Acute Coronary Syndrome
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is acute coronary syndrome (ACS)?
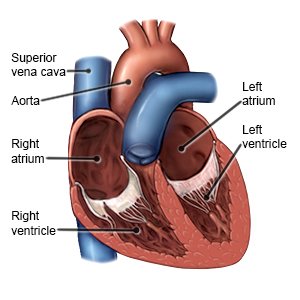
ACS is sudden decreased blood flow to your heart. This causes a lack of oxygen to your heart and can lead to unstable angina or a heart attack.
 |
What causes ACS?
ACS is caused by narrowing of the blood vessels that carry blood and oxygen to the heart muscle. The lack of blood and oxygen supply may lead to unstable angina or heart attack. Unstable angina occurs when part of the artery is blocked, or a clot gets stuck and then breaks free. A heart attack occurs when the artery becomes fully blocked, usually by a blood clot or buildup of plaque.
What increases my risk for ACS?
- A family history of coronary artery disease
- High cholesterol, diabetes, or high blood pressure
- A higher weight than recommended or poor nutrition
- Smoking cigarettes or lack of physical activity
What are the signs and symptoms of ACS?
- Chest pain or discomfort, including squeezing, crushing, pressure, tightness, or heaviness
- Pain or discomfort in your arms, shoulders, neck, back, or jaw
- Heartburn, nausea, or vomiting
- Abdominal pain
- Shortness of breath
- Sweating, weakness, or fainting
How is ACS diagnosed?
Your healthcare provider will ask about your symptoms and examine you. Tell your provider if you have any medical conditions and if you have a family history of heart disease. Your provider may also ask about medicines you take. Any of the following may be used to diagnose ACS:
- An EKG records the electrical activity of your heart. It is used to check for abnormal heart rhythm.
- Blood tests may show if there is damage to your heart muscle.
- An echocardiogram is a type of ultrasound. Sound waves are used to show the structure and function of your heart.
- A CT coronary angiogram uses x-ray pictures to check for plaque buildup in the arteries. Contrast liquid may be given to help arteries show up more clearly. Tell the provider if you have ever had an allergic reaction to contrast liquid.
- Cardiac catheterization is a procedure that uses an x-ray and contrast liquid to check your heart and the blood flow in your arteries. A tube is threaded to your heart through a blood vessel in your leg or arm. Contrast liquid may be given to help arteries show up more clearly. Tell the provider if you have ever had an allergic reaction to contrast liquid.
- An exercise stress test helps healthcare providers see how your heart works when you exercise. An EKG is done while you ride an exercise bike or walk on a treadmill.
- A stress test with medicine may be done if you cannot do the exercise stress test. You are given medicine that makes your heart work harder. You will be connected to an EKG machine.
Related medications
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Which medicines may be used to treat ACS?
- ACE inhibitors and beta-blockers keep your blood vessels open and help your heart pump strongly and regularly.
- Cholesterol medicine helps lower the amount of plaque buildup in your arteries.
- Blood pressure medicine helps decrease the strain on your heart.
- Pain medicine helps decrease your pain and slows your heart rate.
- Blood thinners help prevent blood clots. Clots can cause strokes, heart attacks, and death. Many types of blood thinners are available. Your healthcare provider will give you specific instructions for the type you are given. The following are general safety guidelines to follow while you are taking a blood thinner:
- Watch for bleeding and bruising. Watch for bleeding from your gums or nose. Watch for blood in your urine and bowel movements. Use a soft washcloth on your skin, and a soft toothbrush to brush your teeth. This can keep your skin and gums from bleeding. If you shave, use an electric shaver. Do not play contact sports.
- Tell your dentist and other healthcare providers that you take a blood thinner. Wear a bracelet or necklace that says you take this medicine.
- Do not start or stop any other medicines or supplements unless your healthcare provider tells you to. Many medicines and supplements cannot be used with blood thinners.
- Take your blood thinner exactly as prescribed by your healthcare provider. Do not skip a dose or take less than prescribed. Tell your provider right away if you forget to take your blood thinner, or if you take too much.
- Antiplatelets , such as aspirin, help prevent blood clots. Take your antiplatelet medicine exactly as directed. These medicines make it more likely for you to bleed or bruise. If you are told to take aspirin, do not take acetaminophen or ibuprofen instead.
- Thrombolytics help break apart and dissolve clots.
- Nitroglycerin opens the arteries to your heart so the heart gets more oxygen. It is given as a pill, IV, or topical patch or paste.
What are some other treatments for ACS?
In addition to medicines, your healthcare provider may recommend a procedure or surgery. Ask for information about each treatment. The following are commonly used to treat ACS:
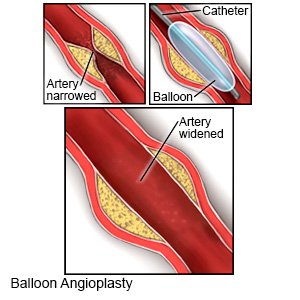
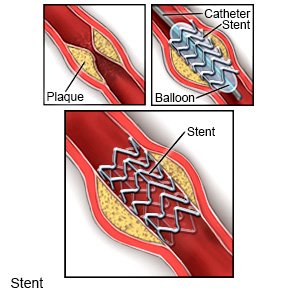
- Angioplasty with stenting may be done to open an artery blocked by plaque. A tube with a balloon on the end is put into the blocked artery. When the tube is in the artery, the balloon is inflated. As the balloon inflates, it presses the plaque against the artery wall to open the artery. A stent may be placed in your artery to keep it open.
