bleeding caused by the ulcer
How is a peptic ulcer diagnosed?
- Blood tests may be done to test for H. pylori.
- A sample of your bowel movement may be sent to a lab for tests. The test can show if you have H. pylori or if there is blood in your bowel movements.
- A urea breath test checks for H. pylori. You will drink a liquid that has a radioactive carbon. Thirty minutes after you drink the liquid, you will blow into a bag. The radioactive carbon will show if H. pylori is present.
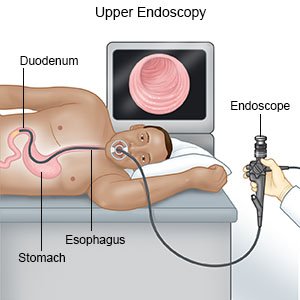
- An endoscopy uses a scope to see the inside of your digestive system. A scope is a long, flexible tube with a light on the end. A camera may be used with the scope to take pictures. During an endoscopy, your healthcare provider may find problems with how your digestive system is working. Samples may be taken from your digestive system and sent to a lab for tests.
- An upper GI x-ray is a picture of your stomach and intestines. You may be given a chalky liquid to drink before the pictures are taken. This liquid helps your stomach and intestines show up better on the x-rays. An upper GI x-ray can show if you have an ulcer.
Related medications
How is a peptic ulcer treated?
- Medicines that decrease the amount of acid made by your stomach may be given. You may also need medicines that protect your stomach lining from acid and antibiotics to treat H. pylori infection. Your healthcare provider may make changes to your current medicines if it caused your ulcer. Do not make changes to your medicines without your provider's direction.
- Surgery may be needed if other treatments do not heal your ulcer. Surgery on the nerves in your stomach may be done to help your stomach make less acid. Another type of surgery removes part of your stomach. Surgery may also be done to close an ulcer that has caused a perforation (tear) through your stomach or intestines.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Call your local emergency number (911 in the US) if:
- You have a fast heartbeat or fast breathing.
- You are too dizzy or weak to stand up.
- You vomit bright red blood.
- You have bright red blood in your bowel movement.
When should I seek immediate care?
- You have severe pain in your stomach.
- Your vomit looks like coffee grounds.
- Your bowel movements are black.
- You have sudden shortness of breath.
When should I call my doctor?
- You have a fever.
- You have diarrhea or constipation.
- Your stomach pain does not go away or gets worse after you take medicine.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Peptic Ulcer
Treatment options
- Medications for Peptic Ulcer
- Medications for Peptic Ulcer with Hemorrhage
- Medications for Peptic Ulcer with Hemorrhage and Obstruction
- Medications for Peptic Ulcer with Hemorrhage and Perforation
- Medications for Peptic Ulcer with Hemorrhage/Perforation/Obstruction
- Medications for Peptic Ulcer with Obstruction
- Medications for Peptic Ulcer with Perforation
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
