Anterior Hip Replacement
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
What you need to know about anterior hip replacement:
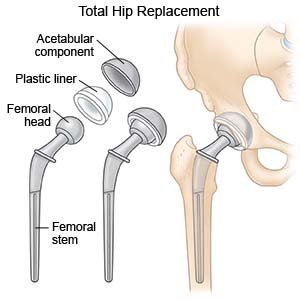
Anterior hip replacement (AHR) is surgery to replace a hip joint damaged by wear, injury, or disease. The hip joint is where the top of your femur (thigh bone) sits in the socket of your pelvic bone. The joint is held together by ligaments and muscles. The top of your femur is shaped like a ball and covered with cartilage. Cartilage is a tissue that helps joints move.
 |
How to prepare for anterior hip replacement:
Your healthcare provider will talk to you about how to prepare for surgery. He or she may tell you not to eat or drink anything after midnight on the day of your surgery. He or she will tell you what medicines to take or not take on the day of your surgery. You will be given an antibiotic through your IV to help prevent a bacterial infection.
What will happen during anterior hip replacement:
- Your healthcare provider may use general anesthesia or a spinal block. General anesthesia will keep you asleep and free from pain during surgery. With a spinal block, medicine is injected to numb the body area where the surgery will be done. You will remain awake during the surgery. Your surgeon may use fluoroscopy (a type of x-ray) to guide him or her during the surgery.
- Your surgeon will make a large incision on the front of your hip. Your healthcare provider will move your muscles aside so he or she can reach your hip joint. The ball of your femur and the socket of your pelvis will be removed. A hip implant will replace the bones that were removed. Your healthcare provider may use medical cement to secure the implant parts. A drain may be placed to remove extra blood and fluids from the surgery area. Your incision will be closed with stitches or staples and covered with a bandage.
What will happen after anterior hip replacement:
You may be asked to get up and try walking within 3 to 4 hours after surgery. You may need to stay in the hospital for 1 to 2 days. You may go home when you can walk a certain distance and go up and down stairs. You will be given a walking device, such as a walker, after surgery. You will be encouraged to bear weight on your hip as much as possible.
Risks of anterior hip replacement:
You may bleed more than expected or get an infection. Your nerves, blood vessels, ligaments, bones, or muscles may be damaged during surgery. Nerve damage can lead to tingling, numbness, weakness, or burning along your thigh. You may have more hip pain, or your hip joint may become stiff or numb. The length of your legs may not be the same after surgery. Your implant may become loose or move out of place. If this happens, you may need another surgery to replace the implant. You may get a blood clot in your limb. This may become life-threatening.
Call 911 for any of the following:
- You have chest pain when you take a deep breath or cough. You may cough up blood.
- Your leg feels warm, tender, and painful. It may look swollen and red.
- You suddenly feel lightheaded and short of breath.
Related medications
Seek care immediately if:
- Blood soaks through your bandage.
- Your incision wound comes apart.
- You urinate less than usual or not at all.
- Your wound is red, swollen, or draining pus.
Contact your healthcare provider if:
- You have a fever or chills.
- You have nausea or are vomiting.
- You have increased pain and swelling in your hip joint, even after you take pain medicine.
- You have questions or concerns about your condition or care.
Medicines:
- Prescription pain medicine may be given. Ask how to take this medicine safely.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Self-care:
- Care for your incision wound as directed. Do not get your wound wet until it is completely healed. Ask your healthcare provider when it is okay to get your wound wet. Change your bandage as directed and if it gets wet or dirty.
- Use a cane or walker as directed. These devices will help decrease your risk for falls right after surgery. Your healthcare provider will recommend that you place weight on your hip as much as possible.
- Do your exercises several times each day as directed. A physical therapist teaches you exercises to help improve movement and strength, and to decrease pain. Exercises build strength and prevent blood clots.
Activity:
You may be able to start driving 1 week after surgery. Ask your healthcare provider when you can return to your normal daily activities, such as work.
Follow up with your healthcare provider as directed:
You will need to have your stitches or staples removed. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
