Lvad (Left Ventricular Assist Device)
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
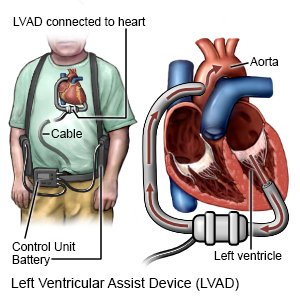
Your LVAD will allow you to be less tired, breathe better, and live longer. Living with your LVAD will be a big adjustment. A family member or friend must learn about your device so he or she can help you. The hospital will tell your electric company and emergency services in your area that you have an LVAD. The electric company will put you on a priority list to fix your power quickly if it goes out.
 |
DISCHARGE INSTRUCTIONS:
Call your local emergency number (911 in US) if:
- You have any of the following signs of a heart attack:
- Squeezing, pressure, or pain in your chest
- You may also have any of the following:
- Discomfort or pain in your back, neck, jaw, stomach, or arm
- Shortness of breath
- Nausea or vomiting
- Lightheadedness or a sudden cold sweat
- You have any of the following signs of a stroke:
- Numbness or drooping on one side of your face
- Weakness in an arm or leg
- Confusion or difficulty speaking
- Dizziness, a severe headache, or vision loss
Call your surgeon if:
- You have a fever higher than 100.4ºF (38ºC).
- Your incision begins to open.
- Your incision begins to drain.
- Your incision is red or warm to the touch.
- You are depressed or overwhelmed.
- You have questions or concerns about your condition or care.
Related medications
Medicines:
You will probably continue to take the heart failure medicines you were taking before surgery. Your surgeon will tell you what medicines to continue. Do not stop taking any medicine unless your surgeon tells you to. The LVAD and medicines will keep your heart working.
- Blood thinners help prevent blood clots. Clots can cause strokes and death. You will have to take blood thinners for the rest of your life. The following are general safety guidelines to follow while you are taking a blood thinner:
- Watch for bleeding and bruising while you take blood thinners. Watch for bleeding from your gums or nose. Watch for blood in your urine and bowel movements. Use a soft washcloth on your skin, and a soft toothbrush to brush your teeth. This can keep your skin and gums from bleeding. If you shave, use an electric shaver. Do not play contact sports.
- Tell your dentist and other healthcare providers that you take anticoagulants. Wear a bracelet or necklace that says you take this medicine.
- Do not start any medicines unless your healthcare provider tells you to. Many medicines cannot be used with blood thinners.
- Tell your healthcare provider right away if you forget to take the medicine, or if you take too much.
- Warfarin is a blood thinner that you may need to take. The following are things you should be aware of if you take warfarin:
- Foods and medicines can affect the amount of warfarin in your blood. Do not make major changes to your diet while you take warfarin. Warfarin works best when you eat about the same amount of vitamin K every day. Vitamin K is found in green leafy vegetables and certain other foods. Ask for more information about what to eat when you are taking warfarin.
- You will need to see your healthcare provider for follow-up visits when you are on warfarin. You will need regular blood tests. These tests are used to decide how much medicine you need.
- Take your medicine as directed. Contact your healthcare provider if you have side effects. Tell him or her if you are allergic to any medicine. Keep a list of the medicines you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Caring for your incision areas:
Your healthcare provider will teach you how to change the bandage on your incision areas. Change the bandage if it gets dirty or wet and as directed. Do not shower until your healthcare provider says it is okay. You will be taught how to keep the driveline dry while showering.
Activity:
- Cardiac rehabilitation (rehab) is a program run by specialists who will help you safely strengthen your heart and prevent more heart disease. The plan includes exercise, relaxation, stress management, and heart-healthy nutrition. Healthcare providers will also check to make sure any medicines you take are working. The plan may also include instructions for when you can drive, return to work, and do other normal daily activities.
- Do not swim or get in a tub. You will have a power source connected at all times. Do not let your power source and controller get wet.
- Always have backup equipment with you. You have to be prepared in case of an emergency or equipment malfunction. You must stay connected to the controller and power source at all times.
- Do not kink or bend the driveline. The pump will not be able to function properly. Also, do not sleep on your stomach or play contact sports. The driveline may become bent.
- Do not drive until your surgeon says it is okay.
Follow up with your surgeon and healthcare providers as directed:
You may need to follow up weekly for some time. Write down questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
