Paracentesis
Medically reviewed by Drugs.com. Last updated on Sep 23, 2025.
AMBULATORY CARE:
Paracentesis
is a procedure to remove abnormal fluid buildup in your abdomen. Fluid may build up because of liver problems, such as swelling and scarring. Heart failure, kidney disease, a mass, or problems with your pancreas may also cause fluid buildup.
How to prepare for paracentesis:
Your healthcare provider will tell you how to prepare. Tell your provider about all the medicines you take, including over-the-counter medicines. Your provider will tell you what medicines to take or not take on the day of your procedure. Tell your provider if you take any blood thinning medicines, including aspirin, an NSAID, or a prescription blood thinner. If you are a woman, tell your provider if you are or think you may be pregnant. Tell your provider if you have ever had an allergic reaction to any numbing medicine. Also tell your provider about any health conditions you have.
What happens during paracentesis:
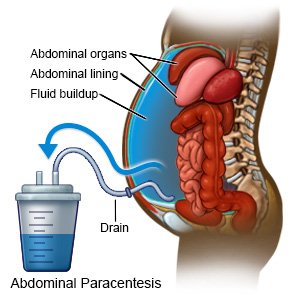
- Your healthcare provider will tap on and feel your abdomen to decide where to insert the needle. Your provider may also use an ultrasound to help decide where to insert the needle. Numbing medicine will be put on your skin where the procedure will be done. This medicine will help prevent pain. A needle will be inserted into your abdominal cavity. A syringe will be attached to the needle to remove a small amount of fluid.
- To remove a larger amount of fluid, a needle will be inserted into your abdominal cavity. A catheter (small, thin tube) is attached to the needle and the needle is removed. The catheter tubing will be attached to a suction device to help remove the fluid. The fluid will drain into a container attached to the tubing. The removal of large amounts of fluid may take up to 6 hours. When your healthcare provider has pulled enough fluid from your abdomen, the catheter will be removed. Your wound (procedure site) will be covered with a bandage. The fluid may be sent to a lab for tests.
 |
What to expect after paracentesis:
You may need to lie on the side without the wound for up to 2 hours. This may prevent fluid leakage from your wound. If the wound leaks and will not stop, your healthcare provider may stitch the area closed. You may need fluids or volume expanders given through your IV after your procedure. These fluids include albumin or saline. Albumin is a protein found in your blood. The IV fluids help prevent a drop in your blood pressure.
Risks of paracentesis:
During paracentesis, the needle may damage your abdominal organs or blood vessels. After paracentesis, you may bleed, or remaining fluid may leak out from your wound. You may get an infection in your wound, or in the lining of your abdomen. If a large amount of fluid is removed during your procedure, your blood pressure may become very low. This may decrease blood flow in your body and make you dizzy or short of breath. You may get a blood clot in your abdomen or lungs. A blood clot in your lungs can cause chest pain and trouble breathing, and can be life-threatening. Even with paracentesis, your kidney or liver function may not improve. Fluid may build up again, and you may need another paracentesis.
Seek care immediately if:
- You have sudden, sharp pain in your abdomen.
- You urinate very little or not at all.
- You feel confused and more tired than usual.
- Your arm or leg feels warm, tender, and painful. It may look swollen and red.
- You suddenly feel lightheaded and have trouble breathing.
- You have chest pain. You may have more pain when you take a deep breath or cough. You may cough up blood.
Related medications
Call your doctor if:
- You have a fever and your wound is red and swollen.
- You have yellow, green, or bad-smelling discharge coming from your wound.
- You have pain or swelling in your abdomen.
- You have nausea or are vomiting.
- Your legs and ankles are swollen.
- You have questions or concerns about your condition or care.
Medicines:
- Diuretics remove extra fluid and prevent new fluid buildup. You may urinate more often when you take this medicine.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Do not drink alcohol:
Alcohol can interact with the medicine you take after your paracentesis.
Wound care:
Ask your healthcare provider when you can remove your bandage, and how to care for your wound.
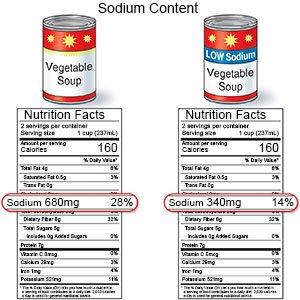
Eat low-sodium (salt) foods:
Sodium causes fluid to build up. Limit your sodium intake to 2 grams each day. Do not add salt to your food. Try to cook your own food instead of eating fast food or processed food. Read the labels on your food to see how much sodium they contain.
 |
Return to your normal activities:
Ask your healthcare provider which activities are safe for you to do. You may need to build up to your normal activity level slowly.
Follow up with your doctor as directed:
Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