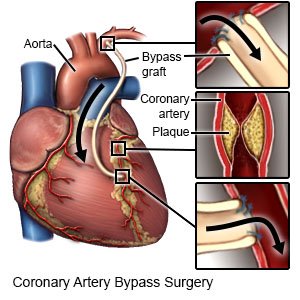
- Coronary artery bypass surgery is open-heart surgery. A surgeon takes arteries or veins from other areas in your body. These are used to bypass (go around) the blocked arteries of your heart.
- Cardiac rehabilitation (rehab) is a program to help you recover and improve your overall health. The program may include exercise, counseling, stress management, and heart-healthy nutrition.
How can I manage or prevent ACS?
ACS cannot always be prevented. The following can help you manage ACS and may help prevent it if you have certain risk factors:
- Manage other health conditions. High blood pressure and high cholesterol levels can worsen ACS. Ask your healthcare provider for more information on managing these or other health conditions. You may need to take medicines for these conditions and make other lifestyle changes.
- Eat heart-healthy foods. Include fresh fruits and vegetables in your meal plan. Choose low-fat foods, such as skim or 1% fat milk, low-fat cheese and yogurt, fish, chicken (without skin), and lean meats. Eat two 4-ounce servings of fish high in omega-3 fats each week, such as salmon, fresh tuna, and herring.

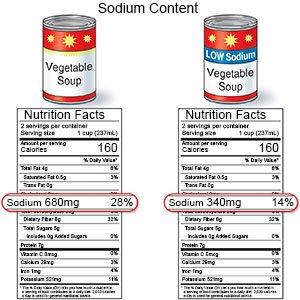
- Limit sodium (salt) as directed. Avoid foods that are high in sodium, such as canned foods, potato chips, salty snacks, and cold cuts. If you add salt when you cook, do not add more salt at the table.
- Be physically active. Physical activity, such as exercise, can lower your blood pressure, cholesterol, weight, and blood sugar levels. Healthcare providers will help you create physical activity goals. They can also help you make a plan to reach your goals. For example, you can break activity into 10-minute periods, 3 times in the day. Find activities you enjoy. This will make it easier for you to reach your goals.

- Maintain a healthy weight. Ask your provider what a healthy weight is for you. Your provider can help you create a safe weight loss plan, if needed.
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can cause heart and lung damage. Ask your provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your provider before you use these products.
- Limit or do not drink alcohol. Alcohol can raise your blood pressure and make your heart work harder. A drink of alcohol is 12 ounces of beer, 5 ounces of wine, or 1½ ounces of liquor. Your provider can tell you how many drinks are okay within 24 hours and within 1 week.
- Manage stress. Stress can raise your blood pressure or cause irregular heartbeat. Find new ways to relax, such as deep breathing or listening to music.
- Ask about vaccines you may need. Your provider can tell you which vaccines you need, and when to get them. The following vaccines help prevent certain diseases that can put more stress on your heart:
- The influenza (flu) vaccine is given each year. Get a flu vaccine as soon as recommended, usually in September or October.
- Ask your healthcare provider about the pneumonia vaccine. The vaccine is recommended for all adults aged 50 or older to prevent pneumococcal disease, such as pneumonia. Adults aged 19 to 49 years who are at high risk for pneumococcal disease should also receive the vaccine. You may need 1 dose or 2. The number depends on the vaccine used and your risk factors.
- COVID-19 vaccines are given to adults as a shot. At least 1 dose of an updated vaccine is recommended for all adults. COVID-19 vaccines are updated throughout the year. Adults 65 or older need a second dose of updated vaccine at least 4 months after the first dose. Your healthcare provider can help you schedule all needed doses as updated vaccines become available.
 |
Call your local emergency number (911 in the US) or have someone call if:
- You have any of the following signs of a heart attack:
- Squeezing, pressure, or pain in your chest
- You may also have any of the following:
- Discomfort or pain in your back, neck, jaw, stomach, or arm
- Shortness of breath
- Nausea or vomiting
- Lightheadedness or a sudden cold sweat
- You have any of the following signs of a stroke:
- Numbness or drooping on one side of your face
- Weakness in an arm or leg
- Confusion or difficulty speaking
- Dizziness, a severe headache, or vision loss
When should I call my doctor?
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Acute Coronary Syndrome
Treatment options
- Medications for Acute Coronary Syndrome
- Medications for Angina
- Medications for Heart Attack
- Medications for Ischemic Heart Disease
- Medications for Prinzmetal's Angina
Care guides
Symptoms and treatments
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
