Prostatic Urethral Lift
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
A prostatic urethral lift
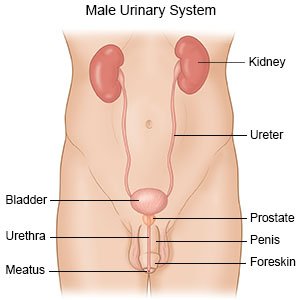
is a minimally invasive procedure to widen your urethra. The procedure is used to treat benign prostatic hyperplasia (BPH), or enlarged prostate. Small, permanent implants hold prostate tissue away from the sides of the urethra. This may make it easier for you to urinate.
 |
How to prepare for this procedure:
- Your healthcare provider will tell you how to prepare. Your provider may tell you not to eat or drink after midnight on the day of your procedure. Arrange to have someone drive you home after you are discharged.
- Tell your provider about all your current medicines. Your provider will tell you if you need to start or stop taking any medicine for the procedure, and when to do so.
- Tell your provider about any allergies you have, including to medicines, anesthesia, stainless steel, nickel, or titanium.
- Your provider will tell you if you need tests before your surgery, and when to have them.
What will happen during the procedure:
- You may be given local anesthesia and medicine to help you relax during the procedure. You may feel pressure or feel like you need to urinate during the procedure. You may be given general anesthesia instead to keep you asleep and pain free during the procedure.
- Your healthcare provider will insert a cystoscope through your urethra. A cystoscope is a thin tube with a small light and a camera on the end. The camera shows your prostate on a screen during the procedure.
- Your provider will put a device into your urethra through the cystoscope. The device is moved up to your prostate. This device is used to place 2 to 4 small implants into both sides of your prostate. The implants pull prostate tissue away to open your urethra.
What to expect after the procedure:
Your healthcare provider will monitor you for any problems. You may be able to go home after your provider sees that you are okay.
- You may go home with a urinary catheter. This is a thin, flexible tube inserted into the bladder to drain urine. Your provider will tell you when the catheter can be removed.
- You may have pelvic pain, blood in your urine, or burning when you urinate. You may feel like you have to urinate urgently or more often. These effects are all expected and should get better within a few weeks.
- Your BPH symptoms should start to improve within a few weeks of the procedure.
Risks of a prostatic urethral lift:
You may leak urine or scar tissue may build up in your urethra. You may have trouble having sex, or develop a condition called retrograde ejaculation. This means semen goes into your bladder when you ejaculate. You may have blood clots in your urine that block your urethra. The procedure may not prevent your BPH symptoms from getting worse. You may need a different procedure or surgery to help with symptoms.
Related medications
Seek care immediately if:
- You see blood clots in your urine.
- You see blood in your urine for longer than you were told to expect.
- You urinate small amounts or not at all.
- You have severe pain in your pelvis or groin.
Call your doctor or urologist if:
- You have a fever or chills.
- You have pain when you urinate that gets worse.
- You have trouble getting an erection or ejaculating.
- You have questions or concerns about your condition or care.
Medicines:
You may need the following:
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. NSAIDs can cause stomach bleeding or kidney problems in certain people. If you take blood thinner medicine, always ask your healthcare provider if NSAIDs are safe for you. Always read the medicine label and follow directions.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Self-care:
- Rest as directed. Your healthcare provider will tell you when you can go back to work or do your usual activities.
- Talk to your provider about sexual activity. You may need to wait a week or longer so the procedure area can heal fully. You should not notice much of a change during sex. You may notice a pulling feeling when you ejaculate. This should get better with time.
Bladder management after the procedure:
- Train your bladder. This will help your bladder hold urine longer. Go to the bathroom at set times, such as every 2 hours, even if you do not feel the urge to go. Work up to every 3 or 4 hours. You can also try to hold your urine when you feel the urge to go. For example, hold your urine for 5 minutes when you feel the urge to go. As that becomes easier, hold your urine for 10 minutes.
- Limit liquids as directed. This may help decrease the amount you urinate. Ask how much liquid to drink each day and which liquids are best for you. Do not drink liquids for several hours before you go to sleep. Limit alcohol and caffeine. These can increase your need to urinate.
- Do Kegel exercises often. Kegel exercises help strengthen your pelvic muscles and improve bladder control. Squeeze these muscles tightly for 5 seconds like you are trying to stop the flow of urine. Then relax for 5 seconds. Gradually work up to squeezing for 10 seconds. Do 3 sets of 15 repetitions a day, or as directed.
- Maintain a healthy body weight. High body weight increases your risk for obstructive sleep apnea (OSA). OSA can cause you to get up at night to urinate. Ask your provider what a healthy weight is for you. Your provider can help you create a safe weight-loss plan, if needed. Eat healthy foods, such as fruits, vegetables, whole-grain breads, low-fat dairy products, beans, lean meats, and fish. Try to get at least 30 minutes of exercise 5 days a week, such as walking.

Follow up with your doctor or urologist as directed:
Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
