Chest Pain
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
Chest pain
can be caused by a range of conditions, from not serious to life-threatening. It is important to follow up with your healthcare provider to find the cause of your chest pain.
Common symptoms you may have with chest pain:
- Fever or sweating
- Nausea or vomiting
- Shortness of breath
- Discomfort or pressure that spreads from your chest to your back, jaw, or arm
- A racing or slow heartbeat
- Feeling weak, tired, or faint
Call your local emergency number (911 in the US) or have someone call if:
- You have any of the following signs of a heart attack:
- Squeezing, pressure, or pain in your chest
- You may also have any of the following:
- Discomfort or pain in your back, neck, jaw, stomach, or arm
- Shortness of breath
- Nausea or vomiting
- Lightheadedness or a sudden cold sweat
Seek care immediately if:
- You have chest discomfort that gets worse, even with medicine.
- You cough or vomit blood.
- Your bowel movements are black or bloody.
- You cannot stop vomiting, or it hurts to swallow.
Related medications
Call your doctor if:
- You have questions or concerns about your condition or care.
Treatment for chest pain
may include medicine to treat your symptoms while your healthcare provider finds the cause of your chest pain.
- Medicines may be given to treat the cause of your chest pain. Examples include pain medicine, anxiety medicine, or medicines to increase blood flow to your heart.
- Do not take certain medicines without asking your healthcare provider first. These include NSAIDs, herbal or vitamin supplements, and hormones, such as estrogen or progestin.
- One or more stents may need to be placed in your heart if pain was caused by blockage. A stent is a wire mesh tube that helps hold your artery open.
Healthy living tips:
If the cause of your chest pain is known, your healthcare provider will give you specific guidelines to follow. The following are general healthy guidelines:
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can cause lung and heart damage. Ask your provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your provider before you use these products.
- Choose a variety of healthy foods as often as possible. Include fresh, frozen, or canned fruits and vegetables. Also include low-fat dairy products, fish, chicken (without skin), and lean meats. Your provider or a dietitian can help you create meal plans. You may need to avoid certain foods or drinks if your pain is caused by a digestion problem.

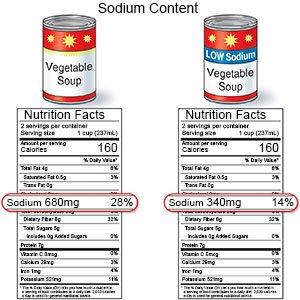
- Lower your sodium (salt) intake. Limit foods that are high in sodium, such as canned foods, salty snacks, and cold cuts. If you add salt when you cook food, do not add more at the table. Choose low-sodium canned foods as much as possible.
- Drink plenty of water every day. Water helps your body to control your temperature and blood pressure. Ask your provider how much water you should drink every day.
- Ask about activity. Your provider will tell you which activities to limit or avoid. Ask when you can drive, return to work, and have sex. Ask about the best exercise plan for you.
- Maintain a healthy weight. Ask your provider what a healthy weight is for you. Ask your provider to help you create a safe weight loss plan if you are overweight.
- Ask about vaccines you may need. Your provider can tell you if you also need vaccines not listed below, and when to get them:
- Ask your healthcare provider about the flu and pneumonia vaccines. All adults should get the flu (influenza) vaccine as soon as recommended each year, usually in September or October. The pneumonia vaccine is recommended for all adults aged 50 or older to prevent pneumococcal disease, such as pneumonia. Adults aged 19 to 49 years who are at high risk for pneumococcal disease should also receive the vaccine. You may need 1 dose or 2. The number depends on the vaccine used and your risk factors.
- COVID-19 vaccines are given to adults as a shot. At least 1 dose of an updated vaccine is recommended for all adults. COVID-19 vaccines are updated throughout the year. Adults 65 or older need a second dose of updated vaccine at least 4 months after the first dose. Your healthcare provider can help you schedule all needed doses as updated vaccines become available.
 |
Follow up with your doctor within 72 hours, or as directed:
You may need to return for more tests to find the cause of your chest pain. You may be referred to a specialist, such as a cardiologist or gastroenterologist. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Chest Pain
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
