Peripheral Neuropathy
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is peripheral neuropathy (PN)?
PN is a type of nerve damage that can develop when your peripheral nerves are damaged. Peripheral nerves are located outside of the brain and spinal cord. These nerves send information from your brain and spinal cord to the rest of your body. Damage to these nerves can slow or stop their ability to send signals. PN is most common in the hands and feet. It can also affect body functions, such as urination or digestion.
What causes PN?
- Trauma or injury
- Infections, such as shingles, HIV, or Lyme disease
- Health conditions such as rheumatoid arthritis, cancer, or lupus
- Pressure on the nerve from a cast or repeated movements such as typing
- Alcohol misuse
- Exposure to toxins, such as industrial chemicals, lead, or mercury
What are the signs and symptoms of PN?
Your symptoms depend on the types of nerves damaged and where they are located. The following are some of the most common signs and symptoms:
- Pain or tingling in your legs, feet, arms, or hands that may feel sharp, stabbing, or burning
- Trouble walking or keeping your balance
- Weakness or trouble holding things
- Loss of your sense of touch or numbness
- Bruising easily
- Trouble controlling your bladder or bowels or having sex
How is PN diagnosed?
Your healthcare provider will examine you and ask about your symptoms. He or she may ask you about your other health conditions and about your family health history. Your provider may touch your skin in different areas with a cotton ball or a pin to check your sense of touch. He or she may also check how well you can feel hot and cold. Your provider will ask you to do simple movements. For example, he or she may ask you to walk or to move your fingers. You may also need any of the following:
- Blood tests may show conditions that may be causing your PN.
- A filament test may show your sensitivity to touch. A soft nylon fiber is brushed over areas of your skin.
- Sensory testing may show how your nerves respond to vibration or temperature changes.
- Nerve and muscle testing may show how quickly your nerves or muscles respond to electrical signals.
- A nerve biopsy is used to take a sample of nerves to be tested.
Related medications
How is PN treated?
- Medicines:
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. This medicine is available with or without a doctor's order. NSAIDs can cause stomach bleeding or kidney problems in certain people. If you take blood thinner medicine, always ask your healthcare provider if NSAIDs are safe for you. Always read the medicine label and follow directions.
- Seizure medicines and antidepressants may help relieve nerve pain. These medicines change how your nerves and brain communicate pain.
- Topical treatments, such as creams or patches may also help decrease pain.
- A physical therapist teaches you movements and exercises to help improve movement and strength, and to decrease nerve pain.
- Transcutaneous electrical nerve stimulation (TENS) stimulates your nerves and may decrease your pain. Pads are attached to your skin and a mild gentle current is given.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
How can I manage PN?
- Treatment of underlying conditions is the best way to manage your PN. This may include treating conditions such as rheumatoid arthritis or an infection. This may also include healing of an injury or trauma.
- Check your skin daily. Look for redness and swelling, and feel for warmth. Sores can form where your skin makes contact with objects or other body parts. They also can form under splints.
- Be physically active at least 30 minutes, 5 days a week. Ask your healthcare provider about the best activity plan for you. Use caution when you exercise if you have decreased feeling in your feet.

- Limit alcohol as directed. Alcohol can cause high blood sugar levels and weight gain if you drink too much. A drink of alcohol is 12 ounces of beer, 5 ounces of wine, or 1½ ounces of liquor. Your healthcare provider can tell you how many drinks are okay to have within 24 hours and within 1 week.
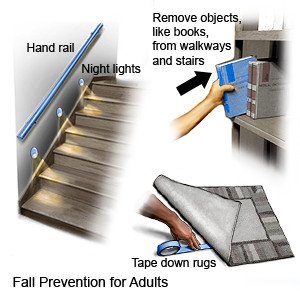
- Prevent falls. Move with care, and stand up slowly. Wear shoes that support your feet, and do not go barefoot. Ask about walking aids, such as a cane or walker. You may want to install railings or nonslip pads in your home, especially in the bathroom. Ask for more information on how to prevent falls.
When should I seek immediate care?
- You are injured from a fall.
- Your legs or feet start to turn blue or black.
- You have severe trouble walking.
- You have a wound that does not heal or is red, swollen, or draining fluid.
When should I call my doctor or neurologist?
- Your pain is severe.
- You cannot control your bladder.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Peripheral Neuropathy
Treatment options
- Medications for Autonomic Neuropathy
- Medications for Peripheral Neuropathy
- Medications for Refsum's Disease
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
